What Are the White Spots on My Skin?
Medical review by Rachelle Lacey, MD
White spots on the skin are usually a cosmetic problem. They can be just as noticeable and bothersome as dark spots, and they may itch, but in most cases they are harmless. That said, whenever you notice a change in your skin, it’s always smart to see a dermatologist.
Here are a few of the skin conditions that can cause white spots on the skin.
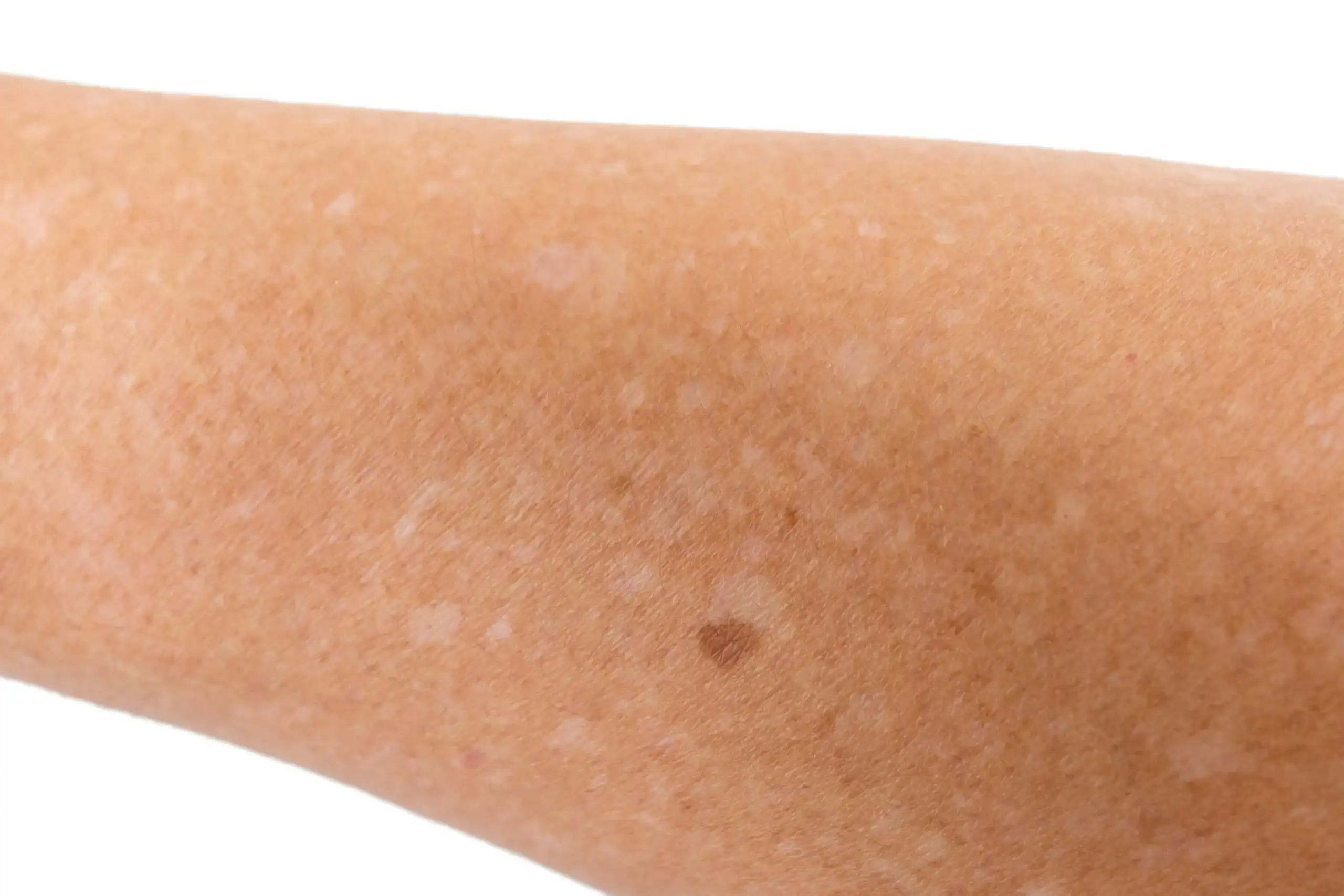
(Pictured above: Arm with idiopathic guttate hypomelanosis)
Idiopathic Guttate Hypomelanosis
Sometimes referred to as “reverse freckles,” idiopathic guttate hypomelanosis (IGH) is a condition in which small (1 to 5 millimeter) flat spots of white skin called hypopigmentedmacules develop. They commonly appear on sun-exposed areas, such as the legs and forearms. The risk of developing IGH increases with age; most people who have it are over 40.
The cause of IGH is unknown, though factors such as chronic sun exposure and genetics may play a role. People with fair skin are more prone to IGH, but the patches are more noticeable on dark skin.
How it’s treated: The macules are benign and don’t have to be removed. A consistently effective treatment has yet to be discovered. Cryotherapy is sometimes used, with mixed results. In some cases, the cryotherapy itself can cause light or dark spots. Practicing sun protection, including using a broad-spectrum sunscreen with SPF 30 or more and wearing protective clothing, can help prevent the spots from becoming more noticeable and also help prevent new spots from forming.
Milia
White spots in the form of hard, raised bumps could be milia, which are small, pimple-like cysts. Milia tend to occur in clusters on the face, usually around the eyes or on the forehead, but they can appear anywhere.
The bumps, which can also be yellowish, usually form when dead skin cells build up under the top layer of the skin. They are more common in people who have acne and blackheads. Other causes include an injury to the skin, such as a burn, sunburn or blistering rash, and using topical corticosteroids for a long period.
How it’s treated: Milia are harmless and don’t need treatment. They may go away on their own, but if they don’t, your skin care provider can remove them. (You can’t “pop” them like a pimple.) Treatment options include chemical peels, dermabrasion, laser ablation, deroofing (removing the top of the cyst with a needle or small scalpel and extracting the contents) and cryotherapy (freezing).
Tinea Versicolor
\Also called pityriasis versicolor, this fungal infection can lead to patches of skin that are whiter, pinker or darker than your normal complexion. It’s common in tropical climates. The fungus isn’t harmful and can be found on healthy skin. It becomes a problem only if it overgrows. Tinea versicolor can also cause itching and scaly skin.
The condition is more common in teenagers and young adults and typically affects the torso and shoulders. Triggers include hot and humid weather, oily skin, hormone changes and a weak immune system.
How it’s treated: Cleansing the affected areas with dandruff shampoo and using an anti-fungal cream or taking anti-fungal medication can help restore your normal pigmentation, though it can take several months after beginning treatment for the normal skin color to return. Tinea versicolor often recurs, so your doctor may recommend maintenance treatments to prevent it from coming back.
Pityriasis Alba
This chronic skin condition, which usually occurs in children and teens, causes round or oval patches that may be red or pink, turning whiter over time. The patches may be scaly and may itch. They most commonly develop on the face. The cause of the condition is unknown, though it may be a sign of a skin condition such as eczema. Pityriasis alba is associated with dry skin, asthma and allergic rhinitis (allergies).
How it’s treated: Pityriasis alba may go away on its own, though it can take several years to do so. Petroleum jelly or a moisturizer with emollients can lessen any scaling. If the skin is also inflamed, red and itchy, see your dermatologist. The doctor may recommend using a corticosteroid cream or a non-steroidal cream.
Vitiligo
People with this disease develop white patches on their skin that may enlarge over time. Vitiligo can affect anyone but is more noticeable on darker skin. Most people have non-segmental vitiligo, which affects both sides of the body and often begins on the feet, hands or around the eyes and mouth. Other types of vitiligo affect just one or a few body parts or may cover most of the body.
The loss of color occurs when cells that produce melanin, skin’s natural pigment, die or stop working. It’s not clear what triggers vitiligo, but it may be an autoimmune disease in which the body attacks its own pigment-making cells. Genetics may play a role. There is also an association between thyroid disease, diabetes and vitiligo. Sometimes, a severe sunburn, skin trauma or a period of severe emotional stress can trigger vitiligo or make it worse.
How it’s treated: Vitiligo doesn’t threaten a person’s physical health but it can cause emotional distress. There is no cure, but some treatments aim to restore normal skin color. These include anti-inflammatory creams, oral corticosteroids and forms of light therapy called psoralen plus ultraviolet-A (PUVA) and narrow band UV-B (NB-UVB). If other treatments don’t work, surgery in the form of skin grafting or pigment cell grafting may be a course of last resort. Treatments in the form of oral and topical medications known as a JAK inhibitor are available. These medications improve vitiligo by tamping down the immune system and blocking inflammatory pathways.
Lichen Sclerosus
This uncommon skin condition typically affects females before puberty or after menopause, though anyone can develop it. Small white patches develop and grow over time, usually in the genital and anal area, though they can appear on the upper body, breasts and upper arms. Other symptoms include itching, pain, bleeding, and blisters.
The causes of lichen sclerosus aren’t well understood, but it may be the result of genetics, an overactive autoimmune system, hormone imbalances or an injury that damages or scars the skin.
How it’s treated: If you suspect you have lichen sclerosus, see your doctor. Lichen sclerosus needs to be treated because the patches can scar and interfere with urination and sex. There’s also a very small chance that the patches could become cancerous. Corticosteroid creams and ointments are the most common form of treatment. Children who develop lichen sclerosus are often fortunate enough to outgrow the condition.
No matter the cause of your white spots, if they appear in areas that see the sun, reducing sun exposure and wearing sunscreen is critically important.
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.
Lotion vs. Cream vs. Ointment: Which to Use When
Medical review by Jennifer Rivera, APRN
Creams, lotions, ointments — they’re all more or less the same, right? Wrong. If you use one moisturizing product for everything, you could be missing out on more effective treatment, whether you’re battling dry skin, oily skin, cracked heels, chapped lips, psoriasis, or other skin challenges.
To know when to use a lotion vs. a cream vs. an ointment helps to understand the differences. The ingredients vary, but all three are ultimately a combination of water and oil in different ratios. Those ratios determine how moisturizing they are, how well they prevent the body’s own moisture from evaporating from the skin, and how light or heavy they feel.
Lotion vs. cream
The main difference between a lotion and a cream is the water content, which also dictates the thickness.
Lotions
Lotions contain more water than creams and are, therefore, thinner. They are typically formulated with lightweight ingredients such as hyaluronic acid, which is hydrating and skin-plumping without leaving a residue or clogging pores, resulting in more frequent applications.
Uses: Lotion is best for people with normal to oily skin and those who live in warm, humid climates. Some lotions are oil-free. Lighter moisturizing ingredients, such as glycerin and hyaluronic acid, are used instead. These can be a good choice if you have acne-prone skin.
Tip: Because they contain more water, lotions require more preservatives. If your lotion irritates your skin, it could be the preservative. Try another brand, or switch to a cream. For best absorption, apply within 5 min of showering on slightly damp skin.
Recommended products:
- Elta MD UV Clear with Broad-Spectrum SPF 46 (Face: acne/rosacea/oily)
- Elta MD UV Daily Broad-Spectrum SPF 40 (Face: Normal/Combination)
- Wederm 15% Glycolic Body Lotion (body)
- Vanicream Moisturizing Lotion (face and body)
- Aveeno Daily Moisturizing Sheer Hydration Lotion (body)
- Eucerin Advanced Repair Lotion (Body and face)
Creams
Creams are thicker than lotions because they contain more oil — typically, they are composed of about half oil and half water. They also contain heavier ingredients, such as lanolin and shea butter. Creams absorb into the skin less rapidly than lotions. Most creams come in a jar or a squeeze tube versus a pump bottle.
In addition to emollients (fats and oils that soften skin) and/or humectants (substances that hydrate the skin by attracting water from deeper layers), some creams contain occlusives, heavy ingredients that form a film, or barrier between the skin and the environment, which prevents moisture from escaping.
Uses: Reach for cream if you have dry skin, sensitive skin or you live in a cold or dry climate. Creams are also helpful for rough spots such as the elbows and heels and for dry hands. Because the skin produces less natural oil with age, many anti-aging face moisturizers come in cream formulas. Products intended to treat skin conditions such as rashes and eczema are also often creams.
Tip: Creams that contain ceramides, such as CeraVe Moisturizing Cream, help shore up the skin’s barrier function. If you’re developing irritation from wearing a face mask, try applying a cream that contains a ceramide before you put your mask on.
Recommended products:
- Wederm Restorative Lipid Replenishing Cream (face)
- Olay Regenerist Ultra Rich Moisturizer (face)
- Eucerin Original Healing Cream (body)
- CeraVe Moisturizing Cream (body)
- Eucerin Advanced Repair Hand Cream (hands)
Balms
Balms are thicker than creams but not quite as thick as ointments. Unlike creams, they don’t contain water. Their texture is typically paste-like or waxy. Beeswax is a common ingredient.
Uses: Lip and foot balm are among the most common balms. Many anti-chafing and blister-blocking products are available as balms.
Tip: For men with dry skin, beard balm is a great way to keep the skin under a beard moisturized.
Recommended products:
- Aveeno Cracked Skin Relief CICA Balm
- Aveeno Eczema Therapy Itch Relief Balm
Ointment vs. cream
Creams are thicker than lotions, and ointments are thicker still, and greasier. An occlusive such as mineral oil or petrolatum (petroleum jelly) is the main ingredient. Medicated products such as topical antibiotics often come in ointment form because ointments stay on the skin longer.
Uses: Ointments are beneficial for very dry, chapped or cracked areas of skin, such as dry heels and psoriasis patches. The ointment is also a good choice for people whose hands are very dry and chapped due to frequent hand-washing. For dry, chapped lips, ointments keep moisture sealed in longer than waxes or balms do. An ointment may be applied to a minor wound before a bandage is placed on it to help seal in moisture, which aids in healing.
Tip: If you find ointments too greasy to use during the day, use a cream during the day and an ointment at night, under a pair of cotton gloves or socks. For extreme hydration, an ointment can be applied under occlusion with the guidance of your healthcare professional.
Recommended products:
- Aquaphor Healing Ointment
- Vaseline Healing Jelly Original
- Vanicream Moisturizing Ointment
- CeraVe Healing Ointment
- Vaseline Lip Therapy
- Neosporin Lip Health Overnight Renewal Therapy
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
Study Shows Tretinoin Top Choice for Anti-aging
March 8 is International Women’s Day, and since 1911, it has been a day to celebrate women around the world. We want to encourage everyone to make a positive difference for all of the women and girls in your life every day. Your Water’s Edge team is committed to celebrating you and delivering the latest news in skin health so you can enjoy a lifetime of looking as young as you feel.
Our number one recommendation for skin protection is to be sure you and your family are using sunscreen to protect skin from the damaging rays of the sun. Regular use of sunscreen is also the number one anti-aging recommendation. Be sure you begin using sunscreen as early in life as possible. To prevent visible signs of aging that already exist, dermatologists recommend a retinol product to stimulate skin cell turnover and collagen production while exfoliating the top layers of skin to reveal fresher, younger-looking skin underneath.
Unlike many retinol skincare products on the market, Tretinoin is approved by the FDA for anti-aging and has become the gold standard for anti-aging skincare. Studies have shown that Tretinoin increases collagen and reduces fine lines and wrinkles by speeding cell turnover. These studies have also confirmed that Tretinoin brightens skin and smooths skin’s texture. It is also effective in reducing hyperpigmentation, skin discoloration and the formation of acne.
When compared with over-the-counter retinoid products, Tretinoin works faster and delivers more powerful results because it contains 20 times the retinol concentration allowed by the FDA for non-prescription, over-the-counter formulations. It is considered a medical grade prescription topical treatment that supports skin becoming stronger with a tighter and firmer appearance.
A recent study of the comparative effects of retinol and retinoic acid in the Journal of Cosmetic Dermatology looked at the efficacy of a retinol formulation for improving skin’s appearance. Four weeks of retinol treatments showed an increase in epidermal thickness, collagen production and a significant reduction in facial wrinkles.
The study results also demonstrate that topical application of retinol affects both cellular and molecular properties in the epidermis and dermis.
Tretinoin is Water’s Edge Dermatology’s most recommended product because it delivers results. Water’s Edge Tretinoin is available by prescription in three strengths with 0.025% retinoic acid; 0.05% retinoic acid and 0.1% retinoic acid.
Many dermatologists recommend that anyone over 30 begin using Tretinoin in order to prevent the visible signs of aging. Our Water’s Edge clients love Tretinoin because they are seeing positive results in healthier and more youthful looking skin. You may notice results in a few as four weeks, and when using Tretinoin, remember to always wear sunscreen to get the full benefit and protect your skin from the sun.
Click here to make an appointment today at Water’s Edge Dermatology and learn more about how Tretinoin can help you look as young as you feel. Also, please share this blog with a friend and refer them to Water’s Edge Dermatology.
Hot Tips for Buying Skincare Products
Water’s Edge Dermatology is celebrating 20 years as Florida’s premiere skincare provider, and if we’ve learned anything over the years when it comes to skincare products, it’s how to help our valued patients buy what’s best for them and what to consider regarding skincare products on the internet. So, the Water’s Edge team has compiled a tips list based on our two decades of experience. Here’s to taking great care of your birthday suit!
Tip #1: Don’t purchase skincare products on the internet from off-brand sites
Quality skincare products can be damaged if they are not stored and shipped properly. Exposure to heat or cold can negatively affect the chemical ingredients, such as delicate antioxidants, that were developed to help your skin look and feel more youthful. Even if they have a top name-brand label on them, products sold on the internet could be past their expiration date. You’ll have no way of knowing that when you shell out your hard-earned cash. Once you receive your product, if you find that you are not happy with it, making a return and getting your money back can be a big challenge.
Tip #2: Beware of counterfeit products
The fake skincare product market is alive and well, just like fake designer handbags and clothing. Because these products often contain cheaper, less effective and sometimes dangerous ingredients, counterfeit products can damage your skin. Price often will tell you if a product is counterfeit. Many fake skincare products are offered at a very low price, enticing buyers who want deep discounts on brand cosmetic products. The truth is that quality skincare products rarely go on sale for more than 20 percent below their retail price. To ensure that you are getting the authentic product, purchase directly from the brand retailer, and look for legitimate sales from that retailer.
Tip #3: Get recommendations from a dermatologist, not retail store clerks
Sales associates at a department store cosmetics counter are paid to sell you their product line. Your dermatologist is committed to helping you get the right product that will deliver the results you want. With years of medical training and experience in skin science, your dermatologist can guide you to the best skincare products for your skin and your goals.
You’ll be able to test a product at your dermatology office before you purchase it, saving you money in the long run. It’s important to remember that not all skincare products – in spite of their great reviews – are right for every individual and skin type. Those with oily skin may fare better with serums rather than heavy moisturizers. People with dry skin typically need added moisture in their skincare products. Making an appointment with your dermatologist is the best place to start.
Your skin is an important asset. It’s one of the first things people notice about you. When you take the time to get the right information and advice backed by medicine and science, your skin will know it and show it. It’s why we practice the Art, Heart and Science of skincare.
Click here to learn more about Water’s Edge MediSpa & Aesthetic Skin Care Services.
Shingles, Seniors & Medicare Coverage
Chances are, most young people have little idea of what Shingles is, much less how doctors treat it, or Medicare covers it. But the skin disease that’s scourge to so many millions of seniors has its roots in childhood. Chickenpox, in fact.
Back in the day as they say, there wasn’t a vaccine preventing most kids from contracting the varicella-zoster virus that causes chickenpox. On the other hand, children traditionally experience a significantly milder version of the virus than adults do. In fact, many parents have breathed a sigh of relief when their little ones presented with the telltale red, itchy spots; relieved to get it over and done with.
Well, there’s over and done with. And then there’s the difficult reality that if you did have chickenpox as a child, your body still hosts the varicella-zoster virus. It hides out in your nerve tissue near the spinal cord, waiting for years. Then, when the immune system of some unsuspecting senior dips low enough, it can reactivate as shingles.
So, What’s Shingles & What Do You Do About It?
While chickenpox is generally not feared, shingles is another story. While not a life-threatening condition, it remains a skin disease dreaded by at-risk seniors. Dreaded, because as anyone who’s suffered through it can tell you, shingles can be extremely painful. Think itchy red rash, fluid-filled blisters, numbness and/or burning in the skin.
The good news is, shingles is preventable for more than 9 out of 10 people, with a new, more effective-than-ever shingles vaccine. And if you do contract shingles, more good news is that it usually goes away on its own after 2-3 weeks.
Getting to your dermatologist’s office in the first 2-3 days of a shingles outbreak can be a huge help. This allows common treatments such as oral antiviral medication, pain relievers and possibly corticosteroids to provide real relief before things get out of hand.
If you’re over 50, certainly if you’re over 60, the shingles vaccine is highly recommended. Good alternative to all the medical care and treatment you’ll need if you do get it. Which raises a question important to so many senior healthcare patients/consumers:
What Will Medicare Cover When It Comes To Shingles?
Medicare Part A covers hospital benefits and Part B covers outpatient benefits. If you develop shingles, your visits to the dermatologist for diagnosis and treatments are covered by Medicare Part B.
After you meet your annual Medicare Part B deductible ($183 in 2018), Medicare pays 80% of the cost of your doctor visits and related lab tests. You’re responsible for the other 20%, unless you purchase “Medigap” coverage to help limit out-of-pocket costs for such deductibles and copayments.
While Part B covers your doctor’s visits related to shingles, the medications for treating and/or preventing shingles are generally going to fall under Medicare Part D coverage.
How can Medicare Part D Drug Coverage help with Shingles?
Beneficiaries purchase Part D policies from private insurance companies. Some Part D companies include the varicella-zoster vaccine in their drug formularies. When considering aPart D policy, you’ll want to check on that. While this vaccine might cost $200 or more without coverage, beneficiaries with Part D often pay around half that amount when they use their coverage.
For individuals with an active case of shingles, Part D plans should cover a number of medications which help control the infection. Having Part D coverage means you’ll only be responsible for your plan’s required copayment for any of these covered medications instead of full cost.
The most common and least expensive medication is Acyclovir. This medication has been around since the 1980’s and is a generic form of the brand-name antiviral medication called Zovirax.
Your doctor may also prescribe valacyclovir or famciclovir, which are two newer forms of antivirals that may treat shingles more rapidly than acyclovir. That means it’s worth checking for Part D coverage of these drugs too.
Do take note though; many seniors with Medicare Part D Drug coverage still have to confront the infamous Medicare Part D “Donut Hole” (till 2020). This is an actual reduction in coverage that kicks in for seniors whose drug costs exceed a prescribed monthly and/or annual limit.
For the time being, seniors and their loved ones need to take this and all the other above information into consideration when evaluating the costs and coverages for prevention or treatment of shingles.
How to Deal With Dry, Itchy Winter Skin

There’s nothing worse than dry skin in winter… except maybe itchy skin in winter. Let’s face it: For most of us, winter skin is not our best skin. But the right winter skin care routine can help skin maintain that healthy summer glow.
What puts the “dry” in dry winter skin?
Winter skin is pretty much synonymous with dry skin (aka xerosis) thanks to outdoor air that’s naturally less humid and indoor air that’s less humid because of forced-air heat. The water content in the top layer of skin tends to change with the water content in the air, so drier air means a drier hide.
Dry skin in winter becomes a bigger issue with age, since the skin thins as we get older and doesn’t hold as much moisture. As the years go on, the skin’s sebaceous glands also produce less oil. This happens in women sooner than in men.
The skin may become so dry that it cracks and bleeds. In winter, eczema is also more likely to rear its ugly head.
RELATED: 5 Reasons Hand Eczema Flares Up (And How to Tame It)
The best moisturizer for dry skin in winter
The best way to prevent and treat dry skin in winter is to get in the habit of applying moisturizer at least twice a day. But choose your moisturizer carefully.
Before you grab a bottle of lotion, understand this: Most lotions contain a lot of water. After you apply the lotion to your skin, some of that water evaporates. When it does, the skin dries out further. Generally speaking, especially if you live in a cold climate, for dry, winter skin you’re better off with a cream or, for real trouble spots, an ointment. Creams and ointments contain more “grease” and less water.
Creams have another advantage over most lotions: Because the contain less water, they require less preservative, which means they have less potential for irritating sensitive skin.
Over-the-counter moisturizer brands dermatologists often recommend include CeraVe, Cetaphil, Vanicream and Eucerin. For ointments, Aquaphor Healing Ointment is one of the best. Other good ointment brands are Vaseline, Cetaphil, CeraVe and Aveeno.
Benefit-boosting ingredients to look for in a moisturizer include lactic acid and urea. Both are humectants, substances that pull water into the outer layer of skin to keep it moist. Ceramides and hyaluronic acid (gentler than it sounds) also pamper winter skin.
Cool your jets to stop the itch
Tempting as a long, steamy shower can be in winter, just say no. Save the hot water for washing dishes. Hot water can strip skin of its natural oils and make dryness and itching worse. Take warm showers instead, and try to limit your time under the spray to 10 minutes. On vacation, bypass the hot tub.
Use soap only where you need it, and choose a mild, fragrance-free soap or a non-soap moisturizing cleanser such as Dove. Pat yourself dry with a towel (don’t rub) and apply moisturizer while your skin is still damp. For extra-dry spots, petroleum jelly works well. After a shower is the best time to apply it, since it works by sealing in existing moisture. Unlike lotions and creams, petroleum jelly doesn’t contain water.
Other winter skin care tips
Slathering on the moisturizer and turning the hot water faucet lower should go a long way toward preventing and easing winter dryness and itching, but don’t stop there. These measures can also help keep your skin soft, supple and crack free all winter long:
- Run a humidifier in the room you use most. A humidifier is the best weapon against dry indoor air.
- Wear loose clothing. Winter is not the time for form-fitting pants or tops if you’re prone to itchy skin. Dress in layers if necessary.
- Review your skin care routine. Continue to use a mild exfoliating product, whether it’s a gentle scrub or an exfoliating cleanser containing glycolic acid, since removing dead skin cells helps moisturizer penetrate better. But if your skin is dry and itchy, you may want to take a break from products containing ingredients such as retinoids, which may be too drying in winter.
- Avoid irritants. That includes wool and other scratchy fabrics. It may even include your regular laundry detergent. Try switching to a hypoallergenic laundry detergent and see if that helps. Wear gloves to protect your hands when washing dishes.
When to see a dermatologist
If you’re still battling dryness and itching after babying your skin, it’s time to consult your dermatologist. You may need a topical steroid cream or another prescription cream or ointment. Your dermatologist can also rule out underlying health conditions, including hypothyroidism, diabetes, kidney disease and liver disease, that can cause dry, itchy skin.
In the meantime, do yourself a favor and resist scratching. It only makes things worse.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Finding Your Family’s Perfect “Skincare Partnership”
Skin problems can begin appearing during infancy, and continue right into old age. That’s why it’s well worth establishing a lifelong “skincare partnership” with the best dermatology practice within your ongoing, convenient reach.
When Benjamin Franklin famously said “An ounce of prevention is worth a pound of cure”, chances are he wasn’t referring to healthy skin. But given how preventable, detectable and treatable most skin disorders and diseases are, he might as well have been.
That’s one big part of having a professional skincare partnership. As you and your family age, the skin issues and challenges facing you keep changing. A great dermatology practice will be by your side throughout. Educating and assisting with preventive care; putting knowledge of each family members’ medical history to good use when needed to develop customized treatment plans.
As with other organs in our human bodies – but on a larger scale because it’s our largest human organ – our skin goes through different stages of development and vulnerability as we age. Getting ongoing, age-appropriate information about a variety of age-specific skin conditions promotes prevention and early detection of skin disease. And that can be life-saving.
Throughout childhood and adolescence, having a qualified partner in skincare can be a game-changer. From molluscum contagiosum in young children to acne in teenagers; from “chicken skin” to warts, hives and assorted rashes… knowing how to prevent such skin conditions and getting personalized treatment for them when needed saves a whole lot of hassles, and heartache.
As we grow into adulthood and then hopefully old age, skincare challenges persist. Our skin gets thinner, and drier. There’s less elasticity and more sagging, as at first fine facial lines and then deeper wrinkles appear. Hormonal changes and challenges can cause adult acne and other skin troubles. And the stress and lack of sleep so many adults endure can cause a wide range of skin disorders.
With such skin vulnerability throughout our lives, it’s undeniable that a skincare partnership with a leading dermatology practice such as Water’s Edge Dermatology can only help you and your family cope — especially in Florida, “The Sunshine State”.
For one thing, WEderm is an undisputed leader in state-of-the-art skin cancer diagnosis and treatment at more than 30 local community offices.
For another very cool thing, when WEderm is your partner, you also have an incredibly effective range of cosmetic and aesthetic anti-aging and beauty-enhancing services at your disposal.
By now, you likely know that exposure to UV rays from sunlight or artificial devices such as tanning beds is the leading cause skin cancer.
The occurrence of skin cancer and its deadliest form, melanoma, doubled from 1982-2011. Upwards of 50 percent of us reaching age 65 will have had at least one occurrence of Basal Cell or Squamous Cell Carcinoma.
A single blistering sunburn in childhood or adolescence can almost double the risk of melanoma. Five before age 20 can raise the risk by 80 percent.
And another American dies from melanoma every 54 minutes.
Statistics don’t lie.
Best defense (alongside faithful sunscreen usage)?
Establish an ongoing relationship with a premiere dermatology practice. One that’s committed to both preventing skin cancer, and to being equipped with the best possible practitioners, technologies and treatment options to beat it whenever necessary.
Whether it’s the scourge of skin cancer, or the more common skin problems that plague so many of us from childhood into adulthood and old age… finding the right skincare partnership and sticking with it will help you and your family achieve and maintain the healthy, beautiful skin you want, through every age and stage of life.
Top 5 Causes of Children's School Year Skin Problems
When summer officially ends every late September, the somewhat stressful “Back-to-School” season is also pretty much over with – whew! The question is, did shopping for school supplies and other preparations also leave you well-prepared for dealing with inevitable school year skin problems?
Below are 5 of the most common causes of skin problems among schoolchildren, plus some practical skincare tips on how to prevent or treat them.
Stress
It’s remarkable how much stress affects the skin. Various rashes and acne are commonly caused by stress. So what can you do to help minimize the impact of stress on your children's skin? Find the right tools and techniques to keep their stress levels low (easier said than done, but think communication, exercise & relaxation). Ensure they gently wash their face twice daily with a mild, natural cleanser and warm rather than hot water. And get them to use a hypoallergenic, lightweight moisturizer (with SPF 30 or higher sun protection) daily.
Hormones
Hormones can play a huge role in causing acne for teens, and for an increasing numbers of "tweens" too. Getting your schoolkids into a consistent daily facial cleansing and skincare routine is extremely important. Visiting a dermatologist for the right acne treatment will be warranted in some cases. In extreme instances, you may also want to ask your family physician if hormone therapy is worth consideration.
Sweat
Let’s face it. Here in South Florida, everyone sweats, which can cause rashes and acne breakouts. Training your children to seek shade outside and stay as dry as possible can help. Same with washing off sweat as soon as possible. Consider adding gentle, individually wrapped facial wipes, a lightweight, comfy cap or hat and a soft, absorbent washcloth or bandana to their daily backpack load. But remember to put that bandana in a baggie to keep it clean, and replace with a clean, dry one each day!
Sports
Autumn sports such as football can cause their own set of skin conditions. In Florida, there’s still the sun and heat causing heavy sweating. And sports helmets can cause folliculitis (inflammation of hair follicles). Washing the face immediately after sports activity and cleaning helmet pads with rubbing alcohol are good preventive measures. Some sports uniforms and gear can also cause allergic reactions to some kids. If skin irritations develop in weeks after donning uniforms, a trip to your nearest Water’s Edge Dermatology office is in order.
Shoes/Clothing
Switching from summer’s tank-tops, shorts, and flip-flops to shoes, sneakers, and school uniforms can trigger common skin conditions, such as athlete’s foot. Breathable socks that wick away moisture from damp feet and over-the-counter foot powders that do the same can help prevent such fungal skin infections. New school uniforms should always be washed before first wearing, and if possible, given a day of “test-wearing” to identify any possible irritation or allergic reaction.
Of course, getting the kids on board with a program that addresses the 5 issues above can be…challenging. Explain to them that getting and keeping the clear skin they crave is the goal, the reason for all the extra efforts. Putting sticky notes on bathroom/bedroom mirrors at home with gentle and/or humorous reminders can also help. And if/when needed, virtually all of our dermatology providers specialize in pediatric dermatology as well as adult skincare.
For questions on common school year skin conditions affecting children, such as skin rashes, skin infections and head lice, please contact Water’s Edge Dermatology for an appointment with one of our practitioners by calling your local office, or toll-free at (877) 900-3223. You can also request an appointment online.
Here's to you and your children having a happy, healthy school year!
5 Common Skin Conditions Treated by Dermatologists Today
Let’s face it -- it’s easy to talk about acne treatments, prevention, and causes simply because it’s such a widespread issue. But acne isn’t the only serious skin problem that your local dermatologist is capable of treating, and it certainly isn’t the only common skin condition that people deal with on a daily basis.
With that in mind, let’s take a quick break from talking about acne, and instead, look at a few other skin-related conditions that can be treated by your local dermatologist:
- Psoriasis: About 7.5 million Americans are currently living with psoriasis, which is a chronic skin condition related to immune system dysfunction. Psoriasis flare-ups typically include flaking, inflammation, or red patches of skin. More than just a patch of dry skin, psoriasis may require prescription-strength topical creams, pills, injections, or even light therapy (phototherapy) to treat.
- Eczema:Eczema is another chronic skin condition that is sometimes linked to immune system disorders, but also to genetics. This condition doesn’t allow moisture to absorb into the skin and it leads to patches of itchy, dry, red, and irritated skin.
- Rosacea: Named for the bright red color that an affected area of skin will turn, rosacea typically appears on the face on the cheeks, chin, and/or nose. This sometimes causes breakouts that look like normal acne, but it might also just cause patches of skin to turn a bright reddish color.
- Varicose veins and spider veins: There are a variety of reasons why people develop varicose veins, ranging from genetics to having a profession that involves a lot of standing. Pain and cramping in the legs accompanies twisted, raised veins that are very visible through the skin. There are many varicose vein treatment options, including laser treatments, injections, and small lifestyle changes that may alleviate the pain and cramping associated with this problem.
- Warts: These are very common growths on skin, most often affecting children. Warts are noncancerous and usually don’t hurt. Nevertheless, warts are still caused by a virus and can spread from person to person, and it’s not hard at all to treat. Cryotherapy is probably the most common treatment for benign growths on the skin and it uses a freezing agent, like liquid nitrogen or carbon dioxide, to remove the growth.
See, your local dermatologist treats tons of conditions that aren’t related to acne at all! Luckily, there are plenty of treatments available for these conditions which are affordable, safe, and simple.
85% of People Get This in Their Lifetimes
Acne is a common skin condition that affects approximately 50 million Americans. Beginning in puberty, acne is well-known for affecting adolescents and teens, and acne and acne scars affect about 40% of teenagers today. However, people well into their adulthood frequently have to deal with acne. People in their 20s, 30s, 40s, and even 50s can have it! Incredibly, 85% of people suffer from acne at least once in their lifetimes.
Because acne is so widespread, there are plenty of acne treatments on the market today. Dermatological research has yielded many effective treatments against acne. Dermatologist acne treatments can be bought both over the counter as well as through a prescription from a dermatologist. Acne is certainly unpleasant to have. There's no reason not to seek treatment -- especially since it's so common!
There are a few things you can do, however, before taking acne medication. Here are a few helpful tips on how to keep your skin healthy in the face of acne (no pun intended):
- Leave Your Pimples Alone: It's very tempting to pick at your pimples, rashes, and other symptoms of acne. However, it is not recommended. Not only does "popping" your pimples not reduce your acne at all, it can lead to long-term scarring of the skin tissue even after the acne goes away. Just leave your zits alone!
- Wash Your Face and Hands on a Regular Basis: One reason why acne proliferates is because harmful bacteria makes contact with your skin, causing it to form acne. To prevent this, be sure to watch your face a few times a day and wash your hands after handling something dirty. This will make a big difference in the health of your skin.
- Keep Your Face Moist: Dry skin is bad enough. Dry skin with acne is even worse. In addition to watching your face, make sure it stays moist. Having dry skin can aggravate existing acne.
For more information, feel free to leave a comment or question at the bottom.