Medical Review By: Ted Schiff, MD
If you have bothersome patches of itchy, red skin, you want relief. But first you need to know what’s causing the problem. If you’ve ruled out insect bites, poison ivy and other types of allergic contact dermatitis, then eczema or psoriasis may be likely contenders. These skin problems can look somewhat alike at first glance, and some of the treatments overlap, but they are distinct conditions with different causes and triggers.
Eczema and psoriasis are both inflammatory skin conditions that run in families and involve the immune system. They often arise in childhood, though more cases of psoriasis begin in adulthood. It’s possible to have both eczema and psoriasis.
The exact causes of eczema aren’t fully understood. People who get eczema may have a family history of eczema, asthma, hay fever or food allergies or sensitivities. The most common type of eczema is atopic dermatitis.
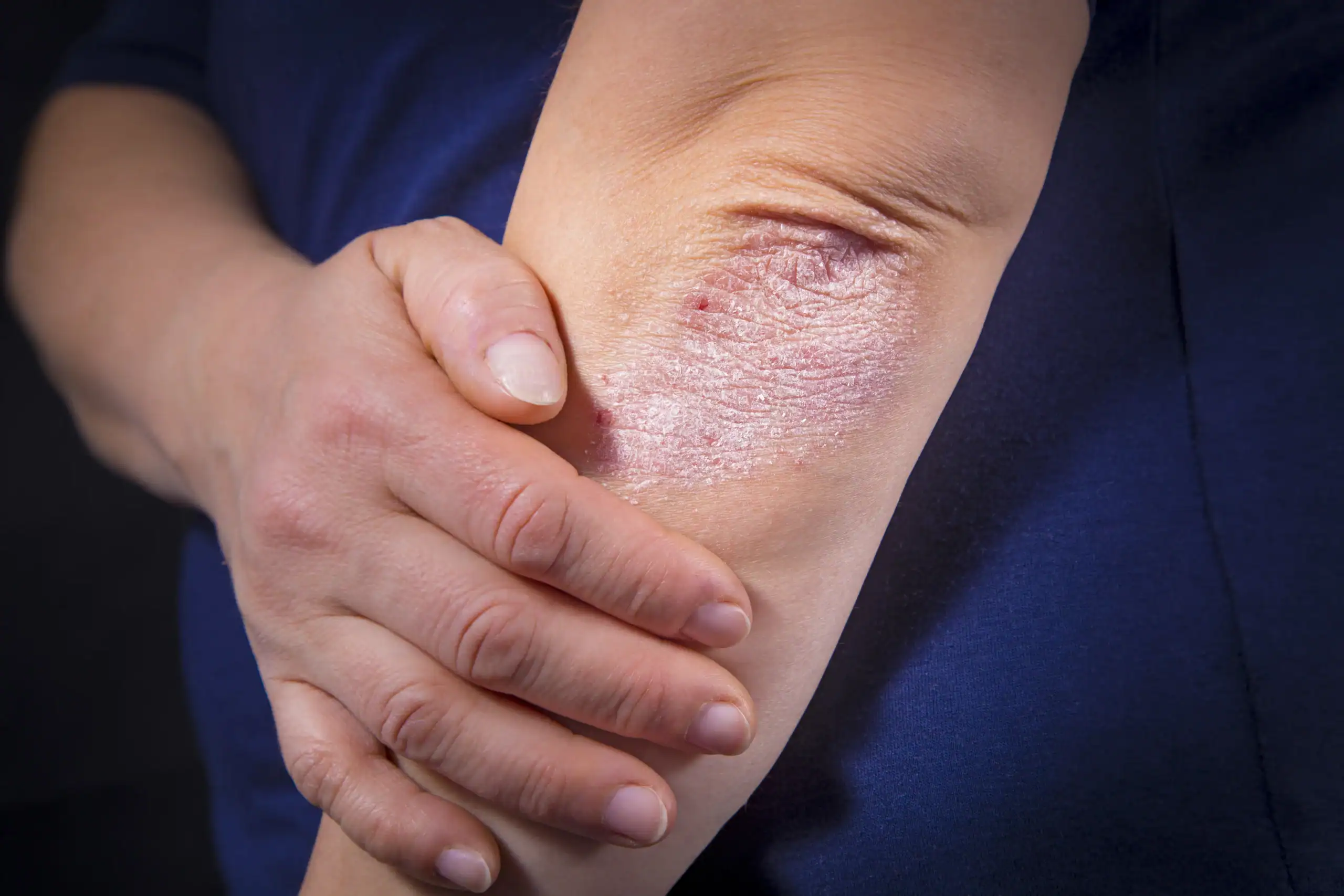
In plaque psoriasis, the most common type of psoriasis, the immune system goes into overdrive, causing new skin cells to develop much faster than normal. These cells pile up on the skin’s surface, causing bumpy, scaly patches called plaques, as you can see in the top photo. Psoriasis is linked with other inflammatory illnesses, including psoriatic arthritis, so getting an accurate diagnosis is important.
Below are some clues your skin care provider will use to tell the conditions apart.
Signs and symptoms
Eczema and psoriasis usually look different upon close inspection, and they feel different, too.
In eczema, the skin tends to be very dry and intensely itchy. In Caucasians, eczema patches appear red; in people with darker skin, the patches may look darker brown, purple or gray. Scratching can cause the skin to break, ooze, bleed and eventually crust. Over time, leathery dark patches may develop in the surrounding skin due to repeated scratching.
Psoriasis patches tend to be raised and well-defined — it’s usually obvious where a patch begins and ends. In Caucasians, the patches look pink or red with thick, silvery-white scales on top. In darker skin, the patches can be dark brown or purple, and the scales may be gray. In people with skin of color, the patches may be more widespread.
One big difference between the two conditions: Eczema causes intense itching, whereas psoriasis may itch mildly but also sting and burn.
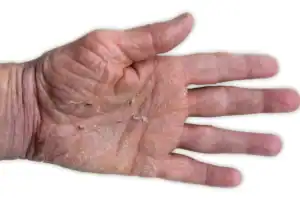
Location Matters
Eczema and psoriasis can show up just about anywhere on the body, but they are more common in some areas than others.
Eczema commonly appears on the:
- Hands
- Backs of the knees
- Insides of the elbows
- Back of the neck
- Face
- Eye area (in adults)
Psoriasis commonly appears on the:
- Elbows and knees
- Scalp
- Face
- Lower back
- Palms of the hands
- Soles of feet
- Fingernails and toenails
- Mouth and lips
- Eyelids
- Ears
Common Triggers
The two conditions are typically activated by different triggers.
In the case of eczema, triggers include exposure to skin irritants, such as wool fabrics, detergents or disinfectants and exposure to allergens, such as dust, pet dander, pollen and mold. Stress and sweating are other triggers. In people with hand eczema, frequent hand washing and dish washing can set off the itching.
With psoriasis, a skin injury such as a scratch, bruise, puncture or sunburn can trigger a flare, as can smoking, drinking alcohol, stress and certain medications, such as beta blockers.
Treatment for Eczema and Psoriasis
Treatment focuses on easing symptoms, lowering the risk of skin infection and reducing flares. Moisturizers help with both conditions, as does avoiding triggers.
Eczema treatments include prescription or over-the-counter topical corticosteroids and the topical medication crisaborole (Eucrisa), which blocks certain immune system proteins to reduce the body’s response to triggers. An antihistamine can sometimes help as well. Light therapy is another option. For widespread moderate to severe eczema, a biologic drug called dupilumab (Dupixent) may be given by injection to tamp down the immune system.
Psoriasis treatments include topical creams such as corticosteroids, retinoids and calcipotriene (a vitamin D derivative), light therapy, and for moderate to severe psoriasis, biologic drugs. The drugs, given by injection or infusion, can improve psoriasis symptoms dramatically. Many people achieve clear or nearly clear skin as a result.
Your dermatologist will recommend a course of treatment once an accurate diagnosis is made — so instead of trying to guess what condition you have, make an appointment.
Article Written By: Jennifer L. Cook, an award-winning editor and writer whose work has appeared in Good Housekeeping, Prevention, Consumer Reports on Health, and Woman’s Day and on Investopedia.com and Bottomlineinc.com.