8 Common Skin Conditions in Elderly Adults
Medical review by Ted Schiff, MD
Like every part of the body, the skin changes with age. The teen years bring dreaded pimples. Middle age brings telltale wrinkles. In elderly adults, skin conditions may become more numerous — and more noticeable — as the skin continues to thin and lose fat, elasticity, and moisture.
Skin cell turnover decreases dramatically, which slows wound healing. Aging weakens the immune system, so skin infections are more common. Age spots may take up more acreage. Large, dark bruises may spring up out of nowhere.
Some skin problems, like dark bruises, are alarming but are mostly harmless. Others require medical attention. Here are eight skin conditions in elderly adults and what older adults, loved ones and caregivers should know.
1. Easy bruising
Why do old people bruise easily? Aging skin is thinner, and there’s less fat to act as cushioning. Also, blood vessels are more fragile and easily broken. Bruises happen when blood leaks out of blood vessels, so more broken vessels means more bruising. Older people who take blood thinners or even over-the-counter painkillers such as aspirin or ibuprofen may bruise more easily.
A minor bump or scrape can result in a surprising amount of bruising and make concerned loved ones wonder what’s happening. The bruises are usually harmless. But anyone who often develops large bruises with no logical explanation should see a doctor to rule out an underlying health problem.
If a loved one or caregiver has any reason to suspect abuse as the cause of bruising, they should investigate. Most accidental bruises occur on the extremities, according to the National Institute of Justice, whereas bruises in abused elders are more likely to occur on the head, neck or torso, and they tend to be large.
Take action
To treat bruises:
- Apply a cold compress for up to 20 minutes a time.
- Apply Dermaka cream, a bruise treatment made with plant extracts and vitamins, according to the package directions.
- If a leg or foot is bruised, keep it elevated when resting.
2. Dryness and itching
Dry skin in elderly adults is very common; in fact, more than half of older adults have it. A loss of sweat and oil glands is one reason. Not drinking enough liquids may be another. In addition, certain chronic health conditions, such as diabetes and kidney disease, can cause dryness and itching, as can some of the medications used to treat them.
Skin may become cracked and painful. Scratching can cause skin irritation and open the way for infection-causing germs to enter.
Take action
If you have dry, itchy skin:
- Take shorter, cooler baths or showers and use a moisturizing soap (skip the deodorant soap)
- Use a moisturizing ointment or cream daily. (Avoid lotions, which contain more water.) CeraVe, Cetaphil and Vanicream all make gentle, effective moisturizers.
- Drink more water.
- Run a humidifier if the air is dry.
- If the itching doesn’t subside, tell your doctor. It could be a sign of liver, kidney or thyroid disease.
3. Age spots

Take action
- Wear sunscreen with at least 30 SPF to help prevent more age spots from developing.
- See a dermatologist to make sure the spots are in fact age spots and not something else, especially if they change in appearance.
- If your age spots bother you, a skin care provider can treat them.
4. Skin tags
Skin tags are soft, spongy, often flesh-colored growths of tissue that typically appear on eyelids, neck, thighs and skin folds such as the armpits, groin and under the breasts. They may hang from the skin on small stalks. Skin tags are more common in women, people who are overweight, older adults and people with diabetes. They can become irritated if clothing rubs them or jewelry snags them.
Take action
- Skin tags are harmless, but if you want one removed, see a dermatologist. A dermatologist will remove it for you.
- Don’t try to remove a skin tag yourself. It’s a bad idea for several reasons.
5. Skin cancer
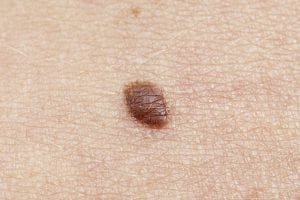
Take action
- Perform a skin check once a month to look for new growths and changes in existing moles. Evaluate moles using the ABCDE test. Make an appointment with your dermatology provider if you see something suspicious.
- Have a skin cancer screening based on the schedule your dermatologist recommends, but at least once a year.
6. Shingles
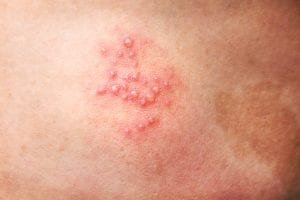
Shingles starts with burning, itching, tingling or extreme sensitivity in one area of the skin. A painful rash then develops, often along with a fever or headache. The rash eventually blisters. Skin infections and long-term nerve pain are possible complications.
Take action
- See a doctor as soon as symptoms appear. Early treatment with an oral antiviral medication may reduce the duration and severity of an outbreak.
- Take an over-the-counter pain medication for pain and use cool compresses, calamine lotion and lukewarm baths with colloidal oatmeal (oats ground into a fine powder) for itching.
- To prevent shingles, get both doses of the Shingrix vaccine.
7. Bed sores
Bedridden or wheelchair-bound older adults are susceptible to open wounds called bed sores or pressure ulcers. These develop in areas subject to pressure when you sit or lie down, such as the tailbone, shoulder blades, backs of the knees and heels. People with diabetes, poor circulation or poor nutrition face a higher risk of bed sores.
Prevention is critical. Bed sores can be very difficult to treat once they develop, and they may become infected.
Take action
- In bed, reposition every two hours. In a wheelchair, change position every 15 minutes.
- Keep skin clean and dry.
- Watch for redness and warmth in one area of the skin; it’s an early warning sign. If you’re a caregiver, call the doctor if you notice this or see a sore, scrape or blister. A wound care nurse may be needed to coordinate care.
- Consider a gel or foam mattress topper or a mattress with alternating air pressure, which can help prevent pressure sores.
8. Skin tears
The fragile skin of elderly adults tears more easily, especially in people who take oral or topical corticosteroids, which can weaken the skin. The skin might tear when you bump into something, or when a caregiver removes wound tape or dressing.
Take action
- Use moisturizer and drink plenty of water to keep skin hydrated, which can help prevent tears.
- Wear long pants and a long-sleeved shirt or arm sleeves to protect the skin.
- If a small tear occurs, wash the wound with gentle soap and water. Put the skin flap back in place if there is one, then cover the wound with gauze.
- See a doctor for more serious tears or if you notice signs of infection, such as redness, swelling, fever, worsening pain or a bad odor.
Written by Jennifer L. Cook, an award-winning editor and writer whose work has appeared in Good Housekeeping, Prevention, Consumer Reports on Health, and Woman’s Day and on Investopedia.com and Bottomlineinc.com.
Shingles, Seniors & Medicare Coverage
Chances are, most young people have little idea of what Shingles is, much less how doctors treat it, or Medicare covers it. But the skin disease that’s scourge to so many millions of seniors has its roots in childhood. Chickenpox, in fact.
Back in the day as they say, there wasn’t a vaccine preventing most kids from contracting the varicella-zoster virus that causes chickenpox. On the other hand, children traditionally experience a significantly milder version of the virus than adults do. In fact, many parents have breathed a sigh of relief when their little ones presented with the telltale red, itchy spots; relieved to get it over and done with.
Well, there’s over and done with. And then there’s the difficult reality that if you did have chickenpox as a child, your body still hosts the varicella-zoster virus. It hides out in your nerve tissue near the spinal cord, waiting for years. Then, when the immune system of some unsuspecting senior dips low enough, it can reactivate as shingles.
So, What’s Shingles & What Do You Do About It?
While chickenpox is generally not feared, shingles is another story. While not a life-threatening condition, it remains a skin disease dreaded by at-risk seniors. Dreaded, because as anyone who’s suffered through it can tell you, shingles can be extremely painful. Think itchy red rash, fluid-filled blisters, numbness and/or burning in the skin.
The good news is, shingles is preventable for more than 9 out of 10 people, with a new, more effective-than-ever shingles vaccine. And if you do contract shingles, more good news is that it usually goes away on its own after 2-3 weeks.
Getting to your dermatologist’s office in the first 2-3 days of a shingles outbreak can be a huge help. This allows common treatments such as oral antiviral medication, pain relievers and possibly corticosteroids to provide real relief before things get out of hand.
If you’re over 50, certainly if you’re over 60, the shingles vaccine is highly recommended. Good alternative to all the medical care and treatment you’ll need if you do get it. Which raises a question important to so many senior healthcare patients/consumers:
What Will Medicare Cover When It Comes To Shingles?
Medicare Part A covers hospital benefits and Part B covers outpatient benefits. If you develop shingles, your visits to the dermatologist for diagnosis and treatments are covered by Medicare Part B.
After you meet your annual Medicare Part B deductible ($183 in 2018), Medicare pays 80% of the cost of your doctor visits and related lab tests. You’re responsible for the other 20%, unless you purchase “Medigap” coverage to help limit out-of-pocket costs for such deductibles and copayments.
While Part B covers your doctor’s visits related to shingles, the medications for treating and/or preventing shingles are generally going to fall under Medicare Part D coverage.
How can Medicare Part D Drug Coverage help with Shingles?
Beneficiaries purchase Part D policies from private insurance companies. Some Part D companies include the varicella-zoster vaccine in their drug formularies. When considering aPart D policy, you’ll want to check on that. While this vaccine might cost $200 or more without coverage, beneficiaries with Part D often pay around half that amount when they use their coverage.
For individuals with an active case of shingles, Part D plans should cover a number of medications which help control the infection. Having Part D coverage means you’ll only be responsible for your plan’s required copayment for any of these covered medications instead of full cost.
The most common and least expensive medication is Acyclovir. This medication has been around since the 1980’s and is a generic form of the brand-name antiviral medication called Zovirax.
Your doctor may also prescribe valacyclovir or famciclovir, which are two newer forms of antivirals that may treat shingles more rapidly than acyclovir. That means it’s worth checking for Part D coverage of these drugs too.
Do take note though; many seniors with Medicare Part D Drug coverage still have to confront the infamous Medicare Part D “Donut Hole” (till 2020). This is an actual reduction in coverage that kicks in for seniors whose drug costs exceed a prescribed monthly and/or annual limit.
For the time being, seniors and their loved ones need to take this and all the other above information into consideration when evaluating the costs and coverages for prevention or treatment of shingles.
Who’s at Risk of Developing Shingles?
Shingles, also known as herpes zoster, is a viral disease that manifests as a painful skin rash with blisters. It develops when the chicken pox virus reactivates in the body, often for unknown reasons.
Anyone who has had chicken pox is at risk for developing shingles. About 20 percent of those who have had chicken pox will get shingles — most develop shingles only once.
It is not clear what reactivates or "awakens" the virus. However the following are thought to cause outbreaks:
- Compromised immunity
- Old age
- Illness
- Trauma
- Stress
Shingles can also be contagious. Though not as contagious as chicken pox, shingles can be transmitted through direct skin contact if blisters break. Because of this, people with shingles should not interact with pregnant women, small children or the immunocompromised.
Shingles typically causes more pain and less itching than chicken pox. A person may feel burning, itching, tingling or extreme sensitivity on the skin. These usually last for one to three days, sometimes more, before a red rash appears in the same area. A shingles rash usually occurs on only one side of the body.
To diagnose shingles, a dermatologist looks at the appearance of the skin and asks how the rash developed. To confirm the diagnosis, a dermatologist may scrape skin cells from a blister for examination under a microscope. Also, the blister fluid containing the virus can be sent to a laboratory for special testing.
Shingles usually clears on its own in a few weeks and seldom recurs. A dermatologist may prescribe an oral medication to help. While shingles is clearing, pain relievers can help ease the discomfort, and cool compresses may provide soothing relief.
The most common problem of shingles is postherpetic neuralgia, which is pain, numbness, itching and tingling that last long after the rash clears. Oral pain medications can help relieve the pain.
A shingles vaccine has been approved by the U.S. Food and Drug Administration (FDA) for people ages 60 and older who have never had shingles. In one study, this immunization decreased the incidence of shingles by more than 50 percent.
If you or someone you know may be at risk for singles, schedule an appointment with a Water’s Edge Dermatology practitioner.


