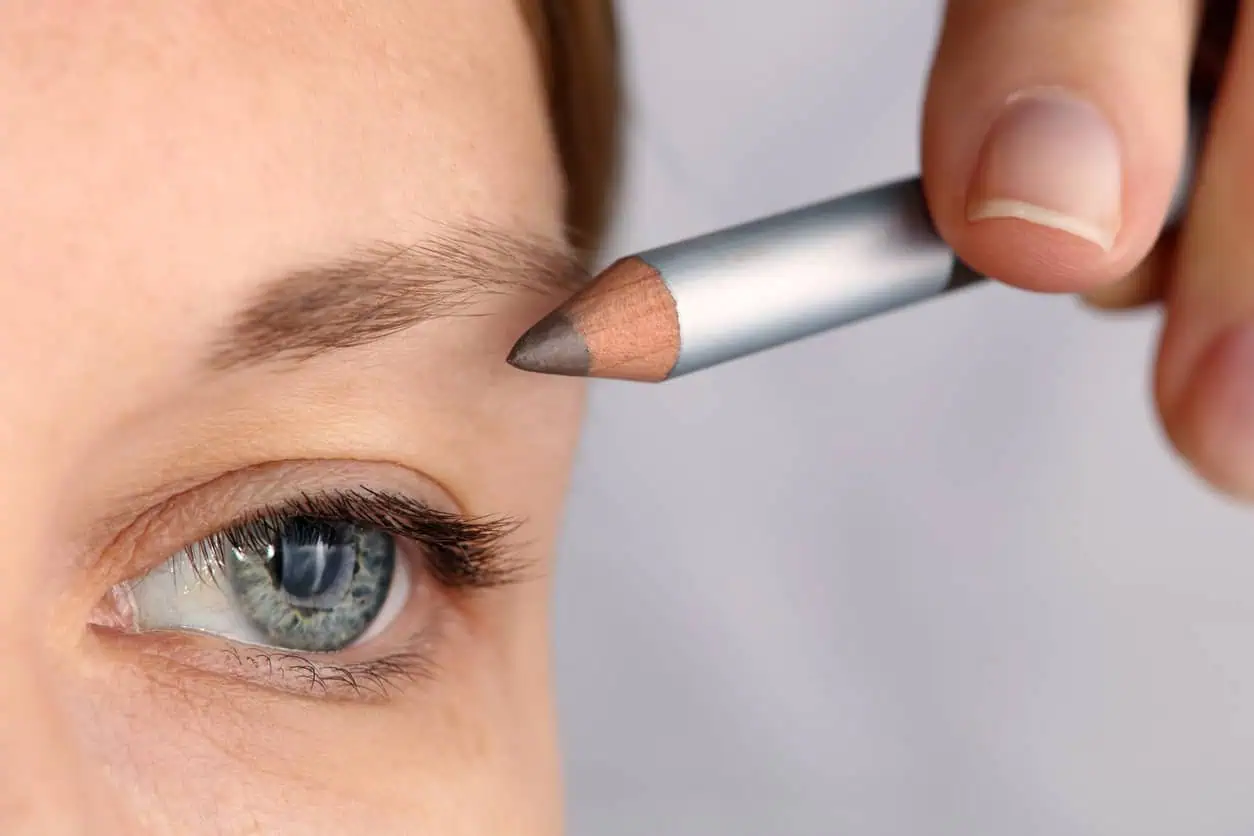
Eyebrow Thinning: Why It Happens and What You Can Do
Medically Reviewed By: Ted Schiff, MD
Are thinning eyebrows making you regret all the plucking you did in your younger years? If your eyebrows are pulling a disappearing act, you’re not alone — eyebrow hair loss is common after a certain age. Here’s what to know about why eyebrow thinning happens, and when it might signal an underlying condition.
Why are my eyebrows thinning?
Blame most cases of eyebrow thinning on aging. Eyebrows start to look sparse due to the natural decline of testosterone (in men) and estrogen (in women) that begins in the 40s. Both of these hormones affect the hair growth cycle and the structure of the hair follicles. Eyebrows thin over time as the hair shafts become finer and some of the follicles stop producing hair.
While aging is a common cause of eyebrow hair loss, many other factors can contribute to eyebrow patchiness and thinning.
Skin conditions
When they affect the eye area, contact dermatitis, atopic dermatitis and seborrheic dermatitis can thin your eyebrows. All three cause itching, so you may lose eyebrow hair if you’re constantly scratching and rubbing. Atopic dermatitis and contact dermatitis also cause inflammation that can interfere with normal eyebrow hair growth.
Tinea capitis (ringworm), a fungal infection of the skin, can thin your eyebrows if its telltale red and ring-like patches develop on the brow.
Thyroid disorders
If your thyroid gland is secreting too little thyroid hormone (hypothyroidism) or too much thyroid hormone (hyperthyroidism), this can interfere with normal hair follicle functioning, leading to thin eyebrows.
Pregnancy and childbirth
Thanks to fluctuating hormone levels, eyebrows may thin during pregnancy and the postpartum period.
Nutrient deficiencies
What you eat can affect the health of your hair. Eyebrow hairs may fall out if you’re not getting enough protein, zinc, biotin or iron.
Telogen effluvium
This form of temporary hair loss most commonly affects the hair on the scalp, but in severe cases it can cause eyebrow hair loss as well. Telogen effluvium develops in response to stress caused by surgery, infections and other physically taxing events.
Autoimmune diseases
Eyebrows may look patchy if you have alopecia areata, an autoimmune disease in which the immune system attacks the hair follicles, slowing or stopping hair production. Another type of alopecia, frontal fibrosing alopecia, can cause eyebrows to disappear. Other autoimmune diseases that lead to eyebrow thinning or loss include psoriasis and certain forms of lupus.
Medication
Undergoing chemotherapy sometimes causes eyebrow thinning because the drugs damage the hair follicles. Other medications that can cause eyebrow loss include anti-thyroid drugs, cholesterol-lowering drugs, blood thinners and valproic acid, used to treat seizures and bipolar disorder.
Trauma
Burns and injuries to the eyebrow can cause hair to fall out.
Over-tweezing or pulling
Over time, tweezing your eyebrows can damage the hair follicles, impairing hair regrowth. So can pulling out the eyebrow hairs, something people with a hair pulling condition called trichotillomania may do. If the follicles become scarred, the hair may not grow back.
How to treat eyebrow thinning
In some cases, your eyebrows will grow back over time, particularly if your eyebrow thinning was caused by telogen effluvium or another non-scarring condition. The treatments below encourage eyebrow hair regrowth.
Latisse
Your doctor may recommend the prescription treatment Latisse to help restore thinning eyebrows. It’s FDA-approved to treat thin eyelashes, but studies suggest it can be used off-label to regrow eyebrows.
Rogaine
Minoxidil (Rogaine), which is available over the counter, isn’t intended for eyebrows, but some people use it there. Use the 2% solution and apply it to your brows with a cotton swab. Be extremely careful not to get it in your eyes, and don’t get it on other areas of your face or you could see unwanted hair growth there.
Corticosteroids and Anthralin
If you lost your eyebrows due to alopecia areata, your doctor may recommend injecting the areas with corticosteroids to encourage hair regrowth. Anthralin, a topical anti-inflammatory cream used to treat psoriasis, can also be helpful for people with eyebrow hair loss caused by alopecia areata and other inflammatory conditions.
Making thin eyebrows look thicker
While you’re waiting, or hoping, for your eyebrow hair to grow back, there’s plenty you can to do to make your eyebrows look thicker and fuller.
Eyebrow makeup
Tinted brow mascara, eyebrow pencils, pens, powders and pomade fill in sparse eyebrows.
Microblading and microshading
These semi-permanent makeup treatments can make brows look fuller for months. During a microblading session, a cosmetic technician applies pigment in natural, hair-like strokes to the skin under your brows with a blade. If you prefer the look of powdered brows, opt for microshading, in which the pigment is applied in tiny dots. Microblading lasts for six to eight months, while microshading lasts for three to six months.
Hair dye
Permanent or semipermanent hair dye can make your eyebrows look fuller and thicker. Getting hair dye in your eyes is a major no-no, so if you want to dye your eyebrows, have a licensed medical aesthetician do it.
Hair transplant
This is the most permanent solution for eyebrow hair loss. A plastic surgeon extracts hair follicles from your head and places them in tiny slits made in your eyebrows. The procedure is very time-consuming, and more than one treatment session is usually necessary. Eyebrow transplant surgery is also expensive, though it may be covered by health insurance if you lost your eyebrows due to an accident or health condition.
Article Written By: Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Why Do I Bruise So Easily?
Medical review by Brian Klein, PA-C
If you’re bruising easily, even when you don’t remember banging yourself, you’re not alone, especially if your younger days are behind you. Often, the answer to “why do I bruise so easily?” is thin skin.
“In many cases, easy bruising is due to normal skin aging,” said Brian Klein, PA-C, a physician assistant at Water’s Edge Dermatology. “You usually see it when you’re in your 70s or sometimes as early as your 60s, which is when your skin is naturally getting thinner.”
Age-related causes of easy bruising
As you get older, your skin produces less collagen, a protein that keeps skin looking firm and plump. When collagen production declines, the dermis — the middle layer of skin that makes up 90% of skin’s thickness — shrinks. The layer of fat beneath the skin also diminishes. In a nutshell, thin skin is the reason many seniors bruise easily.
Eventually, skin becomes fragile and crepe-like to the point that you can easily see structures such as tendons and capillaries in certain areas of your body, including your hands and arms.
“As collagen and fat decrease, the blood vessels lose the cushioning that once protected them from injuries,” Klein said. As a result, vessels become damaged more easily and leak blood that pools under the skin, causing a bruise.
To make matters worse, the blood vessels in the dermis weaken over time, so even the slightest trauma can rupture them and lead to substantial bruising.
RELATED: 8 Common Skin Conditions in Elderly Adults
Other causes of easy bruising
Aging isn’t always to blame for easy bruising. Here are other possible culprits. If you’re younger and you bruise easily, talk with your doctor.
Nutritional deficiencies
You may bruise easily if you’re low in vitamin C or vitamin K. These vitamins are important for blood clotting. A doctor can diagnose nutritional deficiencies with a blood test.
Health conditions
Among the health conditions that may cause easy bruising are:
- Bleeding disorders such as hemophilia and von Willebrand disease
- Endocrine disorders such as Cushing’s disease
- Genetic disorders such as Marfan syndrome
- Connective tissue disorders such as Ehlers-Danlos syndrome
- Certain types of cancer, including leukemia
- Liver disease
Medications and supplements
You may bruise easily if you take medications that reduce the blood’s ability to clot, including aspirin and prescription blood thinners. Other medications that may lead to easy bruising include ibuprofen, naproxen, certain antibiotics, corticosteroids, glucocorticoids, and antidepressants. Don’t stop taking any prescription medicine without talking to your doctor first.
Some supplements can also impair blood clotting and cause easy bruising. These include fish oil, gingko, and ginseng.
Alcohol abuse
Excessive drinking can lead to serious liver diseases such as cirrhosis, which can prevent the liver from producing proteins necessary for blood clotting. As cirrhosis worsens, easy bruising may develop.
How to treat a bruise
Most bruises fade with time. How long does a bruise take to heal?
“If it’s on your face, it will usually fade in a week, whereas bruises on your legs may take two to four weeks to go away,” Klein said. “But the healing process may take longer if you’re older and have thin skin.”
If you bruise easily, these tips can help you speed up the healing.
Use the RICE technique right away
RICE (rest, ice, compress, elevate) enhances the healing process. Rest and elevate the bruised area and apply an ice pack wrapped in a thin towel for 10 to 20 minutes several times a day. If the area is swollen, use an elastic bandage to compress it. Wrap it snugly but not so tight that it cuts off circulation.
Apply Dermaka cream to the injured area
“Dermaka cream contains many natural ingredients that have been shown to reduce bruising, such as arnica, bromelain, and vitamins A and E,” Klein said. It works even better than arnica alone.
How to minimize bruising
In most cases, there isn’t a lot you can do to reverse easy bruising, but depending on your situation, these strategies may help.
Wear sunscreen every day. Ultraviolet light from the sun breaks down collagen, accelerating thinning of the skin and leaving blood vessels more vulnerable to injury. Apply a broad-spectrum sunscreen with an SPF of at least 30.
Reconsider taking supplements. “When it comes to supplements that cause easy bruising, talk to your doctor to see if you really need to take them,” advised Klein.
Get treatment for alcoholism or cirrhosis. If you abuse alcohol, talk to your doctor about ways to quit. It’s also very important to see your doctor if you have signs or symptoms of cirrhosis. Early signs and symptoms include unintended weight loss, poor appetite, nausea, vomiting and mild pain in the upper right side of the abdomen.
Quit smoking. The chemicals in cigarettes interfere with collagen production and slow the healing of skin injuries.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How to Get Rid of Milia Without Scarring Your Skin
Medically reviewed By: Ted Schiff, MD
If you’ve noticed tiny white or yellow bumps on your face, you may have assumed they were whiteheads. But if the bumps are much firmer than whiteheads and aren’t inflamed, chances are you have milia. Since you can't pop them like a pimple, the question is how to get rid of milia.
“Milia and acne are two different issues,” said Ted Schiff, MD, founder, and chief medical officer of Water’s Edge Dermatology. “Milia develop in very small hair follicles or in the sweat ducts in your skin, not in the pores.” Milia on the eyelid and other parts of the face such as the cheeks and nose are particularly common, though these pearl-like cysts can appear anywhere.
What causes milia?
Primary milia sometimes referred to as “milk spots,” form when a protein in skin cells called keratin becomes trapped under the top layer of skin.
“The skin is constantly exfoliating itself, shedding old skin cells and replacing them with new ones,” said Dr. Schiff. “But if some of the old skin cells don’t fall off, they can get trapped under new skin and harden.”
Primary milia is the most common type of milia in adults. It’s also common in newborns. Newborn milia typically appear on the face, scalp, and upper torso and heal on their own within a few weeks.
Another type of milia, called secondary milia, can happen when the skin heals after it’s injured or damaged by a blistering rash (such as a poison ivy rash), a burn, long-term use of steroid cream, or years of sun damage. Using products that are too heavy for your skin type can also cause secondary milia, which may be harder to treat than primary milia.
Get rid of milia: Treatments options
Milia often go away on their own within a few months, but sometimes they can persist for years. They are harmless, but if they bother you, seek professional help. Your dermatologist knows how to get rid of milia.
“People sometimes try to remove milia themselves by popping them as they would pimples,” said Dr. Schiff. “But milia have a very hard texture, and you can’t get rid of them without making an incision in the skin.” Trying to pop a milium (one cyst) can lead to scarring.
Another benefit of seeing a dermatologist: He or she can confirm that the cysts are milia and not something else, such as basal cell carcinoma, which can appear as white, pearly bumps.
Keep in mind that even most professional milia removal treatments carry some risk of scarring, so it’s important to weigh the risks and benefits with your dermatologist before proceeding. Here are the techniques a dermatologist may use.
De-roofing
The simplest way to remove milia is through de-roofing. The dermatologist cuts a tiny opening in the top of the cyst with a lancet and pushes out the keratin plug using a tool called a comedone extractor. You’ll feel a mild prick, nothing more. De-roofing is one of the safer milia removal options for people with dark skin, who are particularly vulnerable to developing dark patches known as post-inflammatory hyperpigmentation after certain skin treatments.
In most cases, de-roofing can be used to remove milia on the eyelid. “Occasionally, if they are large or numerous or close to the eyelid margin, we refer the patient to an ophthalmologist,” said Dr. Schiff.
Laser ablation
This is a milia removal option a dermatologist might choose if you have multiple milia. Laser energy is used to break down the trapped keratin and encourage it to be reabsorbed in the skin. Laser treatments may not be recommended for people with dark skin.
Chemical peel
A mild chemical peel can treat milia by removing the top layer of skin, revealing new, smooth skin. The skin care provider applies a solution containing glycolic acid or salicylic acid to exfoliate the affected skin. Pain relief usually isn’t necessary for mild peels, which cause only a slight stinging sensation.
Cryotherapy
In this less-common procedure, liquid nitrogen is applied to the milia. It freezes and destroys the cysts. You may experience swelling or blistering that disappears in a few days. This treatment may not be recommended if the milia are near the eyes, since the skin in the eye area is thin and delicate.
Tretinoin or oral antibiotics
Cases of a rare type of milia called milia en plaque, which appears as multiple milia on top of a raised red patch of skin, may go away with a prescription retinoid called tretinoin or an antibiotic called minocycline. Milia en plaque often occurs in people with an autoimmune condition or genetic skin condition such as discoid lupus or lichen planus.
Milia treatment at home
There are a few things you can do at home to encourage milia to go away and to avoid developing more of them.
Try using an exfoliating cleanser that contains salicylic acid, citric acid or glycolic acid once a week or more.
At-home chemical peels that contain salicylic acid or glycolic acid can also be helpful, but ask your dermatologist for advice on the best product to use. If you use one that’s too harsh for your skin, you could develop irritation or secondary milia.
Applying a prescription retinoid or over-the-counter retinol product once a day can help treat and prevent milia by speeding up cell turnover.
Finally, don’t forget to use sunscreen to protect your skin from burns and other sun damage that can lead to secondary milia.
Article Written By: Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Sleep and Skin: The Benefits of Beauty Sleep
Most of us have joked about needing our beauty sleep, but is beauty sleep a real thing? When it comes to the skin, the answer is an unequivocal yes.
While you log the recommended seven to nine hours of sleep a night, your skin gets busy repairing the damage it incurred during the day. The connection between sleep and beauty is so strong that a few nights of scant sleep can noticeably affect your appearance.
In one small study, getting only four hours of sleep significantly reduced skin hydration. After four nights of sleep deprivation, skin texture worsened. Skin’s elasticity — its ability to stretch and snap back into place — was affected most of all by lack of sleep. When skin loses elasticity, it can look wrinkled, saggy or leathery.
How beauty sleep works
During the day, your skin is subject to a variety of assaults, including the sun’s ultraviolet (UV) rays, which damage the DNA in skin cells, leading to premature aging and potentially, skin cancer. Air pollution is also linked to prominent signs of aging, such as pigment spots and wrinkles. Other environmental stresses that affect the skin include smoking and exposure to certain chemicals.
Fortunately, a number of processes occur during sleep or after sleep that enables your skin to tackle the damage.
Growth hormone production
Shortly after you fall asleep, your body begins secreting somatotropin, also known as human growth hormone (hGH), which plays a crucial role in the development, maintenance, and repair of skin. Notably, hGH is required for the production of collagen, a protein found in the skin that makes it look plump and youthful.
Increased blood flow
Sleep promotes blood flow to the skin, making it look healthier and giving it an attractive flush. When blood flow is compromised from lack of sleep, you can end up looking pale. In addition, blood can collect under the eyes, causing dark circles. The fluid that builds up on the eyelids and orbits (eye sockets) can leave you with puffy eyes.
Reduced cortisol production
A good night’s sleep helps keep a lid on daytime production of cortisol, the “stress hormone.” Lack of sleep, on the other hand, may cause your body to produce more cortisol. Too much cortisol can affect your skin’s appearance in many ways, causing acne breakouts, dryness and destruction of collagen.
9 tips for getting more beauty sleep
To wake up looking refreshed, get enough good-quality sleep. Harder than it sounds? Try these tips.
1. Create a sleep schedule
Aim to go to bed and wake up at the same times every day. Sleeping late on your days off is tempting, but following a consist sleep routine, even on weekends, makes it easier to fall asleep at the right time, leaving yourself enough hours to get the ZZZs you need. If you’ve been staying up late, start going to bed earlier in 15- to 30-minute increments over several days until you reach a bedtime that allows you to get sufficient shuteye.
2. Develop a bedtime routine
They’re not just for toddlers! Start winding down for bed at least 30 minutes beforehand to get in sleep mode. Do relaxing activities such as stretching, reading or practicing deep breathing. Avoid any activities that can keep you alert, including looking at your computer, cell phone or tablet. Screens emit blue light, which can interfere with your body’s production of melatonin, the hormone that tells your body it’s time to sleep.
3. Keep your bedroom dark and quiet
Light can disrupt your circadian rhythm, which controls your sleep-wake cycle. Wear a sleep mask or put up light-blocking curtains to keep your room as dark as possible. Tune out noise by running a fan or white noise machine or wearing earplugs.
4. Adjust the temperature
Feeling too hot or too cold can interfere with sleep. Studies show that in general, the ideal temperature for sleep is around 65°F, though your ideal may be different.
5. Nap the right way
If you need a nap, take it in the early afternoon and limit it to 20 minutes. Long, late afternoon naps can make it harder to fall asleep at night.
6. Make some lifestyle changes
Certain habits can make it harder to fall asleep at night. These include eating big, spicy or fatty meals late at night, drinking caffeine late in the day, drinking alcohol before bed, smoking, and being sedentary.
7. Take a morning walking in the sunshine
Exposure to sunlight early in the day can help you sleep at night.
8. Use your bed only for sleep and sex
Doing work in bed can make your brain associate bed with work, which won’t help you fall asleep when the time comes.
9. Use sleep medications only as directed
It’s safe to take an over-the-counter sleep medication, such as ZzzQuil or Unisom, for the occasional bout of insomnia, but these drugs aren’t intended for long-term use. Take them too often and you may build up a tolerance, which means they won’t work as well. If you regularly have trouble falling asleep, see your doctor.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
From Stains to Allergies: Hair Dye Tips to Save Your Skin
Medical review by Camila Yepes, PA-C
Dyeing your hair is a fun way to change up your look or keep the grays from showing. But for some people, it’s not as simple as dyeing, rinsing and enjoying. For those with a hair dye allergy or sensitive skin, itching and inflammation can take the fun away.
Then there are those annoying hair dye stains. If certain dyes get on your face or fingers, the stains can seem impossible to remove, sending you running to your nearest electronic device to Google “How to get hair dye off skin.”
Camila Yepes, PA-C, a physician assistant at Water’s Edge Dermatology, has these tips to help make your next dye job a success.
Do you have a hair dye allergy or sensitivity?
Allergic contact dermatitis is a skin allergy to a common substance, and hair dye can be one of those substances. Hair dye reactions are also triggered by sensitivities, which are different from allergies. Irritant contact dermatitis happens when an irritant aggravates the skin by damaging its outer layer.
“You can develop a hair dye allergy or a sensitivity to the ingredients in your hair dye at any time,” said Yepes. “It can happen even if you’ve been dyeing your hair with the same product for years.”
If you develop a reaction to the dye, each time you dye your hair, the reaction may happen faster (in a few days or a few hours), be more severe and last longer.
Most reactions to hair dye are caused by an ingredient called paraphenylenediamine (PPD), found in permanent dye and some semi-permanent dyes. You’re more likely to develop a reaction if you use darker shades of dye, which contain more PPD.
“PPD is a popular ingredient in hair dye because it provides long-lasting color,” said Yepes. “Its potency is also what makes any dye stains you get on your skin so hard to remove.”
PPD allergies are relatively uncommon, affecting 5% of people in the U.S. “Sensitivities are more common, particularly in people who have eczema,” said Yepes.
Hair dye allergy and sensitivity symptoms
Whether you’re allergic to PPD or just sensitive to it, the symptoms are largely the same. They can include swelling, peeling, a red rash and stinging or burning. Both allergies and sensitivities can cause itching, though it’s more likely to be a major symptom if you’re allergic to PPD.
Blistering is more common in allergic reactions, while sensitivities are more likely to make skin dry and cracked.
In rare cases, a hair dye allergy can trigger a potentially fatal allergic reaction called anaphylaxis, which can cause swelling of the tongue and throat, difficulty breathing, nausea and vomiting. Your risk of anaphylaxis is higher if you’ve had it before or if you have allergies or asthma and a family history of anaphylaxis.
How to avoid hair dye reactions
Avoiding reactions comes down to taking a few precautions and switching hair dye if you need to.
Always do a patch test. Before applying the dye, dab a small amount on a patch of skin in an inconspicuous area, then wait 48 hours. Reactions don’t always happen immediately, so don’t cut the time short. If the skin swells, turns red, burns or itches, you shouldn’t use the dye. If you develop symptoms of anaphylaxis, call 911 or go to the ER immediately.
Protect your skin in advance. Cover areas that may come in contact with the dye, such as the hairline, ears and neck, with petroleum jelly to prevent the dye from spreading beyond your scalp. Wear gloves to protect your hands.
Try a PPD-free hair dye. If you’re allergic to or sensitive to hair dye, ask your colorist to use PPD-free dye. While there is no special hair dye for eczema sufferers, PPD-free options may be less likely to cause a problem. If you’re coloring your hair at home, look for brands that don’t contain PPD, such as Madison Reed and Clairol Natural Instincts.
What to do if you have a reaction
If you develop a reaction to hair dye while it’s still on your hair, wash it out immediately with warm water and a mild shampoo. “Do this even if your symptoms are subtle because they could get worse,” said Yepes.
If you notice a reaction afterward, Yepes recommends applying an over-the-counter topical corticosteroid cream (0.5-1% hydrocortisone) to ease discomfort and inflammation. If you also feel itchy, taking an antihistamine medication such as Benadryl can help.
Symptoms often go away on their own or with home treatment, but if they don’t, or if you see signs of infection, such as pus, call your dermatologist.
How to get hair dye off skin
Hair dye stains are the other “dark” side of PPD. If you get dye on your skin, wipe it away ASAP to prevent it from sinking in.
If you see stains after you’ve dyed your hair, start by washing the area with soap and warm water. For more set-in stains, rub the area with olive oil and leave the oil on your skin for up to eight hours. This is the best approach for people with sensitive skin. If sensitivity isn’t an issue, dab the stain with rubbing alcohol or non-gel toothpaste and let it sit for 5 to 10 minutes before washing it off.
Stains on the hands can be removed by rubbing a cotton ball dipped in nail polish remover on the skin for a few seconds, or doing the same with a paste made of gentle dish soap and baking soda.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Mole Removal: Your Questions Answered
Medically Reviewed By: Kelli Bryant, MD
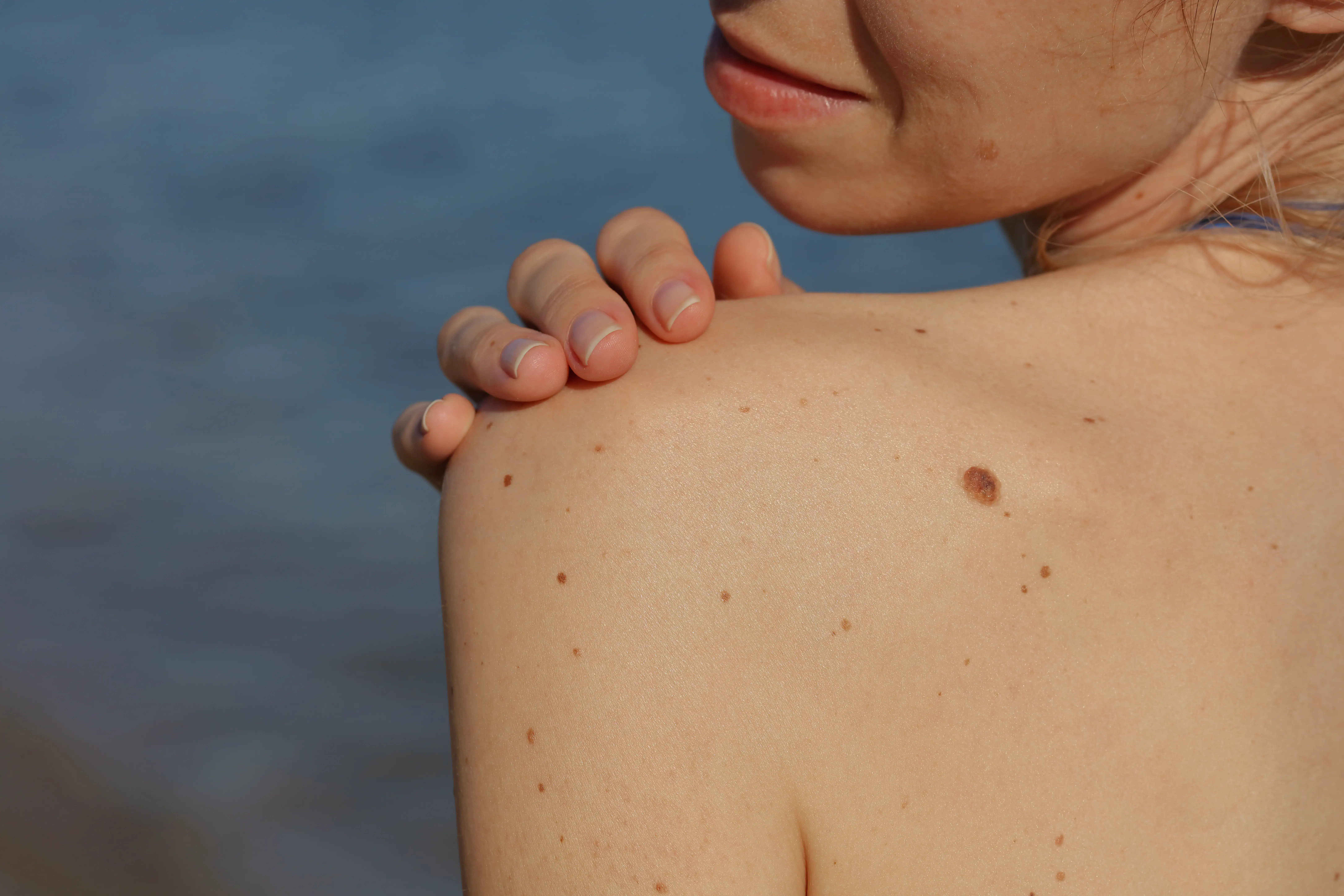
Moles, also called nevi, are sometimes considered beauty marks. But if you have a mole — especially a facial mole — that’s more of an eyesore, or if a mole is easily irritated by clothing or gets snagged on jewelry, chances are you’d rather be rid of it.
Can you remove moles? The answer is often yes. For many moles, mole removal at your dermatologist’s office is an option.
Here, Kelli Bryant, MD, a board-certified dermatologist at Water’s Edge Dermatology, answers common questions about mole removal and explains why you shouldn’t attempt it at home.
Do moles have to be removed?
In most cases, whether or not to remove a mole is entirely up to you. But if the mole shows signs of skin cancer, your dermatologist may have to remove it. Suspicious (atypical) moles are identified using the ABCDE rules:
- A for Asymmetry. One part of the mole doesn’t look like the rest of it.
- B for Border. The border of the mole is irregular or poorly defined.
- C for Color. The mole is multi-colored. You may see shades of tan, brown or black along with red, white or blue areas.
- D for Diameter. The mole is larger than 6 millimeters, which is about the size of a pencil eraser.
- E for Evolving. The mole is changing in shape, size or color.
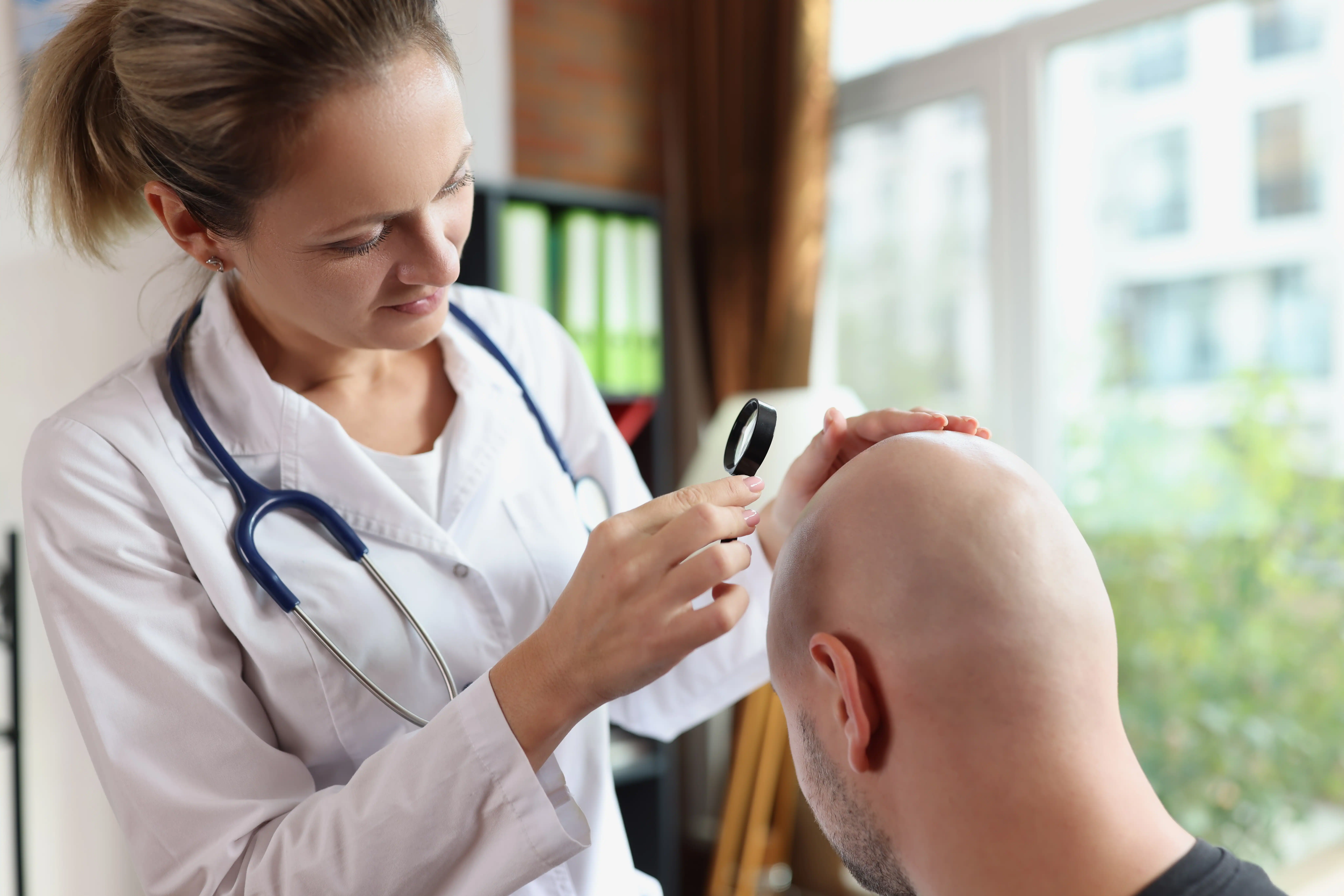
Do atypical moles need to be removed? Not necessarily. “Many benign moles break the ABCDE rules,” Dr. Bryant said. Still, you should have any suspicious mole evaluated by a skin care provider, who may biopsy it to check for cancer.
Is there an effective way to remove moles at home?
At best, home remedies and over-the-counter mole removal tools are a waste of time and money. But in some cases, mole removal at home can be downright harmful.
“Some of the home remedies you see online, such as applying iodine or apple cider vinegar to the mole, can cause a lot of skin irritation, to the point that it’s almost like a chemical burn,” Dr. Bryant said.
Other purported DIY treatments, such as taping a banana peel or garlic clove to the mole, may not be as dangerous but are equally ineffective. What about using a mole removal cream or cauterizing (burning) the mole with a mole removal pen? Those approaches won’t make a mole disappear and may lead to scarring and pitting.
“If those products should happen to work, it’s because the ‘mole’ was actually a different type of skin growth, such as a seborrheic keratosis,” Dr. Bryant said.
Never attempt to remove a mole with a razor blade or scissors. The risk of infection and scarring is far higher than if you have a mole removed professionally. Cutting off a mole at its base with a razor blade can cause profuse bleeding. Also, the risk of mole recurrence after removal is higher if you try to slice off the mole yourself, simply because you probably won’t get it all.
Even if any of these approaches did work, it’s still a bad idea to remove a mole yourself, Dr. Bryant said. “Any mole, no matter how benign it looks, could be malignant, so you should always see a dermatologist to have it evaluated and removed safely.”
How do dermatologists remove moles?
Water’s Edge Dermatology providers offer two mole removal options: shave excision and punch biopsy. Laser mole removal is not an effective method.
Shave excision for raised moles and large moles
Shave excision is the most commonly used mole removal technique and is typically recommended for raised or large moles. The provider injects the treatment area with a local anesthetic, then shaves off the mole with a surgical blade.
Shave excisions can be superficial or deep. If the mole is benign, it’s cut down to the level of the surrounding skin. But if the mole looks suspicious, the dermatologist will likely perform a deep shave excision, or saucerization biopsy. In this case, a curved blade is used to remove the mole and layers of tissue beneath it so they can be checked for cancer cells. Stitches usually aren’t needed to close superficial excisions, but they are often needed for deep ones.
If your mole is very large, you may choose to have it removed by a plastic surgeon rather than a dermatologist in case any reconstruction work is necessary.
Punch biopsy for small moles, flat moles and penetrating moles
For moles that are small, flat or penetrate deeper into the skin, your skin care provider may recommend a punch biopsy.
After injecting an anesthetic, the provider inserts a pen-like instrument into the skin under the mole. The instrument has a sharp end that looks like a tiny round cookie cutter. The device is rotated until the end cuts through the epidermis and dermis and into the fat below. Next, the mole and the plug of tissue beneath it is pulled from the skin with forceps and snipped away with surgical scissors. The area is closed with a few stitches.
Will I have a scar after mole removal?
Removing a mole always creates a scar, regardless of the technique used, Dr. Bryant said. You may be left with an area that’s lighter than the surrounding skin (a hypopigmented scar) or a line that can be either paler or darker than your skin tone.
Some people have an exaggerated scar response to mole removal in which thick, hypertrophic (raised) scars or keloids form. Hypertrophic scars and keloids are somewhat similar, but unlike hypertrophic scars, keloids can extend beyond the treated area.
“If you have a history of keloid scars, it might be better to leave the mole alone,” Dr. Bryant said. Your dermatologist will discuss the risks and benefits of mole removal to help you decide if you want to proceed.
If a mole removal scar does develop, scar treatments are available that can lessen their appearance, such as pulsed dye laser treatments to remove redness and flatten raised scars and cortisone injections to soften firm scars.
Can a removed mole grow back after being removed?
Mole regrowth is possible, particularly if the mole was raised. The reason: “There are almost always some mole cells left behind when you remove a mole,” Dr. Bryant said.
Your dermatologist can try to remove the mole again if it regrows, but you may find that the regrown mole doesn’t bother you as much as the original. “When a raised mole returns, it usually doesn’t grow back to its original height, so it may be less noticeable,” said Dr. Bryant explained.
Make an appointment to discuss mole removal with a Water’s Edge Dermatology provider.
Article Written By: Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
What Is a Nurse Practitioner and What Do They Do?
Medical Review By: Dr. Ted Schiff
Many dermatology practices are staffed with multiple types of providers, including board-certified dermatologists, physician assistants, and nurse practitioners. What exactly is a nurse practitioner, and what are they qualified to do?
Unlike a registered nurse (RN), a nurse practitioner can diagnose and manage health conditions. RNs have an associate degree or bachelor’s degree in nursing, but NPs complete additional training and get an advanced degree — either a Master of Science in Nursing or a Doctor of Nursing Practice. They can prescribe medication and, depending on the state, work without a doctor’s supervision.
A nurse practitioner is a type of advanced practice registered nurse, or APRN. Water’s Edge Dermatology is proud to have many APRNs who specialize in dermatology on staff. They play an invaluable role in treating and educating patients.
Types of nurse practitioners
Nurse practitioners get one of several specialty certifications. Most NPs are family nurse practitioners, who care for patients of all ages. Other specialties include acute care, adult health, geriatric health, neonatal health, pediatric/child health, psychiatric/mental health, and women’s health.
Once they are licensed, NPs can pursue extra training in a sub-specialty if they want to focus on a particular area of medicine, such as dermatology, endocrinology, orthopedics, gastroenterology, or cardiovascular health.
Services nurse practitioners provide
Nurse practitioners can diagnose and treat acute and chronic medical conditions. For dermatology nurse practitioners, these might include severe sunburns, boils, acne, rosacea, eczema, psoriasis, cysts, warts, atypical moles, and skin cancer. They can order, perform and interpret tests. A dermatology nurse practitioner might order skin biopsies, for example, as well as screen patients for skin cancer.
NPs can also perform treatments. A nurse practitioner in a dermatology practice might perform minor skin excisions (for mole removal, for example), extractions and cryotherapy, and/or administer cosmetic treatments such as Botox injections, dermal fillers, laser treatments, and peels.
Finally, nurse practitioners teach patients healthy lifestyle practices, such as proper skincare, and educate them about disease prevention.
How to become a nurse practitioner
In most cases, candidates must have a bachelor of science in nursing (BSN) and then complete a Master of Science in Nursing (MSN) program or a Doctor of Nursing Practice (DNP) program to become an NP. People who have an Associate’s Degree in Nursing (ADN) but not a bachelor’s degree can enroll in an accelerated RN-BSN program or an ADN-to-MSN program.
Advanced nursing degree students take classes in subjects such as advanced health evaluation, ethics, and pharmacology, and they participate in clinical rotations to gain hundreds of hours of patient care experience. Candidates then take an exam administered by an accredited certifying body such as the American Academy of Nurse Practitioners Certification Board to become a nationally certified NP.
Nurse practitioners who want to specialize in dermatology can pursue a certified nurse practitioner (DCNP) credential. There are a few ways to do this — by entering a post-master’s-degree program, taking continuing education courses, or training on the job under a board-certified dermatologist or a highly skilled dermatology NP. To take the Dermatology Nurse Practitioner Certification Exam and earn a DCNP, nurses must have at least 3,000 hours of general dermatology practice. DCNPs must earn continuing education credits and be recertified every three years.
: Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets
Medical Review By: Dr. Ted Schiff
How to Remove Gel Nail Polish at Home
Medical review by Alissa O’Brien, MD
There’s a lot to love about gel manicures, particularly their durability. Unlike a traditional manicure, which can chip in just a few days, gel manicures can last for up to four weeks. The downside is that gel nail polish adheres to the nails so strongly that it can’t be wiped away with nail polish remover, so you have to return to the salon to have it removed. Or, you can remove gel nail polish at home, if you know how.
“Some people try to pick, peel, file or even bite off the polish, but that won’t work, and it can remove the top layer of the nail along with the polish, leaving your nail weak and damaged,” said Alissa O’Brien, MD, a board-certified dermatologist at Water’s Edge Dermatology.
8 Steps to Remove Gel Nail Polish
The better way is to soak off gel polish with acetone by following these steps. Don’t soak your entire fingers or toes in a bowl of acetone or you’ll irritate and potentially damage your skin.
1. Gather your supplies.
You’ll need 100% acetone (available in pharmacies as 100% acetone nail polish remover — don’t use standard nail polish remover or an acetone product that contains other ingredients), cotton balls or pads, scissors, plastic food wrap, a washcloth and a towel.
2. Protect your work surface.
Acetone can damage furniture and even countertops and sinks if it spills. Play it safe and lay plastic wrap on top of your work surface, then cover it with a towel.
3. Cut the cotton to fit your nails.
If you’re using cotton pads, cut them to the size of your nails, cutting larger pieces for the larger nails and smaller pieces for the small nails. The goal is to cover only the nail, not the surrounding skin. If you’re using cotton balls, depending on the size of the cotton ball you might cut them into halves for the larger nails and quarters for the small nails.
4. Apply petroleum jelly to the skin surrounding the nail.
The goal is to protect the skin in the event of acetone exposure. Don’t forget the tops of the fingernails or toenails. Note that you may find it easier to remove the gel nail polish from one hand at a time and use the free hand to apply and remove the cotton and plastic wrap.
5. Soak the cotton pieces in acetone, then place them on your nails.
Wrap the upper part of each finger or toe with plastic wrap to keep the cotton in place. “Many people use foil, but it doesn’t create a tight seal,” said Dr. O’Brien. “As a result, the acetone may drip onto your work surface, clothes or skin.” Wrap it tightly enough to create a good seal, but not so tightly that you cut off your circulation.
6. Let the cotton sit for 10 minutes.
When the time is up, remove the plastic wrap and the cotton. The polish should be mostly or completely gone. Take off any remaining polish by gently rubbing your nails with a washcloth soaked in warm water. Don’t try to scrape it off with an orange stick or you might damage your nails and cause white spots.
7. Wash off the acetone.
Use a mild, fragrance-free soap to clean your hands or feet to reduce the risk of irritation.
8. Soothe the skin around your nails.
Apply petroleum jelly daily to the cuticles and surrounding skin for at least the next several days to reduce any irritation. Cuticle oil is also helpful for rehydrating cuticles.
Repeated use of acetone, either at home or at the salon, can cause nail dryness, brittleness, peeling, and cracking, so consider reserving gel manicures for special occasions when you really want your nails to shine. If you discover that you’re sensitive to acetone, you’ll probably want to skip gel manicures altogether. Signs of contact dermatitis from acetone include red, swollen, itchy or flaking skin.
If you do get gel manicures often, the American Academy of Dermatology suggests wearing gloves with the fingertips cut off or putting sunscreen on your hands to protect the skin from the UV light used to cure the gel, which may slightly increase the risk of skin cancer.
Written by Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How to Get Rid of Hormonal Acne
Medical review by John Minni, DO
Getting acne in your 20s, 30s or 40s seems unfair, but blame your hormones.
“Hormonal acne, or adult acne, is more common than you’d think,” said John Minni, DO, a board-certified dermatologist at Water’s Edge Dermatology. “In my practice, there are times when the number of adult patients I see for acne is higher than the number of teenage acne patients.” Some of them never even had acne earlier in life.
To learn how to get rid of hormonal acne, read on.
What is hormonal acne?
As you probably guessed, hormonal acne is acne caused by fluctuating hormone levels. Women naturally experience more hormone fluctuations than men, so most hormonal acne patients are female. More than 50% of women between ages 20 and 29 and more than 25% of women ages 40 to 49 have hormonal acne.
“The changes in the balance of estrogen and progesterone women experience when they have their period, are pregnant or are going through menopause are usually to blame,” said Dr. Minni. It’s not clear how imbalances of these hormones trigger acne. They may stimulate the sebaceous glands to produce more sebum, which contributes to acne outbreaks.
The stress hormone cortisol can also play a role in hormonal acne because it causes inflammation throughout the body, including the skin.
Hormonal acne can take many forms, including pimples and whiteheads, but it typically appears as deep, painful cysts. “These can cause significant red or brown scars and leave behind a little dip in the skin,” Dr. Minni said. “Concern about scarring is one of the main reasons why people with hormonal acne seek treatment.”
You’re most likely to get hormonal acne on your jawline and around your mouth, but it can also appear on the scalp, shoulders and chest.
What causes hormonal acne?
Anything that causes hormone levels to fluctuate can trigger hormonal acne, including:
Menstruation. Hormonal acne can develop during PMS, during your period, and even in the few days after it ends. “The skin may clear up between periods, but some women never get a break because the inflammation lingers even after the hormone levels return to normal,” Dr. Minni said.
Pregnancy. When hormonal acne occurs during pregnancy, it’s usually worse in the first trimester. Then it eases for a few months and returns as you get closer to your due date. It usually clears up following the birth but may return once you get periods again.
Menopause. Estrogen levels decline during menopause and the years leading up to it, and the decline can cause hormonal acne. The average age of menopause is 51, so some women will experience hormonal acne in their 50s.
Certain health conditions. Hormonal acne often occurs in women with polycystic ovary syndrome (PCOS) due to high levels of hormones called androgens. These hormones cause the sebaceous glands in the skin to produce excess sebum. Other conditions that cause hormonal acne include Cushing syndrome and androgen-secreting tumors. Any type of chronic inflammatory disease, such as irritable bowel disease or rheumatoid arthritis, can also trigger hormonal acne, according to Dr. Minni.
Testosterone supplementation or steroid abuse. When hormonal acne occurs in men, it’s usually due to taking testosterone supplements or abusing steroids, either to feel more youthful or build muscle. “Trying to get your testosterone levels back to where they were when you were a teenager can cause tons of acne as well as prostate problems,” Dr. Minni said.
Medications. Several types of drugs can cause hormonal acne, including certain forms of hormonal birth control, corticosteroids, blood pressure medications and stimulants for conditions such as ADHD, which can increase cortisol levels. Even some vitamins, particularly those labeled for “stress relief” or intended to manage menstrual symptoms, can trigger hormonal acne because they contain synthetic forms of hormones.
Hormonal acne treatments
There are several ways to treat hormonal acne. One option is to take birth control pills that contain estrogen and progesterone. Pills FDA-approved to treat acne include Ortho Tri-Cyclen, Yaz, Beyaz and Estrostep Fe. They treat hormonal acne by decreasing the circulation of androgens.
“Unfortunately, birth control pills can have serious risks, so they’re best for people who have hormonal acne and are also looking for a form of birth control,” Dr. Minni said.
If you don’t need birth control, Dr. Minni recommends spironolactone, a prescription medication that blocks androgens. “I like spironolactone because it has few side effects and the cost is low,” he said.
Dr. Minni also suggests an antibiotic called doxycycline, taken in doses that are too low to cause antibiotic resistance but high enough to tame inflammation.
Very deep cysts can be treated with steroid injections. These must be used cautiously, however, because higher doses of steroids can cause skin dimpling.
In-office treatments such as chemical peels and HydraFacial MD can help treat hormonal acne. Chemical peels are a particularly good choice for women in their 40s, according to Dr. Minni, since they also diminish signs of aging such as fine lines and sun damage.
For pregnant women, the safest options for treating hormonal acne are topical products that combine azelaic acid and clindamycin (an antibiotic) and metronidazole, a topical antibiotic, Dr. Minni said.
Dietary changes may also help. “Some people find that their hormonal acne worsens when they eat certain foods, such as shellfish, red wine or hot sauce,” Dr. Minni said.
And, of course, follow the same practices that help prevent other types of acne. Wash your face with a gentle cleanser, don’t scrub, and don’t smoke.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Laser Hair Removal vs. IPL Hair Removal vs. Electrolysis
Medical Review By: Alyse Penninger
If you’re tired of shaving, plucking or waxing, you may want to get rid of unwanted facial or body hair more permanently. But which method should you choose: laser hair removal, intense pulsed light (IPL) hair removal or electrolysis?
The answer depends on several factors, including the color of the hair, where it’s located, and how much you need to remove. Alyse Penninger, a licensed medical aesthetician at Water’s Edge Dermatology, explains how the three techniques work and who benefits the most from each.
None of these methods gets rid of all hair forever, but you’ll see a major difference. “I like to refer to these procedures as hair reduction,” Penninger said. “Some hairs may grow in sporadically, but they’re much finer and lighter than they were before treatment.”
Laser hair removal: Best for darker hair
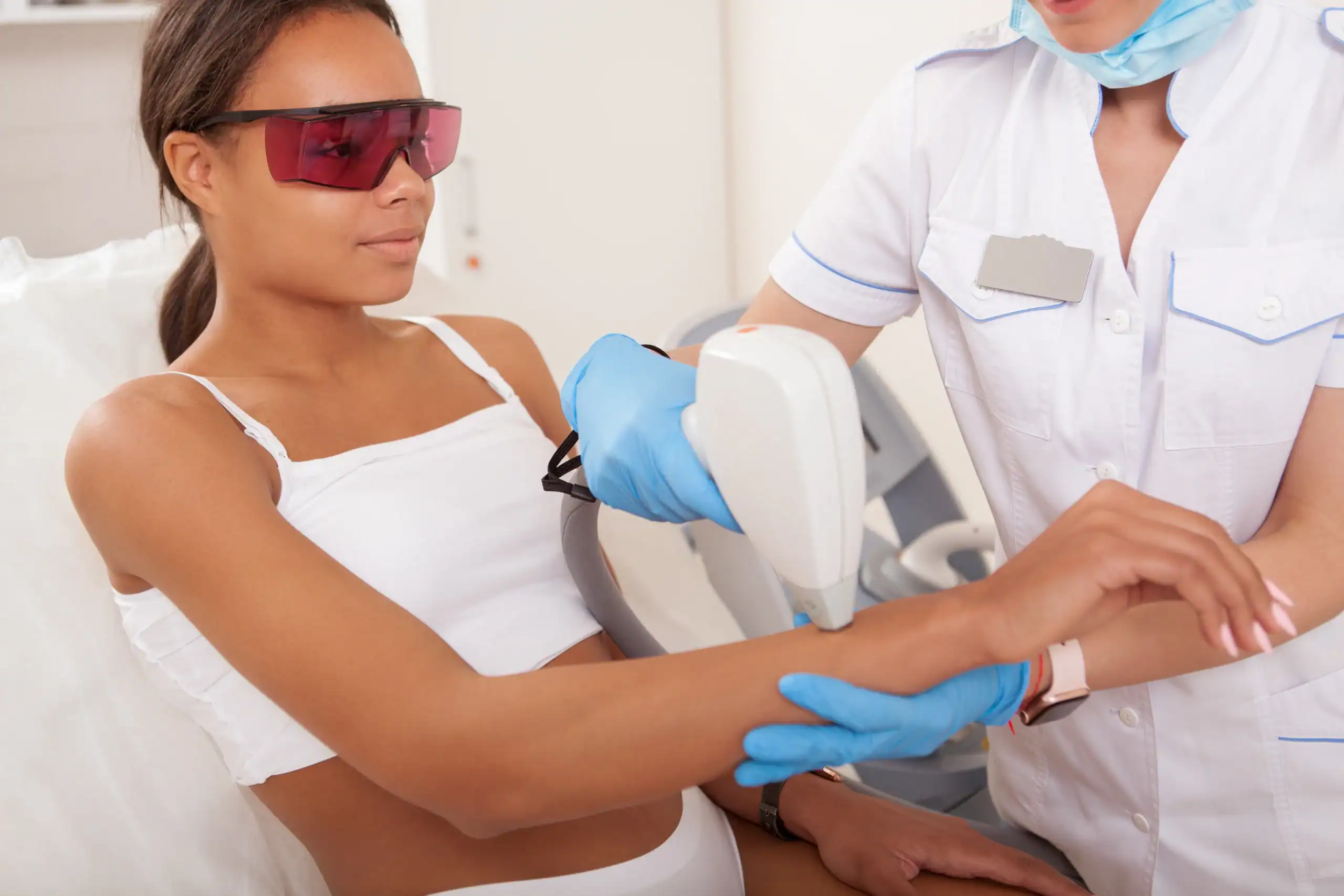
This is the most popular method of the three. During laser hair removal, the provider uses a handheld device to focus a concentrated beam of light on the treatment area. The hair’s pigment, called melanin, absorbs heat from the light. This damages the base of the hair follicle and prevents it from growing new hair. The hairs gradually fall out on their own between sessions.
The downside of laser hair removal is that people with lighter hair aren't good candidates. “Because the laser is absorbed by the melanin in the hair, the treatment works best on darker hair, which has more melanin,” Penninger said. “You won’t get results if your hair is blonde, gray, or white.”
The procedure can cause some discomfort, especially in sensitive areas such as the bikini line or when a large area such as the back is treated. The provider can apply a numbing cream to the area to make you more comfortable. Alternatively, he or she may use a laser device that also delivers pulses of a cryogenic cooling spray during treatment.
Laser hair removal can treat any part of the body except the eyebrows and the area around the eyes, as the laser can cause severe eye injuries. You’ll wear protective eyewear during each session.
Possible side effects: Mild swelling around the hair follicles, slight redness of the skin, pigment changes (particularly in people with dark skin) that are usually temporary, and temporary skin irritation, which may lead to blisters or crusting.
Treatment sessions required: Six, though larger areas such as the legs may require eight. People with dark skin may need eight sessions using a less intense laser to avoid burning the skin. (The melanin in dark skin also absorbs the laser light.) Sessions last 15 to 30 minutes for small areas and 45 to 60 minutes for larger areas. Treatments are performed every four weeks.
IPL hair removal: Best for darker hair and lighter skin
IPL hair removal is similar to laser hair removal, but the handheld device emits pulses of light from multiple wavelengths and the light covers a larger area of skin, so more skin can be treated in less time. It's more effective in people who have darker hair, similar to laser hair removal. But the color of your skin matters, too.
“IPL hair removal is best for people with lighter skin,” Penninger said. “Unlike laser treatments, the intensity of the light can’t be reduced, so there’s a risk that darker skin could burn.” IPL isn’t recommended for anyone who’s darker than Fitzpatrick skin type III, which is fair to beige skin that slowly tans after initially burning.
IPL treatment is somewhat more painful than laser hair removal. It feels like a rubber band is being snapped against your skin. To minimize the discomfort, the provider will apply a cooling gel to the treatment area at the beginning of each session.
IPL hair removal is safe for any part of the body except the eyebrows and the area around the eyes. You’ll wear eye protection during treatment sessions.
Possible side effects: Mild redness or swelling after the procedure that usually disappears in a day or two. Less common side effects include bruising, blistering, and infection. Temporary or permanent skin discoloration is also possible.
Treatment sessions required: Usually, six, though some people may get results with fewer sessions. Treatments are spaced four weeks apart. After six treatments, maintenance treatments spaced at longer intervals may be given if needed, up to 12 treatments in total.
Electrolysis hair removal: Best for small areas such as the chin and underarms
The oldest of the three treatments, electrolysis removes hair via a tiny amount of electrical current. During a session, the provider inserts a very slender needle attached to a pen-like device into each follicle and delivers the current. Then they remove the hair with tweezers.
“Hairs slide out like butter during an electrolysis treatment session,” Penninger said. “You might feel a tingling sensation when the electrical current is delivered, but it’s more annoying than painful.” If a sensitive area of the body is being treated, the provider may apply a topical anesthetic at the start of the session.
Electrolysis is safe and effective for all hair and skin colors. While it can remove hair on any part of the body, it’s best for treating small areas of unwanted hair, such as the chin and underarms, as treating larger areas one follicle at a time can be very time-consuming.
Possible side effects: Slight redness of the skin that disappears shortly after treatment. People with darker skin may notice dark spots on their skin, but these fade over time.
Treatment sessions required: Usually, six spaced two weeks apart. Treatments take 15 to 30 minutes.
Article Written By: Jessica Brown, a health and science writer/editor based in Nanuet, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets