When to Worry About a Spider Bite
Medical Review By: Thomas Pham, MD
Spider bites are more common than you might think. Garden spiders that get trapped in clothing or under hair may bite two or three times before you flick them off or crush them by scratching. Dermatologists sometimes call these bites “breakfast, lunch, and dinner.”
Fortunately, when it comes to spider bites, the ick factor is almost always worse than the bite. While nearly all spiders produce venom, it’s rarely strong enough to harm humans. Plus, most spiders’ fangs are too short to penetrate human skin.
Bites that produce mild pain or itching can usually be treated with over-the-counter hydrocortisone cream or ointment, cold compresses, and an oral antihistamine if needed to help with itching or swelling.
If you’re unlucky, however, you might encounter one of the two types of spiders in the United States that can seriously harm humans: the black widow and the brown recluse. While they’re not aggressive, they do bite in some circumstances, and there’s a chance you may need emergency treatment if you are bitten.
If possible, take a photo of the spider to help your doctor diagnose the bite and choose a course of treatment.
Black widow spiders
What they look like
Black widows have an almost spherical abdomen and are about half an inch long.
Southern black widow spiders are black with a red hourglass pattern on the underside of the body (females) or red and white markings on the sides of the body (males). In Northern black widows, the hourglass pattern is broken, and there may be a row of red spots on the back and diagonal whitish markings on the side (females). Male Northern black widows usually have faint red and white spots on the underside of the body.
What to know
Black widows can be found anywhere in the United States but are more common in the South and West.
While male black widow spiders don’t bite humans, females can and will attack to defend themselves if you disturb them, especially if they’re in their web protecting their eggs.
You’re most likely to run into a black widow’s web in dark and undisturbed areas, such as woodpiles, eaves, fences, and water meter boxes. When indoors, black widows usually build their webs in cluttered areas, such as a garage or basement.
Spider Bite Symptoms and Treatment
Black widow bites cause a sharp, pinprick-like pain. In many cases, reactions are relatively mild and limited to redness and swelling of the bite area. (You may also notice two tiny red spots that are actually tiny fang marks.) These symptoms appear 15 to 60 minutes after you’re bitten and can be treated at home with cold compresses, over-the-counter pain relievers, elevation (if the bite is on your arm or leg), antibiotic cream, or lotion.
Some people develop a severe reaction and experience signs and symptoms such as stiff and painful muscles, fever, chills, nausea, vomiting, difficulty breathing, weakness, tremors, headache, and belly or back pain. These may develop in as little as 15 minutes after the bite or several hours later. If you have a severe reaction, go to the emergency department or call 911.
Fatalities are rare. Elderly people and small children are more likely to have a severe, possibly life-threatening reaction.
Treatments for severe black widow bites include prescription pain relievers, muscle relaxants, and antivenom.
Brown recluse
What they look like
Brown recluse spiders are tan to dark brown with long legs. They often have a darker brown violin shaped-marking just behind their head.

What to know
Brown recluse spiders are typically found in Midwestern and Southern states. They truly are reclusive and would much rather avoid you than attack you. When they do bite, it’s usually because they were trapped against your skin and tried to defend themselves. This may happen if a brown recluse makes its way into your bedsheets, clothes, or shoes.
Brown recluses like to live under rocks, woodpiles, and debris. They’re also well adapted to living indoors, where they prefer dark areas such as basements, attics, closets, and cabinets.
Bite symptoms and treatment
If you’re bitten by a brown recluse, you may not notice right away because the bite is often painless or only mildly painful. In fact, you may never know you’ve been bitten. If symptoms do occur, they typically start three to eight hours after the bite and include redness, tenderness, and a sore at the site of the bite. Other possible symptoms include fever, chills, vomiting, muscle aches, and itching.
Severe symptoms such as extreme pain or trouble breathing require immediate medical attention. Bites in small children, elderly people, and those in poor health also require immediate medical attention.
Brown recluse bites usually heal within three weeks. However, in about 10% of cases, a bite can cause tissue death in the affected area. A skin ulcer or blister with a blue, purple or black center develops and may become infected.
Treatments for severe brown recluse bites include antibiotics, antihistamines, and steroids. Some victims need surgery to remove the damaged tissue around the wound.
At-home treatments for mild bites are the same as those for mild black widow bites.
Hobo and yellow sac spiders: Cause for concern?
These two types of spiders have a nasty reputation. It was once thought that their bites, like that of a brown recluse, could lead to tissue death. But researchers now say there’s no evidence to support that idea. While hobos and yellow sacs do bite occasionally, you’re unlikely to experience symptoms beyond minor pain, swelling, and redness.
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
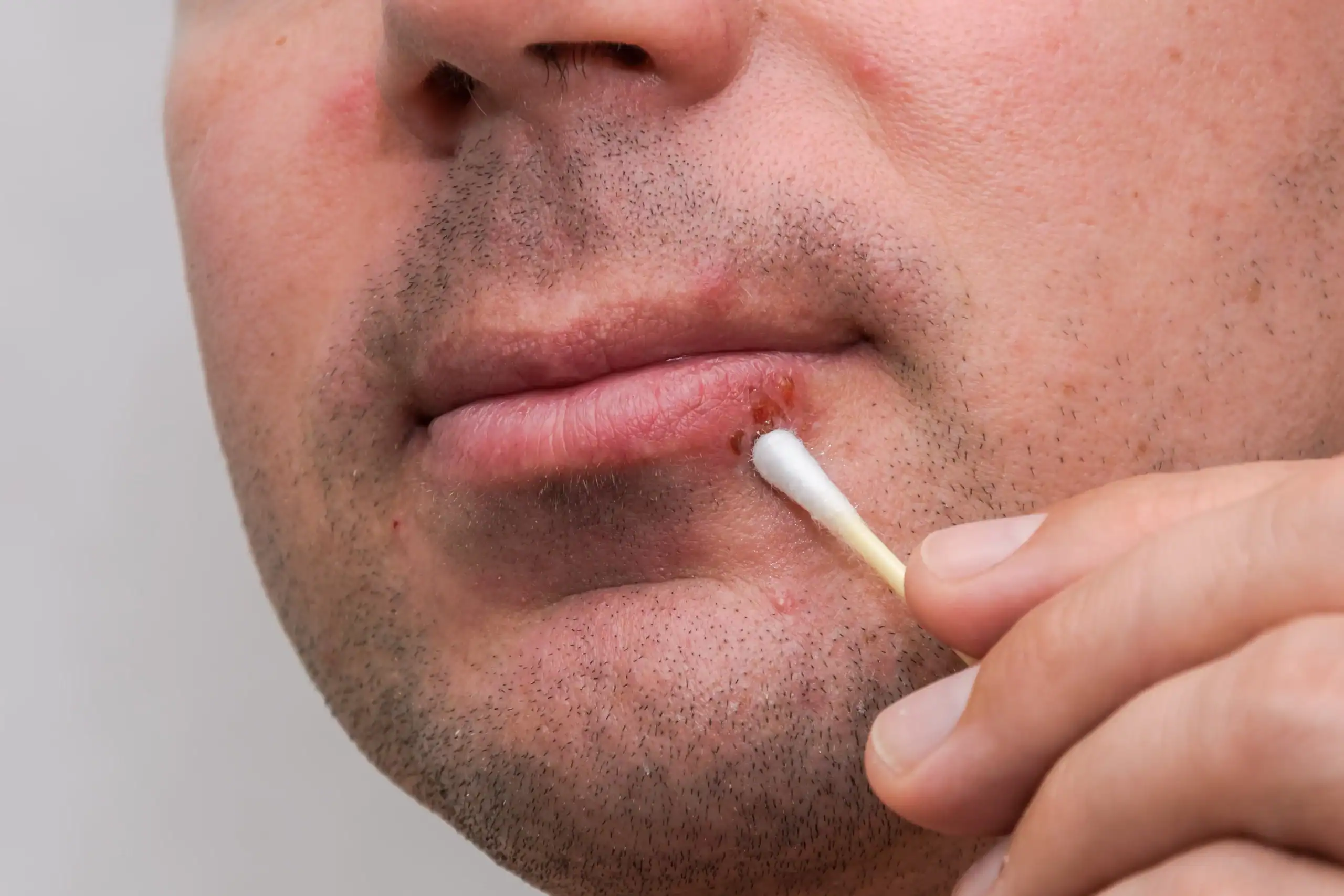
Are Cold Sores Contagious? Here’s What to Know
Medical Review By: Camila Yepes, PA-C
Cold sores, aka fever blisters, are caused by the herpes simplex virus (HSV) — not by colds or fevers. But like colds, they are very contagious. You can spread HSV at any point from the first warning tingle up until the cold sore scab has completely disappeared. It’s even theoretically possible to spread the virus when you don’t have a cold sore.
Read on to learn more about cold sores and how to stop the spread.
What causes cold sores?
Oral herpes infections are spread from person to person, usually through direct contact — for example, through kissing or oral sex. They can also be spread by sharing personal items such as drinking glasses or lip balm.
Of course, you can develop a cold sore without coming into contact with someone who has one. That’s because most adults have already been infected with HSV, typically during childhood, and the virus remains in the body, hiding in nerve cells, for life.
Certain triggers can “wake up” the virus, resulting in a cold sore. These include sun exposure, cold wind, cracked lips, hormonal changes during menstruation or pregnancy, emotional stress, surgery, and anything that taxes your immune system, such as the common cold or another illness.
Cold sore stages
Stage 1: You’ll feel tingling, itching, or burning somewhere around your mouth or at the base of your nose. You’re already contagious at this stage (called the prodome stage). This is the time to apply an over-the-counter product such as Abreva or take an oral antiviral medication such as valacyclovir if your doctor has prescribed one. Valacyclovir is highly effective at shortening outbreaks when taken within the first 24 hours of symptoms.
Stage 2: After a day or two of tingling, blisters filled with clear liquid develop and the skin under and around them reddens. Cold sores spread easily at this stage. Do not break the blisters.
Stage 3: A few days later, usually on day four, the blisters break on their own, creating an open sore. This stage, which doctors call the ulcer or weeping stage, is when a cold sore is the most contagious.
Stage 4: The sore starts to dry out and scab over. It may crack or bleed. The sore is still contagious.
Stage 5: The sore begins to scab over. When the scab falls off, the area may look pink or red for a few days. The sore is no longer contagious once the skin heals.
Stopping the spread
Cold sores can spread through saliva and through skin-to-skin contact. To avoid infecting other people, follow these tips during every stage of a cold sore.
Avoid touching the area. If you must scratch when it itches, wash your hands thoroughly afterward. Apply any topical treatments with a cotton swab, not your finger. Don’t pick at the scab (this will only prolong the healing process).
Don’t share any personal items. This includes food, drinks, eating utensils, straws, toothbrushes, razors, lip balm, petroleum jelly and any cold sore cream or ointment you use.
Don’t kiss anyone or nuzzle your baby. Kissing your baby while you have a cold sore is dangerous because the virus is far more severe in infants, who don’t have a fully developed immune system. You should also avoid close contact with anyone who has a weakened immune system, and anyone who has eczema. People with eczema are at risk of a potentially serious skin infection called eczema herpeticum.
Refrain from oral sex. Genital herpes is typically caused by a different strain of HSV (HSV-2), but it is possible for your partner to develop “oral herpes” (HSV-1) on their genitals from exposure to a cold sore on your mouth.
The best way to avoid spreading cold sores is to avoid getting them in the first place. While you have limited control over some common triggers, you can lower your risk of outbreaks caused by sun exposure by wearing lip balm with an SPF of at least 30.
If you get cold sores several times a year, ask your Water's Edge dermatologist about a prescription for an antiviral medicine to take at the first sign of an outbreak. People who get cold sores many times a year may be prescribed a low-dose antiviral medication to take daily in order to help prevent outbreaks. Taking supplements of the amino acid lysine coupled with avoiding foods high in the amino acid arginine (notably, nuts and seeds) may help, too.
Get Cold Sore Treatment, Contact Our Dermatologists Today!
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org and many other outlets.
Medical Review By: Camila Yepes, PA-C
Why Diabetes Can Cause Dry, Itchy Skin
Medical review by Richard Levine, MD
If you have diabetes, you may know it can affect your heart, kidneys and nerves, particularly if the disease is poorly controlled. But did you know it can also cause dry, itchy skin?
An estimated 79% of people who have diabetes mellitus, the most common form, experience skin issues such as dryness, itching and infections. These can develop at any point during the course of the disease. In some cases, they may even be the first sign that a person has diabetes.
The connection between diabetes and itchy skin
Diabetes can make the body lose too much fluid through urination and evaporation through the skin. The result: dry, itchy skin that can be bothersome and sometimes uncomfortable.
Itching, especially in the lower legs and feet, can also be caused by poor circulation, which is common with diabetes. Some people experience a skin reaction to their diabetes medication or insulin injections.
In addition, itching can be brought on by diabetes complications including nerve damage, kidney disease and liver disease. Certain medications for other health problems common in people with diabetes, such as high blood pressure and high cholesterol, can make the skin itchy, too.
Scientists suspect that those with type 2 diabetes may be vulnerable to itchy skin (and also skin infections) for yet another reason: Their skin’s barrier function is impaired. Exactly how and why this happens is still being studied.
Diabetes and skin infections
Studies suggest that more than half of people with diabetes will develop a skin infection at some point.
Scratching and dryness can create cracks that let bacteria in. It’s not unusual for people with diabetes to develop bacterial infections such as folliculitis, boils and carbuncles.
Itchy fungal infections are also more likely in people with diabetes, possibly due to high blood sugar. Infections caused by the yeast-like fungus Candida albicans often crop up in areas with moist folds, such as the armpits, groin area, under the breasts and between the fingers and toes. Infections caused by mold-like fungi called dermatophytes include ringworm, jock itch and athlete’s foot.
Skin care tips for people with diabetes
If you have diabetes, good skin care is an important part of managing your disease. These tips can help keep your skin soft, calm and infection free.
Keep your blood sugar under control. Follow your doctor’s plan to manage your blood sugar levels. When your diabetes is well managed, your whole body, including your skin, benefits.
Take lukewarm showers and use a moisturizing soap. Hot baths and showers dry out the skin. Dry off well after your shower, especially under the arms and breasts and between the legs and toes.
Use a gentle moisturizer. A cream or ointment is preferable to a lotion since lotions contain more water. Ask your dermatologist for a recommendation. Don’t moisture between your toes.
Avoid scratching if you can. Scratching can create openings in the skin that let in bacteria.
Consider using a humidifier in winter. Dry air can make dry skin worse.
Wash minor cuts right away with mild soap and water. Talk to your doctor about using an antibiotic cream or ointment. Cover the cut with a bandage. Deep cuts require professional treatment.
Practice good foot care. Examine your feet daily. Look for any cuts, blisters or sores. Unless the wound is minor and heals on its own, see a doctor right away. When you cut your toenails, cut them straight across and not too short. Smooth the corners with a nail file if necessary.
Your dermatologist can help
A dermatologist can get to the bottom of why your skin is itching and offer treatment suggestions. He or she can also diagnose and treat other diabetes-related skin problems that don’t involve itching.
Prompt treatment of skin problems is especially important when you have diabetes. See a dermatologist or other doctor if you have signs of an infection. A bacterial infection may cause redness, pain, swelling and oozing. Fungal infections typically itch. The skin may also be red, scaly, swollen, or blistered.
If you develop severe itching, consult your dermatologist or diabetes doctor without delay. It could be a sign that your diabetes treatment plan isn’t working.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
Hot Tips for Buying Skincare Products
Water’s Edge Dermatology is celebrating 20 years as Florida’s premiere skincare provider, and if we’ve learned anything over the years when it comes to skincare products, it’s how to help our valued patients buy what’s best for them and what to consider regarding skincare products on the internet. So, the Water’s Edge team has compiled a tips list based on our two decades of experience. Here’s to taking great care of your birthday suit!
Tip #1: Don’t purchase skincare products on the internet from off-brand sites
Quality skincare products can be damaged if they are not stored and shipped properly. Exposure to heat or cold can negatively affect the chemical ingredients, such as delicate antioxidants, that were developed to help your skin look and feel more youthful. Even if they have a top name-brand label on them, products sold on the internet could be past their expiration date. You’ll have no way of knowing that when you shell out your hard-earned cash. Once you receive your product, if you find that you are not happy with it, making a return and getting your money back can be a big challenge.
Tip #2: Beware of counterfeit products
The fake skincare product market is alive and well, just like fake designer handbags and clothing. Because these products often contain cheaper, less effective and sometimes dangerous ingredients, counterfeit products can damage your skin. Price often will tell you if a product is counterfeit. Many fake skincare products are offered at a very low price, enticing buyers who want deep discounts on brand cosmetic products. The truth is that quality skincare products rarely go on sale for more than 20 percent below their retail price. To ensure that you are getting the authentic product, purchase directly from the brand retailer, and look for legitimate sales from that retailer.
Tip #3: Get recommendations from a dermatologist, not retail store clerks
Sales associates at a department store cosmetics counter are paid to sell you their product line. Your dermatologist is committed to helping you get the right product that will deliver the results you want. With years of medical training and experience in skin science, your dermatologist can guide you to the best skincare products for your skin and your goals.
You’ll be able to test a product at your dermatology office before you purchase it, saving you money in the long run. It’s important to remember that not all skincare products – in spite of their great reviews – are right for every individual and skin type. Those with oily skin may fare better with serums rather than heavy moisturizers. People with dry skin typically need added moisture in their skincare products. Making an appointment with your dermatologist is the best place to start.
Your skin is an important asset. It’s one of the first things people notice about you. When you take the time to get the right information and advice backed by medicine and science, your skin will know it and show it. It’s why we practice the Art, Heart and Science of skincare.
Click here to learn more about Water’s Edge MediSpa & Aesthetic Skin Care Services.
Notes from a Veteran Dermatology Nurse: Getting Started & Sticking With It
A special guest post, written by veteran dermatology nurse Lisa Cheek.
Last week’s observance of National Nurses Week got me thinking and reminiscing. As a veteran dermatology nurse (16 years!), I’ve got plenty of stories, and memories. Some of them good, some of them bad, some happy, some sad.
You may wonder how a young woman gets into dermatology nursing in the first place – and how and why she sticks with it. Allow me to share my story.
I was living in a small Indiana town called Kokomo, going to school for graphic design. A friend working in a dermatologist’s office tells me one day just how busy the office is, that they need help. She asks if I’m interested.
I needed a job and thought to myself, “How hard can it be to treat acne?!” Little did I know how little I really knew about skin, skincare, and dermatology. It didn’t take long after plunging in for me to realize; I had no idea what I was getting myself into.
The jargon and terminology, the difficult diagnoses, the multitude of symptoms, treatments, fluids, smells and more… were just the beginning.
On my very first day, I experienced the smell of cauterization (burning skin) while observing a procedure. Wasn’t sure I was going to make it through the day and remember it like it was yesterday. Could hardly eat my lunch I was so haunted by the smell. But kept telling myself we were helping people… and managed to get past it and move forward.
Onto my next early hurdle. Cysts. If you haven’t seen and smelled what’s sometimes inside one of these, you don’t know what you’re missing – and you don’t want to. Didn't help that the nurse practitioner working with me seemed to express deliver cyst cases my way. Sometimes they ruptured while I was simply numbing the surrounding skin. It seemed like cyst goo followed me around the office.
Then there’s the unique language of dermatology. It was daunting and difficult to get accustomed to. And it kept going into far more depth and detail than I ever imagined it could or would.
To be honest… I really did think dermatology would be mostly acne problems. It didn’t take long to see firsthand just how far off base I was. I had no idea dermatology nurses did so much case-by-case documentation either – the lion’s share, and then some.
There were also aspects of dermatology care I wasn’t even aware of when I started. I had no clue that cosmetic treatments and aesthetic medicine were involved!
Back in the day, it felt like the doctor had to chase some patients around just to inject the filler they’d come to be treated with. Because so unlike today’s treatments, injections involved a very large needle, and it could be painful. Frankly, it was sometimes hard to watch. Thank goodness for the genius who decided we should start adding numbing, painkilling lidocaine to the mix!
I had a lot to learn. A lot. Just like any dermatology nurse, even the ones coming out of nursing school with knowledge and skills I didn’t have when I started. But more so. I set about getting up to speed as quickly as I could, with help.
The dermatologist I was working with would quiz me about each patient’s diagnosis, sometimes right there in the exam room with the patient! It made me nervous and uncomfortable in the beginning. I thought he was just being a pain and trying to make me look dumb.
In fact, he was helping me learn, and grow. It worked. I was like a sponge. I couldn’t get enough of it. I would take notes every day, then go home to study and research dermatology conditions and cases even further.
My compassion and caring for patients and their problems combined with my curiosity and thirst for knowledge. Together, they fueled my professional growth. Developing those habits early on helped make me a better-and-better nurse. They still do. Even 16 years later, I’m still learning about new diagnoses and treatments, still seeing cases I’ve never seen before.
And I am proud of the nurse I have become.
There’s nothing to compare with the gratitude of someone whose suffering has been eased, much less entirely eliminated. To play some small part in that is a great reward.
At the end of the day, that’s what keeps me and most dermatology nurses going, seeing how much we can help people in great distress. That, and for me, the pleasure of sharing my experiences and knowledge with others. Which I look forward to doing more of with all of you, from time to time.
Shingles, Seniors & Medicare Coverage
Chances are, most young people have little idea of what Shingles is, much less how doctors treat it, or Medicare covers it. But the skin disease that’s scourge to so many millions of seniors has its roots in childhood. Chickenpox, in fact.
Back in the day as they say, there wasn’t a vaccine preventing most kids from contracting the varicella-zoster virus that causes chickenpox. On the other hand, children traditionally experience a significantly milder version of the virus than adults do. In fact, many parents have breathed a sigh of relief when their little ones presented with the telltale red, itchy spots; relieved to get it over and done with.
Well, there’s over and done with. And then there’s the difficult reality that if you did have chickenpox as a child, your body still hosts the varicella-zoster virus. It hides out in your nerve tissue near the spinal cord, waiting for years. Then, when the immune system of some unsuspecting senior dips low enough, it can reactivate as shingles.
So, What’s Shingles & What Do You Do About It?
While chickenpox is generally not feared, shingles is another story. While not a life-threatening condition, it remains a skin disease dreaded by at-risk seniors. Dreaded, because as anyone who’s suffered through it can tell you, shingles can be extremely painful. Think itchy red rash, fluid-filled blisters, numbness and/or burning in the skin.
The good news is, shingles is preventable for more than 9 out of 10 people, with a new, more effective-than-ever shingles vaccine. And if you do contract shingles, more good news is that it usually goes away on its own after 2-3 weeks.
Getting to your dermatologist’s office in the first 2-3 days of a shingles outbreak can be a huge help. This allows common treatments such as oral antiviral medication, pain relievers and possibly corticosteroids to provide real relief before things get out of hand.
If you’re over 50, certainly if you’re over 60, the shingles vaccine is highly recommended. Good alternative to all the medical care and treatment you’ll need if you do get it. Which raises a question important to so many senior healthcare patients/consumers:
What Will Medicare Cover When It Comes To Shingles?
Medicare Part A covers hospital benefits and Part B covers outpatient benefits. If you develop shingles, your visits to the dermatologist for diagnosis and treatments are covered by Medicare Part B.
After you meet your annual Medicare Part B deductible ($183 in 2018), Medicare pays 80% of the cost of your doctor visits and related lab tests. You’re responsible for the other 20%, unless you purchase “Medigap” coverage to help limit out-of-pocket costs for such deductibles and copayments.
While Part B covers your doctor’s visits related to shingles, the medications for treating and/or preventing shingles are generally going to fall under Medicare Part D coverage.
How can Medicare Part D Drug Coverage help with Shingles?
Beneficiaries purchase Part D policies from private insurance companies. Some Part D companies include the varicella-zoster vaccine in their drug formularies. When considering aPart D policy, you’ll want to check on that. While this vaccine might cost $200 or more without coverage, beneficiaries with Part D often pay around half that amount when they use their coverage.
For individuals with an active case of shingles, Part D plans should cover a number of medications which help control the infection. Having Part D coverage means you’ll only be responsible for your plan’s required copayment for any of these covered medications instead of full cost.
The most common and least expensive medication is Acyclovir. This medication has been around since the 1980’s and is a generic form of the brand-name antiviral medication called Zovirax.
Your doctor may also prescribe valacyclovir or famciclovir, which are two newer forms of antivirals that may treat shingles more rapidly than acyclovir. That means it’s worth checking for Part D coverage of these drugs too.
Do take note though; many seniors with Medicare Part D Drug coverage still have to confront the infamous Medicare Part D “Donut Hole” (till 2020). This is an actual reduction in coverage that kicks in for seniors whose drug costs exceed a prescribed monthly and/or annual limit.
For the time being, seniors and their loved ones need to take this and all the other above information into consideration when evaluating the costs and coverages for prevention or treatment of shingles.
Understanding Adult Acne
Acne vulgaris is an inflammatory skin condition that affects around 50 million Americans. Acne is typically associated with young adulthood. Indeed, in the throes of pubescence, angry, hormonal teenagers are expected to have unsightly acne. But come adulthood, your acne will disappear and your skin will become surreptitiously clear, right?
Wrong.
While acne typically begins in young adulthood, adults are susceptible to developing acne, too. Approximately 85% of people develop acne at some point in their lifetime; from your early 20s to your late 50s, acne in adults is developed for a number of reasons.
So why do adults suffer from acne? In truth, it could be for a number of reasons, but here are the two most common:
Hormones
Stress or changes in your hormone levels from menopause, menstruation, or birth control can incite acne for adult women.
Medications
Certain medications, such as antiseizure drugs, lithium, and corticosteroids. In addition to medication, adult acne can also be a symptom of other, more serious conditions.
Talk to your local dermatologist to better determine the cause of your adult acne.
Combating Adult Acne
Dealing with adult acne can have grave social and personal consequences regarding positivity and self-esteem. In tandem with a great dermatology clinic, the best skin treatment for acne is relatively simple and can be followed by anyone:
- Wash your face every day, but no more than twice a day.
- When washing your face, use warm water and a gentle cleanser. Avoid harsh exfoliators and extreme temperatures.
- Use a gentle washcloth or baby cloth when washing your face.
- When drying your face, pat it dry, as to avoid irritation.
Seek Help
As far as over the counter solutions go, look for gentle cleansers that won't strip your skin of essential oils. When looking for the best skin care treatments over the counter, look for creams with salicylic acid or retinoid, as well as benzoyl peroxide.
Above all, it is recommended to seek the help of a dermatologist clinic or a dermatologist online for help. Adult acne could be indicative of a more serious problem. For the best treatment possible, as well as the best medications, look to a dermatologist for help.
Adult Dermatology: Changes in Aging Skin
We won’t stay young forever, but that doesn’t mean our skin can’t continue to look its best. Adult skin changes as it ages, and some of these changes are more obvious than others. The trick to keeping your skin looking healthy and young for longer is prevention. Your Water’s Edge adult dermatologist can help you stall some of the side effects of age. Here are the five most-common effects of aging skin:
- Skin gets drier. Your skin produces fewer moisturizing oils as you age, so it’s important to protect your skin from losing moisture to wind, hot baths or the sun.
- Your skin begins to thin. Adult skin thins as you lose some of the fatty layer below your skin. Your skin cells regenerate more slowly and your collagen and elastin levels decrease as you age.
- Skin begins to sag. As your skin thins and you experience lymphatic drainage, gravity begins to pull on your skin. The decreasing levels of collagen and estrogen mean there is less structure for your skin as well.
- Age spots develop on exposed skin. Age spots are areas approximately the size of freckles. They are caused by melanin overproduction due to sun exposure.
- Wrinkles form and deepen. The most common causes of wrinkles are sun exposure, muscle and skin movement from facial expressions, slower skin cell regeneration and less collagen production. These are made more prominent by sagging skin.
Your skin is an indicator of your health, so keep it looking as good as you feel. Your adult dermatologist can treat dry and sagging skin, wrinkles and age spots. Make your appointment with a Water’s Edge dermatologist today and get serious medicine for your skin.
Top 5 Reasons to Consider Juvederm Voluma
Some signs of aging can begin to appear when women are in their mid-30s, such as cheeks losing volume or deepening under-eye circles. Fortunately, there are several ways to keep aging skin from detracting from your natural beauty, such as fillers like Juvederm Voluma. Here are the five top reasons why you should consider Juvederm Voluma when you decide to get a filler treatment.
- Restores fullness to your face by filling both fine and deep lines for a natural appearance.
- Diminishes any scars you may have accumulated over the years.
- Produces immediate results, meaning your face looks as youthful as you feel by the time you leave the office, and no downtime is required.
- Treatment is completed in one visit, so you don’t have to worry about scheduling multiple appointments.
- Results last for months, and when you combine certain fillers, your results can last between three months to a full year.
Juvederm is a smooth gel made from hyaluronic acid, which occurs in your skin naturally. Your Water’s Edge adult dermatologist can use the combination of Juvederm Voluma to smooth your skin and add volume and hydration. It is the latest facial filler option available and it is the only filler approved by the U.S. Food and Drug Administration.
Make an appointment with your Water’s Edge Dermatologist for a consultation about your filler treatment today. You can like us on Facebook to find more tips about skin care and our serious medicine for your skin.
Do You Need a Dermatologist?
There are a number of skin conditions that a person may contract over the course of their lives, from acne, which affects nearly 85% of people at some point during their lifetime, or skin cancer, which will affect an estimated one in five Americans. Fortunately, for the skin conditions that require clinical help, dermatologist specialists offer a number of treatment options for a wide array of skin problems. These range from aesthetic issues, like varicose vein laser treatments, to serious medical problems, such as melanoma and other forms of skin cancer. Can a dermatologist treat your skin condition? Read on to find out.
Research shows that an estimated 7,575 dermatologist clinics in the United States offering treatments for skin problems. One of the most common disorders these clinics treat is acne, which affects an estimated 40 million to 50 million Americans. Many of the people affected by this condition are teenagers: by their mid-teens, more than 40% of adolescents will have acne or acne scarring. However, acne occur at almost any age, and as a result, there are a number of different acne treatment products and methods available. This includes everything from common topical products or even laser acne treatments. A skin care specialist will prescribe a treatment regimen based on the individual needs of the patients that will use different products and combinations of treatments to best rid the patient of their acne.
Skin care specialists also treat a variety of other skin issues, including those which develop in reaction to other, more serious problems in the body. For example, candida infections often form in reaction to a weakened immune system caused by cancer, HIV, and other diseases. It then spreads to various parts of the body, including the lungs, liver and skin. Similarly, Kaposi's sarcoma is a skin condition characterized by dark or purplish lesions on the skin, which forms rarely as a genetic condition and more commonly by the weakened immune system caused by AIDS. Because KS lesions can spread quickly to other parts of the body, including the internal organs, it is important to treat the problem as soon as possible.
The average person will likely experience some form of skin problem over the course over their lives, whether it is as common as acne, as serious as skin cancer or melanoma, or merely an aesthetic concern, like varicose veins. Regardless of the problem, skin care specialists can help you achieve the beautiful, healthy skin you want. Contact a dermatologist today to discuss how they may be able to help you.