What's That Summer Skin Rash?
Medical review by Ted Schiff, MD
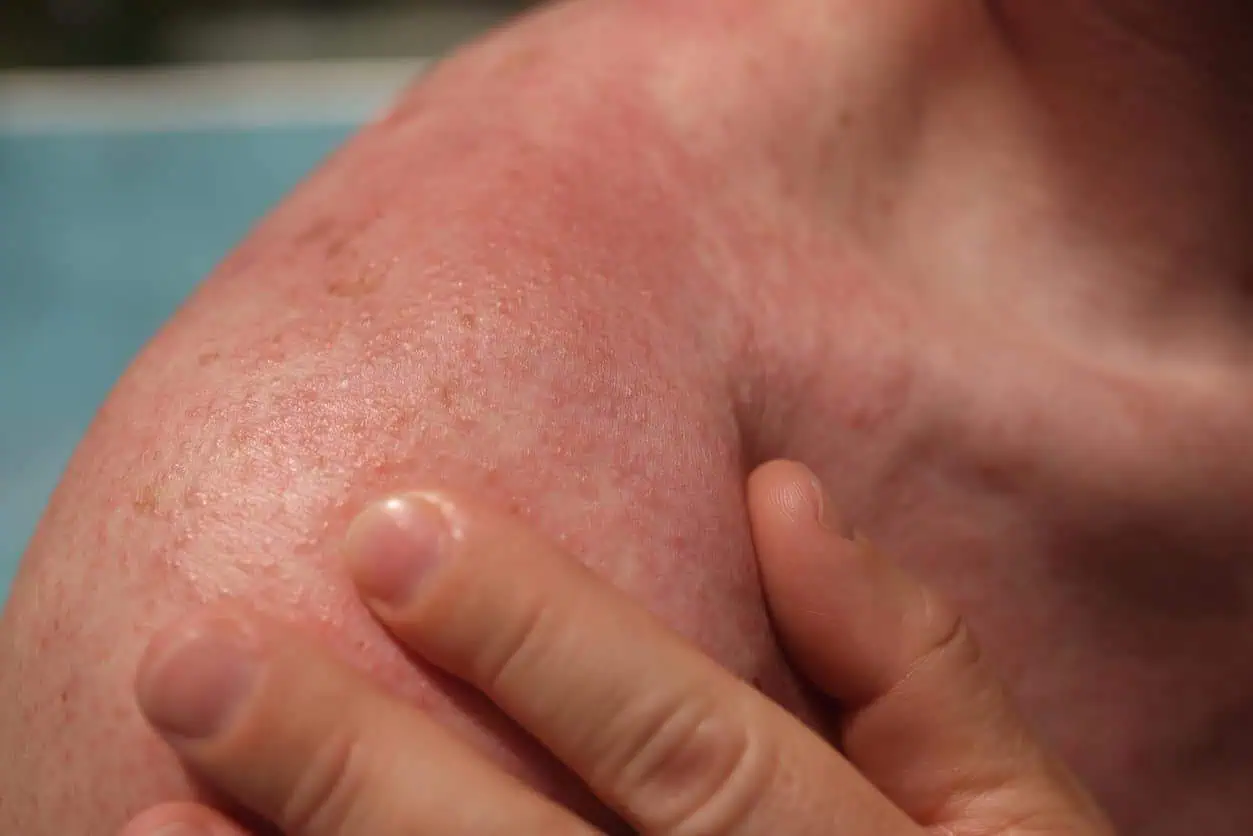
Sunburns are a summer bummer, but they’re hardly the only annoying skin problem that can crop up after fun in the sun. Spending more time outdoors, decked in shorts or a swimsuit, increases your odds of developing a variety of summer skin rashes, from heat rash to folliculitis to swimmer’s itch.
Here are 10 skin rashes to watch for.
1. Heat rash, aka prickly heat
Perspiring helps cool down your body when the mercury hits “sweltering,” but heavy-duty sweating can cause prickly heat, which doctors call heat rash. It occurs when sweat glands get clogged. The result is reddened skin and, in most cases, itchy, blister-like bumps. The rash may sting or tingle. Chilling out in a cool room and keeping your skin dry can help relieve heat rash.
2. Photosensitivity
Certain drugs, health conditions and skin care products can make the skin more sensitive to UV rays. In people with photosensitivity, spending time in the sun may trigger a reaction that looks (and feels) like a bad sunburn or a rash.
Lupus is one condition that can trigger photosensitivity. Retinols, benzoyl peroxide and vitamin C are some of the skin care ingredients that can do the same. Among the oral medications that can lead photosensitivity are hydroxychloroquine and certain:
- Antibiotics, such as doxycycline and tetracycline
- Nonsteroidal anti-inflammatory drugs, such as ibuprofen and naproxen
- Anti-arrythmia drugs
- Antifungals
- Retinoids
- Diuretics
- Statins
- Antihistamines
If your skin blisters or you develop a fever or other flu-like symptoms, see your doctor.
The best way to avoid a bad reaction to the sun is to stay out of it or cover up. If you do expose your skin to the sun, be sure to wear a broad-spectrum sunscreen with an SPF of at least 30.
3. Folliculitis
Every hair on your body sprouts from a tiny structure called a follicle. Wearing tight clothes on a hot day or sitting in a hot tub can damage thefollicles, making it easier forbacteria or fungi to enter and cause an acne-like rash that may itch or hurt. You can get folliculitis any time of year, but your skin is particularly vulnerable when it’s hot and damp. Choose loose-fitting clothes to reduce your risk.
4. Athlete’s foot
There’s nothing like hanging around a pool on a hot summer day, but beware that a microscopic fungus that causes athlete’s foot can lurk on surfaces around the water, as well as the floors of changing rooms and showers. Athlete’s foot causes a red, itchy, scaly skin rash on the feet, often between the toes, and can spread to other body parts. A related problem, jock itch, is more common in warm weather, too.
Wear flip-flops to avoid athlete’s foot, which responds well to anti-fungal treatments. To help prevent jock itch, shower after working out or sweating, wear boxers instead of briefs, change your underwear during the day if you sweat a lot, avoid staying in a wet bathing suit and dry your groin before drying your feet so the towel doesn’t spread foot fungus to your privates.
5. Melasma
Melasma isn’t really a rash, but it’s a skin condition that can worsen from spending too much time in the sun. It occurs when the cells that give skin its color, called melanocytes, make too much pigment. The result is dark patches, usually on the face. Melasma mostly affects women.
If you have melasma, stay in the shade as much as possible, and wear sunscreen (SPF 30 or higher) and a wide-brimmed hat when you go in the sun.
6. Poison ivy rash
Within a few hours or days of a too-close encounter with poison ivy — or one of its evil cousins, poison oak and poison sumac — you can develop a red rash that is unbearably itchy and may blister. Cold compresses, hydrocortisone cream, calamine lotion and oral antihistamines can help with the itching. If you have a severe case of poison ivy rash, your dermatologist might prescribe a stronger corticosteroid cream.
See a doctor if you develop a fever or you can’t sleep because of the discomfort, or if the rash doesn’t fade after seven to 10 days or begins oozing pus.
Learning to recognize these poisonous plants can spare you a lot of misery.
7. Polymorphic light eruption
Polymorphic light eruption (PLME), also called polymorphous light eruption, can cause a variety of skin symptoms, including reddening, tiny bumps, eczema-like dry patches, blisters, and welts similar to hives. No one knows what causes it, but symptoms are triggered by sun exposure, so protect your skin when you’re outdoors. The skin usually clears up on its own over time, but topical or oral corticosteroids prescribed by your dermatologist can help.
8. Sea bather’s eruption
Plunging into the ocean or the local swimming hole is a great way to cool off on sweltering days, but tiny critters in the water can leave you with an itchy rash after your dip. Sea bather’s eruption, aka sea lice, is caused not by sea lice (despite its nickname) but by the larvae of thimble jellyfish or a certain type of sea anemone. These larvae get trapped under your bathing suit. Once there, they release toxins that cause a tingly, itchy rash. The rash gets worse when you take a shower or rub your skin with a towel.
Some doctors recommend applying diluted vinegar or rubbing alcohol for relief. Cool compresses and over-the-counter hydrocortisone cream can also help.
RELATED: 6 Common Water Rashes and How to Treat Them
9. Swimmer’s itch
A swim in the lake is a summer highlight for kids, and plenty of adults, too, but if the water is contaminated with microscopic parasites released by infected aquatic snails, you could break out all over in small, reddish pimples within a day. The pimples may turn into small blisters. Your skin might tingle, burn or itch. The same parasites can contaminate salt water, too. Shallow water near the shoreline is more likely to contain them than deeper water.
Cool compresses, hydrocortisone cream, colloidal oatmeal baths and oral antihistamines are among the remedies that can help relieve swimmer’s itch.
10. Solar urticaria
Just a short spell under the sun can cause people with this rare condition, a form of sun allergy, to develop hot, itchy skin and welts that resemble hives. (“Urticaria” means hives.)
Solar urticaria is more likely to flare up in the summer, when you start wearing shorts, tank tops and bathing suits. That’s because it tends to affect skin that’s normally covered, though even covered skin may react. In some cases, solar urticaria can cause other symptoms, such as light-headedness and vomiting. The good news: Symptoms begin to fade when you take cover. Stay out of the sun until they clear.
If you think you may have solar urticaria, talk to your dermatologist about treatments that can help manage it.
Written by Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.
How Contagious Is Poison Ivy?

The short answer is no. Poison ivy rash, which is caused by an allergic reaction to oil in the plant, is not contagious. Even the fluid from poison ivy blisters is not contagious. Only direct contact with the plant’s oil, called urushiol, can trigger poison ivy rash.
But here’s the rub: Touching the plant isn't the only way to have direct contact with the oil.
Let’s say you got urushiol on your arm from touching the plant. If someone touches your arm before you wash off the oil, and before your skin absorbs it (which happens in a matter of minutes), they can get poison ivy rash. The same is true if you get the oil on your shirt or your shoe and someone else touches it, or touches a surface on which you placed an item. You can even get poison ivy rash from your dog or cat if the pet comes into contact with poison ivy and you touch the fur or hair.
That’s why it’s important to clean any items — and pets — that come into contact with poison ivy. Remove the clothing you were wearing when you were exposed and put it directly into the washing machine. Don’t drop the clothes on the rug or a chair first, and don’t let them touch the outside of the washing machine. If your shoes came into contact with the plant, clean the shoes and put the shoelaces in the wash. If your pet came into contact with poison ivy, shampoo him or her while wearing rubber gloves. As an extra precaution, you should wash the leash, too.
You should also wash other items that may have come into contact with the plant. That includes garden tools (and gloves), camping equipment, golf clubs, a bicycle you were riding and even jewelry you were wearing. You can wash them or remove the oil with rubbing alcohol.
Note, simply putting items aside to "air out" won’t do anything to prevent poison ivy rash, since urushiol can remain on surfaces for years.
Just as someone can get poison ivy rash if they touch your urushiol-contaminated skin, you can transfer it to other parts of your own body while the oil is still on your skin. Wash your exposed skin with soap and water as soon as possible after exposure. Rinse it with water if you don’t have access to soap, and wash with soap when you do. This also reduces the severity of the rash. Be sure to clean under your fingernails, where urushiol can hide.
Poison ivy rash is no fun, but if you’re smart about removing the urushiol from your body, your clothing, and anything else that may be contaminated with it, you can help prevent others from catching it — and avoid getting re-infected yourself later on.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Three Common Skin Rashes in Children
It’s that time of year again when children are back in school. Like every parent, you purchased school supplies and new school clothes so your child is comfortable and ready to hit the school room. But what about your child’s skin health, which can have a serious impact on their ability to thrive in school?
One of the most common skin show-stoppers are rashes. A rash is a skin reaction that can be caused by contact with a skin irritant, allergy, bacteria, or virus. Let’s take a look at three common skin rashes and what to look out for now and throughout the school year.
Eczema causes patches of dry, scaly red skin. Though eczema tends to flare up in cooler, dryer months when there is less moisture in the air, dryness from frequent exposure to air conditioning, overheating and sweating in the summer, and chlorine from swimming pools can also trigger eczema. Tree and plant allergies are also known to cause this skin rash. Your child’s doctor can draw up a treatment plan to help your child feel more comfortable and keep the symptoms under control.
Impetigo is a superficial skin infection caused by streptococcus or staphylococcus bacteria. This rash is often found near the nose and mouth but can occur anywhere on the body. It is more common in warmer months and can also occur as a secondary infection in the skin that has been damaged by insect bites, poison ivy, eczema, or abrasions.
Impetigo begins as small superficial blisters that rupture, leaving red, open patches of skin. It may be itchy and is highly contagious. Children can transfer the infection to other parts of the body or to other children through physical contact. Though rarely a serious disease, it is important to seek treatment. Doctors typically prescribe topical or oral antibiotics and anti-itch medication if needed.
Molluscum contagiosum is a contagious viral infection that causes pearly bumps on the skin. The virus enters the skin through small breaks in the skin barrier causing bumps, also known as “water warts” which may have a dimple in the center. This skin condition is caused by the poxvirus that is more common in hot, humid climates and may be spread in swimming pools, clothing, or towels shared by other children who may be infected. Though the bumps will typically go away on their own in six to twelve months, a dermatologist can help with topical creams to reduce the itching in order to prevent a secondary bacterial infection from occurring.
Water’s Edge Dermatology treats all types of skin rashes and diseases. We provide comprehensive, advanced skincare for children of all ages, whether your child is a newborn, a toddler, teenager, or young adult. We understand the importance of putting kids at ease with our kid-friendly, compassionate approach to care.
As experts in spotting and treating all kinds of skin diseases, we take the time to correctly diagnose the issue and provide an effective treatment plan that is right for you and your child. And we take the time to explain everything, so you and your child can have peace of mind.
Latest Eczema Treatments Offer Hope for a Cure
Anyone searching for effective eczema treatments and dreaming of a cure knows, it can be an emotional roller coaster ride. When scientists identify a previously unknown outbreak trigger for what textbooks call atopic dermatitis, hopes rise. But it's hard to stay positive when the next painfully itchy flare-up strikes.
Although there are a number of eczema treatments already available and giving relief to many people, too many people still suffer. So researchers and scientists keep searching for new treatments, and better understanding of this common but still incurable skin disease.
The good news is that recent research does offer eczema sufferers hope for a future with itch-free, unbroken, healthy skin. In fact more than 40 studies are currently underway to find a cure. In the meantime, a couple of promising new eczema treatments are finally available.
Crisaborole: New Ointment for Eczema
Crisaborole (brand name Eucrisa) is a topical (locally applied), non-steroidal ointment. It’s meant to control the symptoms (itching, redness, inflammation, skin cracking/bleeding) of mild-to-moderate eczema, allowing skin to heal.
Being non-steroidal is a big plus for this promising new eczema treatment. While topical corticosteroid ointments can offer symptomatic relief, they can also have potentially dangerous side effects for some people after 3+ months of use.
After being proven safe and effective with less side effects in clinical trials, Crisaborole received FDA approval. This eczema treatment is intended for mild to moderate cases of the skin disorder, for patients aged 2 and older. It’s the first new topical eczema treatment that has been approved in more than a decade. Hopes are high that it will ease the suffering of millions worldwide.
Dupilumab: New Eczema Injection
Dupilumab (brand name Dupixent) is another promising new eczema treatment. It’s given by weekly or biweekly injection to individuals with uncontrolled, moderate-to-severe atopic dermatitis. This is a treatment only for adults, not for pediatric cases.
The hope is that people who have had no luck with topical treatments may now be able to benefit from these injections. And clinical trial results were promising. A large majority of trial participants saw a 50 percent or greater reduction in the severity of their eczema. Even more encouraging is that a healthy number of them are now enjoying almost completely clear skin.
Time will tell, but just the availability of an alternative to topical creams and ointments is a major step forward in eczema treatment.
New Understanding, New Hope for a Cure
Efforts to finally find a cure for atopic dermatitis have been in progress all over the world for years. Still no cure. But a big breakthrough last year can only help the cause moving forward.
Researchers at Newcastle University in England appear to have found a causative factor to explain why people get eczema in the first place. It seems to come down to a deficiency in levels of the human protein called fillagrin.
According to a Newcastle team spokesman, "We have shown for the first time that loss of the filaggrin protein alone is sufficient to alter key proteins and pathways involved in triggering eczema. This research reinforces the importance of filaggrin deficiency leading to problems with the barrier function in the skin and predisposing someone to eczema."
Needless to say, that discovery is lighting a fire under researchers around the globe. Much of their work can now thankfully focus on addressing the root cause of the disease, and finding a cure. Experts agree that as a result, prospects for a cure have never been better.
The maddening question that nobody can answer is of course...When?
Until we have an answer, know that the new (and some of the older) eczema treatments can still provide great symptomatic relief for many people. It’s just a question of partnering with a great dermatologist near you, and finding out what will work best for your particular skin, and your specific case of atopic dermatitis.