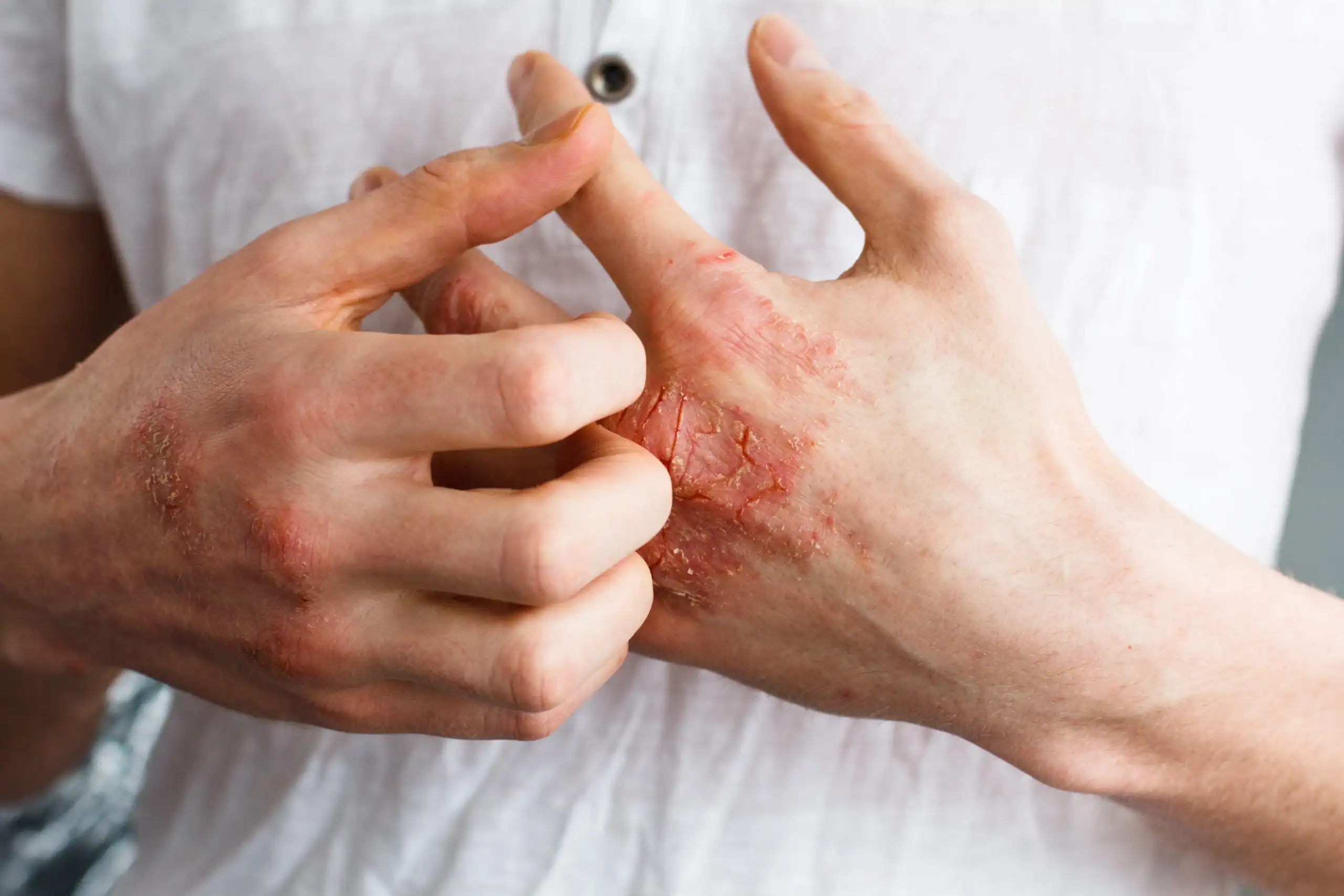
5 Common African American Skin Conditions
Medical review by Rachelle Lacey, MD
Everyone’s skin is different — dry versus oily, thick versus thin, light versus dark. African American skin is different from Caucasian skin in that the top layer contains more pigment, called melanin. But the differences don’t end there. Certain gene mutations more common in African American people mean that certain skin conditions are more common, too.
Rachelle Lacey, MD, a dermatologist at Water’s Edge Dermatology and an expert in treating conditions in skin of color, reveals some of the skin problems she sees most in African American patients.
Atopic dermatitis (eczema)
"Atopic dermatitis is something I see more in African American populations, and the reasons are both environmental and genetic,” said Dr. Lacey. “One major cause is due to the change in the filaggrin in the skin.” Filaggrin is a protein in the top layer of skin that’s essential to maintaining the skin’s barrier function and keeping skin hydrated. A mutation in the gene that codes filaggrin causes a filaggrin deficiency.
African Americans are not only more prone to eczema, but they’re also more prone to severe cases of eczema. In dark skin tones, an eczema rash may appear darker brown, purple or grey instead of red.
Read about eczema treatments here.
Keloids and hypertrophic scars
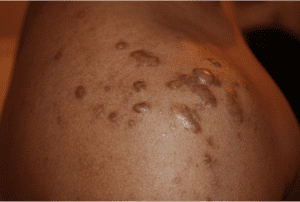
African American skin may contain gene mutations that increase the expression of fibroblasts in scar tissue. Fibroblasts are cells that create collagen. An excess of collagen makes skin much more vulnerable to scar-like formations, including keloids and hypertrophic scars.
Keloids are raised, firm growths of tissue that form over and beyond a wound, such a burn, cut, incision, acne blemish, injection site or ear piercing. They can occur anywhere on the body, but they often develop in less fatty areas, such as on the face, neck, earlobe, chest or shoulders. They can grow much larger than the original wound and may be painful or itchy.
Hypertrophic scars are similar but they don’t typically grow beyond the site of the injury. They may continue to thicken for several months, but they may slightly flatten over a long period of time.
Read about keloid and hypertrophic scar treatments here.
Hidradenitis suppurativa
In hidradenitis suppurativa, also called acne inversa, cyst-like bumps develop in hair follicles in areas where the skin rubs together, such as the underarms, groin, between the buttocks and under the breasts. The bumps can grow deep into the skin. “A lot of times, they can be very painful, and they can drain fluid onto clothing,” said Dr. Lacey. Deep scars can form as the bumps heal.
Tunnels, known as sinus tracts, may develop under the skin between bumps, and they may produce foul-smelling pus if the skin breaks. Sinus tracks also contribute to scarring.
Hidradenitis suppurativa is chronic, but your dermatologist can develop a treatment plan to reduce and help manage flares.
Read about hidradenitis suppurativa treatments here.
Melasma
Melasma, which mostly affects women, causes dark patches, usually on the face. “It’s definitely more noticeable in darker skin types. Often, you can have even more darkening of the cheeks and the forehead because of the increased pigmentation that is naturally found in skin of color,” said Dr. Lacey. “And it can be harder to treat as well.”
Melasma can run in families. Triggers include pregnancy, birth control pills, hormone therapy and sun exposure. In dark-skinned people, skin irritation is another possible trigger, so choosing gentle skin care products is important.
Read about melasma treatments here.
Hyperpigmentation
African American skin contains more melanosomes, tiny structures within melanocytes that make pigment. Melanosomes are also less clustered together within melanocytes and there is also increased transmission of melanin to the surface of the skin. That’s the reason the skin of color appears darker.
As a result, said, Dr. Lacey, “rashes and other skin issues can look a little different. They may also resolve and heal differently. You may have leftover hyperpigmentation that lasts for months once the issue resolves.” In hyperpigmentation, darker patches or spots develop.
“In African American patients, hyperpigmentation is one of the most common issues I see,” said Dr. Lacey.
One type of hyperpigmentation, known as post-inflammatory hyperpigmentation (PIH), can occur as a result of inflammatory acne or even harsh products used to treat it. “You can also get hyperpigmentation as a result of atopic dermatitis, bug bites and even psoriasis,” said Dr. Lacey.
Read about hyperpigmentation treatments here and treating acne in dark skin here.
Whatever skin problem you face, it is important to consult a dermatologist who has experience treating patients with your skin tone to avoid creating new problems, including scarring, hyperpigmentation and hypopigmentation (areas of lighter skin). An experienced, knowledgeable provider can also suggest products and procedures to help your skin look and feel its best.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Why Diabetes Can Cause Dry, Itchy Skin
Medical review by Richard Levine, MD
If you have diabetes, you may know it can affect your heart, kidneys and nerves, particularly if the disease is poorly controlled. But did you know it can also cause dry, itchy skin?
An estimated 79% of people who have diabetes mellitus, the most common form, experience skin issues such as dryness, itching and infections. These can develop at any point during the course of the disease. In some cases, they may even be the first sign that a person has diabetes.
The connection between diabetes and itchy skin
Diabetes can make the body lose too much fluid through urination and evaporation through the skin. The result: dry, itchy skin that can be bothersome and sometimes uncomfortable.
Itching, especially in the lower legs and feet, can also be caused by poor circulation, which is common with diabetes. Some people experience a skin reaction to their diabetes medication or insulin injections.
In addition, itching can be brought on by diabetes complications including nerve damage, kidney disease and liver disease. Certain medications for other health problems common in people with diabetes, such as high blood pressure and high cholesterol, can make the skin itchy, too.
Scientists suspect that those with type 2 diabetes may be vulnerable to itchy skin (and also skin infections) for yet another reason: Their skin’s barrier function is impaired. Exactly how and why this happens is still being studied.
Diabetes and skin infections
Studies suggest that more than half of people with diabetes will develop a skin infection at some point.
Scratching and dryness can create cracks that let bacteria in. It’s not unusual for people with diabetes to develop bacterial infections such as folliculitis, boils and carbuncles.
Itchy fungal infections are also more likely in people with diabetes, possibly due to high blood sugar. Infections caused by the yeast-like fungus Candida albicans often crop up in areas with moist folds, such as the armpits, groin area, under the breasts and between the fingers and toes. Infections caused by mold-like fungi called dermatophytes include ringworm, jock itch and athlete’s foot.
Skin care tips for people with diabetes
If you have diabetes, good skin care is an important part of managing your disease. These tips can help keep your skin soft, calm and infection free.
Keep your blood sugar under control. Follow your doctor’s plan to manage your blood sugar levels. When your diabetes is well managed, your whole body, including your skin, benefits.
Take lukewarm showers and use a moisturizing soap. Hot baths and showers dry out the skin. Dry off well after your shower, especially under the arms and breasts and between the legs and toes.
Use a gentle moisturizer. A cream or ointment is preferable to a lotion since lotions contain more water. Ask your dermatologist for a recommendation. Don’t moisture between your toes.
Avoid scratching if you can. Scratching can create openings in the skin that let in bacteria.
Consider using a humidifier in winter. Dry air can make dry skin worse.
Wash minor cuts right away with mild soap and water. Talk to your doctor about using an antibiotic cream or ointment. Cover the cut with a bandage. Deep cuts require professional treatment.
Practice good foot care. Examine your feet daily. Look for any cuts, blisters or sores. Unless the wound is minor and heals on its own, see a doctor right away. When you cut your toenails, cut them straight across and not too short. Smooth the corners with a nail file if necessary.
Your dermatologist can help
A dermatologist can get to the bottom of why your skin is itching and offer treatment suggestions. He or she can also diagnose and treat other diabetes-related skin problems that don’t involve itching.
Prompt treatment of skin problems is especially important when you have diabetes. See a dermatologist or other doctor if you have signs of an infection. A bacterial infection may cause redness, pain, swelling and oozing. Fungal infections typically itch. The skin may also be red, scaly, swollen, or blistered.
If you develop severe itching, consult your dermatologist or diabetes doctor without delay. It could be a sign that your diabetes treatment plan isn’t working.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
5 Reasons Hand Eczema Flares Up (And How to Tame It)
Hand eczema flare-ups are beyond annoying. It can cause redness, itching, cracks, blisters, and dryness to the point of peeling and flaking, but that’s not all.
During a bad flare-up of hand eczema, fingers can swell and hands can hurt. Without proper treatment, hand eczema can become chronic. A severe case could even make it hard to button your clothes or use a computer.
So, what causes flares? Here are five of the most common triggers and tips for avoiding them.
Trigger 1: Exposure to water
Constantly wetting and drying your hands can break down skin's protective barrier, especially when you have sensitive skin that is prone to dryness. "Even after hands are dried, there's some water left that evaporates. When it does, it reduces skin's natural oils," said Dr. Alissa O'Brien, a dermatologist at Water’s Edge Dermatology. If the water is piping hot, it’s even more irritating and drying.
How to dodge it: For dishwashing and other wet tasks, wear vinyl gloves with a cotton lining (or a separate cotton liner). Latex gloves can cause allergic reactions, so it's best to avoid them. When you wash your hands, use a mild, low-lathering soap free of fragrances, preservatives, and dyes, and use lukewarm water, not hot. After washing and gently drying your hands, apply moisturizer, preferably an ointment. "Aquaphor Healing Ointment is probably one of the best," said Dr. O'Brien. Other ointment brands she recommends include Vaseline, Cetaphil, CeraVe, Eucerin, and Aveeno. If you find ointments too greasy to use during the day, use a cream moisturizer instead and an ointment at night, under a pair of cotton gloves.
Trigger 2: Exposure to allergens or irritants
Hand eczema is often caused or worsened by exposure to a substance that’s irritating — think alcohol, bleach, cleansers or solvents — or one that causes an allergic reaction, such as perfume or certain plants. Florists often get dermatitis on their thumb and forefinger when clipping chrysanthemums and tulips (it’s known as "tulip fingers"). In the kitchen, vegetables — particularly garlic and onion — can lead to a flare-up, especially on the fingertips. Even fabric can exacerbate hand eczema. Rough, coarse materials such as wool and stiff synthetics such as polyester can trigger an itch-scratch cycle that worsens the condition.
How to dodge it: Pay attention to what sets off your eczema. "Whether you're at home or on the job, learn what irritates your skin and avoid or limit contact with those things," advised Dr. O'Brien. Use a washing machine, dishwasher, and food processor when possible and ask other family members for help with housework, cooking and gardening to give your hands a break. Protect your hands from irritants and allergens by wearing vinyl or cotton gloves while you do chores. Wear heavy-duty vinyl or neoprene gloves at work if you’re exposed to triggers there. If the gloves you have irritate your skin, ask your dermatologist for recommendations.
Trigger 3: Stress
Stress triggers the production of hormones, including cortisol and adrenaline, that can suppress the immune system and cause an inflammatory response in the skin. An eczema flare-up can create even more stress, leading to a vicious cycle. If you’re under a lot of emotional or physical stress, you may be at greater risk of dyshidrotic eczema, a type that causes itchy blisters on the palms of the hands that may be filled with fluid.
How to dodge it: Exercise is an excellent way to manage stress. In addition to boosting the production of feel-good chemicals, it also improves sleep, which can help to further decrease stress. To ease anxiety on the spot, take slow, deep, belly-expanding breaths in through your nose and exhale through your mouth.
Trigger 4: Sweating
Whether you’re walking outside, playing with your kids, or exercising, sweating can irritate the skin. The salty residue that’s left behind after sweat evaporates is known to worsen the itch. Some research suggests that people with eczema are more prone to excessive sweating.
How to dodge it: Keep a towel with you as you work out or when you’re outside to wipe away sweat, and rinse off sweat with lukewarm water afterward to prevent salty build-up. Because wearing gloves, especially waterproof gloves, can make your hands sweat, take them off frequently (every 20 minutes or so) to let your skin cool down.
Trigger 5: Physical wear and tear
Minor hand trauma from tasks like digging in the garden with bare hands can cause hand eczema or make it worse, as can friction from activities like handling large quantities of paper.
How to dodge it: Wear task-appropriate gloves. Cotton and fabric gloves can keep hands clean and protect against abrasions, but they may not be adequate for work with rough or sharp materials. Working with thorny plants, palm fronds or brambles may require leather gloves with longer cuffs.
Avoiding eczema triggers often goes a long way toward managing the condition. The key is to be diligent. "It can take a massive amount of effort if you have severe hand dermatitis, and people often want a quick fix, but putting in that effort to take care of your skin really pays off in keeping eczema from coming back," said Dr. O'Brien.
Don’t get discouraged: Hand eczema can be stubborn, and it may take a few months for the patches of red, scaly and inflamed skin to fully heal. After that, your eczema is less likely to return.
END
Article Written By: Karyn Repinski, a Brooklyn, NY-based award-winning health and beauty writer.
Medical Review By: Ted Schiff, MD
Sun Safety
Summertime is fun time to spend outdoors. But in sunny Florida, that means more exposure to the sun’s ultraviolet (UV) rays. Those UV rays can damage unprotected skin in as little as 15 minutes and even lead to skin cancer. Here are some tips to keep you sun safe all year long.
Seek Shade
One of the easiest ways to reduce your exposure to damaging UV rays is to get in the shade. Seek shade under a tree, umbrella or another shelter in order to reduce your risk of sun damage. You’ll help your skin look younger longer and lower your risk of developing skin cancer.
Protective Clothing
Cover up with long-sleeved shirts and long pants when you can to protect your skin from the sun’s harsh UV rays. There are clothing options available that contain a UV protectant built into the fabric. Also, remember that a wet t-shirt provides less UV protection than a dry one, and darker colored clothing protects better than light-colored clothing. Don’t forget to top it off with a hat with a brim all the way around that shades your face, ears, and back of the neck. If you choose a baseball cap instead, be sure to protect your ears and the back of your neck with sunscreen of at least 30 SPF.
Sunglasses
Choose sunglasses that are labeled UV protectant to reduce the risk of developing cataracts. Most of the sunglasses sold in the U.S. block both UVA and UVB rays. Sunglasses also protect the skin around your eyes from sun damage, and wrap-around sunglasses are an excellent option to block UV rays that might sneak in from the side.
Wear Sunscreen
Choosing the right sunscreen can be daunting, so we recommend following these four rules to make it easier:
- Broad-spectrum – Broad-spectrum sunscreen protects the skin from both ultraviolet A (also known as UVA) and ultraviolet B (also known as UVB) rays. Both of these rays can cause skin cancer.
- SPF 30 or higher – The sun protection factor (SPF) rating indicates how well a sunscreen protects you from the sun by blocking harmful UVB rays. Choose a sunscreen with SPF 30 or higher to make sure you are protected.
- Key ingredients – Look for active ingredients like ecamsule, avobenzone, titanium dioxide, sulisobenzone or zinc oxide. Beware of products that include oxybenzone or octinoxate which are harmful to the environment. Some areas of Florida have banned the sale of sunscreen with oxybenzone and octinoxate because these chemicals can damage coral reefs.
- Avoid tanning oils – They generally do not provide enough protection against the harmful effects of the sun.
How to Apply Sunscreen & How Often
To get the maximum protection from your sunscreen, follow these recommendations:
- One ounce of sunscreen is considered the right amount. Cover all exposed areas of the body thoroughly. Don’t skimp. Many people don’t use enough sunscreen.
- Apply sunscreen 15 to 30 minutes before going in the sun. Don’t forget the tips of the ears, feet, back of the legs and bald spot (if you have one). Reapply sunscreen every two hours and use a UV-protective lip balm to cover your lips.
- If you are exercising or are in the water, it’s a good idea to get a sunscreen that is resistant to water and sweat. The FDA defines water resistant to mean that the SPF level stays effective after 40 minutes in the water. Very water-resistant means it is effective after 80 minutes of swimming. These sunscreens are not waterproof, so reapply regularly.
Protecting your skin from the harmful rays of the sun can help you look younger and prevent skin cancer. Just to be on the safe side, be sure to get a skin cancer screening every year, so if you do develop skin cancer, it can be detected and treated early.
Schedule a skin cancer screening at your nearest Water’s Edge Dermatology office.