Hidradenitis
Suppurativa
Call (877) 900-3223
Hidradenitis Suppurativa:
Treatment and Causes
Overview
Signs and Symptoms of Hidradenitis Suppurativa
Causes of Hidradenitis Suppurativa
Treating Hidradenitis Suppurativa
Overview
Hidradenitis suppurativa (HS) is a rare, long-term skin disease that usually begins as pimple-like bumps that develop in areas where the skin rubs together, such as the underarms, groin, between the buttocks, and under the breasts.
Hidradenitis suppurativa tends to start after puberty and can last for many years. Without treatment, it can worsen over time. The pimple-like bumps can grow deep into the skin and become painful. They can rupture, leaking foul-smelling pus onto clothing. They may also cause tunnel-like tracts (fistulas) to develop under their skin.
As the deep bumps heal, scars can form and thicken. Thick scars in the underarm can make it difficult to move the arm, while thick scars in the groin area can make it difficult to walk.
Hidradenitis suppurativa can affect quality of life and emotional well-being. People who have a foul-smelling liquid draining from the breakouts can feel embarrassed. Restricted movement can be painful and fistulas may require surgery to repair.
Diagnosing and treating HS as soon as possible is important to help manage the symptoms, keep new bumps from forming, and prevent complications, such as scarring or depression.
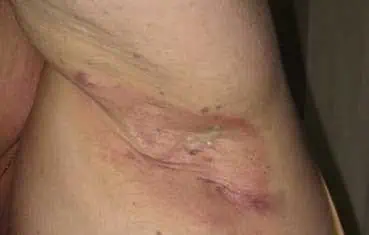
Image used with permission of the Journal of the American Academy of Dermatology. (J Am Acad Dermatol 2009;60:539-61.)
Signs and Symptoms of Hidradenitis Suppurativa
Unlike everyday pimples, hidradenitis suppurativa (HS) occurs in areas where skin touches skin, such as:
- One or both underarms
- Groin area, including the genitals and around the anus
- Buttocks
- Inner thighs
- Underneath women’s breasts
At first, hidradenitis suppurativa looks like a breakout of pimples or boils. Your skin may clear up for a while but then the bumps reappear in the same area. Some people always have breakouts on their skin. The signs and symptoms of HS can change over time.
Without treatment, HS can worsen. Progression of the disease may include:
- Painful, deep breakouts that heal and reappear
- Breakouts that rupture and leak a foul-smelling fluid
- Scars that form as breakouts repeatedly heal and reappear
- Scars that become thicker with time
- Skin that begins to look spongy as hollow passages called fistulas form deep in the skin
- Serious infections
- Skin cancer (rare)
Causes of Hidradenitis Suppurativa
Hidradenitis suppurativa forms when hair follicles clog with bacteria and other substances, although no one knows exactly why this blockage occurs. Because HS occurs after puberty, hormones likely play a role. Another theory is that the person’s immune system overreacts to the plugged hair follicle.
Risk factors include:
Age and Gender: HS typically occurs in women between puberty and menopause. Women are 3 times more likely to get HS than are men.
Genetics: Those who develop HS are more likely to have a blood relative with the condition.
Lifestyle: HS is most common in those who are overweight or obese, as well as smokers.
If a person is susceptible to getting HS, any of these could make HS appear for the first time or worsen existing HS. Although the exact cause of HS is still unknown, we do know that it is NOT contagious and not caused by poor hygiene.
Treating Hidradenitis Suppurativa
There are several treatment options for hidradenitis suppurativa, including prescription medications and surgery for severe cases. Treatments can help minimize or clear existing breakouts, prevent new breakouts, and get rid of scars and fistulas.
Medications
- Antibiotics: These drugs can reduce inflammation, fight infection, prevent HS from worsening, and stop new breakouts.
- Biologics: These drugs work by suppressing the immune system. In 2015, the FDA approved adalimumab (Humira®) for the treatment of moderate-to-severe HS. It is an injection you give to yourself. Other biologics require an infusion at a hospital or clinic. Some patients have seen long-term clearing of their HS with a biologic.
- Corticosteroids: Your Water’s Edge dermatologist may inject a corticosteroid directly into a painful cyst or recommend corticosteroid pills. Both reduce inflammation, which can help clear HS and prevent new breakouts.
- Hormones: Some women with HS get pain and symptom relief by taking birth-control pills, a medicine called spironolactone, or another medicine that regulates hormones. These medicines can decrease pain and the amount of fluid draining from the breakouts.
Surgical Treatments
For severe cases of HS, medicine alone may not be effective. When HS grows deep into the skin, your Water’s Edge dermatologist may recommend an outpatient surgical procedure.
- Laser surgery: This promising treatment, which destroys the hair follicles, is proving effective at clearing new and deep HS breakouts. For some patients, their HS clears up after several treatments.
- Deroofing: During this procedure, the surgeon turns deep, painful HS into scars. Deroofing may be an option for patients who have painful HS that repeatedly returns.
- Incision and drainage: During the surgery, the dermatologist makes an incision to drain one or two lesion or cut them out. While this may bring short-term relief, the HS can return.
- Excision: During this surgery, your dermatologist cuts out the HS along with some normal-looking skin. This creates a deep wound that will need to be covered with a skin graft (skin removed from another part of your body) or skin flap (skin from nearby is pulled over to cover the wound). Although HS will not return to the treated area, it can develop nearby.
Other Treatments
Zinc supplements taken daily may help reduce inflammation and prevent new outbreaks. Over-the-counter acne washes and medicines may be helpful in relieving symptoms but do they do not clear HS. Your Water’s Edge dermatologist may also recommend taking 5- or 10-minute bleach baths to fight colonies of bacteria on your skin.
In addition, making lifestyle changes can help tremendously. For some people with HS, weight loss and maintaining a healthy weight has proven highly effective at preventing breakouts – maybe even more effective than treatment.
No one treatment works for everyone who has HS. Sometimes, a patient needs to try a few different treatments to find one that works.





