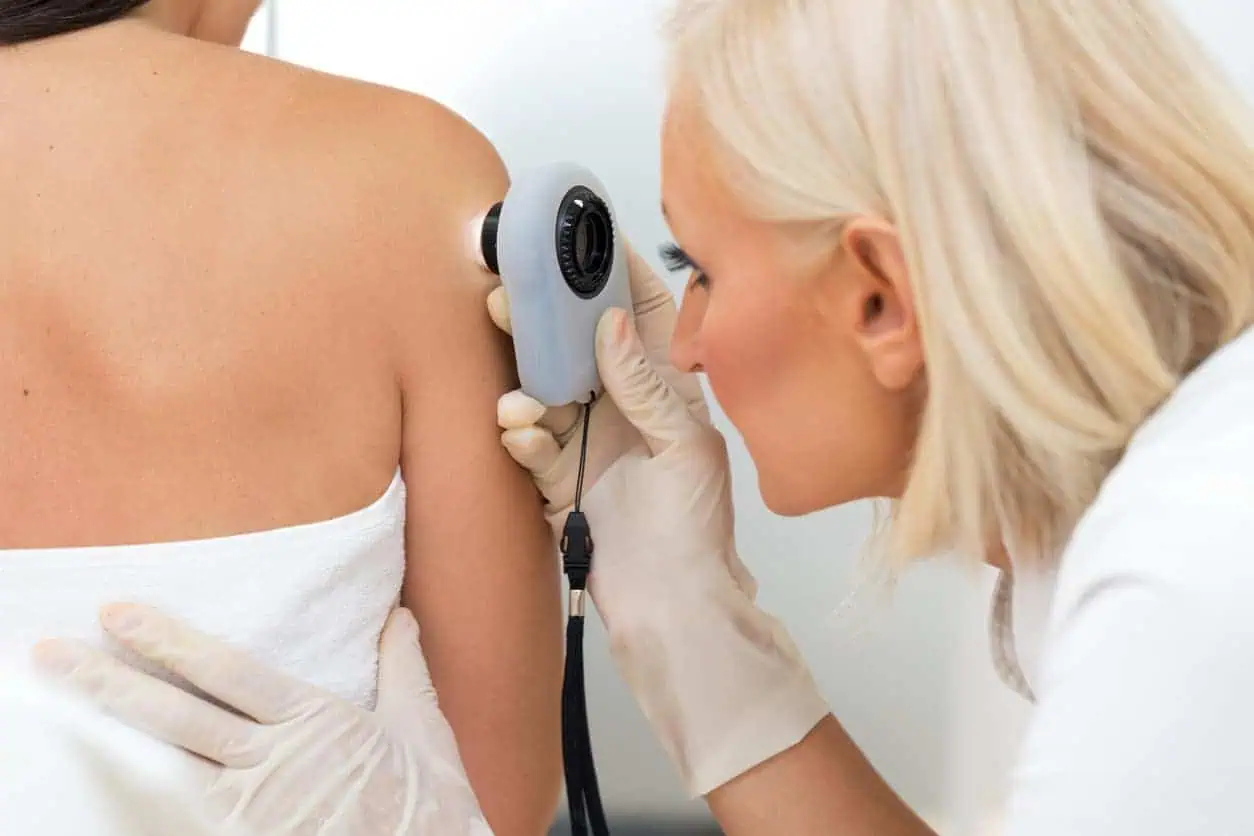
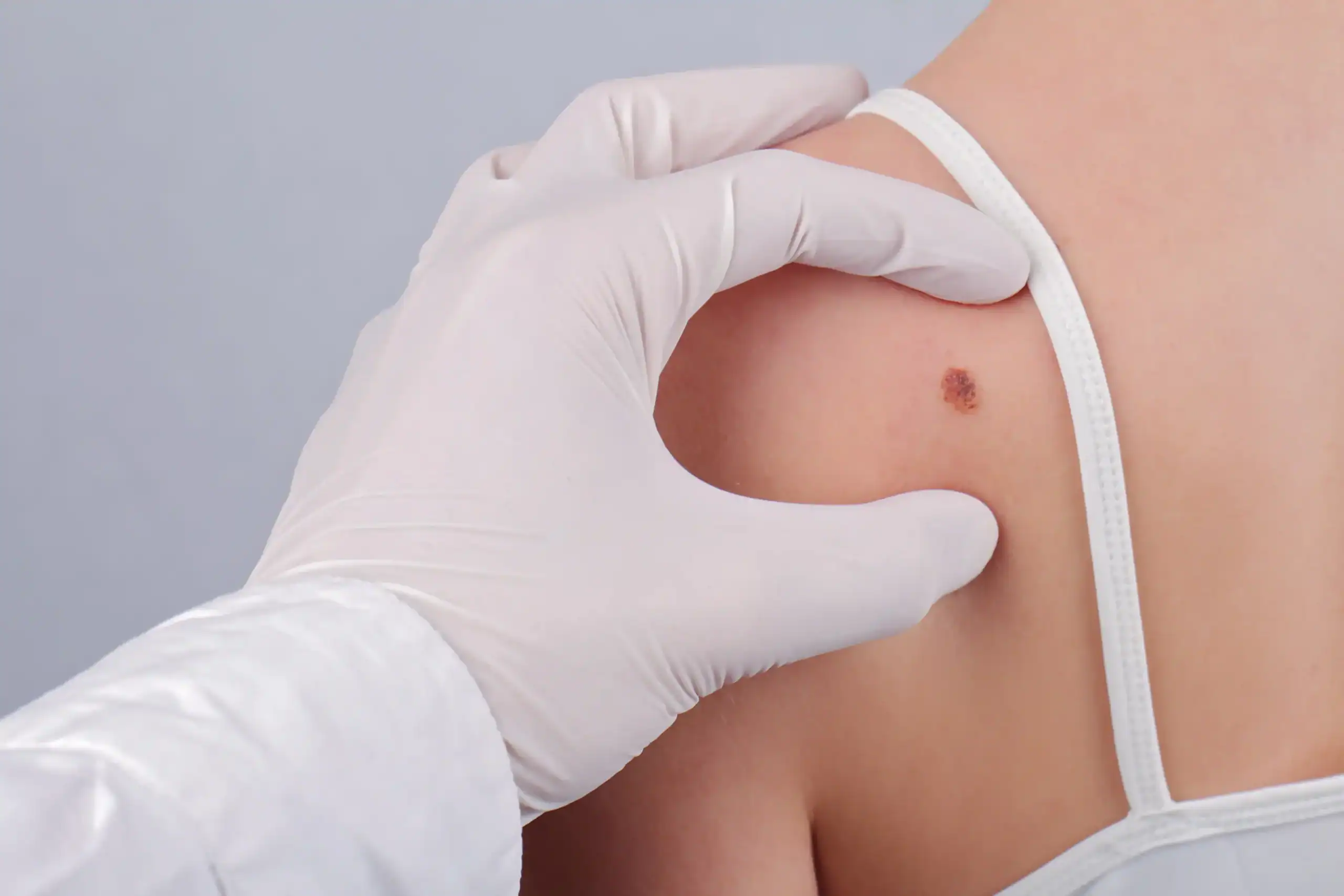
When to Worry About a Spider Bite
Medical Review By: Thomas Pham, MD
Spider bites are more common than you might think. Garden spiders that get trapped in clothing or under hair may bite two or three times before you flick them off or crush them by scratching. Dermatologists sometimes call these bites “breakfast, lunch, and dinner.”
Fortunately, when it comes to spider bites, the ick factor is almost always worse than the bite. While nearly all spiders produce venom, it’s rarely strong enough to harm humans. Plus, most spiders’ fangs are too short to penetrate human skin.
Bites that produce mild pain or itching can usually be treated with over-the-counter hydrocortisone cream or ointment, cold compresses, and an oral antihistamine if needed to help with itching or swelling.
If you’re unlucky, however, you might encounter one of the two types of spiders in the United States that can seriously harm humans: the black widow and the brown recluse. While they’re not aggressive, they do bite in some circumstances, and there’s a chance you may need emergency treatment if you are bitten.
If possible, take a photo of the spider to help your doctor diagnose the bite and choose a course of treatment.
Black widow spiders
What they look like
Black widows have an almost spherical abdomen and are about half an inch long.
Southern black widow spiders are black with a red hourglass pattern on the underside of the body (females) or red and white markings on the sides of the body (males). In Northern black widows, the hourglass pattern is broken, and there may be a row of red spots on the back and diagonal whitish markings on the side (females). Male Northern black widows usually have faint red and white spots on the underside of the body.
What to know
Black widows can be found anywhere in the United States but are more common in the South and West.
While male black widow spiders don’t bite humans, females can and will attack to defend themselves if you disturb them, especially if they’re in their web protecting their eggs.
You’re most likely to run into a black widow’s web in dark and undisturbed areas, such as woodpiles, eaves, fences, and water meter boxes. When indoors, black widows usually build their webs in cluttered areas, such as a garage or basement.
Spider Bite Symptoms and Treatment
Black widow bites cause a sharp, pinprick-like pain. In many cases, reactions are relatively mild and limited to redness and swelling of the bite area. (You may also notice two tiny red spots that are actually tiny fang marks.) These symptoms appear 15 to 60 minutes after you’re bitten and can be treated at home with cold compresses, over-the-counter pain relievers, elevation (if the bite is on your arm or leg), antibiotic cream, or lotion.
Some people develop a severe reaction and experience signs and symptoms such as stiff and painful muscles, fever, chills, nausea, vomiting, difficulty breathing, weakness, tremors, headache, and belly or back pain. These may develop in as little as 15 minutes after the bite or several hours later. If you have a severe reaction, go to the emergency department or call 911.
Fatalities are rare. Elderly people and small children are more likely to have a severe, possibly life-threatening reaction.
Treatments for severe black widow bites include prescription pain relievers, muscle relaxants, and antivenom.
Brown recluse
What they look like
Brown recluse spiders are tan to dark brown with long legs. They often have a darker brown violin shaped-marking just behind their head.

What to know
Brown recluse spiders are typically found in Midwestern and Southern states. They truly are reclusive and would much rather avoid you than attack you. When they do bite, it’s usually because they were trapped against your skin and tried to defend themselves. This may happen if a brown recluse makes its way into your bedsheets, clothes, or shoes.
Brown recluses like to live under rocks, woodpiles, and debris. They’re also well adapted to living indoors, where they prefer dark areas such as basements, attics, closets, and cabinets.
Bite symptoms and treatment
If you’re bitten by a brown recluse, you may not notice right away because the bite is often painless or only mildly painful. In fact, you may never know you’ve been bitten. If symptoms do occur, they typically start three to eight hours after the bite and include redness, tenderness, and a sore at the site of the bite. Other possible symptoms include fever, chills, vomiting, muscle aches, and itching.
Severe symptoms such as extreme pain or trouble breathing require immediate medical attention. Bites in small children, elderly people, and those in poor health also require immediate medical attention.
Brown recluse bites usually heal within three weeks. However, in about 10% of cases, a bite can cause tissue death in the affected area. A skin ulcer or blister with a blue, purple or black center develops and may become infected.
Treatments for severe brown recluse bites include antibiotics, antihistamines, and steroids. Some victims need surgery to remove the damaged tissue around the wound.
At-home treatments for mild bites are the same as those for mild black widow bites.
Hobo and yellow sac spiders: Cause for concern?
These two types of spiders have a nasty reputation. It was once thought that their bites, like that of a brown recluse, could lead to tissue death. But researchers now say there’s no evidence to support that idea. While hobos and yellow sacs do bite occasionally, you’re unlikely to experience symptoms beyond minor pain, swelling, and redness.
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Are Cold Sores Contagious? Here’s What to Know
Medical Review By: Camila Yepes, PA-C
Cold sores, aka fever blisters, are caused by the herpes simplex virus (HSV) — not by colds or fevers. But like colds, they are very contagious. You can spread HSV at any point from the first warning tingle up until the cold sore scab has completely disappeared. It’s even theoretically possible to spread the virus when you don’t have a cold sore.
Read on to learn more about cold sores and how to stop the spread.
What causes cold sores?
Oral herpes infections are spread from person to person, usually through direct contact — for example, through kissing or oral sex. They can also be spread by sharing personal items such as drinking glasses or lip balm.
Of course, you can develop a cold sore without coming into contact with someone who has one. That’s because most adults have already been infected with HSV, typically during childhood, and the virus remains in the body, hiding in nerve cells, for life.
Certain triggers can “wake up” the virus, resulting in a cold sore. These include sun exposure, cold wind, cracked lips, hormonal changes during menstruation or pregnancy, emotional stress, surgery, and anything that taxes your immune system, such as the common cold or another illness.
Cold sore stages
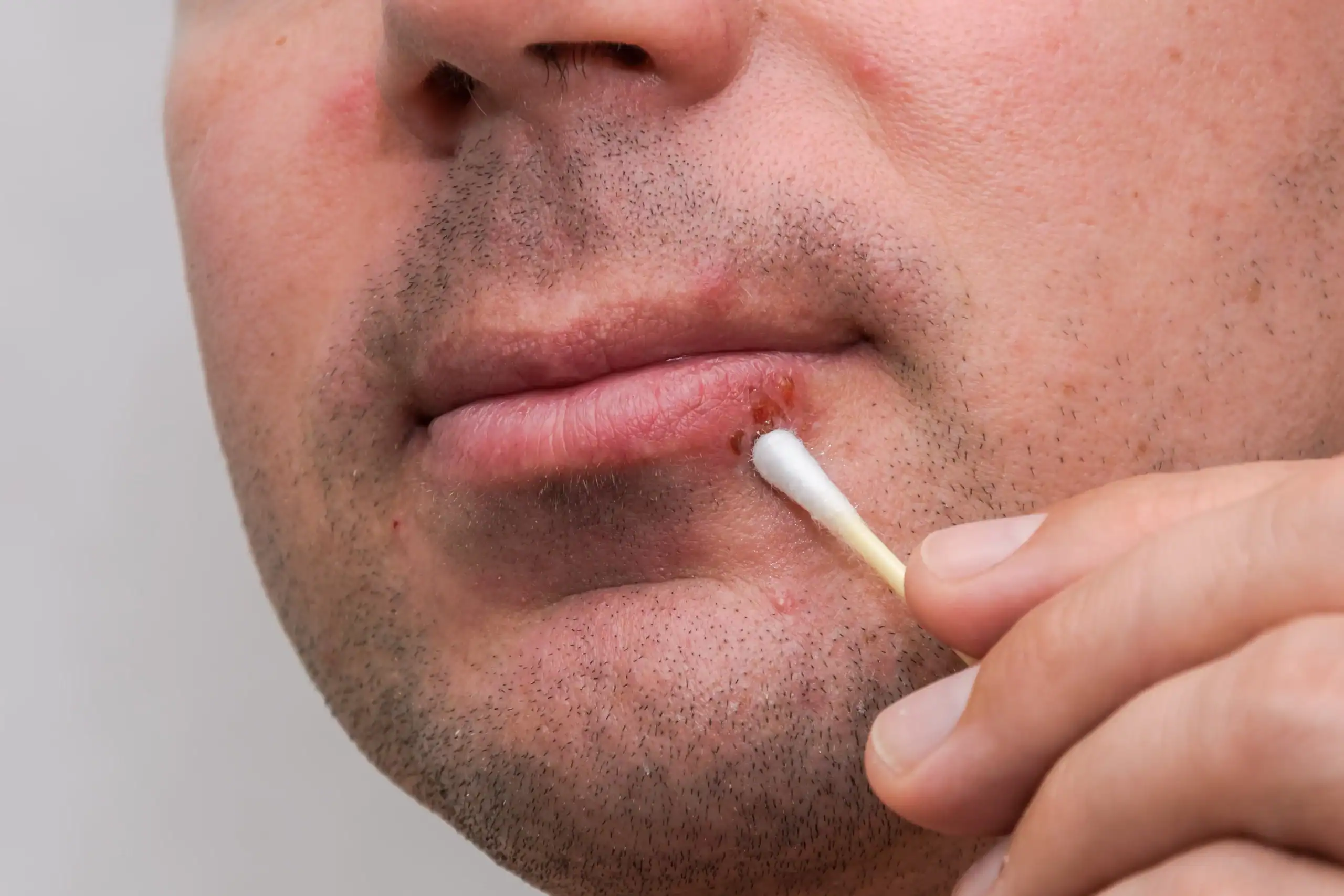
Stage 1: You’ll feel tingling, itching, or burning somewhere around your mouth or at the base of your nose. You’re already contagious at this stage (called the prodome stage). This is the time to apply an over-the-counter product such as Abreva or take an oral antiviral medication such as valacyclovir if your doctor has prescribed one. Valacyclovir is highly effective at shortening outbreaks when taken within the first 24 hours of symptoms.
Stage 2: After a day or two of tingling, blisters filled with clear liquid develop and the skin under and around them reddens. Cold sores spread easily at this stage. Do not break the blisters.
Stage 3: A few days later, usually on day four, the blisters break on their own, creating an open sore. This stage, which doctors call the ulcer or weeping stage, is when a cold sore is the most contagious.
Stage 4: The sore starts to dry out and scab over. It may crack or bleed. The sore is still contagious.
Stage 5: The sore begins to scab over. When the scab falls off, the area may look pink or red for a few days. The sore is no longer contagious once the skin heals.
Stopping the spread
Cold sores can spread through saliva and through skin-to-skin contact. To avoid infecting other people, follow these tips during every stage of a cold sore.
Avoid touching the area. If you must scratch when it itches, wash your hands thoroughly afterward. Apply any topical treatments with a cotton swab, not your finger. Don’t pick at the scab (this will only prolong the healing process).
Don’t share any personal items. This includes food, drinks, eating utensils, straws, toothbrushes, razors, lip balm, petroleum jelly and any cold sore cream or ointment you use.
Don’t kiss anyone or nuzzle your baby. Kissing your baby while you have a cold sore is dangerous because the virus is far more severe in infants, who don’t have a fully developed immune system. You should also avoid close contact with anyone who has a weakened immune system, and anyone who has eczema. People with eczema are at risk of a potentially serious skin infection called eczema herpeticum.
Refrain from oral sex. Genital herpes is typically caused by a different strain of HSV (HSV-2), but it is possible for your partner to develop “oral herpes” (HSV-1) on their genitals from exposure to a cold sore on your mouth.
The best way to avoid spreading cold sores is to avoid getting them in the first place. While you have limited control over some common triggers, you can lower your risk of outbreaks caused by sun exposure by wearing lip balm with an SPF of at least 30.
If you get cold sores several times a year, ask your Water's Edge dermatologist about a prescription for an antiviral medicine to take at the first sign of an outbreak. People who get cold sores many times a year may be prescribed a low-dose antiviral medication to take daily in order to help prevent outbreaks. Taking supplements of the amino acid lysine coupled with avoiding foods high in the amino acid arginine (notably, nuts and seeds) may help, too.
Get Cold Sore Treatment, Contact Our Dermatologists Today!
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org and many other outlets.
Medical Review By: Camila Yepes, PA-C
How Contagious Is Poison Ivy?

The short answer is no. Poison ivy rash, which is caused by an allergic reaction to oil in the plant, is not contagious. Even the fluid from poison ivy blisters is not contagious. Only direct contact with the plant’s oil, called urushiol, can trigger poison ivy rash.
But here’s the rub: Touching the plant isn't the only way to have direct contact with the oil.
Let’s say you got urushiol on your arm from touching the plant. If someone touches your arm before you wash off the oil, and before your skin absorbs it (which happens in a matter of minutes), they can get poison ivy rash. The same is true if you get the oil on your shirt or your shoe and someone else touches it, or touches a surface on which you placed an item. You can even get poison ivy rash from your dog or cat if the pet comes into contact with poison ivy and you touch the fur or hair.
That’s why it’s important to clean any items — and pets — that come into contact with poison ivy. Remove the clothing you were wearing when you were exposed and put it directly into the washing machine. Don’t drop the clothes on the rug or a chair first, and don’t let them touch the outside of the washing machine. If your shoes came into contact with the plant, clean the shoes and put the shoelaces in the wash. If your pet came into contact with poison ivy, shampoo him or her while wearing rubber gloves. As an extra precaution, you should wash the leash, too.
You should also wash other items that may have come into contact with the plant. That includes garden tools (and gloves), camping equipment, golf clubs, a bicycle you were riding and even jewelry you were wearing. You can wash them or remove the oil with rubbing alcohol.
Note, simply putting items aside to "air out" won’t do anything to prevent poison ivy rash, since urushiol can remain on surfaces for years.
Just as someone can get poison ivy rash if they touch your urushiol-contaminated skin, you can transfer it to other parts of your own body while the oil is still on your skin. Wash your exposed skin with soap and water as soon as possible after exposure. Rinse it with water if you don’t have access to soap, and wash with soap when you do. This also reduces the severity of the rash. Be sure to clean under your fingernails, where urushiol can hide.
Poison ivy rash is no fun, but if you’re smart about removing the urushiol from your body, your clothing, and anything else that may be contaminated with it, you can help prevent others from catching it — and avoid getting re-infected yourself later on.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
How to Heal Dry, Cracked Hands
Medical review by Ted Schiff, MD
Frequent hand-washing may be key to staying healthy, especially now and during cold and flu season, but it can really take a toll on your skin. That goes double in winter when colder temps and drier air conspire to zap skin of the natural oils that maintain moisture and provide a protective barrier. This can lead to dry, cracked hands.
"People think water is moisturizing, but it's actually drying — when it evaporates, it reduces skin’s natural oils," said Dr. Alissa O’Brien, a dermatologist at Water’s Edge Dermatology. "And if you're using hot water and harsh soap over and over throughout the day, it’s the perfect storm for drying out your skin."
Soap doesn’t discriminate between germs and the skin’s protective oils; neither does the alcohol in hand sanitizer. With frequent use, both can lead to dryness, irritation, and rash-like dermatitis or eczema. They can also lead to cracks in the skin which allow for the entry of germs like staph that make you more susceptible to skin infections.
To curb dry, cracked hands while practicing good hand hygiene, Dr. O’Brien offered this advice:
Wash your hands correctly
- Steer clear of harsh soap. A gentle moisturizing soap (Dr. O’Brien recommends Dove) will get the job done just as well as antibacterial soap, which is more drying and hasn’t proven to do a better job at preventing illness than regular soap. Of course, if your dermatologist has prescribed an anti-bacterial soap due to recurrent infections or other special circumstances, keep using it.
- Wash with lukewarm water. Lukewarm water is as effective as boiling water is at reducing germs. That’s because the goal of hand-washing isn’t to kill germs. "When you wash your hands, the germs get washed off," Dr. O’Brien explained. "They go down the drain." After washing, pat your skin dry. No need for vigorous rubbing, which can disrupt your skin barrier, lead to irritation and cause dry, cracked skin.
Moisturize regularly
"The best thing is literally to moisturize, moisturize, moisturize," said Dr. O’Brien. Moisture after every hand-washing. This will lock in moisture that got into your skin while washing and prevent evaporation that dries out the skin even more. For extra dry skin, apply an ointment at bedtime and then wear a pair of cotton gloves to help seal it in. Ointments can work extra well overnight when skin naturally loses more water.
Opt for ointment or cream moisturizer
Ointments work better than other types of moisturizers because they penetrate the skin better, according to Dr. O’Brien. "That’s why, when we prescribe topicals, we usually pick ointment forms — more medicine gets in that way." She recommends a product like Aquaphor Healing Ointment or a thin layer of petroleum jelly. "It sounds messy, but it’s extremely moisturizing and your hands are going to love it."
If an ointment is messier than you prefer, choose a cream moisturizer, which contains more oil than water-based lotions. Cream moisturizers are also more effective at trapping water in the skin and repairing its barrier function. Here are a few brands to try: Cetaphil, CeraVe, Eucerin, Gold Bond and Aveeno. Ingredients to search out include petrolatum and ceramides. Petrolatum helps block water loss from your skin; Ceramides are a type of lipid (fat) that helps form your skin’s barrier and increase hydration. Ceramides are a key ingredient in CeraVe products.
Be sure to stay away from lotions and moisturizers with fragrances and dyes. "Some dyes can irritate dry skin, so generally, I wouldn’t get the pink frilly one," said Dr. O’Brien.
Choose the right-hand sanitizer
Washing your hands is your best bet at removing all types of germs — even better than hand sanitizer. For instance, according to the Centers for Disease Control and Prevention, hand sanitizers don’t kill the stomach bug or a type of parasite that causes severe diarrhea. However, hand sanitizer is far better than nothing when you don’t have access to soap and water. If using a hand sanitizer, choose one that contains at least 60 percent alcohol and is enriched with an emollient like glycerin or vitamin E to help counteract the drying effect.
Wear gloves
If your hands are frequently immersed in water, such as when washing dishes or washing your car, wearing rubber or latex gloves can prevent the water from stripping away your skin’s oils. Gloves lined in cotton may be more comfortable on dry skin and are easier to put on and take off. Gloves are also recommended if you work with chemicals or plants, especially if you have sensitive skin that is prone to dryness.
Remember the sunscreen
It won’t be your main line of defense against dry, cracked hands, but because the sun can dry out your skin, sunscreen can help prevent further parching. "The sun not only makes dermatitis worse, but skin will be more prone to burning if it’s already irritated," said Dr. O’Brien. She likes CeraVe AM, a moisturizer with an SPF 30.
Written by Karyn Repinski is a Brooklyn, NY-based award-winning health and beauty writer.
Mohs Surgery for Skin Cancer Treatment
Updated May 19, 2020
The number of people developing skin cancer has been increasing for decades, to the point that skin cancer is now the most common cancer in the United States. Every day, more than 95,000 people are diagnosed with the disease, and one in five people will develop it in their lifetime.
Most cases are slow-growing nonmelanoma skin cancers like basal cell carcinoma (BCC) and squamous cell carcinoma (SCC).
Sun exposure and indoor tanning are the biggest risk factors for developing these skin cancers, and most of them form in areas that get the most sun, such as the head and neck. For people who develop BCC, SCC or some early melanomas, Mohs (pronounced “moes”) surgery is a very effective treatment, with a cure rate of up to 99 percent according to the Skin Cancer Foundation. The technique also provides the best cosmetic results of any skin cancer treatment.
What is Mohs surgery?
Mohs surgery, also known as Mohs micrographic surgery, is a technique invented by Dr. Frederic Mohs in the 1930s. Since being refined in the 1970s, it's become a mainstream treatment for skin cancers on the head and neck.
Mohs surgery differs from more routine skin cancer removal surgery in that it's done in stages. After the surgeon removes a layer of tissue, he or she examines it under a microscope to see whether it contains cancer cells. The process is repeated until no more cancer cells are found. This way, healthy tissue is spared, and the scar is minimized.
In Mohs surgery, all of the edges (called "margins") of the removed tissue are evaluated, which is not the case with conventional surgery according to Dr. Justin Platzer, a board-certified dermatologist at Water's Edge Dermatology. In conventional surgery, "[the sample] is cut differently, and it's only a small fraction of the margin that's evaluated, so you can miss tumors." By contrast, he said, "Mohs surgery allows for recurrence rates of tumors to be as low as 1 percent."
How does Mohs surgery work?
After injecting a local anesthetic to numb the skin, the surgeon removes the visible portion of the cancer along with a thin segment of surrounding skin and examines it under a microscope. Water's Edge Dermatology has an onsite pathology lab where samples are read immediately, and patients learn the results throughout the procedure. (Patients who undergo traditional skin cancer surgery can wait up to a week to get pathology results indicating whether or not the cancer is gone.)
If the sample contains cancer cells, the surgeon removes an additional layer of skin and sends it back to the lab. "If it’s positive [for skin cancer] in just one area, you’re able to take a little more of the skin only in that area, so it keeps the wound smaller," explained Dr. Platzer. This process is repeated until the margins are clean, meaning that no cancer cells remain. Most patients need only two rounds to remove all the cancerous tissue. The procedure lasts a few hours.
After the cancer is removed, the surgeon will decide whether and how to repair the wound. Smaller wounds are often left to heal on their own. Larger wounds may require stitches or even skin grafts. At Water's Edge Dermatology, surgical removal, lab evaluation and wound reconstruction are done in one visit in most cases. When patients walk out of the surgery, they have peace of mind knowing that their cancer is fully treated.
Who should have Mohs surgery?
Mohs surgery is typically recommended for nonmelanoma skin cancers in places where you want to preserve as much healthy tissue as possible to maintain maximum function and provide a good cosmetic result, such as around the eyes, ears, nose, mouth, hands, feet and genitals. Mohs is also used to treat cancers that:
- Returned after initial treatment
- Have a high risk of recurring
- Weren’t completely removed by other treatments
- Are large or aggressive
Will Mohs surgery leave a scar?
All surgical procedures have the potential to leave a scar. Mohs surgery often results in smaller, less noticeable scars than other skin cancer removal methods. Most scars improve in appearance naturally over time. "It takes a full year for scars to fully heal, but most scars from Mohs surgery start looking cosmetically acceptable after four to six weeks," said Dr. Platzer.
Is Mohs surgery covered by insurance?
Most insurance plans, including Medicare, cover Mohs surgery. Check with your insurance provider to confirm that Mohs is covered under your plan.
What should I do if I am concerned about possible skin cancer?
If you have a suspicious area on your skin, make an appointment to have it evaluated as soon as possible. If the dermatologist suspects skin cancer, he or she may perform a biopsy for further examination.
Don't think you’re too young for skin cancer. Nonmelanoma skin cancers typically appear after age 50, but even people in their 20s and 30s can develop them, according to Dr. Platzer. "It takes a while to develop a BCC or SCC, so people usually have to be pretty fair-skinned and have significant amounts of sun damage to have it when they're very young, but it's definitely possible to get it then."
To book an appointment for a skin evaluation, call (877-544-3880) or request one online. It’s a good idea to have your skin examined at least one a year. The sooner skin cancer is detected and treated, the better the chances of a complete cure, and the lower the chances of disfigurement.
Nail Problems and What to Do About Them
Did you know that our nails are essentially hardened skin cells? They might seem tough as, well, nails, but they can present their own unique health problems if they aren’t treated with care and attention.
What Exactly Are Nails?
We want nails to look strong and healthy, serve as an onboard toolset of sorts and protect our fingers and toes. But what makes up a nail and how a nail grows is amazingly delicate.
Your nails are made up mostly of keratin, which is a protein found in the skin and hair. As nails grow out from the matrix – the hidden half-moon area under the cuticle – older cells in the nail are pushed forward and harden to form a visible nail that protects and supports tissues in our fingers and toes.
Common Nail Issues
Nail problems make up about 10% of all dermatological conditions. As we age, nails thicken and become more susceptible to issues such as fungal and bacterial infections. Often these are nothing to worry about, but some may signal disease. Here are some common nail issues:
- White Spots – Typically white spots in the nail are caused by mild trauma such as catching a finger in a door. Typically, the nail will grow out and the white spots will disappear. However, if you see several white spots that do not seem to grow out, those might be an indication of an infection or other medical condition that may need treatment.
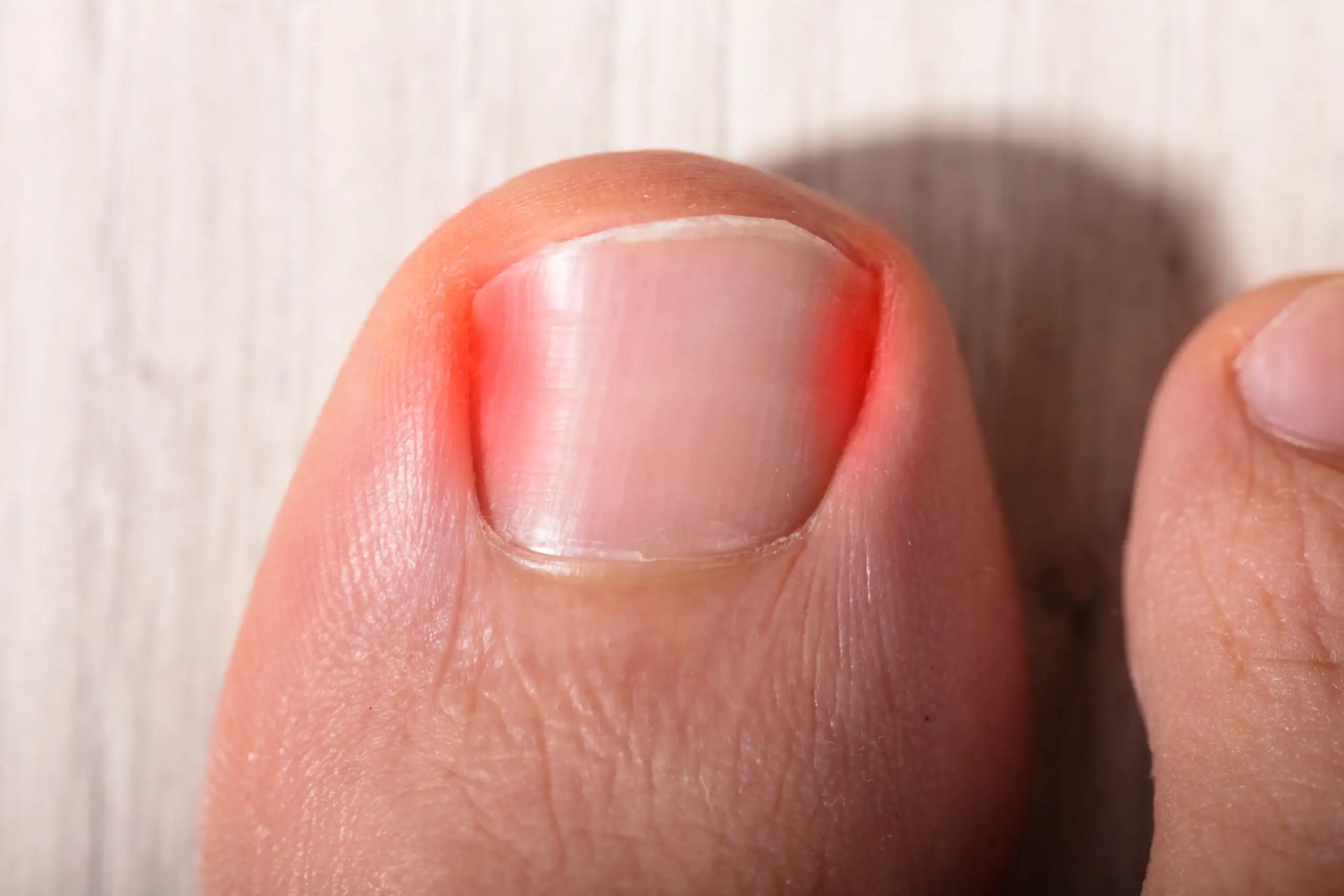
- Ingrown Nail – Most of us have had ingrown nails when the corner of the nail curves into the skin. Ingrown nails can be painful and sometimes get infected.
- Bacterial Infections – Redness, swelling and pain of the skin around the nails can be signs of a bacterial infection. Sometimes the nail may appear green. If you have your hands in water or the skin around the nails is exposed to chemicals on a regular basis, you might be susceptible to developing a bacterial infection.
- Nail fungus – This is a common condition that typically begins as a white or yellow spot under the tip of the nail. The nail may become discolored, thickened, misshaped and maybe even painful. If you see any of these symptoms, make an appointment with your Water’s Edge dermatologist.
- Dark Spots – If dark spots or streaks appear on any nail and you know it’s not because of an injury, see your practitioner. Dark spots or streaks on a nail could be signs of melanoma – the deadliest form of skin cancer. Be sure to get checked out right away.
Tips to Keep Nails Healthy
Practicing good nail habits is key to keeping them healthy. Water’s Edge recommends these tips:
- Keep nails clean and dry to help prevent bacteria, viruses or fungus from collecting under the nail.
- Cut nails straight across, rounding them slightly at the tips for maximum strength.
- Keep nails shaped and free of snags.
- Avoid biting fingernails and do not remove the cuticle.
- Trim toenails regularly to keep them short.
- Soak your feet in warm salt water for 5 to 10 minutes if toenails are thick and difficult to cut. This softens the nails and makes them easier to trim.
- Avoid digging out ingrown toenails, especially if they are infected or sore. See your practitioner for treatment.
- Wear shoes that fit correctly and alternate your shoes so you are not wearing the same shoes every day.
- If you see changes in your nails, such as swelling or pain, see your Water’s Edge provider.
- If you have diabetes or poor circulation, watch your nails carefully. See your Water’s Edge provider at the first sign of a problem.
Your nails can reveal a lot about your health, and changes in nails can signal disease or a medical issue. If you notice any issues or changes in your nails, make an appointment with your Water's Edge provider or call 877-900-3223 .
Time for Your Child’s Summer Skin Check
With kids out of school, it’s time for fun, sun and a lot of activities. It’s also time to schedule a summer skin check and stock up on sunscreen!
At Water’s Edge Dermatology, we are experts in spotting and treating all kinds of pediatric skin, hair and nail conditions, which is why we are encouraging a summer skin health screening for all children.
Potential Skin Issues in Children
Damage from pediatric skin cancer, acne, warts, eczema, rashes and sun damage could have a destructive impact on a child’s life if left undetected and untreated. That’s why we are sharing these quick facts about potential skin issues in children.
Skin Cancer: Skin cancer in children is on the rise. Though the most serious and deadly form of skin cancer – pediatric melanoma – represents only about 1% of new melanoma cases diagnosed each year in the U.S., malignant melanoma is the most common skin cancer in children and teens. It has increased about 2% each year since 1970. Fair-skinned, light-haired children are at the highest risk, but it’s a good idea for all children to get checked out annually.
Acne: Acne is the most common skin problem in the country. It often begins in puberty but can also affect adults in their 20s, 30s, 40s and even into their 50s. Most acne appears on the face, but it can also show up on the shoulders, upper arms, chest, neck and back. While acne is not curable, your Water’s Edge dermatologist can create a plan that helps treat and prevent breakouts.
Warts: Warts are noncancerous skin growths that are caused by a viral infection in the top layer of the skin. Warts are usually skin colored and feel rough to the touch, but they can also appear dark in color or flat and smooth, depending on their location. In children, warts can disappear without treatment over several months to years. However, warts that are bothersome, painful or rapidly multiplying should be treated. Water’s Edge providers use a variety of treatments, depending on the type of wart and the age of the patient.
Eczema: Eczema is often called “the itch that rashes”. Eczema appears in itchy patches that can be widespread or limited to a few areas like the back of the knee or inside of the elbow. Between 10% and 20% of children develop eczema, and at least 80% of these children will have it before the age of five. If your child has eczema, it’s important to see your Water’s Edge provider and have the condition treated.
Rashes: Skin rashes are very common all year round, but especially in the summer months where the warm weather can cause rashes that irritate skin. Active children can develop a heat rash or get into poison ivy and other plants that may cause rashes. For some children, insect bites can cause an allergic skin reaction, while other children might be exposed to bacterial or viral skin infections that cause rashes. Your Water’s Edge provider can correctly diagnose and treat any skin rash your child may develop.
Sun Damage: Damage from the sun’s rays affects children as well as adults. Sun protection should begin in infancy and continue throughout life. We get about 80% of our total lifetime sun exposure in the first 18 years of life. So, protecting your child’s skin from the sun is very important to prevent skin cancer later in life. Be sure you are using a sunscreen with SPF 30 or higher and wear a t-shirt and hat when in the sun. Also, keep your children out of the sun in the middle of the day from 10am-3pm when the sun’s rays are most intense.
We Care About Skin Health
At Water’s Edge, we care about skin health and early detection of skin illnesses in children. As Florida’s premiere dermatology practice, our team delivers the highest standard of skin care and dermatology services. We are ready, willing and able to help ensure the health of your children’s skin.
Schedule a summer skin check for your children by clicking on the link below, and we will get you set up for an appointment at any one of our 36 offices near you. Schedule a summer skin check now.
The ABCDE Rules of Melanoma
The fun and sun of summer is knocking at the door, but so is the deadliest result of too much sun – melanoma. That’s why catching and treating it early is the key to battling and even curing melanoma.
Melanoma is tricky. It can start on the surface of the skin, under a nail or even in the eye. Once it gets started growing, it can grow deep into the skin and spread through the body. That’s what makes it so dangerous.
Anyone can get melanoma, regardless of age, sex or skin color. People with certain risk factors should be especially persistent about getting regular skin checks for melanoma and other skin cancers by a dermatologist.
Melanoma Risk Factors
People with these risk factors have a higher probability of developing melanoma:
- Fair, sun-sensitive skin that burns easily or tans poorly
- Red or blond hair; Blue or green eyes
- Have 50 or more moles
- Unusual or irregular-looking moles that are typically large in size
- A history of sunburns or indoor tanning bed use
- Blood relatives who have or had melanoma
- Immune system weakness due to disease, organ transplant or medication
- History of melanoma or another skin cancer
- Age 50 or older
What to Look For
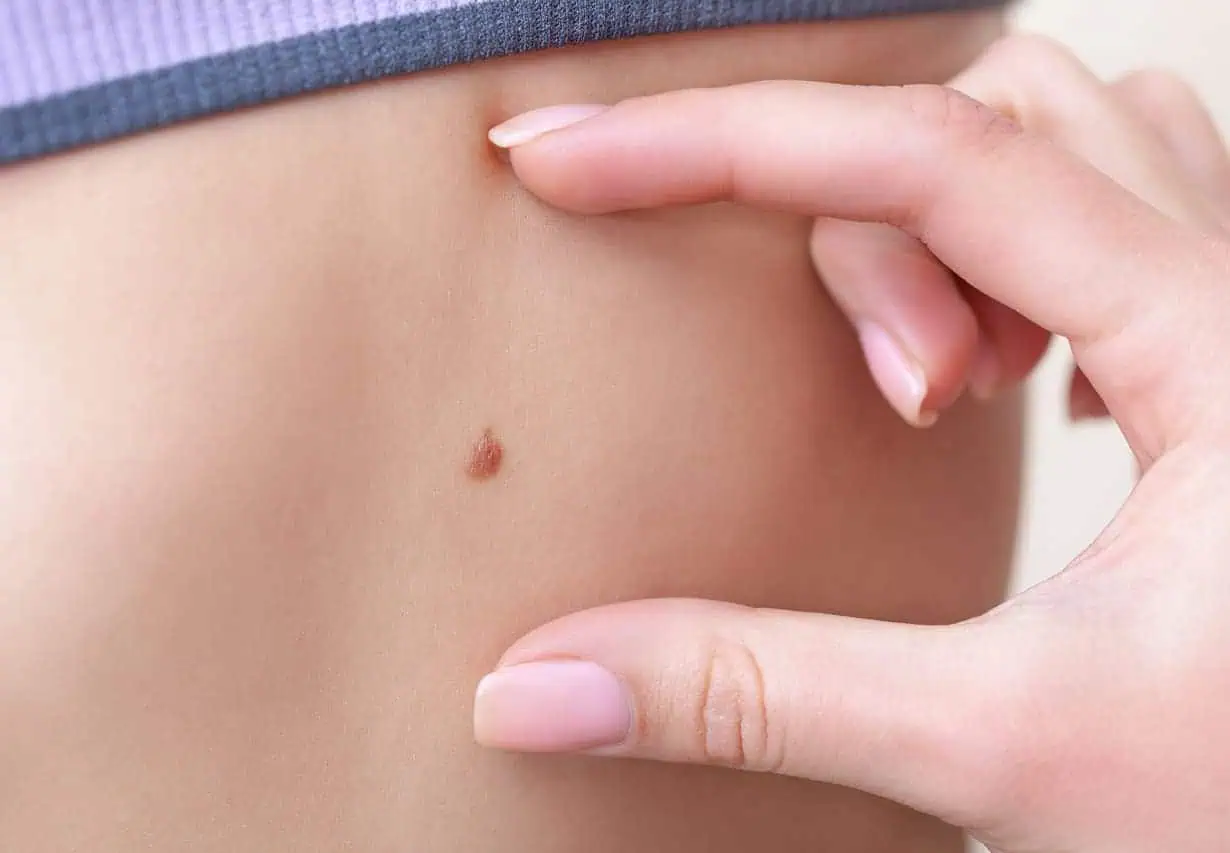
A common warning sign of melanoma is change. Melanoma often begins in or near an existing mole. A change in the shape, color or size of a mole can be a warning sign of melanoma. Also be aware if a mole becomes painful or begins to bleed or itch.
Some melanomas develop suddenly and without warning. Regular skin self-exams can you identify these changes.
The ABCDE Rules of Melanoma
Make sure you are doing regular skin checks. Look for moles and other spots on your skin and apply the ABCDE rules listed below. During a skin self-exam, keep in mind that moles are typically uniform in color, round or oval and have a well-defined border. Though melanomas can vary greatly in appearance, most tend to have one or more of these ABCDE traits, and some have several.
 |
 |
 |
 |
 |
| A = ASYMMETRY One half is different than the other half |
B = BORDER Irregular, scalloped or poorly defined border |
C = COLOR Varied from one area to another with shades of tan, brown, black and sometimes white, red or blue |
D = DIAMETER Melanomas are usually wider than a pencil eraser, but they can be smaller |
E = EVOLVING A mole or skin lesion that looks different from the rest or is changing in size, shape or color |
Make an appointment to see a Water’s Edge Dermatology provider if you notice any of the ABCDE traits. Your practitioner will examine any mole that has one or more of these traits and all new growths.
Remember, early detection and treatment saves lives. Click here to schedule a skin cancer screening at your nearest Water’s Edge Dermatology office.
Skin Cancer Treatments
Hearing the word “cancer” can be scary. However, when it comes to skin cancer, it doesn’t have to be frightening. Although it is the most common cancer in the United States, skin cancer is highly curable when caught and treated early.
If you are diagnosed with skin cancer or a pre-cancerous spot, schedule a visit with one of our highly-skilled skin experts. At Water’s Edge Dermatology, you have the best options for curing your skin cancer. Not only are do we have many highly specialized Mohs surgeons on staff, but we are the only dermatology practice in Florida that also offers electron beam therapy as a non-surgical option for our patients. Both treatment options boast high success rates for curing skin cancer.
Types of Skin Cancer and Pre-Cancer
Actinic Keratosis
This is a “pre-cancer” and is usually treated with liquid nitrogen (freezing) or topical (on the skin) medications.
Basal Cell Carcinoma
The most common skin cancer diagnosed in the US. It is very curable and rarely spreads (metastasizes). Treatments for basal cell carcinoma include: curetting and electrodesiccation, excision, Mohs Surgery or radiation therapy. Occasionally, very superficial and small basal cell carcinomas can be treated with liquid nitrogen (freezing) or topical medication.
Squamous Cell Carcinoma
The second more common skin cancer. Generally, it is very curable and has a low risk of spreading (metastasizing) if small and flat. Treatments for basal cell carcinoma include: curetting and electrodesiccation, excision, Mohs Surgery or radiation therapy. Occasionally, very superficial and squamous cell carcinomas can be treated with liquid nitrogen (freezing) or topical medication.
Malignant Melanoma
This type of cancer is less common than basal cell carcinoma and squamous cell carcinoma and must be treated aggressively. Melanoma requires immediate attention because it is an aggressive cancer that can spread (metastasize) to local lymph nodes or beyond. Treatment of Melanoma is typically managed by a team of providers specializing in Mohs surgery and radiation therapy. Thankfully, many melanomas are detected at a very early stage during annual skin checks performed by our highly skilled skin experts.
Skin Cancer Treatment Options
At Water’s Edge Dermatology, we believe you should have a choice when it comes to treating your skin cancer. Whereas most dermatology practices only offer surgical options, Water’s Edge Dermatology is different. We offer our patients the choice between the standard surgical options and a non-surgical option with electron beam therapy.
Below are the most common skin cancer treatment options available to you at Water’s Edge Dermatology.
Curetting and Electrodesiccation
This procedure involves removing cancerous skin through scraping & cauterization. The resulting wounds can take 4-6 weeks to heal.
Excision
This is an in-office surgical procedure where the cancerous tissue is removed from the patient using a local anesthetic.
Mohs Surgery
Named after Dr. Frederic Mohs, this surgical technique is used to treat basal cell carcinoma and squamous cell carcinoma by completely removing the tumor. Mohs Surgery is most commonly used for people who have skin cancer on high-risk locations (the face, neck or hands), recurrent cancer at any site, a predisposition to multiple skin cancers or rapidly growing or large tumors.
During Mohs Surgery, layers of cancer-containing skin are progressively removed, immediately frozen and then examined by a surgeon under a microscope until all the cancer is gone. Once the cancer is removed, the area is repaired with stitches by the provider or a plastic surgeon, depending on the depth and shape of the wound. This process typically takes 2-4 hours. Mohs Surgery is performed under local anesthetic, adding to the safety of this procedure.
Mohs Surgery offers among the highest cancer cure rate while minimizing removal of the surrounding healthy tissue. It has been cited that the cure rate for Mohs Surgery is between 97% - 99% for basal cell carcinoma, with a lower cure rate for squamous cell carcinoma.
Electron Beam Therapy
Electron beam therapy is a state-of-the-art type of superficial radiation therapy. It is a non-surgical, non-invasive, pain-free treatment option that is highly effective at treating many types of skin cancer while providing excellent cosmetic results. Previously only available at major cancer centers and hospitals, Water’s Edge Dermatology is one of the only dermatology practices in Florida offering this state-of-the-art skin cancer treatment.
This technique uses a finely tailored electron particle beam to selectively destroy cancer cells, “melting away” the cancer and sparing normal tissues. It does not use penetrating radiation and is very different from the type of radiation therapy used to treat other cancers, such as breast, lung and prostate. Treatment is delivered in a series of gentle, two-minute sessions five days a week for a course of 3-6 weeks. The total length of treatment depends on several factors including cancer type, location and medical history. During the course of treatment, there are no limitations on daily activities. You can continue normal activities such as work, exercise, swimming, etc. throughout your treatment.
This non-surgical option is ideal for cancers located on the face, scalp, extremities or any location on the body where surgery might be challenging or where the best possible cosmetic outcome is desired. Additionally, radiation therapy is a safer alternative to surgery for patients with certain medical conditions or who are taking some medications (including blood thinners). Like other common skin cancer treatments, electron beam therapy is generally covered by insurance.
It is important to know that most skin cancers can be treated with surgery or electron beam therapy. Both options come with advantages and disadvantages. If you have received a skin cancer diagnosis and would like to discuss treatment options, please contact us at (877) 544-3880. We are happy discuss the advantages and disadvantages of each treatment option with you and answer any questions you may have.
First Monday in May is Melanoma Monday
Did you know that skin cancer is the most common cancer? Approximately 9,500 people in the U.S. are diagnosed with skin cancer every day. That means approximately one in five Americans develop skin cancer. While melanoma is not the most common type of skin cancer, it is the most dangerous. It is responsible for 10,000 American lives lost every year and is the second most common form of cancer in females ages 15 to 29. The good news is that skin cancer is also the most preventable cancer.
To raise awareness of melanoma and to encourage annual skin checks to help prevent skin cancer in general, the American Academy of Dermatology designates the first Monday in May as Melanoma Monday.
Who gets melanoma?
People of all colors and races get melanoma. Those with light skin who sunburn easily are at higher risk. If you have any of the following risk factors, you need to take extra caution in protecting your skin from the harmful rays of the sun:
- History of sunburns
- Family history of skin cancer
- Exposure to X-rays
- Use of tanning beds or sunlamps
What does melanoma look like?
Melanoma often develops in a mole or appears suddenly as a new dark spot on the skin. Be on the lookout for changes in moles, and if you see irregular edges or unusual colors in a mole, schedule a visit with your Water’s Edge Dermatology provider right away. Catching melanoma early (before it can spread) is key to stopping it. Even though melanoma can be deadly, survival rates can be greater than 90% when treated early.
Preventing melanoma
Tips to help prevent melanoma:
- Wear broad-spectrum, water-resistant sunscreen with an SPF of 30 or more on exposed skin
- Cover up with a hat and clothing
- Stay in the shade when possible, especially 10am-4pm when the sun’s rays are the strongest
- Protect children from sun exposure by playing in the shade, wearing protective clothing and applying sunscreen
- Avoid tanning beds, which can cause skin cancer and wrinkling
- Check your birthday suit on your birthday. If you notice any skin changes, skin growths or bleeding on your skin, see a Water’s Edge Dermatology practitioner immediately
In addition to doing self-exams on your birthday, May is a great month to schedule a skin check by a highly specialized skin care expert. At Water’s Edge Dermatology, our providers are experts in spotting melanoma and treating it early with procedures just right for each of our valued patients. Be safe and schedule your skin cancer check now.
Request an appointment with one of our skin care experts at Water’s Edge Dermatology.