Is it Safe to Get Vitamin D from the Sun?
Lately, vitamin D has been enjoying a moment in the sun as researchers discover more and more health benefits it may offer. At the same time, vitamin D deficiency is common in the United States, even in healthy, young adults.
The solution is simple — and it isn't the sun.
The health benefits of vitamin D
A fat-soluble vitamin, D promotes bone health by increasing calcium absorption in the intestines and regulating levels of calcium and phosphate. But it does much more. Vitamin D modifies the body's immune responses, regulates specific metabolic activities and plays a role in managing inflammation. Some evidence suggests vitamin D may help guard against or fight certain cancers and diabetes. Supplementing with vitamin D may improve symptoms of depression, especially in people whose levels are low.
Interesting fact: While vitamin D has "vitamin" in its name, it's technically a prohormone, a substance the body converts to a hormone. The hormone D becomes is a type of steroid.
Lack of vitamin D could contribute to a person’s susceptibility to viral respiratory infections and lung diseases, though a cause-and-effect relationship hasn’t been proven. Some experts have theorized that increased exposure to the sun’s UV rays was the reason tuberculosis patients benefited from sanitoriums.
More recently, during the coronavirus pandemic, researchers have speculated that healthy levels of vitamin D might benefit COVID-19 patients. They noted a correlation between low vitamin D levels and higher mortality from the virus. It could be that vitamin D helps prevent an immune system overreaction that leads to a cytokine storm, in which the body attacks its own tissues.
Natural sources of vitamin D
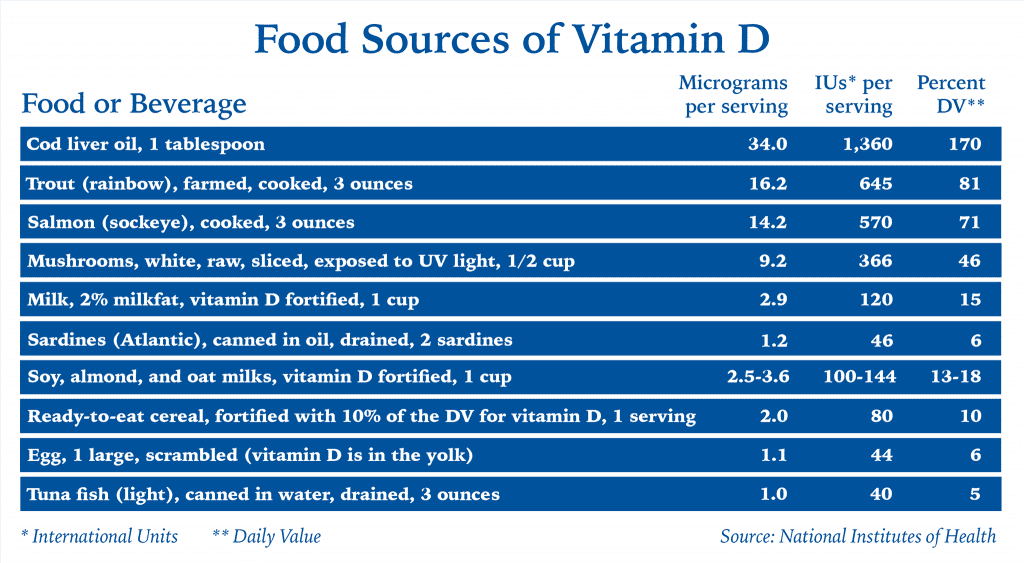
Don’t count on getting all the vitamin D you need from food. Most foods, other than fatty fish, are poor sources of vitamin D, unless they have been fortified. Foods and beverages often fortified with D include dairy milk, soy milk, orange juice, margarine and cereal.
Certain people should avoid it altogether.
The richest natural source of vitamin D — specifically the form known as vitamin D3 — comes not from the ground but from the sky. UVB rays from the sun, which penetrate the outer layers of exposed skin, prompt the body to make vitamin D. It’s not called the "sunshine vitamin" for nothing.
How much vitamin D can you get from the sun? That depends on where you live, the season, the time of day and your skin color. Getting a sufficient daily dose could take as little as 15 minutes, or considerably longer. At some latitudes, it's almost impossible to get adequate vitamin D from the sun, except in summer. As we age, it becomes harder to make D from sunlight.
What level of sun exposure is safe?
Here’s the real problem with getting vitamin D from the sun: Exposure to UV rays significantly increases a person’s risk of skin cancer — so much so, in fact, that the American Academy of Dermatology and the American Cancer Society both advise against getting any unprotected sun exposure. While 15 minutes a day might seem harmless, damage to the DNA from UV rays builds up over time. Eventually, when the scales tip, the result is skin cell mutations that lead to skin cancer.
The intensity of the sun matters as well as the length of exposure. In places where the sun's rays are strong year-round, such as Florida, damage can occur more quickly.
How can I get enough vitamin D?
Assuming you're practicing sun safety by wearing a broad-spectrum sunscreen with an SPF of at least 30, seeking shade and covering up, your doctor may advise you to take a vitamin D supplement in addition to consuming fortified foods and beverages.
Vitamin D3 is generally considered the preferred form of supplement. The recommended dietary allowance for adults up to age 70 is 600 IU. For adults over the age of 70, it jumps to 800 IU. Certain people may need to take more. If you have osteoporosis or any risk factors for vitamin D deficiency, your doctor may want to check your vitamin D levels with a blood test.
As with most supplements, more is not better. It's very possible to take too much vitamin D, which can be toxic at high doses. The Institute of Medicine of The National Academies suggests a tolerable upper intake level of 4,000 IU per day. Most people need far less.
The bottom line: Don't get your sunshine vitamin from the sun. Get it from oily fish, supplements and fortified foods and beverages.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Does Melanoma Itch?
If you have a mole, skin growth, skin lesion or dark spot that begins to itch, don’t panic — but do pay attention. Most moles are harmless, and itching could be the result of irritation from clothing, or even a new detergent. But any itchy mole, growth or wound could also be a symptom of skin cancer — either melanoma or, more likely, another form of skin cancer.
Which skin cancers itch?
Some melanomas itch. The “E” in the ABCDE rule of melanoma is for "Evolving," which means that something about the mole changes. New itching or tenderness falls under "Evolving." So does a change in the size, shape, color or elevation of the mole. A melanoma may also begin to bleed or crust over.
The other ABCDE warning signs of melanoma are:
- Asymmetry — most melanomas are asymmetrical
- Border — the border may be irregular, perhaps with scalloped or notched edges
- Color — instead of being uniform, the color may vary from one area to another, with shades of tan, brown or black; in later stages, red, white or blue may appear
- Diameter — melanomas may be smaller when they first appear, but if a mole is the size of a pencil eraser (about one-quarter inch in diameter) or larger, pay extra attention.
Melanomas tend to have at least one ABCDE trait and may have several. Melanoma can develop in an existing mole or appear as a new mole. It can occur anywhere on the body — not just where the sun shines.
While itching can be a sign of melanoma, it’s more often associated with two other common types of skin cancer: squamous cell carcinoma and basal cell carcinoma.
What is squamous cell carcinoma?
Squamous cell carcinoma is the second-most common type of skin cancer, after basal cell carcinoma. Squamous cells are flat cells near the surface of the skin.
Squamous cell carcinomas (SCCs) most often appear in areas of the body frequently exposed to sunlight, including the lips, face and hands. They can take a variety of forms. For example, a SCC can be:
- A brown spot
- A scaly red patch
- An open sore (possibly with a raised border) that doesn’t fully heal
- A growth that resembles a wart
- A raised growth with a depression in the middle
- A dome-shaped growth
- A horn-shaped growth
Some SCCs may itch, bleed or crust over.
SCCs are typically easy to treat. Left untreated, however, they can grow into deeper layers of skin and even metastasize (spread) to other parts of the body. While much less deadly than melanoma, SCC kills more than 15,000 Americans each year.
What is basal cell carcinoma?
Basal cell carcinoma is the most common type of skin cancer. Basal cells line the deepest layer of the epidermis, the outermost layer of skin.
Like SCCs, basal cell carcinomas (BCCs) can take on many forms, including:
- A reddish patch or irritated area of skin, which may itch or hurt
- An open sore that doesn’t heal, or one that heals and later returns (these sores may bleed, ooze or crust over)
- A shiny, possibly translucent bump or nodule
- A small, pink growth
- A flat, waxy-looking white or yellow area that resembles a scar
- A scar or growth with slightly elevated, rolled edges and/or a depression in the middle
Basal cell carcinomas typically appear in areas that are exposed to the sun. Because they grow slowly, they are usually curable. However, if left untreated, they can grow deep into the skin and cause disfiguration.
What should I do if I notice a suspicious mole?
See a dermatologist promptly if you have a spot or sore that won’t stop itching, you notice a new mole or growth or you notice any changes in an existing mole, lesion, bump, scar or patch of skin. The dermatologist will examine your skin and may remove a small sample of skin tissue for biopsy.
How often should I have my skin checked by a doctor?
An annual skin screening from a board-certified dermatologist is important, especially if you have a large number of moles, other risk factors for skin cancer or live in a place where the sun shines year round (like Florida). Annual skin screenings may identify skin cancer early, when it’s more easily treated. If you have a history of melanoma, your dermatologist may want to see you more than once a year.
Between professional skin screenings, it’s a good idea to periodically check your skin for any new signs of skin cancer. The American Cancer Society shows you how to perform a skin self-exam.
Article Written By: Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Medical Review By: Ted Schiff, MD
How to Avoid Skin Problems from Wearing a Face Mask
Updated June 25, 2020
Medical review by Beth Mitchell, PA-C
During the coronavirus pandemic, wearing a face mask has become as normal as wearing clothes (or at least sweatpants, for those sheltering in place). Some people wear one only to grocery shop or take a walk; others, such as healthcare workers, wear one all day long. While a mask helps protect other people from infection if you have COVID-19 and don't know it, wearing one for long periods can wreak havoc on your skin, leading to pressure marks, irritation, rashes, acne breakouts (dubbed "maskne") and even skin infections.
One problem is the pressure of the mask. Worn properly, a mask hugs the skin, covering the nose and mouth and leaving little room for air to enter around it. Over time, the pressure can cause chafing, temporary red marks and even bruising or sores. Masks also allow oil and sweat to build up, and they trap your breath, creating a warm, humid environment. These conditions can lead to acne, a rash or even an infection if the skin is broken.
For anyone who wears a mask all day, there’s no surefire way to avoid skin problems, but these measures can help:
-
- Wash your face with a gentle cleanser before putting on the mask. This removes dirt and excess oil. “Brands I like include Cetaphil Gentle Skin Cleanser, Vanicream Gentle Skin Cleanser and EltaMD gentle cleanser,” said Beth Mitchell, certified physician's assistant (PA-C) at Water's Edge Dermatology. Use lukewarm water, not hot, and apply the cleanser with your fingertips, not a washcloth. Gently pat the skin dry with a clean towel.
- Apply a moisturizing cream, face balm or ointment. Let it absorb into the skin before putting on the mask.
- Creams: Creams that contain ceramide, such as CeraVe Moisturizing Cream, help shore up the skin’s barrier function by holding skin cells together. Other ingredients to look for include glycerin and nicatinamide (a form of vitamin B3), found in brands such as Eucerin and Aveeno. La Roche-Posay has a moisturizer (Toleriane Double Repair Moisturizer) that’s great for sensitive skin, according to Mitchell, and it contains all three ingredients.
- Balms: One balm Mitchell recommends is Aveeno Eczema Therapy Itch Relief Balm.
- Ointments: Good ointments to try, according to Mitchell, are Aquaphor Healing Ointment and Vanicream Moisturizing Ointment. Use ointments on raw skin, not all over the face.
- Skip the makeup. Eye makeup is fine if it gives you an emotional boost, but don’t wear makeup under a mask. Give your oil and sweat pores a break.
- Ensure the mask is properly fitted. "If you have an ill-fitting mask, it will move and slide on the face, causing more irritation as you are constantly readjusting it. It will also not be working effectively to protect you," said Mitchell.
- Wash your face after removing the mask. Be sure to wash your hands first so you don’t contaminate your face with any virus particles. When you remove the mask, avoid touching the front.
- Put retinols on pause. If you normally use an anti-aging skin product that contains retinols, you might want to put it aside for now. These products can work well for staving off wrinkles, but they can also make your skin more prone to irritation from a mask.
- Use a calming skin product at night, especially if your skin is irritated. Try an ointment, like Aquaphor Healing Ointment or Vanicream HC (it contains hydrocortisone to help with inflammation). Use ointments sparingly and for a short period. Or use a balm. Aveeno Eczema Therapy Itch Relief Balm, according to Mitchell, is "especially helpful."
- To prevent or treat maskne, use an acne face wash that contains salicylic acid. If you have dry skin and you’re experiencing acne breakouts, follow up with a light moisturizer such as Vanicream Light Lotion or Cetaphil Moisturizing Lotion. You might want to also use an acne spot treatment containing salicylic acid or benzoyl peroxide. Another good acne spot treatment option is adapalene, a 1% retinol gel that is now sold over the counter under various brand names. "Adapalene is a great treatment for acne and is used regularly in our dermatology practice as a first-line therapy. Apply a pea-size amount nightly to acne-prone areas," said Mitchell. For persistent acne, a healthcare provider can prescribe a prescription-only product.
- Change and wash cloth masks regularly. A dirty, sweaty mask will contribute to maskne. Wash cloth masks after each use, either in a washing machine on the warmest setting appropriate for the fabric or by hand washing following instructions from the CDC. Don't touch the front of the mask when you remove it, and wash your hands after handling it.
Not sure exactly what's happening with your skin? Get a diagnosis from a dermatologist. If you have a pressure ulcer or infection, you may need a prescription. A dermatologist can also prescribe products to help with acne, rashes and inflammation.
Book an appointment with a Water's Edge Dermatology certified provider by calling (877) 544-3880 or by booking an appointment online.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Home Remedies for Poison Ivy
Medical review by Ted Schiff, MD
Despite the miserable itching it causes, poison ivy rash clears up on its own and can usually be treated at home.
For mild to moderate cases, the home remedies below can help ease the itching. Before you do anything else, thoroughly wash exposed skin with soap and water to remove the culprit, an oil called urushiol, and put any clothing that touched the plant directly into the washing machine (wear gloves).
What to use
- Antihistamine pills. Poison ivy rash is caused by an allergic reaction to urushiol. An oral antihistamine can take the edge off the itching. Follow the directions on the package.
- Hydrocortisone. If you have over-the-counter hydrocortisone cream, now is the time to break it out. It can relieve the itching by decreasing inflammation. Use it for the first few days only.
- Calamine lotion. That’s right - the same lotion you use on chicken pox can help with poison ivy rash as an alternative to hydrocortisone.
- Cold compresses. A cold, wet washcloth can help provide some temporary relief by decreasing inflammation and creating a mild numbing effect.
- Lukewarm baths. Like a cold compress, a lukewarm bath can feel good. Add a store-bought colloidal oatmeal product for benefits that outlast the bath. Don’t have one? Grind whole, uncooked oats into a very fine powder in a food processor. A cup of baking soda is also a good alternative.
- Aluminum acetate. Once the blisters begin to ooze, applying a compress soaked in aluminum acetate solution, which is an astringent, can help dry them up. This can also reduce the itching by shrinking swelling. Domeboro is one brand. Follow the directions on the package.
What not to use
While the following products may seem helpful for poison ivy rash, they can actually make it worse:
- Topical antihistamines (like Benadryl cream)
- Anesthetic creams that contain a pain-relieving agent like benzocaine
- Antibiotic creams that contains neomycin or bacitracin
When to see a doctor
Mild or moderate cases of poison ivy rash don’t usually require a visit to the dermatologist, but if the itching is unbearable, you should make an appointment. The provider can prescribe a corticosteroid cream, pill or injection (in extreme cases). If the rash has become infected, the doctor might also prescribe an oral antibiotic.
You should also see a dermatologist if you’re uncertain what triggered the rash.
Though rare, severe reactions to urushiol can happen and require medical attention. If you have a fever, you’re having trouble breathing, you have a rash near or around your eyes, mouth or genitals or the rash covers most of your body, seek medical help immediately. It is also advised to see a dermatologist if the rash covers a large portion of your face or doesn’t improve after a few weeks.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Survey: Despite Cancer Risk, Many Don't Practice Sun Safety
With summer right around the corner, it's time to think about sun safety. Skin cancer is common — in fact, it's the most common cancer in the United States — yet according to a new survey from the American Academy of Dermatology, only 41 percent of Americans surveyed said they regularly protect themselves from the sun’s rays while outdoors. More than a quarter of respondents said they never or rarely use sun protection.
Here are the survey findings at a glance:

To guard against melanoma and other forms of skin cancer, it's important to apply a broad-spectrum, water-resistant sunscreen with an SPF of 30 or higher to all exposed skin. Reapply every two hours or after swimming or sweating. Staying in the shade, especially when the sun is at its strongest (between 10 a.m. and 2 p.m.), is also important, though it doesn't replace the need for sunscreen. (Sunlight can hit you from other angles, and it's reflected by sand and other surfaces.)
RELATED: How to Choose a Sunscreen
Don't forget to wear a wide-brimmed hat and sunglasses with UV protection. Whenever possible, wear pants and a long-sleeved shirt.
If you're among those who don't always use sun protection, consider these disturbing statistics from the American Academy of Dermatology:
- More than 9,500 people are diagnosed with skin cancer every day.
- Nearly 20 Americans die every day from melanoma, the deadliest form of skin cancer.
According to the Skin Cancer Foundation:
- One in five Americans will develop skin cancer by age 70.
- More than two people die of skin cancer in the United States every hour.
Whether or not you practice sun smarts, it's important to check yourself regularly for signs of melanoma. The reason? The disease has a five-year survival rate of 99 percent — but only if it's detected early.
Look for moles and other spots on your skin, keeping in mind the ABCDE rules found here. Most melanomas tend to have one or more of these ABCDE traits, and some have several.
If you think you see signs of melanoma or another type of skin cancer, make an appointment to see a Water’s Edge Dermatology provider right away.
It's also smart to get a skin cancer screening from a dermatologist at least once a year. Schedule a screening at Water's Edge Dermatology here or call (877) 544-3880.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Water’s Edge Dermatologists Warn about 'COVID Toes'
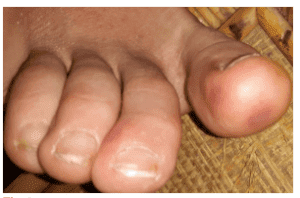
Dermatologists at Water's Edge Dermatology have been warning the public about possible new signs of COVID-19, the novel coronavirus. They include various coronavirus rashes as well as red or purple discolorations on the hands and feet, especially the toes. The phenomenon has been dubbed "COVID toes."
Dr. Alissa O'Brien on CBS12 News
On an April 22 appearance on CBS12 News, Dr. Alissa O'Brien said she's seen several patients who've displayed skin changes that could be the result of the coronavirus. She explained that shortly after hand or foot discolorations appear, small, painful blisters may form, eventually turning into lesions. Other types of rashes have been associated with COVID-19 as well, she noted.
RELATED: Skin Rashes and Purple Spots: Symptoms of the Coronavirus?
If you’re experiencing unexplained rashes or discolorations on your hands or feet with no history of burns, Dr. O'Brien suggested consulting a dermatologist or another physician, at least virtually through telemedicine. If you book a telemedicine appointment, you should be able to send a photo to the provider in advance for assessment. She also suggested inquiring about getting a COVID-19 test if the provider doesn’t mention it. Anyone who is carrying the disease must be isolated to avoid spreading it to others.
Dr. Ted Schiff in Lake Okeechobee News
In an April 22 article in Lake Okeechobee News on purple spots on the toes or fingers, Dr. Ted Schiff, founder and chief medical officer of Water's Edge Dermatology, was cited as an expert source. He explained that the spots are possible early signs of COVID-19 and called them "not an uncommon finding in coronavirus." In children and young adults, he said the spots or a rash may be the only indication of coronavirus infection.
Dr. Schiff noted that the reason for the spots is not yet clear, but constriction or blockage of a blood vessel may be the culprit. The blood vessels can open and close in response to impulses from the nervous system, he said, and COVID-19 can affect the nervous system. The spots may eventually scab over.
Spots don't mean the person has the coronavirus, only that they might — and should get tested if possible. They should also be isolated from others. "If I were a parent and I saw this, I would protect others from this child," said Dr. Schiff. It could save a life, he added.
According to the article, Okeechobee County appears to have only a few confirmed cases of COVID-19, but it's likely that more people have the disease and don't know it or haven’t been tested.
If you or your child is experiencing skin changes like the ones described here, note that Water’s Edge Dermatology offices remain open. Water's Edge Dermatology is also offering teledermatology visits for many skin conditions. To book a TeleDerm visit with a Water's Edge Dermatology provider, go to wederm.com/telederm-appointment.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
Skin Rashes and Purple Spots: Symptoms of the Coronavirus?
Medical review by Ted Schiff, MD
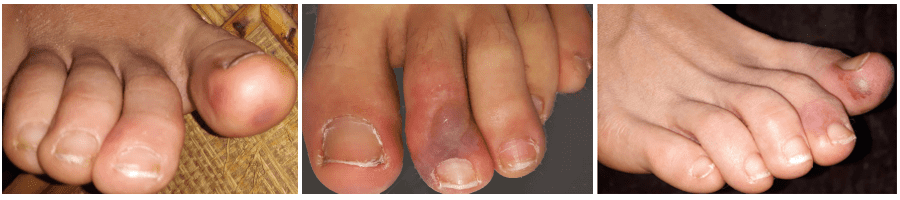
Fever, tiredness, dry cough and shortness of breath are common symptoms of the new coronavirus called COVID-19, but not everyone who develops the disease has the same symptoms. Some people may get a runny nose, sore throat or diarrhea or lose their sense of smell. Doctors are also seeing skin rashes on the body and purple spots on the feet, toes and (less commonly) the hands in some patients diagnosed with coronavirus. (These spots are being dubbed "COVID toes.") In some cases, the coronavirus skin rash or spots may be the first or even the only symptom of COVID-19.
“There have been an increasing number of reports of skin rashes and other skin manifestations, and this is something we’re watching very closely,“ said Ted Schiff, MD, founder and chief medical officer of Water’s Edge Dermatology.

Photo credit: International Federation of Podiatrists
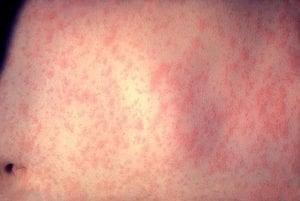
Virus-induced rashes, like the coronavirus skin rash, are not uncommon. They can happen as a result of the immune system’s attempt to fight the invader. With COVID-19, doctors in several countries have reported seeing various types of skin changes, including:
| Exanthems, especially on the torso: widespread, patchy red rashes |
|
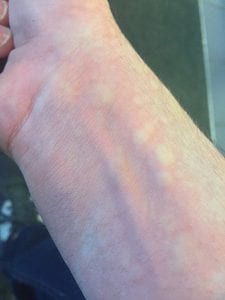
| Urticaria (hives): red or skin-colored bumps that appear suddenly |
|
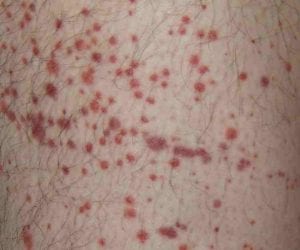
| Purpura Petechiae: clusters of small round spots that may look like a rash and that result from broken blood vessels |
|
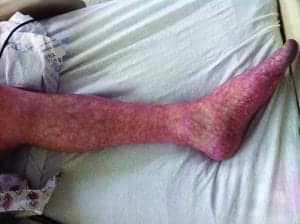
| Livedo reticularis: mottled skin, often on the legs, caused by obstructed small blood vessels near the skin |
|
| Foot and toe lesions: purple spots (aka "COVID toes"), similar to chilblains (lesions caused by blood-vessel narrowing upon exposure to cold air), that may be painful |
|
The purple spots appearing on toes, feet and sometimes hands, which may resemble a bruise, are thought to result from blockages or tiny clots in small blood vessels. For reasons not yet understood, the coronavirus rash appears to occur more often in children and adolescents with COVID-19 than in adults. Some doctors are reporting cases thought to be associated with COVID-19 in which the spots cover the entire tip of the toe. At least one case of scabbing has been reported. The spots heal on their own and don’t appear to dangerous.
Since children infected with SARS-CoV-2, the virus that causes COVID-19, often have no other symptoms of the disease — even though they can pass the virus on to others — purple spots can be helpful as possible signs of infection.
People with unusual skin changes should contact their healthcare provider. A virtual visit with a board-certified dermatologist, primary care physician or pediatrician is likely the best option in non-emergency cases. When a skin change is the primary symptom or the only symptom, a dermatologist may be best equipped to provide an accurate diagnosis.
If the doctor suspects COVID-19, he or she will recommend self-quarantine for 14 days and can help you determine if testing is needed and available.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
What Is a Teledermatology Visit and What Can I Expect?
Medical review by Ted Schiff, MD
You know what a dermatologist is — a doctor who treats skin conditions. (Dermatologists also treat hair and nail conditions.) And perhaps you’ve heard of telehealth, aka telemedicine. They let health practitioners assess, diagnose and treat patients from afar through telecommunications technology, such as video conferencing apps or secure telehealth websites. You can probably figure out, then, that teledermatology is the practice of dermatology from afar.
What is a teledermatology visit?
A teledermatology visit is a virtual appointment with a dermatologist or certified dermatology provider through a smartphone, tablet or internet-connected computer that has a camera and microphone. You can use a telederm visit to address any number of new or existing dermatology-related problems, from acne to rashes to suspicious growths, without leaving the house or missing work and without wasting time in the waiting room. Another bonus is the cost effectiveness: A teledermatology visit is often significantly cheaper than an in-office visit. (These visits are covered by most insurance plans, just like an in-office appointment.)
During the online visit, you and the provider can see and hear each other. You can discuss your current health situation, and you can show the provider any problem areas. You may be able to upload a digital image to the dermatology practice’s patient portal before the visit for the medical team to review before and during the visit.
If the provider decides you need to be seen in person, you can schedule that appointment after the telederm visit. In many cases, the cost of the telederm visit can be applied to that in-person appointment.
Conditions and symptoms that can be addressed
A wide variety of skin, hair and nail conditions can be assessed, diagnosed and treated through a teledermatology visit, including:
- Acne
- Bug bites
- Contact dermatitis
- Cold sores
- Cysts
- Eczema (atopic dermatitis)
- Hair and nail disorders, including alopecia (hair loss)
- Hives
- Lesions
- Moles
- Psoriasis
- Rashes
- Rosacea
- Warts
- Skin cancer surgery (post-procedure follow-up)
- Wounds
In many cases, you can also get a prescription and refill through a teledermatology visit.
Conditions and symptoms that require an in-office visit
If you have a suspected melanoma, the most dangerous form of skin cancer, you will likely need a biopsy — a procedure that requires an in-office visit. You’ll also want to get annual, full-body skin cancer screenings in person if you have a history of melanoma.
Certain symptoms and conditions require immediate medical care at an emergency room or urgent care clinic, including but not limited to heavy bleeding, deep wounds or cuts, facial lacerations, a rash with fever, an allergic reaction that causes breathing trouble and a spider bite that causes extreme pain or other serious symptoms such as fever, nausea or weakness.
How to schedule a telederm visit
Click here to book a telederm visit with a Water’s Edge Dermatology provider.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
How Contagious Is Poison Ivy?

The short answer is no. Poison ivy rash, which is caused by an allergic reaction to oil in the plant, is not contagious. Even the fluid from poison ivy blisters is not contagious. Only direct contact with the plant’s oil, called urushiol, can trigger poison ivy rash.
But here’s the rub: Touching the plant isn't the only way to have direct contact with the oil.
Let’s say you got urushiol on your arm from touching the plant. If someone touches your arm before you wash off the oil, and before your skin absorbs it (which happens in a matter of minutes), they can get poison ivy rash. The same is true if you get the oil on your shirt or your shoe and someone else touches it, or touches a surface on which you placed an item. You can even get poison ivy rash from your dog or cat if the pet comes into contact with poison ivy and you touch the fur or hair.
That’s why it’s important to clean any items — and pets — that come into contact with poison ivy. Remove the clothing you were wearing when you were exposed and put it directly into the washing machine. Don’t drop the clothes on the rug or a chair first, and don’t let them touch the outside of the washing machine. If your shoes came into contact with the plant, clean the shoes and put the shoelaces in the wash. If your pet came into contact with poison ivy, shampoo him or her while wearing rubber gloves. As an extra precaution, you should wash the leash, too.
You should also wash other items that may have come into contact with the plant. That includes garden tools (and gloves), camping equipment, golf clubs, a bicycle you were riding and even jewelry you were wearing. You can wash them or remove the oil with rubbing alcohol.
Note, simply putting items aside to "air out" won’t do anything to prevent poison ivy rash, since urushiol can remain on surfaces for years.
Just as someone can get poison ivy rash if they touch your urushiol-contaminated skin, you can transfer it to other parts of your own body while the oil is still on your skin. Wash your exposed skin with soap and water as soon as possible after exposure. Rinse it with water if you don’t have access to soap, and wash with soap when you do. This also reduces the severity of the rash. Be sure to clean under your fingernails, where urushiol can hide.
Poison ivy rash is no fun, but if you’re smart about removing the urushiol from your body, your clothing, and anything else that may be contaminated with it, you can help prevent others from catching it — and avoid getting re-infected yourself later on.
Written by Marianne Wait, an award-winning health and wellness writer based in New Jersey.
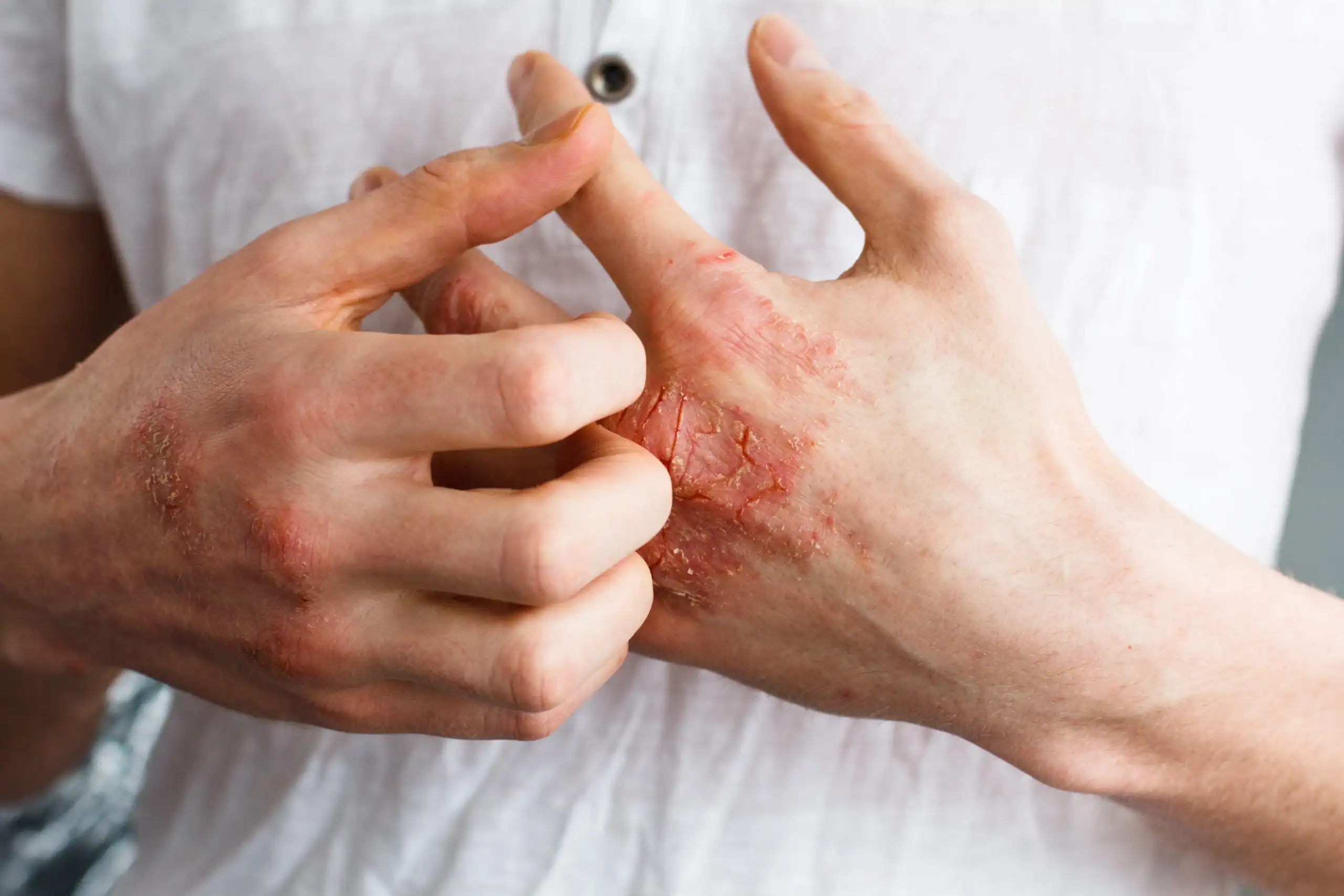
5 Reasons Hand Eczema Flares Up (And How to Tame It)
Hand eczema flare-ups are beyond annoying. It can cause redness, itching, cracks, blisters, and dryness to the point of peeling and flaking, but that’s not all.
During a bad flare-up of hand eczema, fingers can swell and hands can hurt. Without proper treatment, hand eczema can become chronic. A severe case could even make it hard to button your clothes or use a computer.
So, what causes flares? Here are five of the most common triggers and tips for avoiding them.
Trigger 1: Exposure to water
Constantly wetting and drying your hands can break down skin's protective barrier, especially when you have sensitive skin that is prone to dryness. "Even after hands are dried, there's some water left that evaporates. When it does, it reduces skin's natural oils," said Dr. Alissa O'Brien, a dermatologist at Water’s Edge Dermatology. If the water is piping hot, it’s even more irritating and drying.
How to dodge it: For dishwashing and other wet tasks, wear vinyl gloves with a cotton lining (or a separate cotton liner). Latex gloves can cause allergic reactions, so it's best to avoid them. When you wash your hands, use a mild, low-lathering soap free of fragrances, preservatives, and dyes, and use lukewarm water, not hot. After washing and gently drying your hands, apply moisturizer, preferably an ointment. "Aquaphor Healing Ointment is probably one of the best," said Dr. O'Brien. Other ointment brands she recommends include Vaseline, Cetaphil, CeraVe, Eucerin, and Aveeno. If you find ointments too greasy to use during the day, use a cream moisturizer instead and an ointment at night, under a pair of cotton gloves.
Trigger 2: Exposure to allergens or irritants
Hand eczema is often caused or worsened by exposure to a substance that’s irritating — think alcohol, bleach, cleansers or solvents — or one that causes an allergic reaction, such as perfume or certain plants. Florists often get dermatitis on their thumb and forefinger when clipping chrysanthemums and tulips (it’s known as "tulip fingers"). In the kitchen, vegetables — particularly garlic and onion — can lead to a flare-up, especially on the fingertips. Even fabric can exacerbate hand eczema. Rough, coarse materials such as wool and stiff synthetics such as polyester can trigger an itch-scratch cycle that worsens the condition.
How to dodge it: Pay attention to what sets off your eczema. "Whether you're at home or on the job, learn what irritates your skin and avoid or limit contact with those things," advised Dr. O'Brien. Use a washing machine, dishwasher, and food processor when possible and ask other family members for help with housework, cooking and gardening to give your hands a break. Protect your hands from irritants and allergens by wearing vinyl or cotton gloves while you do chores. Wear heavy-duty vinyl or neoprene gloves at work if you’re exposed to triggers there. If the gloves you have irritate your skin, ask your dermatologist for recommendations.
Trigger 3: Stress
Stress triggers the production of hormones, including cortisol and adrenaline, that can suppress the immune system and cause an inflammatory response in the skin. An eczema flare-up can create even more stress, leading to a vicious cycle. If you’re under a lot of emotional or physical stress, you may be at greater risk of dyshidrotic eczema, a type that causes itchy blisters on the palms of the hands that may be filled with fluid.
How to dodge it: Exercise is an excellent way to manage stress. In addition to boosting the production of feel-good chemicals, it also improves sleep, which can help to further decrease stress. To ease anxiety on the spot, take slow, deep, belly-expanding breaths in through your nose and exhale through your mouth.
Trigger 4: Sweating
Whether you’re walking outside, playing with your kids, or exercising, sweating can irritate the skin. The salty residue that’s left behind after sweat evaporates is known to worsen the itch. Some research suggests that people with eczema are more prone to excessive sweating.
How to dodge it: Keep a towel with you as you work out or when you’re outside to wipe away sweat, and rinse off sweat with lukewarm water afterward to prevent salty build-up. Because wearing gloves, especially waterproof gloves, can make your hands sweat, take them off frequently (every 20 minutes or so) to let your skin cool down.
Trigger 5: Physical wear and tear
Minor hand trauma from tasks like digging in the garden with bare hands can cause hand eczema or make it worse, as can friction from activities like handling large quantities of paper.
How to dodge it: Wear task-appropriate gloves. Cotton and fabric gloves can keep hands clean and protect against abrasions, but they may not be adequate for work with rough or sharp materials. Working with thorny plants, palm fronds or brambles may require leather gloves with longer cuffs.
Avoiding eczema triggers often goes a long way toward managing the condition. The key is to be diligent. "It can take a massive amount of effort if you have severe hand dermatitis, and people often want a quick fix, but putting in that effort to take care of your skin really pays off in keeping eczema from coming back," said Dr. O'Brien.
Don’t get discouraged: Hand eczema can be stubborn, and it may take a few months for the patches of red, scaly and inflamed skin to fully heal. After that, your eczema is less likely to return.
END
Article Written By: Karyn Repinski, a Brooklyn, NY-based award-winning health and beauty writer.
Medical Review By: Ted Schiff, MD