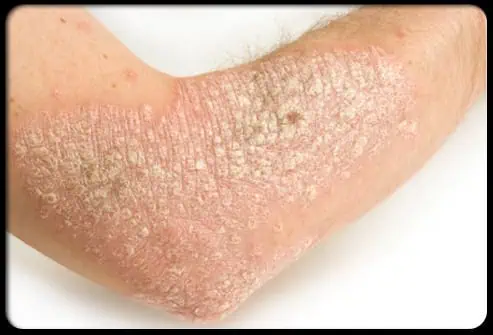
Don’t give up. You can live with Psoriasis.
As difficult as the physical symptoms of psoriasis can be, the effect on an individual has emotional and social effects that are even more challenging. Studies have shown that psoriasis can have the same impact on quality of life as congestive heart failure or diabetes. It can be demoralizing to live with skin that’s different, and embarrassing to have people stare at you – or even avoid you – as if you had something contagious.
Psoriasis is a chronic autoimmune disease that appears on the skin. It happens when skin cells quickly rise from below the surface of the skin and pile up before they have a chance to mature.
The good news is that people don’t have to let psoriasis affect their quality of life. At Water’s Edge Dermatology, our practitioners are trained and experienced in treating psoriasis. We all have experience in treating this chronic condition. While there’s no cure yet, there’s plenty we can do together to make the psoriasis patient’s quality of life more manageable.
If you are suffering from psoriasis, it’s important to know that you’re not alone. As many as 7.5 million Americans deal with the challenges of psoriasis. With today’s treatments, you can live the life you want. Evolving treatments can improve the symptoms of psoriasis or even send them into remission. With patience and persistence, psoriasis patients can get back the life they want.
One question patients always seem to ask is “How severe is my psoriasis?” One way to measure the severity is how much of the body is covered. Mild is less than 3% of the body is covered. Moderate is 3% to 10% and Severe is more than 10%. A patch of psoriasis the size of the palm of your hand is equal to about 1% of your body surface.
Psoriasis often appears between the ages of 15 and 35, but can affect people of all ages and races, men and women equally. After treatment, it will often clear up for months, only to start again. Up to 30% of those with psoriasis also eventually develop psoriatic arthritis, which causes stiffness and swelling in and around the joints.
Putting together a successful treatment plan for the psoriasis patient depends on several factors. First, your practitioner will consider the amount of your body surface covered by the disease. But even more important is the severity of the patient’s symptoms and how they affect the quality of life.
How the patient feels about having the disease is very personal. One person may not be troubled by patches of psoriasis that can be kept covered. Someone else who has small patches on an area clearly visible may feel very embarrassed and want to try a more aggressive treatment.
Psoriasis is a non-contagious common skin condition that causes rapid skin cell reproduction resulting, in red, dry patches of thickened skin.
Guttate Psoriais looks like small salmon-pink drops on the skin.
At Water’s Edge Dermatology, our practitioners work with patients to determine what the patient wants from treatment, how long the patient has had the disease and what treatments have already been tried. This information is factored into the patient’s lifestyle, overall health and severity of symptoms. The most important factor in treatment is to follow the treatment plan that is developed exactly.
Treatment is dependant on the severity of the disease. Topical drugs may be used in mild to moderate cases of psoriasis. These topical drugs may be medicated lotions, ointments, creams, gels or shampoos. Most require a prescription.
Phototherapy uses ultraviolet light to treat moderate to severe psoriasis. There are three types of phototherapy. Ultraviolet B (UVB) – The patient’s skin is exposed to UVB rays generated from a special lamp or laser. The exposure causes reactions in skin cells that decrease their overproduction and help clear up plaques. Psoralen and Ultraviolet A (PUVA) – The patient ingests, applies topically or bathes in a drug called psoralen, then undergoes UVA exposure. The combination of the drug and the ultraviolet light slows skin cell growth. Excimer laser – A controlled beam of UVB light targets only affected areas, reducing inflammation and fast-growing skin cells. This treatment is appropriate for patients with very localized, mild disease. Body-wide medications – Moderate or severe psoriasis that has resisted other types of treatment may be treated with medications that treat your entire system. These medications may be taken orally, injected or infused by IV. They include Acitretin, Cyclosporine, Methotrexate, Alefacept, Adalimumab, Etanercept, Golimumab, Infliximab and Ustekinumab.
Psoriasis of the scalp may have fine, dry, scaly skin or have heavily crusted plaque areas. Psoriasis may only involve the nails.
Alternative approaches include sun and water therapy – short exposure to daily sunlight and the addition of water-ocean, hot springs or hot tub-helps soften plaques. Meditation can encourage an improved immune system response. Yoga teaches meditation and controlled breathing, which reduce stress (a common trigger). Nonprescription topical treatments, including aloe vera, evening primrose oil and capscaicin have all proven effective in clinical trials.
Medical treatment will go a long way toward helping the psoriasis patient control the disease. Making lifestyle changes can also be helpful in easing skin discomfort and minimizing periodic flare-ups. Adequate sleep, eating a balanced diet, regular physical exercise and drinking plenty of water will keep stress levels down and the body in top condition to fight off infection.
Diseases of the skin, like psoriasis, are reasons why everyone should have an annual skin examination by a dermatologist. At Water’s Edge Dermatology, our practitioners are highly experienced in psoriasis and all diseases of the skin. If you have any questions about psoriasis or other questions relating to skin care, Email them to me below. And if you haven’t had a skin examination in the past year, call one of our convenient locations for an appointment.
What Every Floridian Must Know About Skin Cancer
If you're like most Floridians, you've taken advantage of our summer and spent a good deal of time outdoors playing golf, tennis, boating, fishing, or just walking our magnificent beaches. In Florida, we are fortunate to enjoy these activities year-round. However, all of that exposure to the sun is something of which to be mindful. Skin cancer in Florida is more common because of the intensity of the sun.
According to the American Cancer Society, more than a million Americans will be diagnosed with skin cancer this year. In my dermatology practice, I have noted the increased number of patients that we are seeing with skin cancer. That’s not surprising when you understand the risk factors for skin cancer.
Exposure to UV radiation that comes from the sun, sun lamps, tanning beds or tanning booths is a primary risk factor. A person’s risk of skin cancer is related to lifetime exposure to UV radiation. Most skin cancer appears after age 50, but the sun damages the skin from an early age. UV radiation affects everyone. That’s why an annual skin exam is so important.
The two most common types of skin cancer are basal cell cancer and squamous cell cancer. They usually form on the head, face, neck, hands and arms. But skin cancer can occur anywhere. Basal cell skin cancer grows slowly. Squamous cell skin cancer sometimes spreads to lymph nodes and organs inside the body. The third form of skin cancer, Melanoma, is generally the most serious form of skin cancer because it tends to spread (metastasize) throughout the body quickly.
The most common warning sign of skin cancer is a change in the appearance of the skin, such as a new growth or a sore that will not heal. Unexplained changes in the appearance of the skin lasting longer than two weeks should be evaluated by an experienced dermatologist. According to the National Cancer Institute, the cure rate for basal cell and squamous cell cancers could be 100% if they were brought to a dermatologist’s attention before they had a chance to spread. Because cumulative sun exposure is a primary risk factor, it’s very important for all of us to have an annual skin cancer exam. In that manner, we can compare changes in the patient’s skin, from year-to-year.
Checking your skin for new growths or changes is a good idea. You should report any changes to your dermatologist right away.
Often, the first sign of melanoma is a change in the size, shape color or feel of an existing mole. Melanoma may also appear as a new mole. It may be black, or "ugly looking."
Don’t use photos to try to diagnose your own skin cancer. They can’t take the place of a dermatologist's examination.
If you haven’t made an appointment for your summer-ending skin cancer exam, now is the time. Skin cancer is the most common form of cancer. The earlier it is diagnosed, the better the chance for cure.