Flat Warts: What They Look Like and How to Treat Them
Medically reviewed by Julie Forero, DO
Could you have warts and not even know it? You might if they’re flat warts, known medically as verruca plana. These warts are flatter, smoother and smaller than their uglier, bulbous cousins. If you’ve noticed small, slightly raised growths on your face, hands or other body parts and dismissed them as age spots or stubborn acne, the real culprit may be flat warts.
Flat warts aren’t harmful or painful, but you may want to get rid of them for aesthetic reasons. If you suspect you have flat warts on your face, hands, legs or elsewhere, read on to learn why they develop, how to tell them apart from other common skin conditions and options for flat wart treatment.
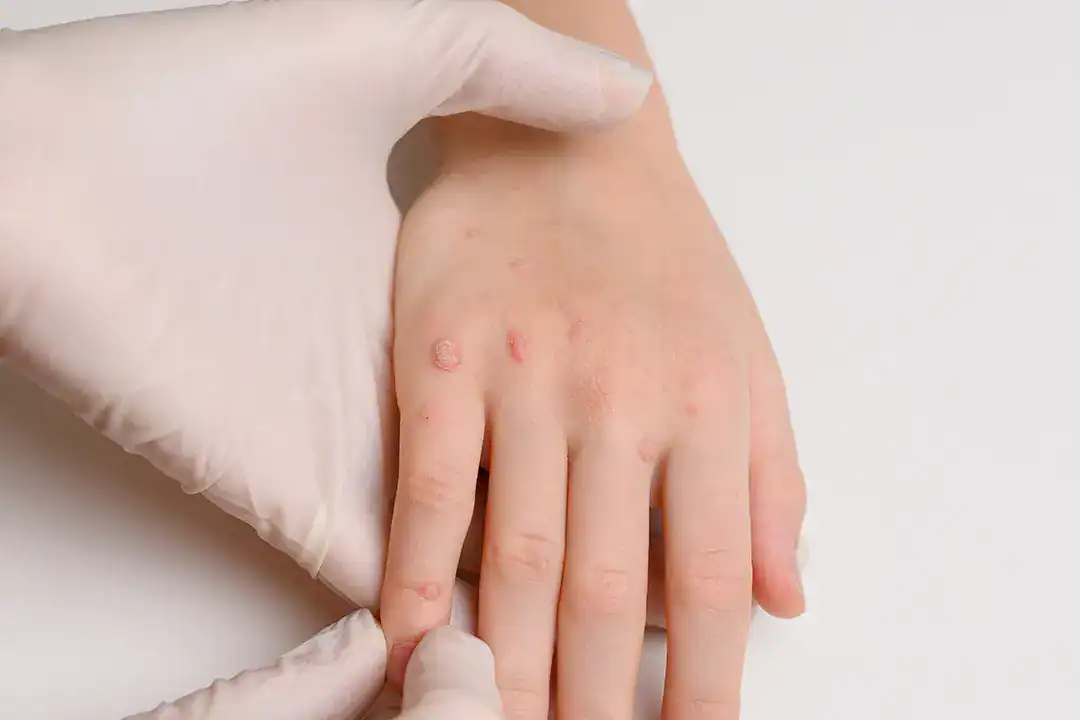
What do flat warts look like?
Flat warts are small, usually 1-5 millimeters wide. They are slightly raised and tend to be round or oval. They’re often the same color as your skin, though they may be pink or yellow brown.
Flat warts commonly appear on the face, legs and back of the hands. Even though they’re small, they tend to show up in clusters of 20 to 100, so they can be hard to miss.
What causes flat warts?
Like all warts, flat warts are caused by human papillomavirus (HPV), a common and contagious virus. They can be caused by one of four strains — different from the strain that causes flat genital warts.
You can contract the strains of HPV that cause flat warts through cuts or breaks in the skin, especially nicks from shaving. That may explain why flat warts are common in young people who are just learning to shave, and why women tend to see flat warts on their legs while men get flat warts on their face, including the beard area.
Other risk factors for flat warts include:
- Close contact with someone who has HPV
- Touching something handled by a person with HPV
- Poor hygiene
- Having a weakened immune system
Other skin conditions that look similar to flat warts
It’s easy to confuse flat warts with other skin conditions. Brown flat warts, for example, can sometimes resemble age spots or small moles, while pink ones could look like acne. Flat warts can also be mistaken for skin tags, milia and seborrheic keratoses.
Flat wart vs. skin tag
Some skin tags are connected to the skin by a stalk, but others are fixed on the skin and can look like flat warts when they’re small. Location is one way to help distinguish the two: Skin tags usually appear on areas where the skin folds, such as the eyelids, underarms and beneath the breasts.
Milia vs. flat warts
Small bumps on your face? They could be small cysts called milia. Flat warts and milia share several traits—they’re both small, can be yellowish and appear in clusters. But flat warts have a flat top, whereas milia are firm, domed-shaped bumps. Flat warts can occur on the face, hands or legs, but milia occur mainly on the face. And while milia can be yellowish, they are often pearl-colored.
Flat wart vs. seborrheic keratoses
Like flat warts, benign skin growths called seborrheic keratoses are round or oval and at least slightly raised. But they’re typically rough, with a lumpy surface. They may look scaly, waxy and “pasted on.” They can be light tan, brown or black.
Flat wart treatment
Flat warts usually go away on their own, but it can take months or years. If you don’t want to wait, you can try to treat them at home with an over-the-counter wart remover that contains salicylic acid. (Ignore any wart home remedies you see online—some could burn and even scar your skin.) If you don’t see results, visit your dermatologist.
The usual wart treatments, such as freezing them with cryosurgery or burning them with an electric needle and then scraping them off, typically aren’t ideal for treating multiple flat warts. Chemical peels are often a better bet. Your dermatologist may prescribe prescription-strength salicylic acid, glycolic acid, tretinoin or some combination of these topicals for you to apply to the flat warts at home every day.
Laser treatment is another option, as is photodynamic therapy. In photodynamic therapy, the doctor applies a topical medicine that damages the DNA of fast-growing cells and activates the medicine with light, usually from a laser.
Is there any way to prevent flat warts?
Protecting your skin from HPV viruses involves the same strategies as protecting it from other microbes.
- Keep your skin clean and dry.
- Avoid skin-to-skin contact with anyone who has flat warts.
- Don’t share personal items such as towels or clothing with anyone who has flat warts.
- Wear flip-flops at the pool and in locker rooms and public showers.
- Don’t bite or chew your fingernails or cuticles.
- Clean cuts and scratches with soap and water.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Common Viruses of the Skin & What You Should Know
Common viruses of the skin include Molluscum Contagiosum, warts, and Herpes Simplex Virus Type 1 and 2. These viruses are common because they are contagious with skin-to-skin contact. Although most are only an annoyance, some do have the potential to cause harm to the person affected. Our goal at Water’s Edge Dermatology is to educate and alleviate any possible concerns of our patients.
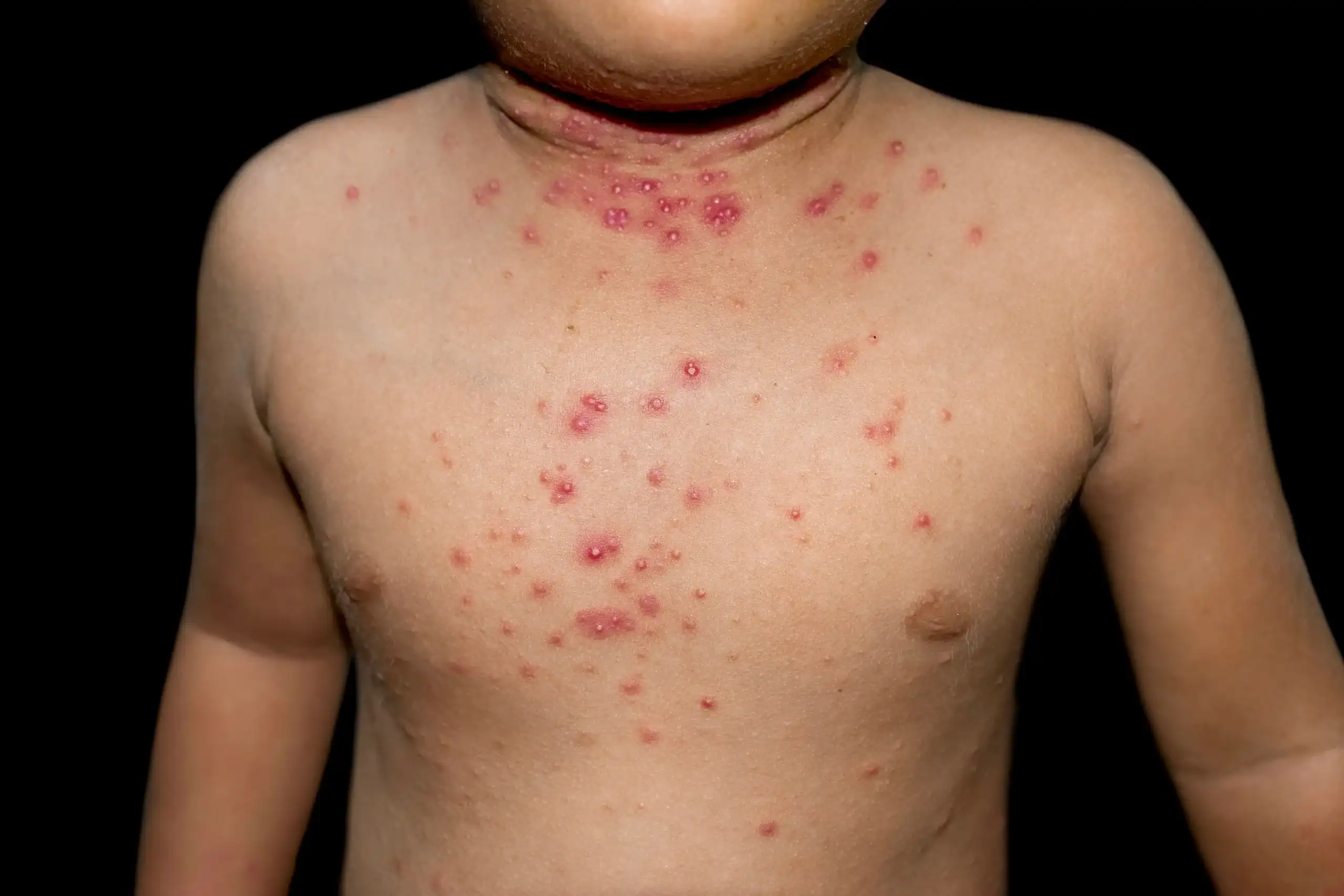
Molluscum Contagiosum is a common skin condition, especially in children, that comes from the Poxvirus. The virus presents as small umbilicated blisters and is usually diagnosed by a trained eye but can be confirmed with a biopsy. Contagiosum is an adjective that well describes the condition because it is so contagious. Children have more skin-to-skin contact and a lower immunity than adults, explaining why it is more commonly seen at a younger age. There are treatments such as liquid nitrogen or Cantharone (a topical agent) that are often used if the condition is bothersome or spreading. Treatment is not necessary because Molluscum Contagiosum is not harmful and with time should go away on its own. This condition can be sexually transmitted, but more commonly is spread by touching or scratching the area. Helpful tips for prevention include avoiding direct skin-to-skin contact, avoid sharing towels with someone who is infected, frequent hand washing and protecting the skin's barrier by keeping it well moisturized.
Warts are caused by a virus called the Human Papilloma Virus (HPV), which is easily transmitted. Warts are also more common is children because their immunity is lower than adults. Most often, warts are diagnosed by a trained eye but can also be confirmed by a biopsy. There are different types of warts including common warts, flat warts, plantar (under the surface of the foot) warts, and genital warts. Treatment may be the same as for Molluscum Contagiosum and is also a condition that may resolve on its own. Warts are typically raised but can be flat as in the flat warts or on the plantar surface of the foot. If warts are found in the genital region, they are usually considered to be sexually transmitted. However, common warts can also be transferred to the genitalia. Warts can be eradicated with treatment but they can return. Women who have a partner diagnosed with genital warts are at a higher risk for cervical cancer and should have regular pap smears. Helpful tips for prevention include frequent hand washing; avoiding skin-to-skin contact with affected areas; wearing shoes in locker rooms, water parks, public pools and public showers to protect the feet; and protecting the skins barrier by keeping it well moisturized.
Herpes Simplex Virus (HSV) has two types (I and II), that when active, present with blisters or sores that can be painful. Type I is the cold sore virus and is generally found on the face, and type II is the sexually transmitted virus that is typically found in the genital area. However, type I has been found in the genitalia and type II has been found in other parts of the body. Once exposed to the virus, it may lay dormant for a long period of time, or may be such a mild case making it difficult to identify the source of infection. Stress and sun exposure can activate the dormant virus. HSV is contagious during flares but can also be contagious when no lesions are present. HSV is most commonly diagnosed by a trained eye, but a viral culture or blood work can be taken to confirm the diagnosis. HSV is treatable but there is no cure. Symptoms that may indicate the virus is active include tingling, itching, tenderness or burning sensation in the affected area. The treatment is antiviral medications like acyclovir or valacyclovir. If the medication is taken at onset, the symptoms may be minimized and the duration may be shortened. The symptoms will go away on their own with no treatment but may take longer than with the medication. Tips for prevention include avoiding skin-to-skin contact to the affected area of a person with known HSV and avoiding sharing drinks, towels, lip balms or other products that may come in contact with the affected area.
These are some of the most common viruses of the skin but certainly not all of them. The key is early diagnosis and prompt treatment for any condition. Proper hand washing may not prevent these conditions, but is the number one way to avoid spreading infections. If you have any questions, please feel free to contact any of our offices. We are happy to help you in any way we can.