Medical review by Ted Schiff, MD
Most doctor’s offices are still open — and in fact never closed — during the coronavirus pandemic. But some people have been avoiding seeing the doctor for fear of catching COVID-19. If you have a health condition that needs medical attention, however, that strategy can backfire. Left untreated, some conditions, including certain skin conditions, can pose serious threats.
See a dermatologist or other skin care provider, either via an in-office visit or a teledermatology (telemedicine) visit, if you experience any of these symptoms.
1. A bad, worsening or spreading rash
Some rashes, like poison ivy rash, typically resolve on their own and don’t usually require a doctor’s care. Other rashes need to be taken more seriously. For example, a rash that’s painful or gets worse quickly could stem from a serious infection. A rash all over the body could also indicate an infection, or an allergic reaction. If you have a rash combined with a fever or breathing difficulty, get to the emergency room. If you have a rash near your eye or on your genitals, especially if it blisters, see a doctor right away.
An infected rash is another reason to see a doctor. Infected rashes may be painful or warm to the touch and may crust or leak yellow or green fluid. Red streaks may appear on the skin near the rash.
2. A suspicious mole or other growth
If you notice an unusual new bump or growth on your skin or a suspicious mole — one that has changed in shape, size or color — don’t put off seeing a dermatologist, especially if you’ve had skin cancer in the past or you have a family history of skin cancer.
The provider may examine your growth or mole via a telederm visit, but if there’s any concern about skin cancer, you’ll need to be seen in person and possibly undergo a skin biopsy.
Whether or not you notice any suspicious growths, you’ll also want to keep up your annual skin cancer screenings, especially if you have a history of melanoma.
3. A sore that doesn’t heal
An open sore that won’t heal, or one that heals and then returns, could be a sign of basal cell carcinoma. It could also indicate a skin ulcer caused by diabetes, leg swelling or physical pressure from being bed- or wheelchair-bound. Whatever the cause, it needs medical attention.
4. Raised, scaly, itchy patches
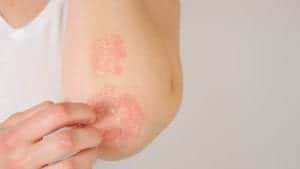
People with psoriasis face an increased risk of cardiovascular disease, diabetes and psoriatic arthritis, an inflammatory joint disease, which makes getting an accurate diagnosis especially important.
5. Purple discolorations on the hands or feet
A strange symptom appearing in some COVID-19 patients is purple spots on the hands or feet, especially the toes. So-called COVID toes are thought to stem from blockages or tiny clots in small blood vessels. They sometimes appear in children who have no other signs of the coronavirus — a helpful tipoff to the disease. The spots may eventually scab over. COVID-19 may also cause rashes in some people. See photos here.
A provider can examine any purples spots or rashes via a telederm visit. You should be able to send a photo in advance. If there’s a suspicion of COVID-19, you’ll want to get tested.
6. A painful red rash on one side of the body
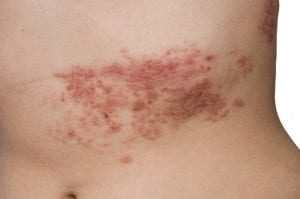
The pain may be bad enough that you need prescription painkillers, but that’s not the only reason to see a doctor right away. When shingles is diagnosed within 72 hours, oral antiviral medication can be prescribed to treat the shingles and also help prevent post-herpetic neuralgia, a long-lasting condition that involves burning pain.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.