Summer Skin Care
Summer is here. This means barbecues, the beach and other outdoor fun. However, rising temperatures, a poor diet and sunscreen can irritate pores and cause oilier skin. Water’s Edge’s team of acne dermatologists answer questions and provide advice on the best summer skin care for acne prevention.
Is diet important for clear skin?
It is not proven that ingesting fried or greasy foods causes acne, according to our acne dermatologists, but oils remaining on the skin can clog the pores. Certain foods may trigger breakouts and should be avoided to prevent flare-ups. A healthy diet and plenty of hydration is recommended to enhance the well-being and look of your skin.
What is the oil on skin?
The oil produced on our skin is called sebum and its purpose is to keep the skin from drying out. However, an increase in production may cause breakouts and irritation. Prevent breakouts by minimizing the oil and bacteria on the skin. A regimen can be as simple as washing the face with soap and water. Antibacterial soap like Dial or Cetaphil will reduce the bacteria. Wash immediately after sports and workouts. If oil persists, a toner or benzoyl peroxide product may need to be added.
What kind of skin products should I use?
Clogged pores may need a retinoid. Retinoids, like Retin A Micro, speed up the skin-cell turnover time by putting a light peel on the skin, which prevents pores from clogging. Be careful to choose makeup, moisturizers and sunscreens that don’t clog pores. Check the labels and look for wording like non-comedogenic, non-greasy or oil-free. Products like Cerave and Cetaphil are just two available options. EltaMD and Minus Sol are sunscreens available in our office. A facial is recommended by our cosmetic dermatologists and estheticians, and this service is available in many of our offices.
Look your best all year!
Good skin care is recommended all year. Our desire at the Florida center for dermatology is to help you look great, but protecting your skin from damage and harmful rays is most important. Always moisturize your skin, keep it well hydrated and use protective clothing and sunblock. The skin is our first line of defense and should be protected every day.
Sunscreen is Beauty’s New Best Friend
We all know sunscreen is an important step in protecting yourself from skin cancer and those painful sunburns. But did you know there is a new reason to slather it on? Water’s Edge Dermatology wants to encourage you to take a couple minutes to reapply sunscreen and make your skin look younger. The National Health and Medical Research Council of Australia funded a study to look for the truth in sunscreen use and dietary supplements such as beta-carotene. After reading their findings, you’ll be searching for that sunscreen bottle.
The researchers down under found more than 900 people under the age of 55 to either slather on sunscreen as per instructions or to keep up their usual routine. They were also given either a beta-carotene supplement or a placebo to test out the effects of dietary supplements meant to prevent skin damage and aging.
After four years of keeping track of all these people’s sunscreen regimen, researchers found that regular sunscreen use does slow the aging of skin while the beta-carotene supplement had no overall effect. The people who reapplied sunscreen on the hour and after getting wet were 24% less likely to show increased aging.
The main reason is the ability of UV-A rays to break down the collagen and elasticity of skin. Collagen isn’t only used to make your lips pouty, it holds your skin together and keeps it looking young. When collagen can’t do its job because of all the UV-A exposure, your skin begins to lose the battle for elasticity and a youthful experience.
So, even if it takes a couple minutes out of your day here or there, try to reapply whenever you can. Water’s Edge even sells non-oily sunscreen. Not only will it help prevent skin cancer, it’ll keep you looking pretty for longer.
The Long and Short of UV rays
Coolers, beach chairs, umbrellas and sunscreen — lots of sunscreen — are popping up in endless colorful displays throughout stores nationwide! This could only mean one thing, summer is on the horizon!
Picking out a sunscreen to protect yourself and your family can be a bit confusing. What brand do I want? What SPF do I need? What does UVA and UVB protectants even mean?
Let's start with the basics.
Ultraviolet UV rays are emitted from the sun in three lengths. UVA are the long rays, UVB are the short rays and UVC are absorbed in the ozone layer before they even make it to earth. Over the years research has shown that both UVA and UVB can cause damage to the skin. These rays are proven human carcinogens which means they can cause genetic mutations in the skin leading to skin cancers.
UVA rays are the long rays which can penetrate their way deeper into the skin and are responsible for skin aging and wrinkling. They are present during all daylight hours and remain even throughout the year. The tilt of the earth during various seasons does not change the level of UVA rays found in sunlight. These UVA rays can penetrate clouds and even glass when you are indoors or in your car. As you can see, the recommendation of daily sunscreen as part of a good skin care regimen is important.
UVA rays are responsible for damaging the keratinocytes which are found in the basal layer of the epidermis. Basal cells and squamous cells are both types of keratinocytes. Damage to these cells can lead to both basal cell carcinoma and/or squamous cell carcinoma which are the first and second most common forms of skin cancer.
UVB are the short rays which penetrate and damage the more superficial layers of the skin known as the epidermal layers. These short rays are responsible for burning and reddening of the skin. The intensity of the UVB rays varies with season, location and time of day. UVB rays are most intense between the hours of 10 a.m. and 4 p.m. from April through October. Avoidance of the sun during these peak hours is an effective way to prevent skin damage. Although, at higher altitudes and with reflection on ice or snow, UVB rays can cause damage throughout the year. In contrast to UVA, UVB do not significantly pass through glass.
Protection is key!
Now that we know both UVA and UVB rays can cause long-lasting skin damage, what do we do? Protecting yourself and your family is your primary prevention. Hats, sunglasses, sunscreen and sun protective clothing are key. When choosing a sunscreen, read carefully and select a product with "broad-spectrum" coverage for both UVA/UVB protection and an SPF of 30 or higher!
Reference: www.skincancer.org, 2013 The Skin Cancer Foundation | 149 Madison Avenue Suite 901 New York, New York
Skin Cancer Screenings for Skin Cancer Month
According to the American Cancer Society, skin cancer accounts for nearly half of all cancers in the United States, with one in five people having some form of skin cancer. Melanoma, the most serious type of skin cancer, will account for more than 76,600 cases of skin cancer in 2013, resulting in roughly 9,000 deaths annually.
“It’s so unfortunate when a patient waits too long to be screened and melanoma is found way too late, as it’s very treatable if found early,” says Justin Platzer, M.D., a board-certified dermatologist and Mohs skin cancer surgeon at Water’s Edge Dermatology.
Darlene Moore of West Palm Beach, Fla., echoes Dr. Platzer’s sentiment of the importance of diagnosing melanoma early. During a regular skin cancer screening at Water’s Edge Dermatology, Shanna Stone, ARNP, saw a few areas of concern on Ms. Moore’s ear and arm and took biopsies. Ms. Moore was diagnosed with Stage 1 melanoma on her arm and basal cell carcinoma on her ear.
“The basal cell, frankly, I wasn’t as concerned about,” says Ms. Moore. “Dr. Platzer reassured me that Mohs surgery was very effective for basal cell carcinoma and he was able to get it all. But I was really concerned about melanoma, because my brother-in-law died of melanoma.”
Surgery is the best way to remove early melanomas, with later stages usually requiring more extensive treatment, such as radiation and chemotherapy. Mohs surgery saves the greatest amount of healthy tissue, appears to reduce the rate of local recurrence and has the highest overall cure rate — about 94 percent to 99 percent — of any treatment for squamous cell carcinoma. And generally, Mohs surgery is 98 percent or better for basal cell carcinoma, according to the Skin Cancer Foundation.
“As the old saying goes, ‘An ounce of prevention is worth a pound of cure,’” says Dr. Platzer. “Say no to tanning beds and always wear sunscreen. And, if you live in sunny Florida, it is critical to have regular skin cancer screenings — and there’s no better time than this month, Skin Cancer Month.”
Many Water’s Edge Dermatology clinics are open Saturdays and late during the workweek. To make an appointment, visit wederm.com and fill out the online appointment form, email info@WeDerm.com or call (561) 694-9493 for more information.
Skin Cancer Prevention Tips for Skin Cancer Awareness Month
May is Skin Cancer Awareness Month, and Water’s Edge Dermatology recommends the following skin cancer prevention tips to have fun in the sun and reduce risk for skin cancer at the same time:
- Generously and regularly apply water-resistant sunscreen that has a sun protection factor (SPF) of 30 or more. Make sure the sunscreen is labeled as “broad-spectrum,” indicating it protects against ultraviolet A (UVA) and ultraviolet B (UVB) rays. Reapply sunscreen every two hours and after swimming or sweating — and use it year-round.
- Use extra caution when taking sun-sensitizing medications or near water, snow and sand. Some over-the-counter medications, such as ibuprofen, and prescription drugs, such as antibiotics, can make your skin more sensitive to sunlight. Water, snow and sand can reflect and/or intensify sun rays, making it easier to burn.
- Wear protective clothing, including long-sleeved shirts and pants, a wide-brimmed hat that provides more coverage than a baseball hat and UVA/UVB protective sunglasses.
- Seek shade during the middle of the day, between 10 a.m. and 4 p.m., when the sun’s rays are strongest, and try to schedule outdoor activities for other times of the day — even when it is cloudy.
- Say no to tanning beds. Ultraviolet light from tanning beds can cause skin cancer. New self-tanning lotions and spray booths provide a tan without the risk of cancer.
- Check your entire body routinely and report skin changes to your dermatologist. New growths, changes in existing moles or bleeding on the skin require an immediate appointment with a dermatologist. Skin cancer is very treatable when caught early.
“As the old saying goes, ‘An ounce of prevention is worth a pound of cure,’” says Dr. Platzer. “Say no to tanning beds and always wear sunscreen. And, if you live in sunny Florida, it is critical to have regular skin cancer screenings — and there’s no better time than in May, Skin Cancer Awareness Month.”
Who’s at Risk of Developing Shingles?
Shingles, also known as herpes zoster, is a viral disease that manifests as a painful skin rash with blisters. It develops when the chicken pox virus reactivates in the body, often for unknown reasons.
Anyone who has had chicken pox is at risk for developing shingles. About 20 percent of those who have had chicken pox will get shingles — most develop shingles only once.
It is not clear what reactivates or "awakens" the virus. However the following are thought to cause outbreaks:
- Compromised immunity
- Old age
- Illness
- Trauma
- Stress
Shingles can also be contagious. Though not as contagious as chicken pox, shingles can be transmitted through direct skin contact if blisters break. Because of this, people with shingles should not interact with pregnant women, small children or the immunocompromised.
Shingles typically causes more pain and less itching than chicken pox. A person may feel burning, itching, tingling or extreme sensitivity on the skin. These usually last for one to three days, sometimes more, before a red rash appears in the same area. A shingles rash usually occurs on only one side of the body.
To diagnose shingles, a dermatologist looks at the appearance of the skin and asks how the rash developed. To confirm the diagnosis, a dermatologist may scrape skin cells from a blister for examination under a microscope. Also, the blister fluid containing the virus can be sent to a laboratory for special testing.
Shingles usually clears on its own in a few weeks and seldom recurs. A dermatologist may prescribe an oral medication to help. While shingles is clearing, pain relievers can help ease the discomfort, and cool compresses may provide soothing relief.
The most common problem of shingles is postherpetic neuralgia, which is pain, numbness, itching and tingling that last long after the rash clears. Oral pain medications can help relieve the pain.
A shingles vaccine has been approved by the U.S. Food and Drug Administration (FDA) for people ages 60 and older who have never had shingles. In one study, this immunization decreased the incidence of shingles by more than 50 percent.
If you or someone you know may be at risk for singles, schedule an appointment with a Water’s Edge Dermatology practitioner.
Treatment Options for Eczema
If you or someone you know has eczema, you know it can be itchy, irritating and hard to manage. It often can feel like no matter what you do to get rid of it, the rash stays or keeps coming back.
Eczema often starts at a young age, with 10-20 percent of children diagnosed with the condition. While it can be lifelong, eczema tends to become less severe with age.
Unfortunately, there are not effective, easy, over-the-counter treatments for eczema. There are, however, tools dermatologists can use to appropriately diagnose and treat eczema.
Medical research continues to show that the most effective treatment plan involves treating the skin and making lifestyle changes.
Eczema Treatment Options
Your Water’s Edge Dermatology practitioner may recommend any number of combinations of the following options to manage your eczema:
- Corticosteroid or an immune-modifying medication, which can help reduce the inflammation and itch
- An antihistamine can improve eczema that’s triggered by allergies
- Antibiotics if there’s an infection, which is common
- Ultraviolet (UV) light therapy
Lifestyle Changes for Eczema
Talk to your Water’s Edge Dermatology practitioner before you implement any of these lifestyle changes:
- Frequently applying an appropriate moisturizer
- Avoiding certain clothing
- Using eczema-friendly bathing techniques
If you think you or a loved one has eczema, schedule an appointment to have your condition properly diagnosed and to begin the path toward relief.
When to See a Dermatologist for a Mole
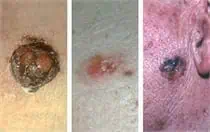
Skin moles are common. Almost everyone has a few, and some people develop hundreds. And melanoma, the deadliest type of skin cancer, can develop in or near moles.
Don’t get frightened — most skin moles are not melanoma. So how do you know when to see a dermatologist for your moles? It’s easy; just keep in mind your ABCs.
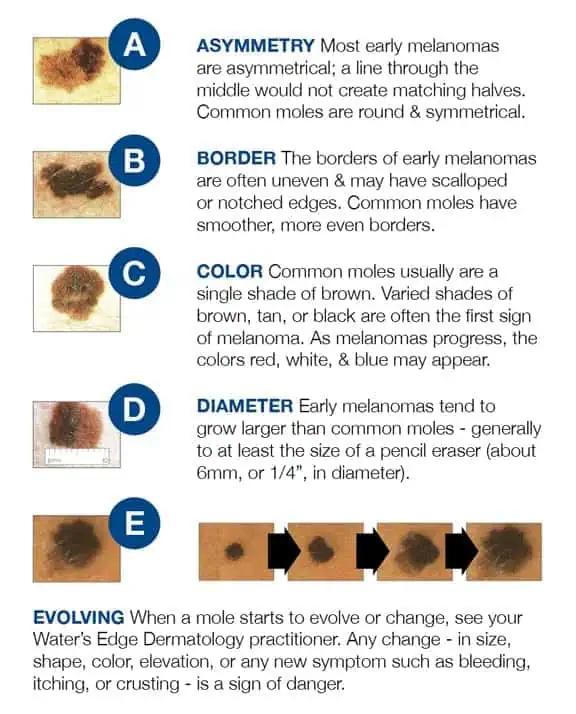
A stands for ASYMMETRY: If one half of the mole is unlike the other half, have it looked at.
B stands for BORDER: If your mole has an irregular, scalloped or poorly defined border, it could be an early melanoma. Only a biopsy can provide conclusive results.
C stands for COLOR: If a mole’s color varies from one area to another, or if it turns shades of tan, brown and black (opposed to brown, which is normal), call your dermatologist.
D stands for DIAMETER: Melanomas are usually greater than 6mm (the size of a pencil eraser) when diagnosed, but they can be smaller. If a mole is large, have it examined and stay very aware of changes or growth.
E stands for EVOLVING: A mole or skin lesion that looks different from the rest or is changing in size, shape or color could be a sign of early skin cancer.
If you have a mole that shows any of these signs, be sure to schedule an appointment with a Water’s Edge Dermatology provider today. If something doesn’t seem right, or keeps grabbing your attention, come see us.
When it Comes to Staph Infections, Prevention is the Key
Different varieties of Staphylococcus aureus bacteria, commonly called "staph," exist. “Staph infections” are common and a term I remember hearing since I was a child, so this is not something new. Staph bacteria are normally found on the skin and in the nose of about one-third of the population. The bacteria are generally harmless unless they enter the body through a cut or other wound, and even then they usually cause only minor skin problems in healthy people. However, Methicillin-Resistant Staphylococcus Aureus (MRSA) is different. MRSA infections are caused by a strain of staph bacteria that's become resistant to the antibiotics commonly used to treat ordinary staph infections.
Most MRSA infections occur in people with questionable immune function who have been in hospitals or other healthcare settings, such as nursing homes and dialysis centers. When it occurs in these settings, it's known as healthcare-associated MRSA (HA-MRSA). HA-MRSA infections typically are associated with invasive procedures or devices, such as surgeries, intravenous tubing or artificial joints.
Another type of MRSA infection occurs in the wider community — among healthy people. This form, community-associated MRSA (CA-MRSA), often begins as a painful skin boil. It's spread by skin-to-skin contact. At-risk populations include groups such as high school wrestlers, child care workers and people who live in crowded conditions.
Staph skin infections, including MRSA, generally start as small red bumps that resemble pimples or boils. It is not uncommon for the patient to suspect a spider bite. These can quickly turn into deep, painful abscesses that require surgical draining. In most situations, the bacteria remain confined to the skin. But in the case of the HA-MRSA, they can also burrow deep into the body, causing potentially life-threatening infections in bones, joints, surgical wounds, the bloodstream, heart valves and lungs.
Antibiotic Resistance
MRSA is the result of decades of unnecessary antibiotic use. For years, antibiotics have been prescribed for colds, flu and other viral infections that don't respond to these drugs. Even when antibiotics are used appropriately, they contribute to the rise of drug-resistant bacteria in part because they don't destroy every germ they target. In addition, patients who do not take their entire course of antibiotics also play a role in the emergence of these resistant strains. Bacteria live on an evolutionary fast track, so germs that survive treatment with one antibiotic soon learn to resist others.
Because hospital and community strains of MRSA generally occur in different settings, the risk factors for the two strains differ.
Risk Factors for HA-MRSA
- Being hospitalized. MRSA remains a concern in hospitals, where it can attack those most vulnerable — older adults and people with weakened immune systems.
- Having an invasive medical device. Medical tubing — such as intravenous lines or urinary catheters — can provide a pathway for MRSA to travel into your body.
- Residing in a long-term care facility. MRSA is prevalent in nursing homes. Carriers of MRSA have the ability to spread it, even if they're not sick themselves.
Risk Factors for CA-MRSA
- Participating in contact sports. MRSA can spread easily through cuts and abrasions and skin-to-skin contact.
- Living in crowded or unsanitary conditions. Outbreaks of MRSA have occurred in military training camps, child care centers and jails.
- Men having sex with men have a higher risk of developing MRSA infections.
When to See a Healthcare Professional
Keep an eye on minor skin problems — pimples, insect bites, cuts and scrapes — especially in children. If wounds become infected, seek medical care. Do not attempt to treat an MRSA infection yourself. You could worsen it or spread it to others.
What You Can Do
Create a list that includes:
- Detailed descriptions of your symptoms
- Information about medical problems you've had
- Information about the medical problems of your parents or siblings
- All the medications and dietary supplements you take
- Questions you want to ask the doctor
What to Expect During Your Visit
During your physical exam, your doctor will closely examine any skin lesions you may have. He or she might take a sample of tissue or liquid from the lesions for testing.
Both healthcare-associated and community-associated strains of MRSA still respond to certain antibiotics. In some cases, antibiotics may not be necessary. For example, your doctor, NP or PA may choose to drain a superficial abscess caused by MRSA rather than treat the infection with drugs.
Preventing HA-MRSA
In the hospital, people who are infected or colonized with MRSA often are placed in isolation as a precaution to prevent the spread of MRSA. Visitors and healthcare workers caring for people in isolation may be required to wear protective garments and must follow strict hand hygiene procedures. Contaminated surfaces and laundry items should be properly disinfected.
Preventing CA-MRSA
Wash your hands. Careful hand-washing remains your best defense against germs. Scrub hands briskly for at least 15 seconds, then dry them with a disposable towel and use another towel to turn off the faucet. Carry a small bottle of hand sanitizer for times when you don't have access to soap and water.
Keep wounds covered. Keep cuts and abrasions clean and covered with sterile, dry bandages until they heal. The pus from infected sores may contain MRSA, and keeping wounds covered will help keep the bacteria from spreading.
Keep personal items personal. Avoid sharing personal items such as towels, sheets, razors, clothing and athletic equipment. MRSA spreads on contaminated objects as well as through direct contact.
Shower after athletic games or practices. Shower immediately after each game or practice. Use soap and water. Don't share towels.
Sanitize linens. If you have a cut or sore, wash towels and bed linens in a washing machine set to the hottest water setting (with added bleach, if possible) and dry them in a hot dryer. Wash gym and athletic clothes after each wearing.
Most patients have come to know and often fear the term MRSA. However, when these infections are encountered the general community, in patients who are otherwise healthy, there is little to fear. Your healthcare provider will know exactly how to manage your condition and you are sure to recover without complication. Even so, it is still good behavior to practice the sound preventive measures we discussed above.
The Skinny on Tanning Beds and Skin Cancer Risk
As dermatology providers, we have often been asked the question from our patients as to the risks of indoor versus outdoor tanning.
Well, the answers have recently become clear and are alarming! The rise in skin cancer rates happens to coincide with the growth of indoor tanning, which was first introduced in the U.S. in the 1970s. Just one single indoor tanning session can increase users’ chances of developing the most serious form of skin cancer, melanoma, by 20%. Each additional session during the same year increases the risk almost another 2%.
These figures are based on a recent exhaustive analysis of 27 studies by the International Research Institute in Lyons, France. Essentially, people who tan indoors are 74% more likely to develop melanoma in their lifetime. Those who started tanning before age 35 have an even higher risk of 87% of developing melanoma. The majority of tanning bed patrons are girls and women ages 16 to 29. They display a high level of knowledge about the risks of UV exposure, but this awareness does not alter tanning behavior.
The number of melanoma cases has tripled in the past twenty years. In 2012, melanoma has affected an estimated 76,250 people, killing 9,180 in the U.S. alone. The British Medical Journal published a study linking more than 5% of all melanomas to tanning bed use.
Heredity can play a major role in melanoma, but the disease is often be triggered by intense, intermittent sun exposure. Fair-skinned people with light hair and eye color and those who have had sunburns or tend to burn easily are at increased risk of developing melanoma. So are those who have a family history of the disease or have ever themselves had a melanoma or other skin cancer. People with unusual-colored and large-sized moles are at a higher risk. In the earliest stages, melanoma is readily treatable. Left untreated, however, it can spread to vital organs and become life-threatening. Among patients with advanced disease, just 15% survive longer than 5 years.
Further studies have shown the role of indoor tanning on nonmelanoma skin cancers. Close to 171,000 (or about 3%) of nonmelanoma skin cancers diagnosed each year in the U.S. are attributed to indoor tanning. A single UV tanning session increases squamous cell skin cancers (SCC) by 67% and basal cell skin cancer (BCC) by 29%. Additionally, indoor tanners under the age of 25 double their risk of SCC and increase their risk of BCC by 40%.
Skin cancer prevention is optimally about sun protection. Nonetheless, secondary prevention involves early detection. An annual head to toe skin exam by a dermatology provider is recommended by the Skin Cancer Foundation, with a monthly self-examination. Familiarize yourself with suspicious appearing lesions, new or changing moles, spots, sores, lesions or growths. When patients are diagnosed and treated at an early stage of skin cancer, almost all make a full recovery.
Remember to wear sunscreen, apply 1 oz (2 TBS) to your entire body 30 minutes before going outside. Reapply every 2 hours or after swimming or excessive sweating.
Unfortunately, despite recent efforts to educate the public and limit young people's access to indoor tanning facilities, sunbathing and indoor tanning have not significantly decreased. Thirty million Americans still visit indoor tanning salons, annually. Suntans and sunburns occur from overexposure to UV radiation, and both are signs of damage to skin cells. So, let’s get the word out there.
Learn more about skin cancer, or request a skin cancer screening at Water’s Edge Dermatology.
Sources
Publication of the Skin Cancer Foundation, Revised 2012
Robbins, Perry, M.D., The Numbers Add up:Just One Tanning Session Multiplies Skin Cancer Risk., Sun and Skin News, Winter 2012, Vol. 29, No.4
ReedK., BrewerJd Lohsce Cm, et al, Demierre MF, LazovichD, et al, Karagas MR, et al, Swerdlow AJ, Weinstock. Teen Tanners, The New Face of Melanoma, Skin Cancer Foundation Journal, Vol XXX, 2012, 34-37