How to Identify Scabies (With Pictures)
Medical review by Ted Schiff, MD
If your skin has red bumps that are mighty itchy, the cause could be a mite. Here’s what to know about the contagious infestation known as scabies and how to recognize it so you or your child can get treated before the itching becomes unbearable.
What is scabies?
Scabies is a skin condition caused by an infestation of microscopic eight-legged mites called Scarcoptes scabiei. The mites cause extreme itching and a rash. Symptoms develop after pregnant female mites burrow into the skin and lay eggs. When the eggs hatch, the young mites return to the surface of the skin via the burrows created by the females. Without treatment, the cycle repeats itself as the young mites mate and tunnel under the skin to lay their eggs.
What does scabies look like?
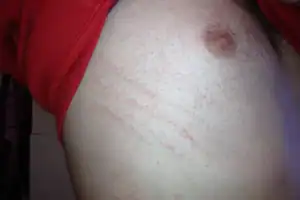
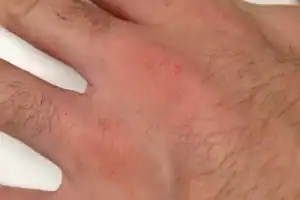
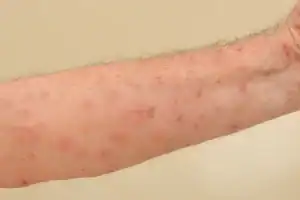
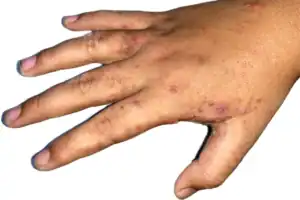
The scabies rash takes the form of small, red bumps that may look like pimples, bug bites, hives or knots under the skin. You might be able to see the burrow tracks created by the mites, which appear as raised lines of tiny blisters or bumps. Some people develop scaly patches that resemble eczema.
Because the rash is so itchy, sores may result from constant scratching and can become infected. Itching is worse at night and can interfere with sleep.
A less common and more severe type of scabies called crusted or Norwegian scabies happens when an exceptionally large number of mites invades the skin. There may be hundreds or thousands of mites compared with only 10 or 20 in typical scabies. People with crusted scabies develop thick crusts of skin that contain mites and eggs. They may or may not experience itching and a rash.
Once someone has been exposed to scabies, symptoms develop four to eight weeks later. (In someone who’s had scabies before, symptoms may develop in just a few days.) It’s possible to spread scabies to others during the pre-symptomatic stage as well as the symptomatic stage.
Adults who contract scabies tend to develop the rash in certain areas of the body, which include:
- Armpits
- Between the fingers
- Inner elbows
- Sides of the wrists
- Waist
- Around a nipple
- Knees
- Buttocks
- Male genitals
- Soles of the feet
- Areas covered by jewelry like bracelets, watches and rings
Infants and very young children are more likely to get scabies on the:
- Head
- Face
- Neck
- Palms
- Soles of the feet
How do you get scabies?
Scabies is transmitted by prolonged skin-to-skin contact with someone who has it. A quick hug or handshake is unlikely to spread scabies; you’re more likely to get it from a member of your household or through sexual activity. You can also contract scabies by touching personal items that someone with scabies has used, such as towels, furniture, bedding and clothing, though this mode of transmission is less common. You cannot get scabies from an animal that has mites.
Who gets scabies?
Scabies has nothing to do with poor personal hygiene or dirty surroundings. In truth, anyone can get it. People who are more vulnerable to contracting scabies include:
- Children
- Mothers of young children
- Sexually active young adults
- People who live in group settings, such as nursing homes, assisted living facilities and extended care facilities
- Elderly people
- People with a weakened immune system
- People who have received an organ transplant
Crusted (Norwegian) scabies primarily affects elderly people and those with a weakened immune system, disability or neurological condition. It’s more contagious than typical scabies because it spreads via person-to-person contact and also through the shedding of the skin crusts. When crusts fall off, the mites inside can survive for up to a week, which gives them time to find another host.
Scabies treatment
If you suspect you might have scabies, see a dermatologist promptly. He or she will check for signs of mites and may take a skin scraping from the area and look for mites and their eggs under a microscope.
Scabies is treated with prescription medications called scabicides, which kill the mites. Permethrin 5% is the most commonly prescribed scabicide. While these medications kill mites quickly, the itching may last for several weeks. Skin usually heals within four weeks.
Treating crusted scabies is more challenging, and treatment may last for several weeks or longer if necessary. People with crusted scabies may be prescribed both a scabicide and another mite killer called benzyl benzoate, along with a keratolytic cream, which helps reduce crusting of the skin and allows for better absorption of permethrin or benzyl benzoate.
Some scabies patients may be prescribed additional medications such as an antibiotic (if an infection is present) and medications to help control itching, such as a steroid cream and antihistamine.
Because scabies is highly contagious, your dermatologist may recommend that members of your household and your sexual partner(s) be treated for scabies as well. You’ll also need to do a thorough cleaning of your home, including vacuuming floors, rugs and all upholstered furniture. (Discard the vacuum bag afterward.) Items such as towels, sheets, blankets and clothing should be washed in hot water and dried on high heat or dry-cleaned. Another option is to seal the items in a plastic bag for at least 72 hours, since mites that aren’t in skin crusts die within a few days without a host.
The good news is there’s no need to use insecticides or fumigants to get rid of mites — in fact, the Centers for Disease Control and Prevention doesn’t recommend them — so you don’t have to expose your family to these chemicals or endure their odor to make your home safe again. And, since the scabies mite can’t survive on animals, there’s no need to treat your pet.
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.
*Wikimedia Commons photo licenses:
Man's chest with scabies: Fhgd, CC BY-SA 3.0 via Wikimedia Commons
Hand scabies: Fhgd, CC BY-SA 3.0 via Wikimedia Commons
8 Common Skin Conditions in Elderly Adults
Medical review by Ted Schiff, MD
Like every part of the body, the skin changes with age. The teen years bring dreaded pimples. Middle age brings telltale wrinkles. In elderly adults, skin conditions may become more numerous — and more noticeable — as the skin continues to thin and lose fat, elasticity, and moisture.
Skin cell turnover decreases dramatically, which slows wound healing. Aging weakens the immune system, so skin infections are more common. Age spots may take up more acreage. Large, dark bruises may spring up out of nowhere.
Some skin problems, like dark bruises, are alarming but are mostly harmless. Others require medical attention. Here are eight skin conditions in elderly adults and what older adults, loved ones and caregivers should know.
1. Easy bruising
Why do old people bruise easily? Aging skin is thinner, and there’s less fat to act as cushioning. Also, blood vessels are more fragile and easily broken. Bruises happen when blood leaks out of blood vessels, so more broken vessels means more bruising. Older people who take blood thinners or even over-the-counter painkillers such as aspirin or ibuprofen may bruise more easily.
A minor bump or scrape can result in a surprising amount of bruising and make concerned loved ones wonder what’s happening. The bruises are usually harmless. But anyone who often develops large bruises with no logical explanation should see a doctor to rule out an underlying health problem.
If a loved one or caregiver has any reason to suspect abuse as the cause of bruising, they should investigate. Most accidental bruises occur on the extremities, according to the National Institute of Justice, whereas bruises in abused elders are more likely to occur on the head, neck or torso, and they tend to be large.
Take action
To treat bruises:
- Apply a cold compress for up to 20 minutes a time.
- Apply Dermaka cream, a bruise treatment made with plant extracts and vitamins, according to the package directions.
- If a leg or foot is bruised, keep it elevated when resting.
2. Dryness and itching
Dry skin in elderly adults is very common; in fact, more than half of older adults have it. A loss of sweat and oil glands is one reason. Not drinking enough liquids may be another. In addition, certain chronic health conditions, such as diabetes and kidney disease, can cause dryness and itching, as can some of the medications used to treat them.
Skin may become cracked and painful. Scratching can cause skin irritation and open the way for infection-causing germs to enter.
Take action
If you have dry, itchy skin:
- Take shorter, cooler baths or showers and use a moisturizing soap (skip the deodorant soap)
- Use a moisturizing ointment or cream daily. (Avoid lotions, which contain more water.) CeraVe, Cetaphil and Vanicream all make gentle, effective moisturizers.
- Drink more water.
- Run a humidifier if the air is dry.
- If the itching doesn’t subside, tell your doctor. It could be a sign of liver, kidney or thyroid disease.
3. Age spots

Take action
- Wear sunscreen with at least 30 SPF to help prevent more age spots from developing.
- See a dermatologist to make sure the spots are in fact age spots and not something else, especially if they change in appearance.
- If your age spots bother you, a skin care provider can treat them.
4. Skin tags
Skin tags are soft, spongy, often flesh-colored growths of tissue that typically appear on eyelids, neck, thighs and skin folds such as the armpits, groin and under the breasts. They may hang from the skin on small stalks. Skin tags are more common in women, people who are overweight, older adults and people with diabetes. They can become irritated if clothing rubs them or jewelry snags them.
Take action
- Skin tags are harmless, but if you want one removed, see a dermatologist. A dermatologist will remove it for you.
- Don’t try to remove a skin tag yourself. It’s a bad idea for several reasons.
5. Skin cancer
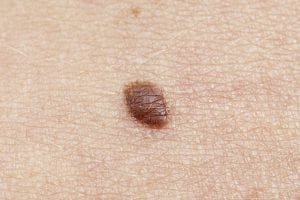
Take action
- Perform a skin check once a month to look for new growths and changes in existing moles. Evaluate moles using the ABCDE test. Make an appointment with your dermatology provider if you see something suspicious.
- Have a skin cancer screening based on the schedule your dermatologist recommends, but at least once a year.
6. Shingles
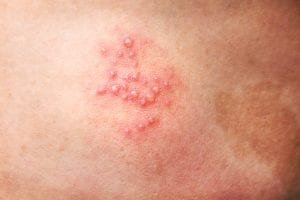
Shingles starts with burning, itching, tingling or extreme sensitivity in one area of the skin. A painful rash then develops, often along with a fever or headache. The rash eventually blisters. Skin infections and long-term nerve pain are possible complications.
Take action
- See a doctor as soon as symptoms appear. Early treatment with an oral antiviral medication may reduce the duration and severity of an outbreak.
- Take an over-the-counter pain medication for pain and use cool compresses, calamine lotion and lukewarm baths with colloidal oatmeal (oats ground into a fine powder) for itching.
- To prevent shingles, get both doses of the Shingrix vaccine.
7. Bed sores
Bedridden or wheelchair-bound older adults are susceptible to open wounds called bed sores or pressure ulcers. These develop in areas subject to pressure when you sit or lie down, such as the tailbone, shoulder blades, backs of the knees and heels. People with diabetes, poor circulation or poor nutrition face a higher risk of bed sores.
Prevention is critical. Bed sores can be very difficult to treat once they develop, and they may become infected.
Take action
- In bed, reposition every two hours. In a wheelchair, change position every 15 minutes.
- Keep skin clean and dry.
- Watch for redness and warmth in one area of the skin; it’s an early warning sign. If you’re a caregiver, call the doctor if you notice this or see a sore, scrape or blister. A wound care nurse may be needed to coordinate care.
- Consider a gel or foam mattress topper or a mattress with alternating air pressure, which can help prevent pressure sores.
8. Skin tears
The fragile skin of elderly adults tears more easily, especially in people who take oral or topical corticosteroids, which can weaken the skin. The skin might tear when you bump into something, or when a caregiver removes wound tape or dressing.
Take action
- Use moisturizer and drink plenty of water to keep skin hydrated, which can help prevent tears.
- Wear long pants and a long-sleeved shirt or arm sleeves to protect the skin.
- If a small tear occurs, wash the wound with gentle soap and water. Put the skin flap back in place if there is one, then cover the wound with gauze.
- See a doctor for more serious tears or if you notice signs of infection, such as redness, swelling, fever, worsening pain or a bad odor.
Written by Jennifer L. Cook, an award-winning editor and writer whose work has appeared in Good Housekeeping, Prevention, Consumer Reports on Health, and Woman’s Day and on Investopedia.com and Bottomlineinc.com.
Why Diabetes Can Cause Dry, Itchy Skin
Medical review by Richard Levine, MD
If you have diabetes, you may know it can affect your heart, kidneys and nerves, particularly if the disease is poorly controlled. But did you know it can also cause dry, itchy skin?
An estimated 79% of people who have diabetes mellitus, the most common form, experience skin issues such as dryness, itching and infections. These can develop at any point during the course of the disease. In some cases, they may even be the first sign that a person has diabetes.
The connection between diabetes and itchy skin
Diabetes can make the body lose too much fluid through urination and evaporation through the skin. The result: dry, itchy skin that can be bothersome and sometimes uncomfortable.
Itching, especially in the lower legs and feet, can also be caused by poor circulation, which is common with diabetes. Some people experience a skin reaction to their diabetes medication or insulin injections.
In addition, itching can be brought on by diabetes complications including nerve damage, kidney disease and liver disease. Certain medications for other health problems common in people with diabetes, such as high blood pressure and high cholesterol, can make the skin itchy, too.
Scientists suspect that those with type 2 diabetes may be vulnerable to itchy skin (and also skin infections) for yet another reason: Their skin’s barrier function is impaired. Exactly how and why this happens is still being studied.
Diabetes and skin infections
Studies suggest that more than half of people with diabetes will develop a skin infection at some point.
Scratching and dryness can create cracks that let bacteria in. It’s not unusual for people with diabetes to develop bacterial infections such as folliculitis, boils and carbuncles.
Itchy fungal infections are also more likely in people with diabetes, possibly due to high blood sugar. Infections caused by the yeast-like fungus Candida albicans often crop up in areas with moist folds, such as the armpits, groin area, under the breasts and between the fingers and toes. Infections caused by mold-like fungi called dermatophytes include ringworm, jock itch and athlete’s foot.
Skin care tips for people with diabetes
If you have diabetes, good skin care is an important part of managing your disease. These tips can help keep your skin soft, calm and infection free.
Keep your blood sugar under control. Follow your doctor’s plan to manage your blood sugar levels. When your diabetes is well managed, your whole body, including your skin, benefits.
Take lukewarm showers and use a moisturizing soap. Hot baths and showers dry out the skin. Dry off well after your shower, especially under the arms and breasts and between the legs and toes.
Use a gentle moisturizer. A cream or ointment is preferable to a lotion since lotions contain more water. Ask your dermatologist for a recommendation. Don’t moisture between your toes.
Avoid scratching if you can. Scratching can create openings in the skin that let in bacteria.
Consider using a humidifier in winter. Dry air can make dry skin worse.
Wash minor cuts right away with mild soap and water. Talk to your doctor about using an antibiotic cream or ointment. Cover the cut with a bandage. Deep cuts require professional treatment.
Practice good foot care. Examine your feet daily. Look for any cuts, blisters or sores. Unless the wound is minor and heals on its own, see a doctor right away. When you cut your toenails, cut them straight across and not too short. Smooth the corners with a nail file if necessary.
Your dermatologist can help
A dermatologist can get to the bottom of why your skin is itching and offer treatment suggestions. He or she can also diagnose and treat other diabetes-related skin problems that don’t involve itching.
Prompt treatment of skin problems is especially important when you have diabetes. See a dermatologist or other doctor if you have signs of an infection. A bacterial infection may cause redness, pain, swelling and oozing. Fungal infections typically itch. The skin may also be red, scaly, swollen, or blistered.
If you develop severe itching, consult your dermatologist or diabetes doctor without delay. It could be a sign that your diabetes treatment plan isn’t working.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
Are Chemical Peels Safe?
If you’re tired of seeing fine lines, acne scars, sun spots, or dark patches every time you look in the mirror, you may be considering getting a chemical peel. In this procedure, a mixture of acids is applied to the skin to slough off the top layers and reveal the smoother, more even-toned skin beneath. But just how safe — or dangerous — is a chemical peel?
“When patients ask me about peels, they’re often nervous and have a lot of questions,” said Shawna Sopher, a licensed medical aesthetician at Water’s Edge Dermatology. Some of them are remembering a 2002 episode of the TV show “Sex in the City” in which a character named Samantha undergoes a peel and ends up with raw, red skin that hurts whenever she moves her face. “Patients still bring up that storyline all these years later,” Sopher said.
Samantha’s experience wasn’t very realistic then, and it’s even less realistic now that peels have become gentler. Here, Sopher and Jenna Steffel, APRN at Water’s Edge Dermatology, answer the questions they hear most about chemical peels.
What conditions can be treated with a chemical peel?
Chemical peels are often ideal for treating scars, fine lines, uneven skin tone, and sun damage, which typically call for a mild- to moderate-strength peel. These peels can be performed by a licensed aesthetician.
Chemical peels are also beneficial for acne, noted Sopher. “I have many acne patients who get a peel every six months because it does a better job of drying up oil and clearing blackheads than a lot of other treatments on the market,” she said.
Deep peels, which penetrate the epidermis (the top layer of skin) and into the dermis, can address wrinkles, severe sun damage and precancerous cells. These peels can also stimulate new collagen production, making skin look younger and smoother. Due to the depth of the peel, deep peels are performed only by a dermatologist or other medical provider, and are a once-in-a-lifetime treatment.
"The patient condition and skin type dictate the depth of peel needed to achieve the desired outcome,” Steffel said.
Are chemical peels safe for sensitive skin?
Most people with sensitive skin can tolerate today’s milder peels. “In the past, there was just one very strong acid practitioners could use,” Sopher said. “But now, there are gentler acids that can be mixed together and tailored to a patient’s skin type.”
It’s best to get a chemical peel from an experienced, board-certified dermatologist or a licensed aesthetician working at a dermatology practice rather than finding the best deal on Groupon, Sopher added. The provider you choose should have the skills and knowledge to evaluate your skin and select a chemical mixture that’s both safe for your skin and best suited to the problem you want to treat.
Are chemical peels safe for dark skin?
Superficial to medium-depth peels are sometimes used successfully in people with dark skin to treat problems such as acne, melasma and post-inflammatory hyperpigmentation (dark spots). While peels can lighten dark spots, in some cases they can also cause them. That’s why it’s important to consult with a skin care provider who has significant experience treating skin of color before having a peel.
Deep peels are not recommended for people with darker skin. They can lead to hyperpigmentation or hypopigmentation (areas of lighter skin).
Who should avoid getting a chemical peel?
Peels are not recommended for anyone who is pregnant or nursing, has inflamed acne or a sunburn or is taking Accutane. People who use retinoids can get a chemical peel but must stop using the product three to four days before treatment.
What happens during the procedure?
For a mild to moderate peel, the provider will cleanse your skin with a degreasing treatment, then apply the chemical one layer at a time, checking the skin after each application (called a pass) for any unwanted reaction. Most people require about four passes, Sopher said, though people with thicker, oilier skin may need up to six passes. The process usually takes less than 30 minutes.
A deep peel uses a stronger chemical, usually phenol, and takes about 90 minutes. You may be given a local anesthetic and a sedative to make the procedure more comfortable. To prep your skin for the peel, you’ll need to follow a pre-treatment plan for up to eight weeks prior to your appointment. The provider will also give you post-treatment instructions to follow.
Do chemical peels hurt?
Mild to moderate peels can be somewhat uncomfortable. “Your face will feel hot, but you’ll be given a handheld fan to rest on your chest during the procedure to minimize the sensation,” Sopher said. Your skin may also feel prickly and tight after each pass.
Following the treatment, you’ll be given a calming cream you can use to manage any lingering warmth and tingling. Within six to 10 hours after the procedure, your skin will cool down. Any redness will fade over time.
After a deep peel, your face may feel hot and uncomfortable for some time. Your eyelids may swell shut. Your doctor may recommend taking a pain reliever and using ice packs as needed.
How long does it take to see results?
After a mild or moderate peel, you should see a difference in two weeks or less. Your skin will start peeling approximately three or four days after the treatment.
“The amount of peeling can vary from a little flakiness to sheets of skin coming off your face,” Sopher explained. “People sometimes don’t peel much and worry that the treatment was ineffective, but there’s no relationship between the amount of peeling and how well the treatment works.”
After a deep peel, you’ll see new skin begin to appear after two weeks. You may experience significant peeling, along with redness, swelling and crusting as the skin heals. Any swelling should go down in a couple of weeks. Redness may linger for up to three months.
How often is too often?
Your skin care provider will recommend how many peels you need in order to achieve the outcome you want. More is not always better. Typically, mild peels can be performed as frequently as every one to two weeks, and moderate peels, every four to six weeks.
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. She has written for Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many other outlets.
What’s the Difference Between Eczema and Psoriasis?
Medical Review By: Ted Schiff, MD
If you have bothersome patches of itchy, red skin, you want relief. But first you need to know what’s causing the problem. If you’ve ruled out insect bites, poison ivy and other types of allergic contact dermatitis, then eczema or psoriasis may be likely contenders. These skin problems can look somewhat alike at first glance, and some of the treatments overlap, but they are distinct conditions with different causes and triggers.
Eczema and psoriasis are both inflammatory skin conditions that run in families and involve the immune system. They often arise in childhood, though more cases of psoriasis begin in adulthood. It’s possible to have both eczema and psoriasis.
The exact causes of eczema aren’t fully understood. People who get eczema may have a family history of eczema, asthma, hay fever or food allergies or sensitivities. The most common type of eczema is atopic dermatitis.
In plaque psoriasis, the most common type of psoriasis, the immune system goes into overdrive, causing new skin cells to develop much faster than normal. These cells pile up on the skin’s surface, causing bumpy, scaly patches called plaques, as you can see in the top photo. Psoriasis is linked with other inflammatory illnesses, including psoriatic arthritis, so getting an accurate diagnosis is important.
Below are some clues your skin care provider will use to tell the conditions apart.
Signs and symptoms
Eczema and psoriasis usually look different upon close inspection, and they feel different, too.
In eczema, the skin tends to be very dry and intensely itchy. In Caucasians, eczema patches appear red; in people with darker skin, the patches may look darker brown, purple or gray. Scratching can cause the skin to break, ooze, bleed and eventually crust. Over time, leathery dark patches may develop in the surrounding skin due to repeated scratching.
Psoriasis patches tend to be raised and well-defined — it’s usually obvious where a patch begins and ends. In Caucasians, the patches look pink or red with thick, silvery-white scales on top. In darker skin, the patches can be dark brown or purple, and the scales may be gray. In people with skin of color, the patches may be more widespread.
One big difference between the two conditions: Eczema causes intense itching, whereas psoriasis may itch mildly but also sting and burn.
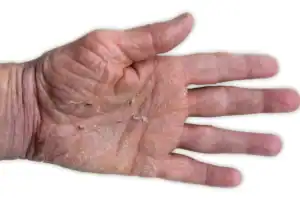
Location Matters
Eczema and psoriasis can show up just about anywhere on the body, but they are more common in some areas than others.
Eczema commonly appears on the:
- Hands
- Backs of the knees
- Insides of the elbows
- Back of the neck
- Face
- Eye area (in adults)
Psoriasis commonly appears on the:
- Elbows and knees
- Scalp
- Face
- Lower back
- Palms of the hands
- Soles of feet
- Fingernails and toenails
- Mouth and lips
- Eyelids
- Ears
Common Triggers
The two conditions are typically activated by different triggers.
In the case of eczema, triggers include exposure to skin irritants, such as wool fabrics, detergents or disinfectants and exposure to allergens, such as dust, pet dander, pollen and mold. Stress and sweating are other triggers. In people with hand eczema, frequent hand washing and dish washing can set off the itching.
With psoriasis, a skin injury such as a scratch, bruise, puncture or sunburn can trigger a flare, as can smoking, drinking alcohol, stress and certain medications, such as beta blockers.
Treatment for Eczema and Psoriasis
Treatment focuses on easing symptoms, lowering the risk of skin infection and reducing flares. Moisturizers help with both conditions, as does avoiding triggers.
Eczema treatments include prescription or over-the-counter topical corticosteroids and the topical medication crisaborole (Eucrisa), which blocks certain immune system proteins to reduce the body’s response to triggers. An antihistamine can sometimes help as well. Light therapy is another option. For widespread moderate to severe eczema, a biologic drug called dupilumab (Dupixent) may be given by injection to tamp down the immune system.
Psoriasis treatments include topical creams such as corticosteroids, retinoids and calcipotriene (a vitamin D derivative), light therapy, and for moderate to severe psoriasis, biologic drugs. The drugs, given by injection or infusion, can improve psoriasis symptoms dramatically. Many people achieve clear or nearly clear skin as a result.
Your dermatologist will recommend a course of treatment once an accurate diagnosis is made — so instead of trying to guess what condition you have, make an appointment.
Article Written By: Jennifer L. Cook, an award-winning editor and writer whose work has appeared in Good Housekeeping, Prevention, Consumer Reports on Health, and Woman’s Day and on Investopedia.com and Bottomlineinc.com.
Is Sun Good for Acne?
If you’re constantly battling pimples due to acne, it’s tempting to try just about anything to get rid of them. Some people believe lying out in the sun will help. The thinking goes that sunlight will dry out the oil in the skin and/or prevent oil production, resulting in clearer skin.
Sounds logical, right? After all, excessive oil production often plays a role in acne development, along with other factors such as bacteria and hormone imbalances. But in fact, the dehydrating effect the sun has on the skin ultimately does more harm than good, said Sydney VanHoose, a board-certified advanced practice registered nurse at Water’s Edge Dermatology.
“Sitting in the sun can make it seem like your acne is improving at first, but it leads to more breakouts later,” said VanHoose.
What’s more, if you don’t use sunscreen or cover up with protective clothing when you’re outdoors, you’re exposing yourself to UV rays that could make other complexion issues worse, and even lead to skin cancer.
How the sun triggers breakouts
“After you’ve been in the sun, the epidermis [the top layer of skin] starts to dry and thicken,” VanHoose explained. “When this happens, your body responds by producing even more oil to compensate for what was lost – and that can lead to more breakouts.”
This effect doesn’t occur immediately, which may be why people don’t realize the connection between sunlight and worsening acne. Another source of confusion is the fact that dermatologists sometimes recommend light therapy to treat acne; however, the blue light used in this FDA-approved treatment is very different from the sun’s rays. It kills acne-causing bacteria (P. acnes) without damaging the skin the way UV light does. Sunlight does not kill P. acnes.
Why people think the sun helps
A day, weekend or week in the sun can indeed make a difference temporarily, but not for the reasons people may think. If you get a tan, for instance, that can make red pimples stand out less. The stress-reducing effects of a vacation can also help, since stress is known to exacerbate acne.
A shortsighted trade-off
Even if sun worshipping did somehow lead to a clearer complexion, the other risks it poses to your skin simply aren’t worth it.
"Exposing acne to UV rays without any protection leads to an increased risk of scarring and hyperpigmentation," VanHoose said. "So, while people may think their complexion looks better when they tan, the trade-off is that they’re going to end up with more marks and dark spots, and possibly skin cancer, in the future."
Sun damage caused by unprotected sun exposure can also lead to premature skin aging and wrinkles. "A lot of people who have acne also want to treat fine lines on their face, and the sun’s not going to help with that, it’s going to make it worse," said VanHoose.
Even short bouts of sun exposure contribute to skin damage, so it’s important to wear a broad-spectrum, water resistant sunscreen with an SPF of at least 30 every day. Worried sunscreen will make your face look greasier or cause more breakouts? Read the label and find a product that is oil free and noncomedogenic.
Professional help for clear, beautiful skin
If you feel like you’ve tried everything to clear your complexion and nothing is working, see a dermatologist. “It’s best to get in the office, get a skin exam and have the dermatologist develop a targeted treatment plan that’s personalized for you,” VanHoose said.
A bonus: The dermatologist can recommend or prescribe products that can make your skin clearer and smoother, now and later in life. Retinoids, for example, not only unclog pores but help reduce the look of fine lines.
As VanHoose put it, "You’re going to be pretreating your skin for the future."
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
How to Prevent Head Lice
Fall brings cooler weather, shorter days, and something else: head lice. It’s peak season for the spread of these tiny, scalp-infesting insects. And while cases of head lice aren’t quite as universal as the common cold, American kids between the ages of 3 and 11 experience 6 million to 12 million of them per year.
There’s no surefire way to keep your child from getting head lice, but you can take steps to lower the risk and, if your child does bring them home, prevent the spread to other family members.
How does lice spread?
Lice typically spread through direct head-to-head contact. If you’re wondering how far lice can jump, the answer is, they can’t. (Fleas, yes, lice, no.) Head lice move by crawling.
Head lice affect young children more often than older ones because young kids tend to play closer together. Older kids who engage in contact sports, however, face similar risks.
In African American children, head lice is much less common. The width and shape of their hairs may make it harder for the lice common in this country to grab onto, according to the CDC.
Protecting your child at school or day care
Schools and day cares are hotbeds for head lice transmission. Social distancing rules appear to be reducing head lice cases, but prevention measures are still worthwhile.
If someone at your child’s school has been diagnosed with head lice, check your child for lice, even if they don’t show symptoms (itching, a rash). Don’t rely on the school nurse to identify it; research shows school lice screenings don’t do much to stop the spread.
If a child at your kid’s school has head lice, encourage your kid to:
- Avoid sharing headphones, earbuds, headbands and hats
- Avoid hair-to-hair contact with other kids during play and sports
- Store their jacket and other belongings in their cubby or locker
Kids with head lice can and should attend school while they’re being treated. (Head lice are more of a nuisance than a health risk.) A child with lice who’s undergoing lice treatment is less likely to transfer them than one who isn’t.
Lice can’t be prevented by preemptively using lice shampoo, washing the hair more often (head lice will dine on a dirty or clean scalp) or cutting the hair short.
Preventing the spread at home
If you have one child with head lice and you want to contain the spread while you treat it, submerge their comb and hair brush in hot water (130°F) for 10 minutes, and make sure those items don’t get shared. Wash bedding, clothing and towels in hot water, and vacuum rugs and couches.
If the child has worn or touched any dry-clean-only clothing or items such as stuffed animals with glued-in eyes or plastic parts that can’t be washed in hot water, store them in plastic bags or airtight containers for two weeks.
Siblings should not hug, share a bed or share blanket forts until the infected child is lice free. Pets don’t contract head lice, so pet snuggles are fine.
How to identify head lice
Not sure if your child has lice? Do a spot check, starting at head lice’s favorite spots: around the ears and at the nape of the neck. Wet the hair (the water slows lice down) and use a fine-tooth comb to search from root to tip.
Adult head lice are the size of sesame seeds. They have six legs and are light brown or tan. Immature head lice, called nymphs, are smaller and grey or tan. Both stay close to the scalp. Head lice are nocturnal, so you might notice your child swatting or scratching in their sleep. You might also see small red bumps, caused by an allergic reaction to lice. Scratching them can introduce bacteria and lead to infection. Identifying and treating head lice early is the best defense.
Nits (lice eggs) are the size of a pinhead and can be tan, yellow or brown. You may need a magnifying glass and flashlight to see them. Misdiagnosis of nits is somewhat common. Seborrheic dermatitis and dandruff can look like nits, but the flakes are easily brushed out of the hair, whereas nits stick to the hair shaft.
Keep your cool and carry on
If a child in your kid’s circle has head lice, don’t panic. While head-to-head transmission is common, the risk of transmission from shared objects (combs, towels, scarves, hats) and spaces (a couch, bunk beds) is fairly small. Even if your child falls victim, a case of head lice is not the end of the world. Parental stress is often a major side effect, but it doesn’t have to be. Head lice are basically harmless, and with proper treatment, they will be gone before you know it.
Written by Kate Sullivan, a health and skin care writer and editor in New York City. Her work has been featured in Women’s Health, Allure and Redbook, among other publications.
The Best Facial Cleanser for Your Skin Type
The right facial cleanser can provide benefits plain old soap and water can’t touch. Not only do facial cleaners lift off makeup and remove airborne pollutants, sebum and bacteria, but today’s products also help skin look its best by way of ingredients designed to calm inflammation, boost moisture retention, clear clogged pores and more.
The trick is choosing the right facial cleanser for your skin type. “Yes, it does make a difference,” said Kimberly Van Keuren, director of cosmetic services at Water’s Edge Dermatology.
Here are Van Keuren’s ingredient recommendations for six different skin types, along with specific product picks.
Skin type: Oily/Acne-prone
The goal: Prevent sebum and skin cells from building up in pores and causing breakouts.
The ingredients: “Look for cleansers formulated with salicylic acid, glycolic acid or retinol to clean and clear pores, exfoliate dead skin cells, regulate oil production and remove dirt and grime without stripping the skin of its natural oils, which can cause oil production to go into overdrive,” said Van Keuren. Another ingredient, benzoyl peroxide, suppresses the development of bacteria and inhibits blemishes. Van Keuren finds it works well for skin that is highly acne-prone.
The product: wederm Exfoliating Gentle Cleanser
Skin type: Sensitive
The goal: Calm the skin, retain moisture and avoid an unwanted reaction to an ingredient in the cleanser. “A gentle cleanser that is pH balanced to remove oil and makeup without drying skin and is enriched with calming, soothing antioxidants is the perfect choice for sensitive skin,” said Van Keuren.
The ingredients: Seek out products with plant-derived antioxidants such as green tea polyphenols, emblica and bisabolol, advised Van Keuren. Yucca root and panthenol help sensitive skin retain moisture, she added.
The product: EltaMD Foaming Facial Cleanser
Skin type: Dry
The goal: Help skin retain moisture to make up for a lack of natural oil.
The ingredients: “Look for creamier cleansers with hyaluronic acid, lipids, ceramides, squalene or glycerin,” advised Van Keuren. “As they clean, they also hydrate and nourish skin as well as restore the skin barrier.”
The product: ZO Skin Health Hydrating Cleanser
Skin Type: Combination
The goal: Cleanse the skin without stripping moisture from dry areas, which can lead to irritation, or over-stripping an oily T-zone (the forehead, nose and chin). “Over-stripping can increase oil production,” said Van Keuren.
The ingredients: “Specially formulated cleansers for combination skin contain a low percentage of salicylic or glycolic acid,” said Van Keuren. These ingredients help brighten skin, unclog pores and keep breakouts at bay. Avoid harsh ingredients such as benzoyl peroxide, which can be too drying for combination skin.
The product: wederm Exfoliating Gentle Cleanser
Skin type: Rosacea-prone
The goal: Address any pus-filled bumps and avoid irritating rosacea-prone skin and stripping away moisture.
The ingredients: Choose gentle cleansers that contain salicylic acid. Salicylic acid treats pus-filled bumps by loosening clogged pores. Other beneficial ingredients include tea tree oil and plant extracts that help calm inflamed skin. Moisturizing ingredients such as humectants and emollients can also help.
The product: EltaMD Foaming Facial Cleanser
Skin Type: Aging/Sun Damage
The goal: Restore skin to a younger-looking state. “As we age, our pores enlarge and our oil production can either go into overdrive or stop,” said Van Keuren. In addition, “chances are there are some spots you would like to remove or brighten.”
The ingredients: Antioxidants combat free radicals that contribute to skin aging, and glycolic acid gently exfoliates the skin, making it smoother, brighter and more even-toned.
The product: wederm Moisturizing Glycolic Cleanser
Written by Jennifer L. Cook, an award-winning editor and writer whose work has appeared in Good Housekeeping, Prevention, Consumer Reports on Health, and Woman’s Day and on Investopedia.com and Bottomlineinc.com.
The Best Pillowcase for Acne
Medical review by Sydney VanHoose, APRN
Looking for a simple way to pamper your face and make your acne easier to control? Look beyond your medicine cabinet — to your linen closet.
“Your pillowcase does matter,” said Sydney VanHoose, APRN, a board-certified nurse practitioner at Water’s Edge Dermatology who specializes in medical and surgical dermatology. Some pillowcases hinder acne treatment, while others help.
To help you choose the best pillowcase for acne, VanHoose offered this advice.
Kiss cotton goodbye
Cotton is perfect for absorbing water from your skin after your shower or bath, but that same absorbent quality makes it less than ideal for your pillowcase. If your skin is oily, the pillowcase soaks up the oil — and then you sleep on that oil night after night. Along with oil, a cotton pillowcase retains bacteria, dirt and allergens.
“A cotton pillowcase can irritate acne-prone skin unless you’re washing or changing the pillowcase every couple of days,” said VanHoose. It can exacerbate existing acne and even make new acne outbreaks more likely.
Cotton and other absorbent materials, including polyester, microfiber and hemp, also rob your face of the moisturizer or serum you apply at bedtime.
If not these fabrics, then what? “Satin, silk and bamboo are better for acne-prone skin because they’re less absorbent and do not draw oil away from the face,” said VanHoose.
Think smooth
Silk and satin offer another skin-saving plus: Because they’re smooth, they don’t irritate acne lesions as rougher materials can.
“Acne lesions are inflammatory in nature to begin with,” said VanHoose. “Irritation from rough fabrics can further inflame acne lesions and exacerbate breakouts.”
Smooth fabrics also don’t crease or wrinkle the skin, unlike cotton fibers, noted VanHoose. They’re also gentler on the hair because there’s less friction. You may see smoother hair after a night on a silk or satin pillowcase.
Silk versus satin: Which is superior?
While both of these soft, slippery fabrics are smart choices, one comes out on top. “Silk is my go-to for my patients with acne or acne-prone skin,” said VanHoose. “Silk is superior because it is made from 100 percent pure, natural fiber. It’s smooth and breathable and it doesn’t harbor bacteria.”
Satin may be more affordable than silk — and unlike silk, it’s typically machine-washable — but today’s satin is usually made from a blend of fibers, such as silk, polyester, rayon and nylon. “Synthetic satin feels soft and supple like silk but it’s not ideal for skin because it’s more absorbent,” said VanHoose.
Bamboo: You get what you pay for
High-end bamboo pillowcases are soft and smooth and don’t absorb moisture, but like pure silk, they can be pricey. The less-expensive bamboo pillowcases tend to be more absorbent.
Silver doesn’t beat silk
Some anti-acne pillowcases feature silver-coated threads woven into the fabric. Silver has well-established anti-bacterial activity, which could make these pillowcases better than plain cotton for acne-prone skin, but more research is needed. “There’s not enough data to say that silver is better than silk,” said VanHoose.
Tips to care for your pillowcase — and your face
No matter which pillowcase you choose, follow these tips to keep your pillowcase clean and your skin as clear as possible.
- Wash your pillowcase often. VanHoose advises washing or changing cotton pillowcases every two or three days and silk pillowcases every week. (Because silk doesn’t absorb dirt and oil, it can go longer between washings.) Launder silk pillowcases according to the instructions on the tag; they need to be hand washed or dry-cleaned.
- Consider a bacteria-fighting spray. Try misting your pillowcase with a spray containing tea tree oil, lavender or another natural antibacterial agent each day. Tea tree oil also has anti-inflammatory powers to help calm the skin. According to VanHoose, these sprays can even extend the life of your pillowcase.
- Wash your face at bedtime. Use a gentle, noncomedogenic cleanser (one that won’t block pores) before hitting the hay. VanHoose recommends a CeraVe cleanser or EltaMD Foaming Facial Cleanser.
- Moisturize at night. After you wash your face, apply a good moisturizer and/or a moisturizing hyaluronic acid or retinol serum, even if your skin is oily. “Acne treatment and/or retinol serums can be drying or irritating to the skin,” said VanHoose. “Applying the right moisturizer can prevent your skin from becoming dry and irritated. Silk pillowcases aid in hydration.” She recommends CeraVe Moisturizing Cream, CeraVe PM Facial Moisturizing Lotion or wederm Ultra Lite Facial Moisturizer.
Written by Cheryl Sacra-Paden, a New Jersey-based editor and writer specializing in health and well-being.
Breast Cancer Skin Changes to Watch For
Medical review by Ted Schiff, MD
Imagine you notice one of your breasts has become red and feels warm to the touch. Or the skin looks different — say, pebbly, like an orange peel. You do the smart thing and make an appointment with a dermatologist, expecting to go home with a prescription for a skin cream. But it’s possible you might instead get a referral to an oncologist.
A breast lump is the classic sign of breast cancer, but it’s not the only sign. In rare cases, breast cancer can cause skin changes that offer early clues to the disease, according to dermatologist and dermatopathologist Ted Schiff, MD, founder and chief medical officer of Water’s Edge Dermatology. It’s much more likely that another, less-serious condition is the cause, but the following signs and symptoms could potentially indicate breast cancer and merit a trip to the doctor.
- A reddish rash. A reddish or purplish patch on the breast, either flat or slightly raised, could be a symptom of inflammatory breast cancer (IBC). This form of breast cancer, which is typically aggressive, occurs when cancer cells clog lymph vessels in the skin. IBC is quite rare, making up just 1% to 5% of all breast cancers. The breast may also be swollen and the skin may feel warm. But don’t panic if you develop these symptoms. “Most of these cases are not breast cancer,” said Dr. Schiff. Other possible causes of a red rash on the breast include a fungal infection, psoriasis, eczema and contact dermatitis.
- Dimpling. IBC can change the skin’s texture from smooth to dimpled, like an orange peel (the symptom is sometimes called peau d’orange, French for “skin of an orange”). In addition to the pebbly appearance and feel, the skin may become firm. Other possible causes of peau d’orange include cellulitis, a bacterial infection.
- Inverted nipple. If one of your nipples begins to pull inward, don’t ignore it. “A nipple that inverts can be an early sign of breast cancer,” said Dr. Schiff. Inverted nipples might be accompanied by other skin changes linked to breast cancer, such as skin dimpling. However, certain infections and other conditions can make a nipple turn inward, too. And some people are born with inverted nipples.
- Red, scaly nipple and areola. Paget’s disease of the breast is another rare form of breast cancer. “This type of breast cancer starts in a nipple,” said Dr. Schiff. The nipple may look red and/or scaly and may itch. The symptoms may spread to the areola, the ring of colored flesh around the nipple.
Dr. Schiff stressed that the majority of patients he sees with breast skin changes do not have breast cancer. Most have a condition that responds well to common treatments. For example, a rash on the breast caused by eczema usually clears up with cortisone cream. For an infection, antibiotics usually do the trick.
But go back to the doctor promptly if the treatment prescribed doesn’t seem to be working. “Symptoms that are persistent or recurrent should be evaluated,” said Dr. Schiff. The doctor may perform a skin biopsy, in which a small amount of tissue is removed and examined. Every now and then, Dr. Schiff or one of his colleagues detects breast cancer, and in those cases, the patient is referred to an oncologist for care.
Women who have a family history of breast cancer should be especially vigilant about watching for any signs and symptoms of breast cancer, including skin changes, and should talk with their gynecologist about appropriate screening, said Dr. Schiff.
Written by Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.