How to Get Rid of Cystic Acne
Medical review by Jenna Steffel, APRN
If you’ve ever had cystic acne, you know how painful and how persistent it can be. This aggressive form of inflammatory acne is no minor annoyance. It’s also not something you can treat effectively with an acne product you grab off the shelves.
The pus-filled nodules that characterize cystic acne, which form when bacteria, oil and dead skin cells get trapped in the pores, extend well beneath the skin’s surface. Over-the-counter topical treatments can’t penetrate deep enough to reach them, according to Jenna Steffel, a board-certified advanced practice registered nurse with Water’s Edge Dermatology. “You have to treat it from within,” said Steffel.
What’s more, cystic acne can leave permanent scars — another reason to treat it early and aggressively. Prescription medication is often necessary.
Antibiotics
A low-dose oral antibiotic, typically doxycycline, is often Steffel’s first line of defense. “It targets inflammation, not infection,” she explained. At the low strength, “it’s very safe for anyone over the age of 12 who has all their teeth, and patients can stay on it for years if necessary.”
If the provider sees clinical signs of infection — for example, the cyst is red and painful to the touch — he or she might prescribe a seven-to-14-day course of higher-strength doxycycline to treat the infection, then taper down to the lower, inflammation-fighting dose.
Prescription topicals
For cystic acne patients taking an antibiotic, Steffel typically also prescribes a topical treatment to help clear the acne. Topical treatments include:
- Aczone 5% gel — an antibiotic that treats bacteria and inflammation
- MetroGel 75 (metronidazole) — an antibiotic that treats bacteria and inflammation (also commonly prescribed for rosacea)
- Azelaic acid 15% — a naturally occurring acid that fights bacteria and inflammation and slows the production of keratin, a substance that can make dead skin cells stick together, clogging pores. Azelaic acid also can help decrease post-inflammatory hyperpigmentation (dark spots caused by acne). It comes in a lower-strength over-the-counter version.
Exfoliating face washes
While oral antibiotics are doing their work, Steffel recommends using an exfoliating cleanser containing glycolic acid or sulfur to remove dead cells from the surface of the skin before they can contribute to clogged pores. One glycolic acid cleanser she likes is wederm Exfoliating Gentle Cleanser. “It’s a good option as it won’t dry out skin,” said Steffel.
Use an exfoliating cleanser both in the morning and at night. Steffel notes that a sulfur wash is perfect for use in the shower.
Avoid products containing salicylic acid, Steffel advised. “They are really irritating and drying and can cause more breakouts.”
Hormonal treatments
Hormone imbalances can trigger cystic acne in both men and women, according to Steffel. In men, the imbalances are typically caused by the use of testosterone or steroids.
In women, an excess of androgens (sometimes called “male hormones,” though everyone has them) can cause the glands in the hair follicles on the skin to produce more oil, which can clog pores. Women typically experience hormonal acne on the lower face, including the jawline. A medication called spironolactone works to control levels of androgens. Because it may cause birth defects, it’s not for women who are pregnant or trying to get pregnant.
For some women, especially those with irregular or heavy periods, oral contraceptives may help with cystic acne.
Isotretinoin
For severe cystic acne, a skincare provider might turn to isotretinoin, a derivative of vitamin A best known as Accutane, though that brand is no longer available. “It actually kills the oil gland and is the closest thing to a cure for cystic acne,” said Steffel.
It’s usually used after other treatments fail, said Steffel, “but if scarring exists at the first visit, we start the Accutane discussion.” Because isotretinoin can cause birth defects, it can’t be used by pregnant women or women planning to become pregnant. For others, the drug is safe and highly effective, says Steffel.
Doctors who prescribe isotretinoin and patients who take it must participate in a risk management program called iPLEDGE that requires use of two forms of birth control and monthly pregnancy tests.
Other potential side effects of isotretinoin include joint pain, which can be relieved with OTC pain medication, and dryness of the skin and lips. Steffen recommends Aquaphor for chapped lips. For parched skin, she favors products containing pure hyaluronic acid, such as wederm Pure Hydration — Hyaluronic Acid Serum.
Isotretinoin usually delivers results in four to six months.
Steroid injections
For especially large, single cysts, a skin-care provider can inject a small amount of a corticosteroid called Kenalog to shrink the cyst and relieve inflammation.
Home remedies
There’s little you can do to treat cystic acne on your own. Pressing an ice cube to a cyst may temporarily ease the discomfort, but it won’t fix the problem. If you’re tempted to reach for over-the-counter hydrocortisone, don’t. “It can cause discoloration in your face and won’t penetrate deep enough to have effects,” said Steffel.
Though you can’t effectively treat cystic acne by yourself, you can take steps to help prevent future outbreaks.
- Cut carbs. “Carbs turn into glucose in your body, which contributes to inflammation,” said Steffel. The first carbs to cut are refined carbs, found in white bread, white rice, most baked goods and many breakfast cereals. Steffel recommends keeping total carbs under 50 grams per day.
- Get physical. Regular exercise helps by decreasing stress. Stress increases levels of cortisol, which increases inflammation. Steffel recommends using a glycolic or sulfur wash as soon as possible after workouts to wash away sweat.
- Get enough sleep. Sleeping too little puts stress on the body, which raises cortisol levels — and inflammation.
Cystic acne presents a tough challenge, but with professional help, it can be overcome. “Eventually, with the right treatment prescribed by your dermatologist, we can get you clear, or almost clear, within four to six months,” said Steffel.
Written by Maura Rhodes, a New Jersey-based writer and editor specializing in health and well-being.
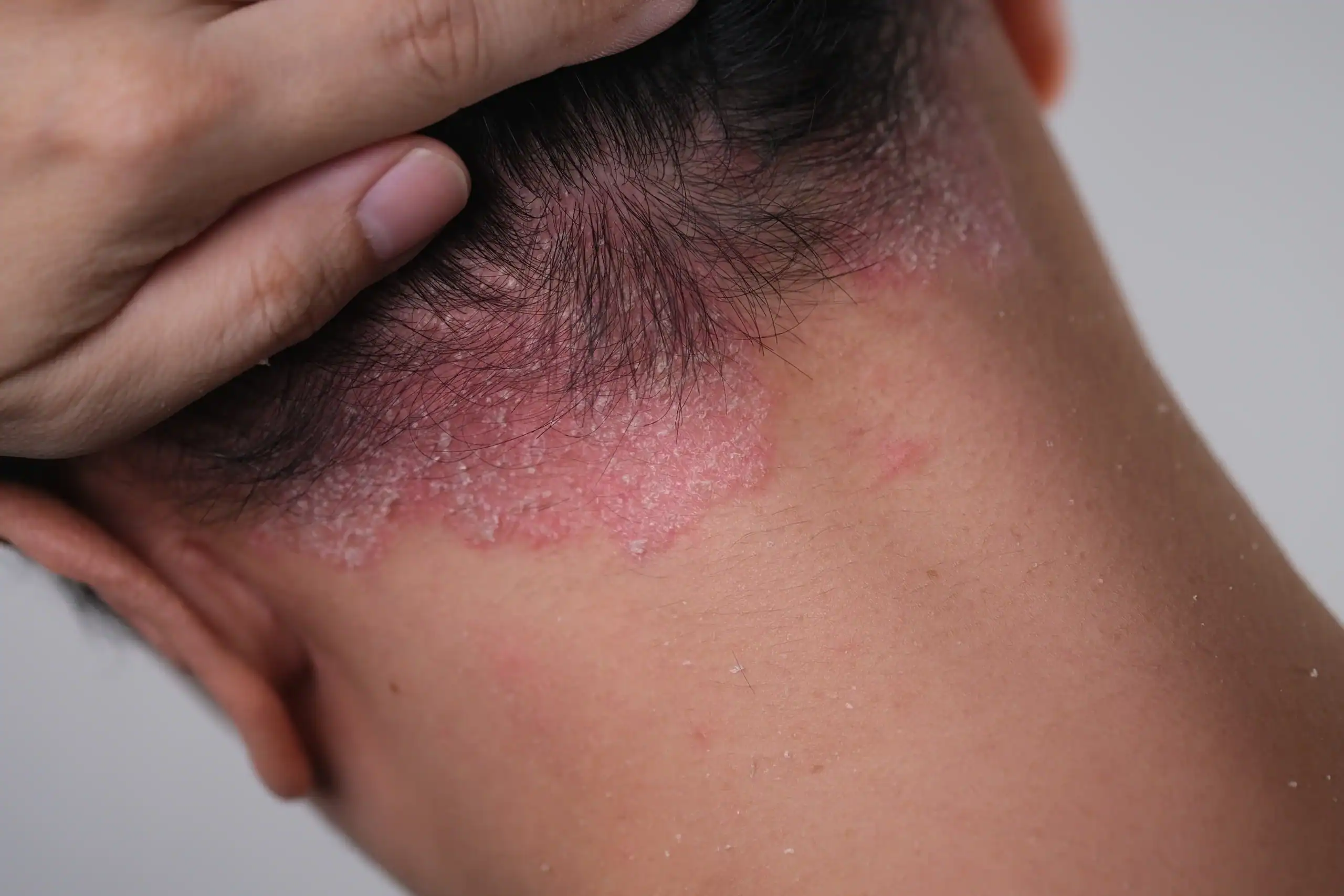
What Does Scalp Psoriasis Look Like?
Itchy, flaky scalp? It could be dandruff — or scalp psoriasis, a form of plaque psoriasis caused by an overactive immune system that makes skin cells grow too quickly.
Much like plaque psoriasis elsewhere on the body, psoriasis on the scalp typically appears in the form of reddened plaques covered with silvery scales, though the scales are often thickened and even itchier.
“Scalp psoriasis is usually very scaly, and there can be caking of the hair and even some hair loss,” said Dr. John Minni, a board-certified dermatologist at Water’s Edge Dermatology who is also board-certified in family practice.
About half of people with psoriasis will have psoriasis on their scalp at some point. Still, because scalp psoriasis can look like other scalp conditions, and sometimes exist at the same time, it can be hard to diagnose.
Is it psoriasis or seborrheic dermatitis?
Psoriasis on the scalp can look and feel a lot like seborrheic dermatitis, which causes dandruff. Seborrheic dermatitis inflames skin on the scalp and can cause redness, itching, scales and flakes. But there are some differences that can help you and your dermatologist tell them apart.
The location
The first difference is where on the scalp the problem occurs. “Seborrheic dermatitis is often scattered throughout the whole scalp,” said Dr. Minni. “It fades in and out of the skin across the whole scalp.” Scalp psoriasis, by contrast, tends to have a clear beginning and end.
Scalp psoriasis is also more likely to appear beyond the hairline — on the neck or forehead or behind (or even in) the ears.
The scales
Psoriasis patches are often drier than the greasy scales common with seborrheic dermatitis. They may also be more tender and itch more. If you scratch or pick at psoriasis scales, you may experience bleeding.
“Seborrheic dermatitis is generally a lot less inflamed and is often less scaly,” Dr. Minni said. “You’re more likely to have a dusting of flakes rather than the large flakes that can happen with psoriasis.”
Your skin elsewhere
It’s rare for people to have psoriasis only on their scalp. If you don’t have psoriasis somewhere else on your body, your scalp issues are most likely to be seborrheic dermatitis.
People can also have sebopsoriasis, a mix of both conditions. Sometimes dermatologists can’t tell where one condition ends and the other begins, even when they test a sample of skin.
Scalp psoriasis treatment
Whether you have pure scalp psoriasis or a mix of conditions, treatment often involves a combination of therapies. Dr. Minni usually begins with a potent foam or liquid corticosteroid. These steroids can quickly reduce scalp inflammation as well as redness, itching and scaling.
Along with topical steroids, Dr. Minni may recommend a medicated shampoo that contains coal tar or salicylic acid. Coal tar can reduce itching, while salicylic acid softens and helps lift away thick scales so it’s easier for steroids to reach the scalp. He uses a similar combination of treatments for sebopsoriasis.
These treatments don’t always work well enough to control symptoms, which can have a huge effect on a person’s quality of life. When topical treatments aren’t sufficient or scalp psoriasis is severe, Dr. Minni often turns to oral medicines, such as methotrexate, that tamp down immune system activity. For other patients, biologics are the answer. These are more powerful, highly targeted and given by injection or infusion.
Dr. Minni advises his patients not to scratch or pick at their scalp psoriasis. “Every time you scratch scalp psoriasis, you can actually make more psoriasis through a process called the Koebner response,” he explained.
If your scalp is itchy and scaly, getting an accurate diagnosis from a dermatologist is the first step to finding relief.
“Scalp psoriasis can be very frustrating for patients, but we can usually bring it under good control with the right therapies,” said Dr. Minni.
Article Written By: Emily Delzell, a freelance health and medical journalist based in Birmingham, Ala.
Medical Review By: John Minni, DO
4 Hidden Risk Factors for Skin Cancer
Medical review by Sean McGregor, DO, PharmD
Research has shed plenty of light on what makes some people more susceptible to skin cancer — having fair skin or multiple moles, using tanning beds and getting too much unprotected sun exposure, for example. But you may be at increased risk for melanoma or non-melanoma skin cancer without knowing it if you have one of these four lesser-known risk factors.
1. Blue, green or hazel eyes
Fair skin increases the risk of skin cancer, especially melanoma, but so do light-colored eyes. “People with lighter-colored eyes and skin tend to lack the photoprotective mechanism provided by melanin, the pigment activated by UV light that darkens skin to help shield it from damage,” said Sean McGregor, DO, PharmD, a board-certified dermatologist at Water’s Edge Dermatology who specializes in high-risk skin cancer.
Light-eyed people also tend to have blond or red hair and fair skin, placing them low on the Fitzpatrick scale, a scale used to assess skin cancer risk based on skin type. The lower you fall on the scale, the greater your risk.
According to one study, people with genes tied to blue eyes also tend to have more freckles and moles in childhood, which could potentially increase the risk of melanoma in adulthood. Having 10 or more atypical moles (moles with irregular features — see the ABCDE signs) raises the risk of melanoma by a factor of 12.
2. A weakened immune system
Your immune system protects you from illness by recognizing and routing out bacteria and other microbes that can make you sick. It could also potentially recognize precancerous conditions such as actinic keratosis (AK) and head them off at the pass. AK is caused by sun exposure and often appears as dry, scaly, rough patches.
"We know that the immune system plays an important role in skin cancer," said Dr. McGregor. "In someone with a compromised immune system, there is a loss of immune surveillance of tumor cells, allowing for the development of skin cancer."
Skin cancer in someone with a weakened immune system tends to grow more quickly and is more likely to be fatal.
3. Immunosuppressants
Taking a medication that suppresses the immune system increases the risk of skin cancer. Organ transplant recipients take immunosuppressants — often several different ones — for the rest of their lives to prevent organ rejection, which puts them at an especially high risk of developing skin cancer. On average, their risk is:
- 65 times higher than average for squamous cell carcinoma
- 10 times higher for basal cell carcinoma
- 3.6 times higher for melanoma
The degree of immune suppression necessary, and therefore the increase in skin cancer risk, varies with the organ transplanted. “People who’ve received a heart or lung transplant are at higher risk of skin cancer than those who’ve received a kidney or liver,” said Dr. McGregor.
Having other skin cancer risk factors, such a prior history of skin cancer or a lifetime of sun exposure, plays a role, too. “For example, a farmer who has worked outside their entire life, with a previous history of skin cancer, is potentially at a much higher risk of developing skin cancer earlier and/or more frequently,” said Dr. McGregor. The farmer might get skin cancer 10 months after a transplant (for example) versus 10 years.
Twenty years after an organ transplant, more than half of all transplant recipients will have developed a skin cancer.
4. Radiation treatment
Nonmelanoma skin cancers such as basal cell and squamous cell carcinoma are more likely to develop in areas of skin that received radiation treatment for lymphoma, breast cancer or another type of cancer. The increase in risk is more significant in people who undergo radiation therapy before the age of 20 and those who develop a side effect called radiation dermatitis, which may cause redness and peeling.
According to the American Academy of Dermatology, the increase in risk after radiation therapy persists for at least 40 years. The average time frame for developing skin cancer after radiation is 20 years.
What to do if you’re at increased risk
If you think you may be especially susceptible to skin cancer — whether it’s because you have a family history of skin cancer, you had a few blistering sunburns (all it really takes is one), you have fair hair, freckles and baby blues or greens or you’ve had an organ transplant — it’s essential to be vigilant about protecting your skin.
“The foundation of skin cancer prevention is sunscreen and sun-protective clothing,” said Dr. McGregor. Other key steps include checking your skin for changes, including changes in moles, and getting screened regularly.
"It’s important to come into the office to be screened for skin cancer," said Dr. McGregor "The earlier we detect a potential malignancy, the better the prognosis."
Written by Maura Rhodes, a New Jersey-based writer and editor specializing in health and well-being.
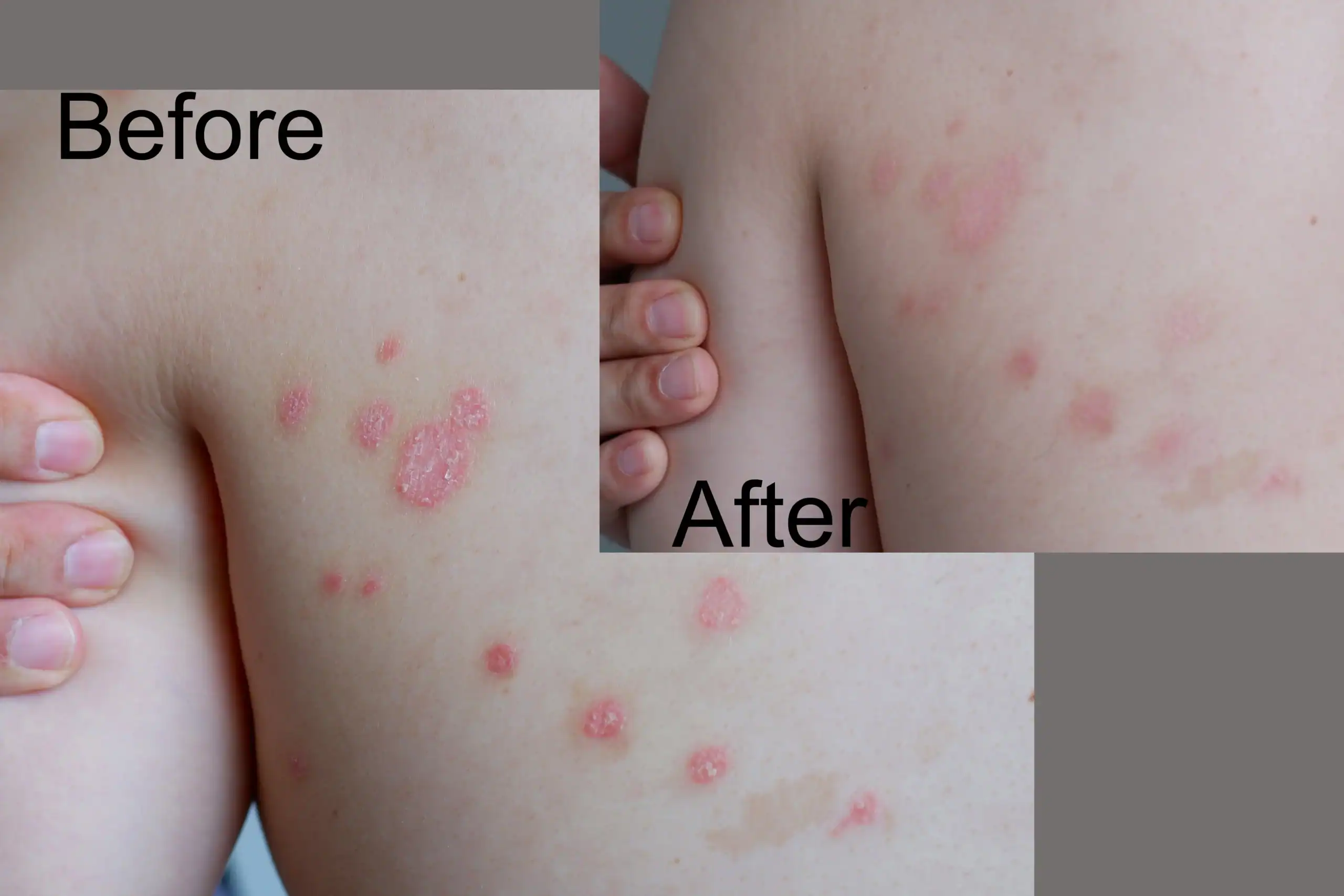
Treating Acne in Dark Skin
Medical review by Rachelle Lacey, MD
Acne is no fun for anyone, but acne in Black skin and other skin of color often poses a special challenge. Inflammation from inflammatory acne — or even some harsh products used to treat acne — can leave behind dark spots, known as post-inflammatory hyperpigmentation (PIH), which often last longer than the acne itself.
"Sometimes the treatment can cause PIH if the wrong product is used or if the patient is being treated by someone who isn’t experienced in treating acne in skin of color,” said Kimberly Van Keuren, director of cosmetic services at Water’s Edge Dermatology.
Dark skin, seen in people of African, Asian, Hispanic, Mediterranean, Middle Eastern and Native American descent, contains more melanin, the natural pigment that gives skin its color. Inflammation can trigger the skin to produce additional melanin, potentially leading to dark spots.
The solution, said Van Keuren, is to treat the acne early, before it gets bad, and start with the gentlest of acne products, working in partnership with your skin care provider to limit inflammation from both the acne and the acne treatment. Read on to discover more advice for treating acne in Black skin and other skin of color.
RELATED: How to Get Rid of Acne Scars
Consult with a skin care provider
“I like to think of the treatment of acne as a partnership between the provider and patient,” said Van Keuren. Because each person’s skin is unique, treating acne requires a customized plan, which may involve a combination of different products and other treatments — and some trial and error.
“What works for your sister or friend may be too harsh for you and cause further skin damage,” said Van Keuren.
During follow-up appointments, the provider can help you adjust your at-home regimen and may recommend an in-office treatment, such as enzyme or chemical exfoliation, to keep your skin looking its best.
“Chemical and enzyme peels help to even skin tone and smooth texture,” said Dr. Rachelle Lacey, a board-certified dermatologist at Water’s Edge Dermatology. “I find that superficial to medium-depth peels such glycolic acid peels can help fade the dark marks left behind by inflammatory acne.”
It is important to consult with a skin care provider who has significant experience treating skin of color before having a chemical peel, microdermabrasion or laser therapy because certain treatments can cause hyperpigmentation in darker skin.
Start with gentler products
Using a harsh acne product, such as one that contains a high concentration of benzoyl peroxide, can backfire.
“The treatment for acne may reverse or shorten breakouts, but on the other hand, it can dry out and irritate the skin. It’s a vicious cycle that can leave some people feeling defeated,” said Van Keuren.
Many experts advise treating mild acne with a low-dose retinoid to unclog pores, reduce inflammation and help prevent new breakouts (retinoids can also help fade dark spots), and benzoyl peroxide to get rid of the bacteria that cause acne.
“The staples in my regimen include a benzoyl peroxide product and a retinoid such as adapalene or tretinoin,” said Dr. Lacey. “Both of these medications target different problems in the acne pathway and work quite well together.”
Start with a 2.5% concentration of benzoyl peroxide. (Don’t worry, it may bleach clothing and towels but it won’t bleach your skin.) If that’s too strong, try using it every other day.
In addition to benzoyl peroxide and retinoids, Van Keuren likes toning pads containing glycolic acid or salicylic acid. These gentle acids help unclog pores and prevent new acne breakouts.
Also think gentle when it comes to choosing a cleanser, and don’t scrub. Apply it with your fingertips using a circular motion.
Protect yourself from the sun
"For some reason there is a myth that people of color can’t get sunburns or skin cancer," said Van Keuren. But these aren’t the only risks of sun exposure. "The sun on active, inflamed acne creates new hyperpigmentation. It can also darken existing hyperpigmentation."
Using a broad-spectrum sunscreen daily can help fade dark spots left behind by acne while also protecting against future ones, according to Dr. Lacey. She recommends choosing a sunscreen carefully, as not all are friendly to acne-prone skin.
"When selecting an SPF, look for words such as 'non-comedogenic' or 'oil free,'" Dr. Lacey advised. "La Roche-Posay, Avene and CeraVe are great choices."
Check your hair products and makeup
If your acne is limited to your upper forehead and/or temples, one of your hair products may be to blame. For example, oil- or cream-based hair serums and pomades are common culprits. Shampoos that contain sulfates may also trigger acne in some people. Try switching hair products and see if it helps.
If you use makeup to cover dark spots, your makeup could be making your acne worse. The American Academy of Dermatology suggests choosing mineral makeup or makeup labeled "non-comedogenic."
"There are some great, natural-looking, non-comedogenic makeup products that work well," said Van Keuren. "I’ve yet to find one that matches my skin tone, so I combine a couple of products to get the best color match."
Resist the urge to pop pimples
As tempting as being your own Dr. Pimple Popper can be, resist the urge to pop pimples. Popping a pimple can push bacteria deeper into the skin and increase the risk for swelling, redness and scarring.
Treating dark spots
Skin lighteners can gradually fade dark spots and also brighten the skin. Ingredients to look for include hydroquinone, vitamin C and a retinoid such as retinol, tretinoin, adapalene or tazarotene.
"We seem to be re-discovering and combining different lightening agents all the time," said Dr. Lacey. "My favorite lightening product at the moment is the SkinCeuticals Discoloration Defense, which contains 3% tranexamic acid, 1% kojic acid and 5% niacinamide. It is great for slowly fading discoloration left by acne."
As with acne treatments, skin lighteners need time to work, so be patient. It could take months to being seeing results.
Acne and the dark spots that linger afterward aren't insurmountable. With some diligence and the help of an experienced skin care provider, you can achieve the clear, even-toned skin you long for.
Written by Sheryl Kraft, a freelance journalist specializing in health and wellness. Sheryl’s work has appeared in CNBC, Parade Magazine, PBS Next Avenue, Everyday Health and Weight Watchers. She’s also written for Jenny Craig, Prevention and many others.
Who Should Get Biologics for Psoriasis?
If you have psoriasis, a disease that causes raised, red plaques and silvery scales on the skin, you may be wondering if biologics are right for you. While many of today’s drugs are made by combining chemicals to create new compounds, biologics are grown, often with the help of living cells. They work by targeting specific proteins to tamp down an overactive immune system. Currently, 11 biologics are FDA-approved as psoriasis treatments.
Biologic therapy can improve psoriasis symptoms dramatically — many people achieve clear or nearly clear skin. Given by injection or infusion, they also tend to have fewer side effects than older psoriasis medications that shut down more of the immune system.
It's a quality-of-life question
Mild cases don’t require a biologic. "Mild psoriasis means that once in a while, your symptoms are a minor annoyance," said Dr. John Minni, a board-certified dermatologist at Water’s Edge Dermatology who is also board certified in family practice. If that’s true for you, a topical cream such as a corticosteroid or retinoid may be all you need.
You may be a good candidate for a biologic, however, if you have moderate to severe psoriasis. "Basically, that’s anyone whose psoriasis gets in the way of their daily life," said Dr. Minni. "If your symptoms bother you every day, you should see a dermatologist who is comfortable prescribing biologics and ask about that option."
Biologics may also be the best type of medication for you if:
- You have psoriasis in hard-to-treat areas, such your scalp, nails or genitals
- You also have psoriatic arthritis, a chronic inflammatory disease that damages both joints and skin
- Your current treatment isn’t working well for you
An under-prescribing problem
Although the first biologic for psoriasis was approved more than 15 years ago, some people who could benefit from these drugs still aren’t offered the option. One reason, according to Dr. Minni: Doctors who don’t specialize in treating skin conditions (and even some who do) may not fully appreciate the physical and emotional effects of psoriasis. “Sometimes primary care doctors just see a skin rash and prescribe a cream,” he said.
The severity of psoriasis is often calculated as a percentage of skin affected. At Water’s Edge Dermatology, doctors also consider how the disease affects the patient’s life.
"I focus less on numbers and more on whether my patient is happy with the results of their current treatment. If they’re not, it’s time to discuss biologics," said Dr. Minni.
Benefits that are more than skin deep
Some people with psoriasis — about 20% to 30% — also have or will have psoriatic arthritis. Biologics are often the best treatment option for psoriatic arthritis, according to Dr. Minni.
"Considering biologics for people with psoriatic arthritis is very important because some of these medicines can help prevent disabling joint damage," he said. "This is especially important for people who are diagnosed with psoriatic arthritis at younger ages and have years to either add to or prevent damage."
Psoriasis and psoriatic arthritis increase the risk for other serious conditions, including heart disease, diabetes and depression. Biologics may lower some of these risks.
Powerful medications with fewer side effects
As with many medications that reduce immune system activity, most biologics can increase the risk of infection. They may also very slightly increase the risk of certain cancers. But they spare patients the side effects commonly seen with some other psoriasis drugs.
Methotrexate, for example, can cause liver and lung damage along with mouth sores, vomiting and fatigue. Cyclosporine can damage the kidneys and cause high blood pressure, and treatment guidelines advise against long-term use because of these and other risks. Neither drug is safe for use by women who are pregnant or planning to become pregnant.
The risks and benefits of different biologics vary. Before deciding on the best one for you, your doctor should consider your medical history and current health, including any other conditions you have.
"We have a whole smorgasbord of biologic options now, and if a patient has certain risks, we can usually find a safe option for them," said Dr. Minni. "I tell my patients that it’s very rare for me to have to stop a biologic because of side effects."
He noted that biologic treatment options continue to expand for patients of all ages.
"The FDA recently approved a biologic for children with psoriasis who are as young as 6," said Dr. Minni. "We now have the ability to treat people in a wide spectrum of age groups with these very safe medicines."
Article Written By: Emily Delzell, a freelance health and medical journalist based in Birmingham, Alabama.
Medical Review By: John Minni, DO
Can Adults Get Hand, Foot and Mouth Disease?
Medical review by Ted Schiff, MD
If you’re a parent, especially the parent of a child who’s ever been in daycare, you may be familiar with hand, foot and mouth disease, which causes fever, mouth sores and a rash. It most often affects children under the age of 5, but older kids — and yes, adults — can get it too.
What is hand, foot and mouth disease?
Hand, foot and mouth disease (HFMD) is a highly contagious illness caused by a number of different viruses. In the United States, it’s most often caused by Coxsackievirus A16, one of a group of viruses known as enteroviruses. It’s usually not serious and resolves on its own in seven to 10 days. Symptoms appear in stages and may include:
- Lethargy
- Fever
- Decreased appetite
- Sore throat
- Small, painful sores in the mouth, often on the tongue or the roof of the mouth, that typically begin as flat red spots and may blister
- An itchy skin rash in the form of flat red spots, usually on the palms of the hands and/or soles of the feet, and sometimes on the knees, elbows, buttocks and/or genitals, that may blister
People can get HFMD at any time of the year, but it’s most common in summer and fall. There’s no specific treatment. Over-the-counter pain medicine can ease the pain and fever. (Don’t give aspirin to children or teens due to the risk of Reye’s syndrome.) A numbing mouthwash or spray can dull mouth pain, as can drinking cold liquids, which also provide hydration. Sucking on ice cubes or popsicles may also help. Avoid juice popsicles, which may be too acidic for comfort. Soft food may be preferable until the mouth sores begin to heal.
RELATED: Three Common Skin Rashes in Children
How does hand, foot and mouth disease spread?
The nose and throat secretions, saliva, blister fluid and feces of an infected person can all contain the virus. If your child is sick with HFMD, you can catch it by breathing in droplets from a cough or sneeze, changing a dirty diaper, kissing and hugging the child, sharing cups or utensils and touching blisters or contaminated surfaces, such as toys and pacifiers.
An infected person is most contagious the first week of the illness, but they can remain contagious for weeks after symptoms disappear. Children who develop HFMD should be kept home from school while they have symptoms and should avoid close contact with other kids for a few weeks afterward.
Symptoms of hand, foot and mouth disease in adults
Adults may experience the same HFMD symptoms as kids, though when adults develop symptoms they are usually milder (and may be misdiagnosed). Most of the time, however, adults have no symptoms, so they don’t know they’re contagious. If you do know or suspect you have HFMD, stay home from work.
A board-certified dermatologist can diagnose HFMD in both kids and adults. Note, if you had HFMD as a child, you’re probably immune.
Prevention measures
To avoid catching or spreading HFMD, practice good hygiene. Wash your hands with soap and water for at least 20 seconds:
- before eating
- after touching a contaminated surface, changing a diaper or using the toilet
- after blowing your nose
- before and after caring for someone who’s sick (including wiping a child’s nose)
Avoid touching your eyes, nose or mouth until you’ve washed up. Teach your kids to wash their hands, too.
It’s also smart to disinfect toys, doorknobs, faucet handles, pacifiers and other frequently touched surfaces. Limit close contact, to the extent possible, with a child who has the illness, and don’t share cups or utensils. If you or your child has HFMD, avoid close contact with pregnant women. The virus, especially if contracted near the end of pregnancy, can increase the chance of stillbirth or infect the infant.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
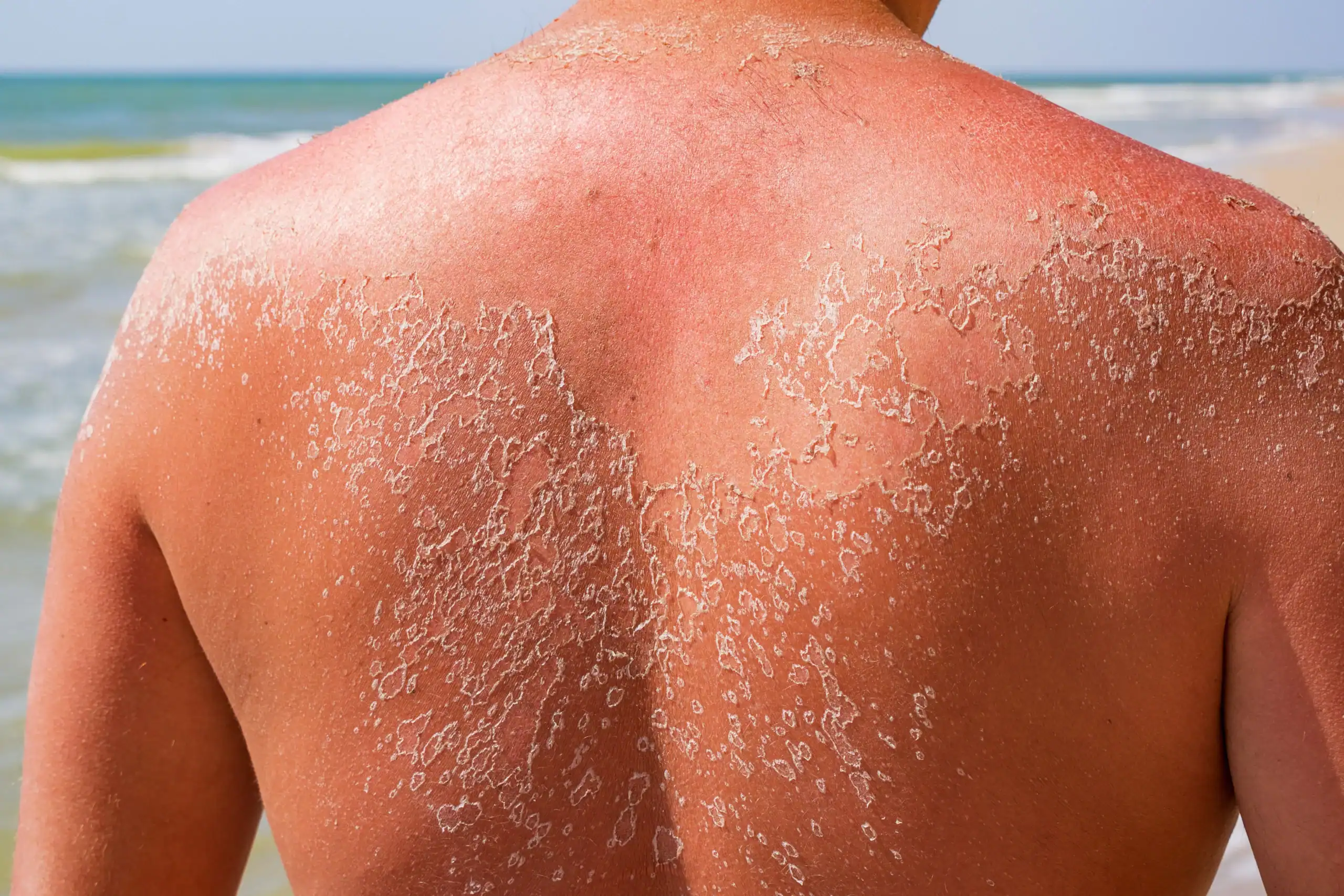
How to Treat Peeling Skin After a Sunburn
If a day at the beach, in the pool, on the boat or in the yard has turned you into a lobster, you can be pretty sure of what comes next, in a few days or a week after the initial sunburn: peeling skin. And with it, perhaps, a strong temptation to pull off the unsightly dead skin.
"The topmost layer of skin peels after a sunburn as part of the healing process," said Micaela Wolfe, a board-certified dermatology nurse practitioner at Water’s Edge Dermatology. "It’s the body’s way of getting rid of damaged cells. The peeling ceases around the same time the skin underneath is ready for exposure."
Here are some steps to take — and a few to avoid — to ease sunburn pain, help the skin heal and, if you’re lucky, limit skin peeling. (The only surefire way to avoid peeling is to protect yourself against sunburn in the first place.)
The first step: Treat the burn
Treat a sunburn right away to speed up the healing process and limit the after-effects.
Do:
- Take cool showers or baths to cool the skin and temporarily relieve the pain
- Apply cold compresses.
- Gently slather on store-bought pure aloe vera gel, especially after a shower. Aloe vera acts as an anti-inflammatory as well as a moisturizer and may reduce the amount of peeling you face later on. (Tip: Keep the aloe in the fridge for a nice cooling effect.) If you don’t have aloe, the American Academy of Dermatology recommends a moisturizer that contains soy.
- Take an over-the-counter painkiller such as ibuprofen or aspirin ASAP — within the first few hours if possible — to help with sunburn pain and limit swelling (unless your doctor has advised you not to take these medications).
- Apply an over-the-counter hydrocortisone cream, following the package directions, if the burn is bothersome.
- Drink extra water to stave off the dehydration a burn can cause.
- Stay out of the sun or wear protective clothing (UV-blocking clothing is best) to protect the skin while the burn heals.
Don’t:
- Apply petroleum jelly or an oil-based skin cream, as these trap the heat of the burn, which slows the healing process and increases irritation
- Take a hot shower
- Use harsh soap (try a moisturizing body wash instead)
- Rub the skin
Treating the peeling skin
If your skin peels despite your best efforts, follow these tips:
Do:
- Continue to regularly apply aloe vera gel or moisturizer. “This will speed skin healing as well as soften the dead skin and make it less tempting to remove,” said Wolfe.
- Protect yourself from the sun. Your burned skin needs time to heal. In fact, your skin is more prone to damage from UV rays for as long as several weeks after a burn. “I highly encourage the use of SPF protective clothing to help with sun protection, along with sunscreen use,” said Wolfe.
Don’t:
- Peel the dead skin. “Until the dead skin falls away on its own, the skin underneath is too raw for exposure and prone to infection,” said Wolfe. If you find it hard to resist the temptation to peel, cover your skin with loose clothing so you don’t see it.
- Exfoliate the skin by scrubbing.
The worst of the peeling should be over in about a week. “Help the skin stay healthy by keeping the skin moisturized, especially after a shower,” said Wolfe. In the meantime, stock up on broad-spectrum sunscreen so you don’t find yourself in the same red-hot situation again. Remember, getting too many sunburns or even just one that blisters increases your risk of developing skin cancer, as does any unprotected UV exposure, even without the sunburn.
Article Written By: Marianne Wait is an award-winning health and wellness writer based in New Jersey.
Medical Review By: Micaela Wolfe, APRN
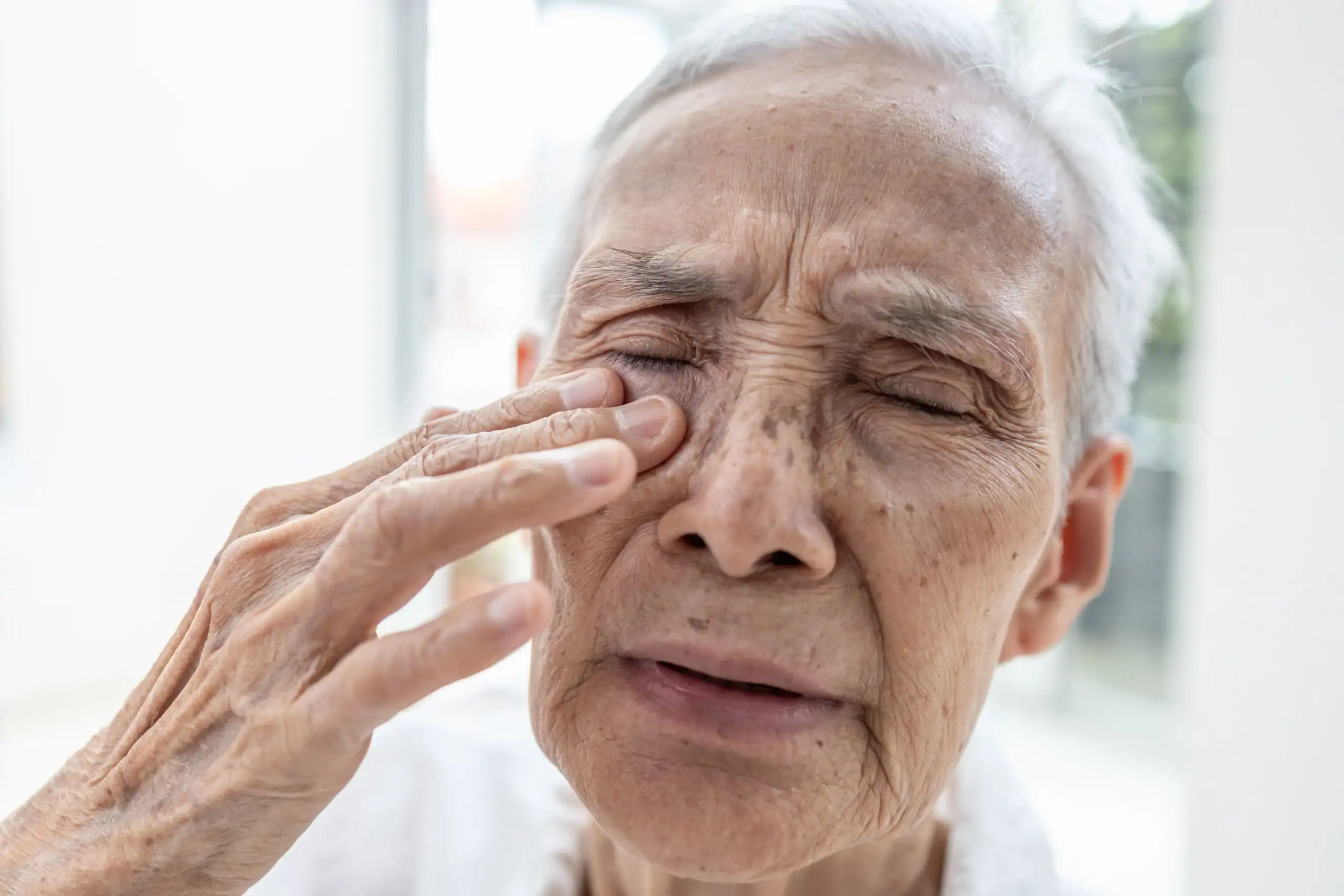
What to Know About Eyelid Cancer
When you hear "cancer," eyelid cancer probably isn’t the first type that springs to mind. Maybe you didn’t even know it existed. But skin cancer on the eyelid is common, accounting for up to 10% of all skin cancers. If you think about it, it’s not so surprising — eyelid skin is very thin and sensitive, and unless you wear a hat and/or sunglasses, it gets a lot of sun.
“Eyelid cancer is directly related to sun exposure,” said Dr. David Herold, a board-certified radiation oncologist at Water’s Edge Dermatology who specializes in treating skin cancer. Anyone can get eyelid cancer, but it’s more common in fair-skinned people over the age of 50. “Lighter-colored skin has less melanin to help block out damaging UV rays,” Dr. Herold explained.
There are two common types of eyelid tumor. Most are basal cell carcinomas, slow-growing cancers that rarely spread to other parts of the body. They are generally easy to treat, and the chance of recurrence is usually very low. The other nonmelanoma eyelid cancer is squamous cell carcinoma. This type of cancer can spread, but it’s easily treated if caught early. Melanoma, one of the most dangerous types of skin cancer, makes up only 1% of eyelid cancers.
Early detection of eyelid cancer is important because the cancer can grow into deeper layers of the skin and potentially cause disfigurement. “Anything near the eye needs to be taken care of as soon as possible,” said Dr. Herold. “We’ve had some cases where the cancer had grown for 10 years and wrapped around the eye socket.”
When eyelid cancer is detected early, there’s a better chance of removing it completely and minimizing the amount of tissue that needs to be removed.
Eyelid cancer symptoms
If you notice a lump on your eyelid, it could be a stye (caused by an infection) or some other noncancerous condition. To be on the safe side, you should have it evaluated by a board-certified dermatologist.
“Eyelid cancer typically presents as a painless, flesh-colored or pinkish bump,” said Dr. Herold. Sometimes the bump bleeds — for instance, you may scratch it in your sleep — and it can develop a crust or scab.
Other symptoms of eyelid cancer include:
- Roughness or thickening of the eyelid skin
- Change in the eyelash pattern or eyelash loss. “The cancer often occurs in the hair-bearing area of the eyelid,” said Dr. Herold. "Sometimes people notice when they’re applying mascara that eyelashes are falling out or there’s a patch of eyelashes missing."
Skin cancer can occur anywhere on the eyelid, including the inner and outer corners of the eyes, but it’s most common on the lower eyelid. "The upper eyelid seems to be protected by the eyelashes,” said Dr. Herold. “It’s like they’re holding a hat over the area."
Diagnosing eyelid cancer
Basal cell carcinoma (BCC) can grow very slowly, so oftentimes, the skin cancer has been there for months or even years when it’s diagnosed. “I’ve had many patients say, ‘I’ve had this benign cyst and it’s been looked at many times by my primary care provider, but I think it’s a little bigger,’” said Dr. Herold. “Lo and behold, it’s a BCC.”
If the growth looks suspicious, the dermatologist may perform a biopsy. During this quick procedure, the area is numbed and a sample of the tissue is removed. It’s then sent to the pathology lab for examination under a microscope. (Water’s Edge Dermatology has an in-house pathology lab with a dedicated lab team and a board-certified dermapathologist who provide a thorough review and a fast turnaround on results.) If the diagnosis is skin cancer, the doctor then discusses treatment options with you.
Eyelid cancer treatment options
Eyelid cancer is typically treated with surgery or radiation.
Mohs surgery
The most common treatment for nonmelanoma eyelid cancer is Mohs surgery, a procedure that’s done in stages. The surgeon removes a thin layer of tissue, then examines it under a microscope to see whether it contains cancer cells. The process is repeated until no more cancer cells are found. This approach spares healthy tissue and minimizes scarring.
A highly skilled surgical team may also perform Mohs surgery on certain eyelid melanomas. Others require traditional surgical excision.
Electron beam therapy
For delicate areas like the eyelids, where surgery can be challenging and often requires reconstructive surgery afterward, a form of radiation therapy called electron beam therapy (EBT) can be especially useful. EBT uses a very thin electron beam to destroy cancer cells in the targeted area while avoiding healthy cells. The beam stops at the skin, which helps limit side effects to organs and body tissue.
“It’s a gentle, painless way to treat eyelid cancer,” said Dr. Herold. “It effectively melts away the cancer.”
With EBT, you receive daily treatment for three to six weeks. Each treatment takes just two minutes. After about two weeks, the cancer is approximately 50% smaller; over time, it completely flattens out and disappears. The cure rate with EBT is more than 95%.
How to prevent eyelid cancer
Sun exposure is the enemy of eyelids (and the rest of the skin). To help prevent eyelid cancer, “sunglasses and hats are your best friends,” said Dr. Herold. In both cases, bigger is better. Opt for large, wraparound sunglasses to filter light entering from either side. Choose sunglasses with 100% UVA/UVB protection. A broad-brimmed hat, ideally at least 4 inches wide, also helps protect your eye area.
People tend to forget their eyelids when it’s time to apply sunscreen — and that’s a mistake. But choose your product carefully. “Sunscreen can burn your eyes,” said Dr. Herold. Sunscreen sticks are less likely to run into the eyes. In addition, dermatologists often recommend mineral sunscreens that contain zinc or titanium, which adhere to the skin better than chemical sunscreens.
Article Written By: Karyn Repinski, a Brooklyn, NY-based award-winning health and beauty writer
Medical Review By: David Herold, MD, MBA
How to Get Rid of Acne Scars
Acne is double trouble: First there's the ugly blemishes. Then, in many cases, there are the scars that result. If you’re wondering whether it’s possible to get rid of acne scars, or at least make them less noticeable, the answer is yes.
The best acne scar treatment depends on your skin tone and the type of acne scars you have. Some acne scars are elevated, but most are depressed (indented). These are known as atrophic scars.
Common types of atrophic acne scars include:
| Ice pick scars — these are very small and deep, like the mark an ice pick would make | 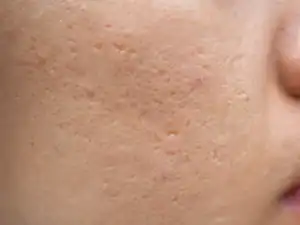 |
| Boxcar scars — these are wide, box-like depressions with distinct edges | 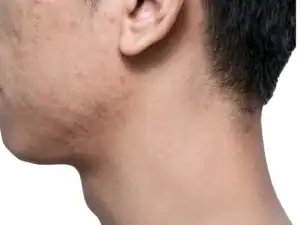 |
| Rolling scars — these have sloped edges and give the skin a wavy texture; they can be smoothed out if the skin is stretched | 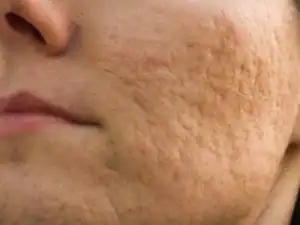 |
Acne scar treatments include fractional CO2 laser therapy, microneedling, subcision, chemical peels, dermabrasion, dermal fillers and mini-excision. Some treatments aren’t ideal for skin of color because they pose a risk of hyperpigmentation (dark patches) or changes in skin color. For the best results, you may need a combination of different treatments. A dermatologist can determine the appropriate treatment plan for your acne scars.
Remember, picking at acne blemishes can increase the chances of scarring, so if you’re guilty of that habit, do your best to break it.
Fractional CO2 laser therapy
Fractional CO2 (carbon dioxide) laser therapy, a new twist on CO2 lasering, has revolutionized the treatment of acne scars. The laser makes microscopic perforations in the skin, and as these wounds heal, new collagen is produced under the skin, which can smooth out the surface and raise depressed scars. Other benefits include tighter skin and a brighter complexion. “Fractional” means the beams of light are split into thousands of columns so that only a fraction of the targeted skin is perforated, leaving unperforated areas between the “dots.” This speeds healing and lowers the risk of complications.
Prior to beginning this procedure, the provider injects or applies a local or topical anesthetic. Following the treatment, your skin will look red and possibly swollen and may flake for a week or more. You won’t see full results for at least three months. People with very dark skin may not be good candidates for this treatment.
Fractional CO2 laser therapy may be combined with chemical peels, subcision, microneedling, dermal fillers and/or platelet-rich plasma (PRP) therapy. In PRP therapy, plasma is taken from your own blood and injected into your skin. Proteins in the plasma stimulate collagen-producing cells in the skin to produce more collagen. One study found that fractional CO2 lasering combined with PRP produced better, faster results for atrophic acne scars than lasering alone.
Microneedling
Microneedling is all the rage these days for reducing the look of wrinkles, crow's feet and enlarged pores, but microneedling for acne scars isn’t new. In microneedling, a dermaroller (a hand-held device shaped like a mini paint roller and covered with small shallow needles) is used to make tiny punctures in the skin. The body responds by filling the wounds with collagen and elastin, which makes the skin look smoother and tighter. You’ll see continued improvement over the course of weeks and months as the collagen and elastin do their work.
Microneedling is safe for multiple skin types and tones. The procedure is mostly painless. You might have some mild swelling and bruising. Typically, several treatment sessions are needed.
For faster results, perhaps with fewer treatments, there’s microneedling with radiofrequency, aka microneedling RF, in which heat is applied between the needles. This boosts the production of collagen and elastin. Microneedling RF can be further enhanced by applying platelet rich plasma (PRP) to the skin after the procedure. PRP, derived from your own blood (which means you’ll need to have blood drawn), contains proteins that help the skin repair itself.
Subcision
Rolling or boxcar acne scars, which often have fibrous attachments anchoring the base of the scar to underlying tissue, are excellent candidates for subcision. In subcision, a specialized hypodermic needle is inserted through the scar and used to release the base. This allows for the generation of new collagen beneath the scar, which lifts and smooths the surface.
“The procedure generally takes 15-30 minutes," said Dr. Christopher Spock, a dermatologist with Water’s Edge Dermatology. “Patients typically require multiple treatments, usually spaced six to eight weeks apart. Topical numbing gel and injectable anesthesia are used to keep them very comfortable throughout the procedure.”
Chemical peel
In a chemical peel, acid is applied to the skin to make it smoother and softer while minimizing the look of fine lines and brown spots. There are two types of chemical peels for acne scars.
In the CROSS technique, which works well for ice pick and boxcar scars, a high concentration of trichloroacetic acid (TCA) is placed in the scar. Wound healing triggers the production of collagen, which smooths the skin’s surface.
The second chemical peel approach is a total face chemical peel, which uses a lower concentration of TCA, or Jessner’s solution, salicylic acid or glycolic acid, to remove the top layer of skin, which smooths the surface. This type of chemical peel also stimulates the production of skin-rejuvenating collagen.
Generally speaking, superficial chemical peels (which affect only the top layer of skin) are safe for all skin types, including dark skin. Side effects include a slight burning sensation, redness and possibly some swelling.
Dermabrasion
In dermabrasion (not to be confused with microdermabrasion), the provider uses a small, hand-held medical-grade sander to sand the outer layers of skin and precisely contour underlying scars. You’ll be given a local anesthetic beforehand. Following the procedure, you may have swelling and feel some pain (usually minimal). The skin usually heals in seven to 10 days, though pinkness or redness may last for up to three months. Multiple sessions are often needed.
Dermabrasion may not be the best choice for people with darker skin.
Dermal fillers
Dermal fillers such as Restylane, Juvederm or Belotero can be injected under depressed acne scars to lift the indented skin, making skin look smoother immediately. The results last for many months. Some of the improvement may be permanent.
Fillers make the most sense when acne scars are isolated. They work especially well on rolling scars. They may not work as well for ice pick scars.
Mini-excision
Raised scars and scars that are very deep are often best removed surgically. With mini excision, the scar is cut out completely and the skin edges are stitched together. The scar that results, in the form of a fine line, is much less visible than the original acne scar — and it can be minimized with other scar treatments if you want even smoother skin.
Article Written By: Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Medically Reviewed By: Christopher Spock, MD
6 Common Water Rashes and How to Treat Them
Medical review by Alissa O'Brien, MD
Splish, splash, you got a rash? It's not uncommon for a swim in the ocean or a soak in the hot tub to spell trouble for the skin. And summer — when water activities are in full swing and bothersome sea life can thrive — is the prime time to develop a water rash, especially a pool rash, saltwater rash or lake water rash.
While rashes can be itchy and irritating, they’re usually harmless. “Water rashes may make you uncomfortable and put a damper on your summer, but they’re generally not serious and usually can be treated at home,” said Dr. Alissa O’Brien, a board-certified dermatologist at Water’s Edge Dermatology.
A native Floridian, Dr. O'Brien has had a lifetime of personal experience with a number of water rashes. Here, she gives the lowdown on the most common ones, including how to recognize and treat them.
1. Sea lice
If you develop a red, itchy rash under your swimsuit or rash guard after being in the ocean, sea lice may be to blame. No relation to head lice, these tiny, translucent larvae of thimble jellyfish are born during the summer spawning season.
Sea lice can get trapped in your hair or under your swimsuit, which is why the rash is usually most prominent on the neck, back, chest, abdomen, groin and backside. Pressure on the larvae causes them to release their toxins. You may feel a slight prickling sensation. Over several hours, a rash, sometimes called "sea bather’s eruption," develops.
For immediate relief, look in your kitchen. "Vinegar is quite helpful in neutralizing sea lice and reducing symptoms," said Dr. O'Brien. "In fact, many Floridians keep vinegar spray on their boat and spray down when getting out of the water. We smell like salad dressing, but it helps!"
The rash usually resolves on its own after a week or two. An oral antihistamine such as Benadryl, along with hydrocortisone cream or calamine lotion, can also ease itching and pain. Cool compresses and a nonsteroidal anti-inflammatory drug (NSAID) such as ibuprofen may help, too.
Some people may experience more severe symptoms, including fever, nausea, diarrhea and chills. "These usually affect children and people with allergies," said Dr. O’Brien. A doctor may prescribe a steroid in the event of a serious reaction.
Infestations of sea lice come and go. On some beaches, purple flags may warn swimmers of the risk. Wearing as little clothing as possible when in the water — no T-shirts or long shorts, and bikinis for women instead of one-piece bathing suits — can help you avoid a sea lice rash.
2. Chlorine rash
The disinfecting power of chlorine (it’s the same chemical found in household bleach, just in a lower concentration) can strip the protective oils from skin, leaving it dry, red and itchy with chlorine rash. In people with eczema, this irritation can cause eczema flare-ups.
Hydrocortisone cream can help tame the symptoms of a chlorine rash. Skin usually calms down after a few days, but you should take a break from the pool until it does to avoid further irritation.
To prevent future rashes from pool water, do more than rinse off when you get out of the pool; shower and wash diligently with a gentle soap to remove some of the film that chlorine forms on skin. If you swim frequently, you may want to purchase a special swimmer’s soap or body wash designed to remove chlorine. Ingredients such as vitamin C break the bonds it forms on skin. Finish up with moisturizer to offset the drying effect of the pool water (the more you get in and out of the pool, the worse the effect is), and reapply it often. Keep in mind that most sunscreens are moisturizing — another good reason to reapply sunscreen after swimming.
3. Swimmer’s itch
This rash can develop after swimming in fresh water, such as lakes, ponds and rivers. It's caused by tiny parasites, called schistosomes, released by infected snails. The parasites burrow into skin not covered by your swimsuit — you may feel a tingling sensation as they dig in — and trigger an allergic reaction. (Don’t worry, they can’t survive in humans and die almost immediately.) The parasites have been found in lakes in all 50 states but are most common around the Great Lakes.
"The rash shows up pretty quickly, usually within 24 hours, though it happens faster if you’ve had exposure in the past," said Dr. O’Brien. "You’ll have itchy red dots all over the place from where the parasites got into the skin." Swimmer's itch is uncomfortable, but it usually clears up on its own in a few days to a week. In the meantime, you can control the itching with oral Benadryl and hydrocortisone cream.
4. Hot tub rash
You might think nothing can survive in the toasty water of a hot tub, but that’s just not true. "Bacteria love to live in hot water, especially if it’s not chlorinated well enough," said Dr. O’Brien. Worse still, "The skin is easier to penetrate when it’s warm, so it creates the perfect environment for an infection to develop."
Hot tub rash, aka hot tub folliculitis, is an infection of the hair follicle by the Pseudomonas aeruginosa bacterium. Most people see breakouts about 12 to 48 hours after being exposed. The bright red bumps, which may be pus filled, can appear on any part of the body that has hair, but they tend to be worse in areas your swimsuit covered.
The rash usually clears up in a few days. "It doesn’t tend to be intensely itchy like some other rashes," said Dr. O'Brien. But if you find yourself scratching a lot, oral Benadryl and calamine lotion should help. Skip the hydrocortisone cream, since steroids can make infections worse.
5. Jellyfish stings
Jellyfish and the Portuguese man-of-war thrive in saltwater and their stings are common around the Florida coast. Most jellyfish and man-of-war stings usually aren’t very dangerous, but the toxin they release causes immediate pain and burning that can last for several hours. Use these tips immediately after being stung to help reduce the pain:
- Rinse the area with vinegar, which can neutralize the venom.
- Do not rinse with plain water as it can trigger the release of more toxin.
- Do not urinate on the sting; urine can also aggravate the stingers and worsen the pain.
- Use tweezers to remove any tentacles still on the skin. Do not scrape them away with a credit card or other scraping device — you’ll only cause the stingers to release more venom.
Shortly after you’re stung, a line of red welts develops where the tentacle touched you — it can look like you’ve been hit with a whip. You may experience itching and swelling, and some people may develop hives or blisters. Oral Benadryl, NSAIDs and hydrocortisone cream can help reduce pain and inflammation, which should resolve after a week or two.
6. Blue-green algae rash
Blue-green algae, also known as cyanobacteria, is what most people know as “pond scum.” It floats on the top of the water or lies below the surface and can “bloom” when the water is warm and calm. It sometimes produces toxins (cyanotoxins) that can be irritating to skin or trigger an allergic reaction. Coming into contact with it can make skin red, swollen and sore. Small blisters sometimes develop.
Blue-green algae can be found in fresh water, salt water or mixed “brackish” water. If you’re exposed to it, remove any contaminated clothing and jewelry and wash your skin with soap and water for 10 to 15 minutes. Not everyone who comes into contact with blue-green algae develops symptoms, but if you do, antihistamines and hydrocortisone cream can help relieve them.
To protect yourself from these toxic blooms, steer clear of water that’s discolored and smelly or that has green scum on the surface.
Written by Karyn Repinski is a Brooklyn, NY-based award-winning health and beauty writer.