 Medical Review By: John Koziarski, MD
Medical Review By: John Koziarski, MD
Thin, squiggly veins that are visible through the skin can be as mystifying as they are frustrating.
What causes spider veins? While there are many risk factors, a common underlying problem is venous insufficiency. In this condition, the valves in the veins become weakened or damaged. Normally, the valves close after the vein pumps blood back to the heart. But when the valves aren’t working properly, some of the blood leaks backward and pools. This causes the vein to bulge and branch out, creating web-like or tangled spider veins. Spider veins typically affect the legs but sometimes appear on the face. They may be red, blue or purple.
“I compare the venous insufficiency to leaks that occur in an underground lawn sprinkler system that create puddles on the surface,” said John Koziarski, MD, a board-certified general/vascular surgeon at The Vein Center at Water’s Edge Dermatology. “The puddles, like spider veins, are the visible result of the leaks.”
Risk factors for spider veins
The risk factors that make someone vulnerable to spider veins include:
Aging. Veins naturally weaken over time, making spider veins more likely.
Genetics. Spider veins run in families. You may have inherited valves that are prone to weakening. While spider veins don’t occur very often in young people, family history is usually the culprit when they do. “I’ve had some patients who are as young as teenagers, and the problem is that they simply had bad veins to begin with,” Dr. Koziarski said.
Being overweight or obese. Extra weight puts more pressure on the veins and may eventually cause the valves to fail.
Pregnancy. Pregnant women are vulnerable to spider veins due to weight gain and fluctuations in estrogen and progesterone levels, which can weaken the veins. While spider veins are usually permanent, those that develop during pregnancy sometimes go away once the baby is born and hormone levels stabilize.
Standing still for long periods. The contraction of your leg muscles helps pump blood through your vessels. Standing for long periods allows blood to stagnate in the veins. Dr. Koziarski noted, “You often see spider veins in people who have jobs that require hours of standing still, such as hair dressers and assembly line workers.”
A sedentary lifestyle. Too much sitting also causes blood to stagnate. As for crossing your legs while seated, contrary to popular belief, it’s not a major contributor to spider veins, said Dr. Koziarski. It can, however, cause pain in people who already have them by reducing blood flow out of the legs.

Sun exposure. While the sun doesn’t directly cause spider veins, heating the skin causes existing veins to dilate, or get larger, to help dissipate the heat.
Injuries. It’s uncommon, but some traumas, such as being hit with a softball, can damage the veins and lead to spider veins.
Are spider veins dangerous?
Spider veins themselves are not harmful to your health. However, they may indicate that a more serious problem, such as venous insufficiency.
Spider veins can be very uncomfortable. “While some people seek treatment for them for cosmetic reasons, most want to remove them because they may itch and cause a throbbing, burning or heavy sensation,” Dr. Koziarski explained.
How to prevent spider veins
You can’t necessarily prevent spider veins, especially if they run in your family, but these measures can help you lower your risk:
- Wear compression socks or stockings if recommended by your doctor; they help minimize the pooling of blood in the skin of the legs
- Maintain a healthy weight
- Exercise regularly
- Take walking breaks if you have to stand or sit for long periods
- Wear low-heeled shoes
- Elevate your legs above your heart when you lie down
How to get rid of spider veins
When you consult a vein surgeon, an ultrasound will be used to identify which veins are affected. Determining the source of the leakage that may be causing the spider veins helps the surgeon decide how to treat them.
Spider vein treatment options include:
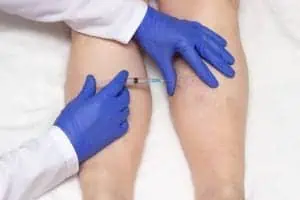
Ultrasound-guided foam sclerotherapy. In this variation of sclerotherapy, the provider uses ultrasound to help guide him or her to the affected vein. A foam solution is then injected that destroys the inner lining of the vein. This method may be recommended for larger veins.

Ohmic thermolysis. While this technique can be used on any area of the body, it’s often recommended for very fine spider veins on the face. A topical anesthetic may be applied to the treatment areas. The surgeon then uses a very fine needle to deliver small bursts of energy just below the skin but above the affected vein. The energy heats the vein, causing the blood to coagulate and the walls to collapse. Ohmic thermolysis has a very small risk of scarring.
With so many treatment options available, your surgeon should be able to find one that will effectively eliminate your spider veins, putting an end to any discomfort or itching they’ve caused and improving your appearance.
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.






