The ABCDE Rules of Melanoma
The fun and sun of summer is knocking at the door, but so is the deadliest result of too much sun – melanoma. That’s why catching and treating it early is the key to battling and even curing melanoma.
Melanoma is tricky. It can start on the surface of the skin, under a nail or even in the eye. Once it gets started growing, it can grow deep into the skin and spread through the body. That’s what makes it so dangerous.
Anyone can get melanoma, regardless of age, sex or skin color. People with certain risk factors should be especially persistent about getting regular skin checks for melanoma and other skin cancers by a dermatologist.
Melanoma Risk Factors
People with these risk factors have a higher probability of developing melanoma:
- Fair, sun-sensitive skin that burns easily or tans poorly
- Red or blond hair; Blue or green eyes
- Have 50 or more moles
- Unusual or irregular-looking moles that are typically large in size
- A history of sunburns or indoor tanning bed use
- Blood relatives who have or had melanoma
- Immune system weakness due to disease, organ transplant or medication
- History of melanoma or another skin cancer
- Age 50 or older
What to Look For
A common warning sign of melanoma is change. Melanoma often begins in or near an existing mole. A change in the shape, color or size of a mole can be a warning sign of melanoma. Also be aware if a mole becomes painful or begins to bleed or itch.
Some melanomas develop suddenly and without warning. Regular skin self-exams can you identify these changes.
The ABCDE Rules of Melanoma
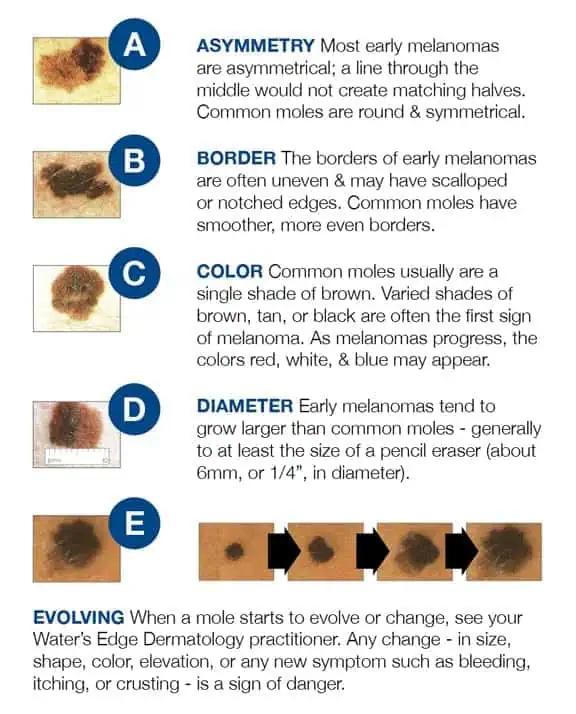
Make sure you are doing regular skin checks. Look for moles and other spots on your skin and apply the ABCDE rules listed below. During a skin self-exam, keep in mind that moles are typically uniform in color, round or oval and have a well-defined border. Though melanomas can vary greatly in appearance, most tend to have one or more of these ABCDE traits, and some have several.
 |
 |
 |
 |
 |
| A = ASYMMETRY One half is different than the other half |
B = BORDER Irregular, scalloped or poorly defined border |
C = COLOR Varied from one area to another with shades of tan, brown, black and sometimes white, red or blue |
D = DIAMETER Melanomas are usually wider than a pencil eraser, but they can be smaller |
E = EVOLVING A mole or skin lesion that looks different from the rest or is changing in size, shape or color |
Make an appointment to see a Water’s Edge Dermatology provider if you notice any of the ABCDE traits. Your practitioner will examine any mole that has one or more of these traits and all new growths.
Remember, early detection and treatment saves lives. Click here to schedule a skin cancer screening at your nearest Water’s Edge Dermatology office.
Cancerous Moles: What to Look For and When to See a Doctor
When a new mole appears, a brief panic sets through your mind as you consider the possibility of it being cancerous. Moles are tiny growths on the skin that develop when pigment cells, known as melanocytes cluster together, rather than being distributed across the skin. As years pass, moles can change, or even disappear. However, if you have a mole that changes color, size, or shape, you may want to have it checked out.
Most moles are between the size of a pencil tip and the size of an eraser, and are pink, brown, or tan in color. If your mole is dark, uneven in color, or asymmetrical, it can be a sign that it is cancerous. Other important signs to look for are dry skin around the surface of the mole, or the mole becoming hard or bumpy. If the mole begins to itch, bleed, or ooze, contact your doctor immediately.
Keep an eye on any new growths on skin that you may find, as they could be signs of skin cancer, such as Melanoma. Melanoma is characterized by the growth of pigment-producing cells, and is the most dangerous form of skin cancer. While Melanoma is highly curable if detected early, unchecked Melanoma can spread to the lymph nodes and internal organs, and some cases have resulted in death. If you have more than 50 moles, large moles, or atypical moles, you have a substantially increased risk of developing melanoma or other forms of life-threatening skin cancers.
If you are unsure whether or not an atypical mole is dangerous, it’s best to go make an appointment with a dermatologist right away, especially if your family has a history of cancerous moles. While most growths on the skin turn out to be benign moles, it’s better to be safe than sorry.
Common and Atypical Moles
Skin cancer is a prevalent problem in the United States, with an estimated one in five Americans developing the condition over the course of their lifetime. Typically caused by a combination of UV exposure, risk factors, and genetic predisposition, skin cancer is not only life-threatening, but can also result in a number of troubling side effects, including a weakened immune system and candida infections in the lungs, liver, and skin.
For this reason, it is important that patients take measures to prevent harmful sun exposure, stay informed of their risk factors, and schedule regular appointments with dermatology and skin cancer specialists at a local dermatologist clinic. This is especially important for people who have more than 50 moles, large moles, or atypical moles, as these conditions can substantially increase one's risk of developing melanoma and needing treatment for skin cancer. This article aims to answer many questions people with these moles, or atypical nevi, may have, including how to identify a cancerous mole and when you may need to undergo a dysplastic nevus removal. Read on to learn about this common risk factor.
Moles
Moles are a common physical feature that are either present at birth or appear during childhood. By adulthood, most people will have anywhere from ten to 40 moles, also called nevi, above the waist on areas exposed to the sun. They are typically smaller than 5 mm, have defined edges, and can be pink, tan or brown. New moles can develop over time due to sun exposure, but it is important to regularly check all of these marks for physical changes, as pain or a difference in appearance can be a sign of cancer.
Atypical Moles
In contrast, a mole with unusual characteristics is called a dysplastic nevus. These nevi may be bigger, have an uneven shape, mixed colors, or an irregular border. Like normal moles, these are typically found in areas that receive a lot of sun exposure, but can also develop in areas that are not exposed to the sun and below the waist. People with a high number of typical moles often have several dysplastic nevi mixed in. Having a high number of these nevi is part of a condition called dysplastic nevus syndrome, which has an even higher likelihood of developing melanoma.
Having dysplastic nevi can be nerve-wracking, as the moles often naturally resemble skin cancer. However, while a person's chances of developing melanoma and other skin cancers increases with the number of dysplastic nevi they have, these moles often remain stable as long as the person protects their skin, eschews tanning, and performs a self-exam at least once a month. If a change is noticed in a mole's texture, appearance, or sensation, the patient should make an appointment with their dermatologist immediately. Some patients may wonder if they can undergo a dysplastic nevus removal to avoid these measures; however, because new moles and patches can form on the skin, this is often pointless and expensive. Instead, a dysplastic nevus removal is typically reserved for the process of identifying and treating skin cancer.
Having an increased risk of skin cancer can be a frightening prospect. However, by taking the proper steps, you can help protect yourself from the condition, even if you have common or atypical moles. How do you protect yourself from skin cancer?
What is Dysplastic Nevus Syndrome?
With skin cancer now estimated to affect one in five people in the United States at some point in their lives, many people are now aware of the various risks associated with this condition and how to prevent it. However, even if you wear sunscreen and check your skin fairly regularly, you may still have an increased risk of developing this disease. This is especially true if you have dysplastic nevus syndrome, a condition that has been linked to serious conditions like melanoma.
It is commonly known that a person with 50 or more moles has an increased risk of developing skin cancer, especially melanoma. Accordingly, dysplastic nevus syndrome refers to the presence of a high number of unusual moles, called dysplastic nevi. These may resemble melanoma from the onset and signify an unusually high risk of developing a real case of the condition. Someone with dysplastic nevus syndrome may have 10 or 12 times the risk of developing skin cancer and melanoma than the general population, and as a result, dysplastic nevi are much more common among skin cancer patients than those without the disease. Dysplastic nevus syndrome runs in families and represents an inherited tendency to develop different types of skin cancer.
There is no dysplastic nevus treatment that can reduce the risk of developing skin cancer, but because of the nature of the condition, it is important that people with this disorder see dermatology and skin cancer specialists as soon as possible to prevent potential problems. Because the syndrome runs in families, dermatologists typically recommend that patients begin receiving full-body exams at age 10, including checks on the scalp, eyes, genitals, nails and other areas. Because a high percentage of people with dysplastic nevus syndrome develop melanoma in their teens, this is one of the most effective preventative options available. Patients who also have a family history of pancreatic cancer are also offered the chance to receive screenings starting at age 50, or 10 years before the age that their earliest family member was diagnosed.
Research shows that only 2-8% of the Caucasian population have dysplastic nevi. However, if you have noticed a number of atypical moles on your body and have close family members with skin cancer or melanoma, you have good reason to discuss your chances of developing these conditions with a dermatologist specialist. Fortunately, the field of dermatology has experienced a number of scientific breakthroughs in everything from acne therapies to skin cancer treatment, meaning that you have a good chance of treating any problems that may have occurred due to this genetic prevalence. Visit a dermatologist clinic today to discuss these options and preventative care with a professional today.
How to Give Yourself a Skin Mole Exam
You frequently hear dermatologists and skin cancer experts talk about the importance of regularly examining your skin, but do you know the best way to check yourself? Your skin moles should remain fairly constant, but here are the steps to find any new or changed moles.
Skin Mole Self-Examination:
- Start with your face, ears, scalp and neck. Use a hand mirror to see the back of your neck and a comb to part your hair to make this easier. Or, ask friend to help check your scalp.
- Stand in front of the mirror and look at the front and back of your body. Remember to raise your arms to look at your sides.
- Next, look at your hands and arms. Carefully examine your fingernails, palms and elbows, and look at your arms from all directions.
- Look at your legs from all angles using your mirror. Remember to check swimsuit areas for moles as well.
- Sit down and examine the bottoms and tops of your feet, your toenails and the spaces between your toes.
- Finally, take notes about your skin’s appearance and mark the dates of your skin mole exam. This will help you identify changes in your moles in the future.
Most of the moles you find likely developed when you were young, and you will continue developing skin moles until the age of 40. Most moles are harmless, but checking your skin regularly will help you track any changes and alert you to seek mole treatment if necessary.
If you find any suspicious or new moles, make an appointment with your Water’s Edge dermatologist to learn if you need skin mole treatment.
When to See a Dermatologist for a Mole
Skin Moles are common. Almost everyone has a few, and some people develop hundreds. And melanoma, the deadliest type of skin cancer, can develop in or near moles.
Don’t get frightened—most skin moles are not melanoma. So how do you know when to see a dermatologist for your moles? It’s easy; just keep in mind your ABCs.
A stands for ASYMMETRY: If one half of the mole is unlike the other half, have it looked at.
B stands for BORDER: If your mole has an irregular, scalloped or poorly defined border, it could be an early melanoma. Only a biopsy can provide conclusive results.
C stands for COLOR: If a mole’s color varies from one area to another, or if it turns shades of tan, brown and black (opposed to brown, which is normal), call your dermatologist.
D stands for DIAMETER: Melanomas are usually greater than 6mm (the size of a pencil eraser) when diagnosed, but they can be smaller. If a mole is large, have it examined and stay very aware of changes or growth.
E stands for EVOLVING: A mole or skin lesion that looks different from the rest or is changing in size, shape or color could be a sign of early skin cancer.
If you have a mole that shows any of these signs, be sure to schedule an appointment with a Water’s Edge Dermatology provider today. If something doesn’t seem right, or keeps grabbing your attention, come see us.