What Is a Dermatology Physician Assistant and What Do They Do?
Medical review by Ted Schiff, MD
When you make an appointment with a dermatologist, there’s a chance you may see the provider’s dermatology physician assistant (PA) instead. If you do, you may find yourself wondering what qualifications PAs have and what kinds of services they can provide. You may have even considered becoming a PA yourself.
Below are answers to some of the most commonly asked questions about dermatology PAs.
What is a dermatology physician assistant?
Certified dermatology PAs, or PA-Cs (physician assistant-certified), are medical professionals who are licensed to practice medicine in collaboration with a dermatologist. While they don’t have a medical degree, they do have to complete a rigorous education program and attain thousands of hours of clinical experience.
Dermatology PAs can perform many of the same services a dermatologist provides, but they do so under the direction and supervision of a dermatologist. An experienced PA sees patients on their own, but they may consult with a dermatologist on more complicated cases or ask the dermatologist to take over.
What services can a dermatology PA provide?
The duties dermatology PAs are permitted to carry out depending on the setting in which they work, level of experience, and state laws. PAs may be able to:
- Take medical histories
- Perform physical exams, including skin cancer screening exams
- Diagnose and treat skin conditions, such as acne, eczema, and rosacea
- Order and interpret tests
- Perform biopsies, wide excisions, and cryotherapy
- Develop treatment plans
- Prescribe medication
- Provide information about preventive care
- Perform certain minimally and non-invasive cosmetic procedures, such as Botox injections, laser skin resurfacing, and mild or moderate chemical peels
- Assist in surgeries, such as Mohs surgery
Services that only a dermatologist can provide include deep chemical peels and invasive surgeries.
What level of education and training must a PA have?
Candidates who apply to PA programs need a bachelor’s degree, ideally in a scientific field such as biology or chemistry. They may need to take an additional year to complete prerequisite courses. Even people who have a scientific undergraduate degree may have to attend classes that weren’t required in their bachelor’s program, such as physics, ethics, and statistics.
The next step is to gain experience working with patients. PAs must have patient care experience (PCE), in which they are directly responsible for a patient’s care, or healthcare experience (HCE), in which they are indirectly responsible for a patient’s care. Most PA programs require at least 1,000 hours of PCE or HCE. They can get them through jobs such as:
- Registered nurse
- Certified nursing assistant
- Medical assistant
- Paramedic
- Emergency medical technician
- Surgical technician
- Emergency room technician
- Lab assistant/phlebotomist
- Medic or medical corpsperson
- Peace Core volunteer
PA programs typically last approximately 26 months (three academic years). Graduates must take the Physician Assistant National Certifying Exam, which is administered by the National Commission on Certification of Physician Assistants. Once they pass the exam, they can begin practicing medicine.
PAs receive a general medical and surgical education. They can choose a specialty such as dermatology once they become certified. They learn more about the specialty through on-the-job training provided by a doctor. PAs are free to change specialties throughout their career.
After a PA is certified, they must complete 100 hours of continuing medical education (CME) credits every two years and take a recertification exam every 10 years.
What training does a PA program consist of?
Students take a variety of classes, including anatomy, pharmacology, physical diagnosis, behavioral science, and medical ethics. Similar to medical students, PA students must complete clinical rotations, typically in physician offices, ambulatory clinics, and acute or long-term care facilities. Types of rotations required typically include family medicine, internal medicine, obstetrics and gynecology, and psychiatry and dermatology.
How does someone apply to a PA program?
Most candidates apply to an accredited PA program through the Centralized Application Service for Physician Assistants, which allows them to apply to multiple PA programs with one application. Candidates are expected to submit undergraduate/post-graduate transcripts, letters of recommendation, a list of PCE or HCE hours and a personal statement that explains why they want to be a PA and why they’re a good candidate for the program. An interview is required.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Radiation Therapy for Skin Cancer
Medical review by David Herold, MD, MBA
Learning you have skin cancer can be a shock. The disease is rarely fatal, but many people worry about the effects treatment could have on their appearance, particularly if they have skin cancer on the face.
Scars from skin cancer surgery can be very noticeable and even disfiguring in some cases. But radiation therapy can remove many skin cancers just as effectively as surgery, without the risk of scarring.
“Unfortunately, patients who are diagnosed with some of the most common forms of skin cancer, such as basal cell and squamous cell carcinoma, are often told they need surgery and aren’t informed that there are other options,” said David Herold, MD, MBA, a board-certified radiation oncologist at Water’s Edge Dermatology. “Many of these patients could get better cosmetic results with radiation therapy, particularly if the lesions are on their face.”
What is radiation therapy?
When you undergo radiation therapy for skin cancer, a beam of low-energy rays (such as x-rays) or particles such as electrons is aimed at the treatment area for a set period time. These rays or particles break apart the DNA in cancer cells, ultimately killing the cells. While some healthy surrounding cells may be damaged in the process, it isn’t a cause for concern.
“Healthy cells have incredible repair mechanisms, and they start healing themselves seconds after treatment,” Dr. Herold said. “Cancer cells die because they’re unable to repair themselves from the effects of radiation.”
Radiation therapy is sometimes confused with chemotherapy, but the two treatments are nothing alike. Radiation therapy is delivered externally and penetrates only as far as the skin, so there are few or no side effects. Chemotherapy is administered internally, either intravenously or orally. It affects the whole body and can lead to side effects such as nausea and hair loss.
Types of radiation therapy for skin cancer
Superficial radiation therapy (SRT) uses a beam of low-energy x-rays to destroy cancer cells. A newer, more versatile type of radiation therapy is electron beam therapy (EBT), which uses a very thin, non-penetrating electron beam.
Dr. Herold specializes in EBT. Water’s Edge Dermatology is one of the few dermatology practices in Florida that offer it.
Advantages of electron beam therapy
EBT for skin cancer offers several advantages over SRT for skin cancer.
“Electron beam therapy can treat larger skin cancer lesions on the face and head compared to SRT, such as big lesions that appear on the scalp,” said Dr. Herold. “It also treats deeper skin cancers without causing irritation or pain in the cartilage or bone beneath the lesion, which happens sometimes if you use a higher dose of SRT to treat a deeper skin cancer.”
Another major advantage of EBT is that it more effectively treats lesions on irregular skin surfaces, such as the tip of the nose or curved areas of the ear. “SRT uses a flat beam that doesn’t work as well on areas like these,” Dr. Herold said.
EBT is the better radiation therapy for basal cell carcinoma of the nose as well as squamous cell carcinoma of the nose.
Who can get electron beam therapy?
This form of radiation therapy is most often used to treat basal cell carcinoma (the most common type of skin cancer) and squamous cell carcinoma (the second most common type of skin cancer).
According to Dr. Herold, EBT is used as a stand-alone treatment in 95% of cases but is occasionally used after surgery to clear any margins (the border of the tissue removed during surgery) that contain cancer cells. The cure rate of EBT for skin cancer — 90% to 98%, depending on the location of the lesion — is equivalent to that of skin cancer surgery, he added.
EBT isn’t recommended as a standalone treatment for melanoma except in some cases of melanoma in situ (stage 0). Stage 0 means the cancer hasn’t spread beyond the outermost layer of skin. EBT can also be used to treat a rare type of cancer called cutaneous lymphoma, a group of lymphomas that start in the lymph system and affect the skin.
While EBT can treat skin cancer lesions on any area of the body, it’s most commonly used to treat skin cancer on the face to avoid serious scarring and resulting complications.
“Surgically removing lesions on the face can sometimes lead to terrible outcomes,” Dr. Herold said. “I’ve seen patients who had surgery on their nose or eyelid who are now missing the tip of their nose or who can’t close their eye completely, which wouldn’t have happened if they’d had radiation therapy.”
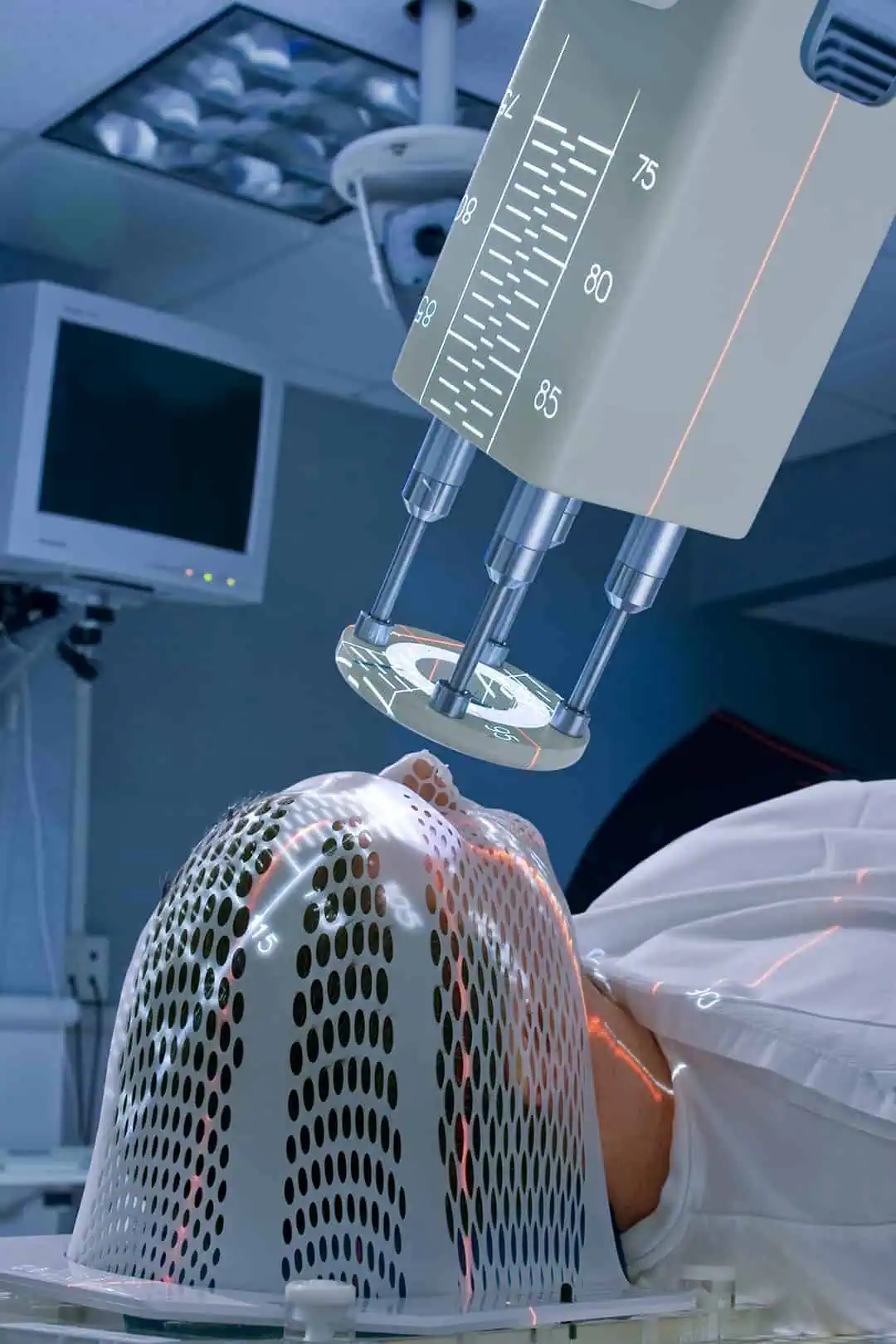
What happens during an EBT session
Undergoing EBT for skin cancer on the face is quite simple. Before your treatment sessions start, your doctor will make a mold of your face and the sides and top of your head to create a plastic mesh mask you’ll wear during each session to keep your head and neck stationary. A piece of lead in the shape of the lesion is placed on the lesion to prevent electrons from scattering to nearby healthy skin.
You’ll be instructed to lie down on a table beneath the machine that delivers the electron beam, called a linear accelerator. The beam is aimed at the lesion for about 90 seconds. All told, the appointment takes less than 5 minutes.
“EBT is painless, so there’s no need to numb the skin beforehand,” Dr. Herold explained. “Patients may experience some redness in the treated area after a session, so I advise them to apply Aquaphor or a prescription cream to help with healing.” Patients can resume their normal activities (working, swimming, exercising) immediately after treatment.
While sessions are very quick, you do have to get them five days a week for anywhere from two weeks to six weeks. How long you undergo treatment depends on several factors, such as the location of the cancer:
- Small lesion on the cheek: two weeks
- Lesion on the ear: four or six weeks, depending on the size
- Large scalp lesion: four or six weeks
- Tip of the nose: six weeks
Once you’ve completed your sessions, the treated area will heal in one to three weeks. In some cases, radiation therapy for skin cancer can lead to loss of pigment in the area, but the effect is subtle (if it occurs at all) with EBT because the doses of radiation are so low.
“Most people who receive EBT look like they never got any kind of treatment,” Dr. Herold said.
“I’m very dedicated to educating patients about the procedure because they should be able to make an informed decision about how they want to be treated, and surgery isn’t always the best choice,” he added.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
How to Get Hair Dye, Sharpie, Super Glue and Other Messes Off Skin
Medical Review By: Jenna Steffel, APRN, DNP
A slip of the Sharpie, a drip of the hair dye, a misplaced squirt of the tie-dye bottle — it happens. And then there’s the challenge of getting the ink or dye, or the glue or other substance, off your skin, or off your child’s skin.
Don’t panic. In most cases, you probably have something in the house that will remove the stain or stickiness and leave your or your little one looking like nothing ever happened.
How to get hair dye off skin
Simple soap and water may be enough to tackle hair dye if you catch it before it dries. If the stains are on your face and they aren’t budging, apply a small amount of rubbing alcohol on a cotton ball or cotton pad and dab it on the affected areas. (Don’t use rubbing alcohol near your eyes.) If you don’t have rubbing alcohol, gently rub the stains with a small amount of non-gel toothpaste. Let the toothpaste sit for 5 to 10 minutes, then wash it off with a washcloth and warm water.
People with sensitive skin may prefer to try olive oil. Pour a small amount onto a cotton ball or your fingertip, gently rub in the oil and leave it for up to 8 hours before washing with warm water.
If the hair dye has gotten on your hands, there are more options for removing it because the skin there may be able to tolerate harsher products. Try rubbing the stains with acetone nail polish remover or a paste made with baking soda and gentle dish soap.
How to get food coloring off skin
Food coloring is quite stubborn but rubbing the stains with acetone nail polish remover or rubbing alcohol may do the trick. If the dye doesn’t disappear, try using over-the-counter hydrogen peroxide (3% concentration).
For people with sensitive skin, a gentler option is baking soda. Wet your fingertips with water, dip them in baking soda, and rub the affected area.
How to get super glue off skin
Super glue is super strong, but thankfully, it isn’t so super at gluing fingers together. To remove super glue from fingers, rub a small amount of acetone nail polish remover on the bonded parts of the skin, gently peel the skin apart and then wash the area with soap and water.
Removing super glue from more delicate areas is trickier. You may be able to remove super glue from your lips by washing them with a lot of warm water and then gently peeling or rolling the lips apart. If that doesn’t work, see your doctor.
If you get the glue on your eyelashes or eyelids, flush the area with water. If your eye is stuck closed, seek immediate medical attention.
How to get paint off skin
The way to get paint off skin varies depending on the type of paint. For water-based paints (acrylic, fabric, latex), scrub the paint marks with a washcloth and bar soap or dish soap. Add a little salt or sugar to the lather for exfoliation if the soap alone isn’t enough. Or try wiping away the paint with a cotton ball dipped in rubbing alcohol.
For splotches of oil-based or enamel-based paint, paint thinner and turpentine are removal options. Both can be harmful to your health with frequent exposure, but if you’re not someone who frequently has to remove paint from their skin (like a house painter or artist), you can rub away the splotches with a small amount of either if you feel comfortable doing so. Apply glycerin first if you happen to have it on hand to loosen the paint first. Wash the areas with soap and water when you’re finished.
Alternatively, apply a generous amount of mayonnaise, vegetable oil, olive oil, or baby oil. Scrub with your fingers for a few minutes to loosen the paint, then let the oil sit on your skin for another few minutes. Wipe it off with a paper towel and rinse with water.
How to get ink off skin
If your skin has been stained with water-soluble ink (found in rollerball pens and some gel pens), washing with soap and water should do the trick.
If soap and water fail, the ink may be oil-based, in which case, wipe the areas with rubbing alcohol on a cotton ball or washcloth. If you don’t have to rub alcohol, try using alcohol-based hand sanitizer, hair spray (one that contains alcohol), acetone nail polish remover, or white vinegar. These may not work quite as well as rubbing alcohol, so you may have to treat the stained areas more than once.
Rubbing alcohol is also effective against permanent ink found in permanent markers such as Sharpie pens, especially if you attack the stain ASAP. Dip a cotton ball in it and hold it on the skin for a few seconds. Repeat as needed. Another option is Amodex Ink and Stain Remover, a Sharpie-approved product available online. It removes permanent ink and many other substances that stain the skin. You can also try applying makeup remover, olive oil, or exfoliating cleansing cream.
If you can’t get permanent ink off, don’t worry, it will disappear on its own over time.
How to get tie-dye off skin
Rinse the skin with water as soon as possible after the dye gets on your skin. If it has already been set, it may come off with plain old soap and water. If it doesn’t, Rit, a dye maker, recommends exfoliating the affected skin with a body scrub or a mix of sugar and hand lotion.
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
The Surprising Link Between Breast Cancer and Skin Cancer
Medical Review By: Dr. Ted Schiff
Anyone who’s had breast cancer or skin cancer should know the unfortunate truth: Having one of these diseases seems to increase the likelihood of developing the other.
The risk for getting hit with this double whammy appears to be highest among younger women. And unfortunately, the form of skin cancer most closely associated with breast cancer also happens to be the most dangerous, melanoma.
Here’s a summary of what the science says.
Young breast cancer survivors at increased melanoma risk
A 2004 study looked at a large database of health records for women in nine regions of the United States. Breast cancer survivors age 50 and younger had a 46% increased risk for later being diagnosed with melanoma. Women who’d had melanoma were more likely than others to develop breast cancer, though the increase in risk was much lower.
In a 2011 study, female breast cancer survivors under age 45 had a 38% increased risk for developing melanoma compared to the general population. Among women over 45 who survived breast cancer, the increased risk for melanoma was 12%.
A weaker link between other skin cancers and breast cancer
Any association between breast cancer and non-melanoma forms of skin cancer, which include basal cell and squamous cell cancers, is less clear. Study have yielded mixed results.
A 2013 study found that women (average age 66) who’d had non-melanoma skin cancer had a 19% increased risk for eventually being diagnosed with breast cancer. A study of more than 70,000 postmenopausal women published the same year found no link between non-melanoma skin cancers and breast cancer, but it discovered that women with a history of basal cell or squamous cell cancer who developed breast cancer were more likely to have an advanced case of breast cancer.
Are BRCA genes a double threat?
If your mom or sister had both breast cancer and skin cancer, does that mean a similar fate may await you? Research offers clues that a risk for both conditions could be inherited in your genes, though whether that’s true remains unclear.
Genes called BRCA1 and BRCA2 increase the risk for breast cancer. Some research has linked them, especially BRCA2, to melanoma, too. But the authors of a 2021 scientific review of the current evidence called that association “relatively weak” and argued that neither gene is likely to have much influence over whether or not a person develops melanoma.
What you can do
Researchers still have a lot to learn about the link between breast cancer and skin cancer, but early diagnosis of either disease is critical no matter what, as are skin cancer prevention measures.
Mammograms
Most women should consider having annual mammograms when they turn 40, according to the American Cancer Society, and make mammograms a yearly event at age 45 (then consider reducing the frequency at age 55). Women who have a family history of breast cancer or who know they carry genetic mutations such as the BRCA gene that increase their risk should begin screening earlier.
The benefits of having a doctor physically examine your breasts, or examining your own breasts regularly, has recently come into question, but the American Cancer Society suggests at least being familiar with your breasts and reporting any changes to a doctor.
Skin checks and self-exams
Frequent skin self-exams, on the other hand, are essential. Your dermatologist can advise on how often to perform them, though monthly is a common rule of thumb. The American Cancer Society has a guide on how to do a skin self-exam.
Most people should also have an annual full-body skin exam at their dermatologist’s office.
Sun protection
Everyone should protect their skin from the damaging effects of the sun, but double down on those efforts if you’re a breast cancer survivor or if you’re undergoing treatment for breast cancer or any other malignancy. Chemotherapy may make skin more vulnerable to the harms of UV rays, and radiation may have already caused skin redness or burns.
You know the rules: Use a broad-spectrum sunscreen with an SPF of 30 or higher on any day that you’ll be outside, and cover up with protective clothing.
Article Written By: Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.
The Best Face Wash and Moisturizer for Oily Skin
Medical review by Beth Mitchell, PA-C
If your skin is oily and you’re constantly fighting shine, it can be tempting to go to extremes to get oiliness under control. Maybe you buy the most drying face wash you can find, or you’ve convinced yourself that you should never use moisturizer, regardless of how light it is. Your skin is already producing more than enough oil, so isn’t extra moisture the last thing you need?
Unfortunately, getting over-aggressive in the battle against oil can make skin even greasier.
“When you over-strip the oils from your skin, the skin tries to repair itself by producing more oil,” said Beth Mitchell, PA-C, a certified physician assistant at Water’s Edge Dermatology. “So you end up in a never-ending cycle in which your skin is either too oily or too dry.”
For many people with oily skin, skipping moisturizer is also a bad idea. Well-hydrated skin provides more protection against infections, chemicals, and everyday pollutants.
Keeping skin shine-free yet clean, well-hydrated, and free of blemishes and irritation takes the right face wash in combination with the right moisturizer.
Best face wash for oily skin
First things first: If you’re still buying the same oil-fighting cleanser you used when you were a teenager, it’s probably time to stop. Many of the cleansers marketed to teens to treat acne contain benzoyl peroxide, which is too harsh for adult skin.
“Benzoyl peroxide works well, but it’s very drying,” Mitchell said. “The typical adult patient who just has some oiliness in their T zone doesn’t need such an aggressive cleanser.”
Gentler ingredients that remove excess oil from pores include salicylic acid and glycolic acid. Salicylic acid is the more drying of the two, and it does a great job of killing some of the bacteria that can cause acne, Mitchell said. Glycolic acid is milder and is particularly effective at promoting cell turnover, which helps keep pores clear and discourages blemishes from forming. Many face cleansers for oily skin contain both of these acids.
To avoid over-drying your skin, look for a cleanser that contains 2% salicylic acid, which is the most common strength available over the counter. The ideal amount of glycolic acid a cleanser should contain ranges from 10% to 20%, and the percentage you should choose depends on what your skin can tolerate.
“Glycolic acid can cause some dryness and irritation, so if your skin isn’t accustomed to it or you have sensitive skin, I wouldn’t recommend buying a cleanser with 15% or 20% glycolic acid,” Mitchell said.
Signs your cleanser is too harsh include redness (particularly around the eye area) and flaking. If washing your face with an acid cleanser twice a day makes your skin a little too dry, consider using it only once a day and switching to a gentler option for the second wash.
Top face wash picks
Mitchell like these face washes for oily skin:
- Wederm Exfoliating Cleanser with salicylic acid and glycolic acid (available in two glycolic acid strengths)
- Neutrogena Oil-Free Acne Wash with salicylic acid
- CeraVe Acne Control Cleanser with salicylic acid
- La Roche-Posay Effaclar Medicated Gel Cleanser with salicylic acid
Gentler options she recommends if those are too drying:
- La Roche-Posay Toleriane Purifying Foaming Cleanser
- Cetaphil Pro Dermacontrol Oil Removing Foam Wash
Best moisturizer for oily skin
Does oily skin need moisturizer? In some cases, no. If you have very greasy skin, you may not need to use moisturizer, or at least not every day. But if you have combination skin or your skin is only mildly or moderately oily, it’s important to use a light moisturizer to keep your skin healthy. And if you’re using a harsh cleanser or an acne product that dries your skin, or you’re using makeup wipes throughout the day to combat oiliness, you may need a moisturizer to combat the dryness and irritation that can result.
Another benefit of using moisturizer: “Newer moisturizers contain a lot of ingredients that are really healthy for your skin, such as those that fight free radicals and UV damage,” said Mitchell.
The first rule of buying a moisturizer for oily skin: “Make sure the words ‘non comedogenic’ are on the label, which means the product won’t clog pores,” Mitchell said. “Don’t buy a moisturizer that just says ‘oil free’ because it may contain other ingredients that could cause breakouts.”
The right moisturizer for you depends on how oily you are. If your skin is moderately oily, look for a serum or water-based cream that contains hyaluronic acid, which is a very lightweight humectant. Humectants work by drawing moisture from the air into the upper layer of skin.
“People with oily skin are often nervous about putting anything on their face, but hyaluronic acid is very light,” Mitchell said. “It helps protect and repair your skin, which is particularly important for those with oily skin who may be using potentially irritating cleansers and scrubs.”
If your skin is less oily, choose a light lotion that contains ceramides. These are naturally occurring fats found in the skin that prevent moisture from evaporating.
“Ceramides help repair the skin barrier, which is what prevents invaders such as bacteria and viruses from entering the underlying structure of your skin and your organs,” Mitchell explained. “When the barrier is compromised, you’re more susceptible to infections and skin breakdown in general.”
Most moisturizing serums and lotions for oily skin are designed to be absorbed quickly, typically in about 10 minutes, so you don’t have to worry about looking shiny, she added.
Keep in mind that your skin may have different needs in different seasons. If you usually use a serum, for example, you might find you need to switch to a lotion in winter, when the air is drier.
Top moisturizer picks
Mitchell likes these face moisturizers for very oily skin:
- Wederm Pure Hydration Serum with hyaluronic acid
- La Roche-Posay Hyalu Pure Hyaluronic Acid Serum
- Neutrogena Hydro Boost Hydrating Serum with hyaluronic acid
For people with mildly or moderately oily skin, Mitchell recommends these moisturizers:
- CeraVe Daily Moisturizing Lotion with hyaluronic acid and ceramides
- Cetaphil Daily Oil-Free Hydrating Lotion with hyaluronic acid
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Does Stress Cause Acne?
Medical Review By: Dr. John Minni
Pimples have a way of showing up at the worst possible time. Days or hours before a wedding, a reunion, a hot date, or a big presentation at work, a big fat blemish (or two, or three) appears, giving you yet another reason to feel stressed.
But does stress actually cause acne? Not exactly.
“There are several causes of acne, but stress isn’t one of them,” said John Minni, DO, a board-certified dermatologist at Water’s Edge Dermatology. “If you already have acne, however, stress can make it more severe.”
The stress-acne connection
Genetics and fluctuating levels of androgen hormones during puberty, menstruation, pregnancy, and menopause are two main factors that set the stage for acne. Taking certain medications, such as birth control pills, lithium, and corticosteroids, can also make people susceptible to acne.
Stress won’t give you acne if you’re not already predisposed to it, but it can make acne worse by causing levels of certain hormones to temporarily increase.
“When your fight-or-flight response is activated, the body releases stress hormones, such as cortisol and androgens,” Dr. Minni explained. “These hormones increase your skin’s oil production, which can exacerbate acne.”
Stress, anxiety, and fear might also worsen acne by triggering the production of cytokines, tiny proteins that stoke inflammation, including inflammation of the area around sebaceous glands, the glands that produce oil.
Stress-related disruptions in healthy habits play a role, too. “When you’re anxious, you may not sleep or eat as well as you normally do, which can worsen acne,” Dr. Minni said.
Some people turn to smoking, which is linked to an increase in blemishes. Others pick at their skin when they’re stressed, which can make blemishes more irritated and inflamed.
How to prevent stress-related acne breakouts
You can’t avoid stress altogether, but if you’re prone to acne, you can take steps to limit the effects stress has on your skin.
Develop a stress-relief habit
Dr. Minni encourages patients to embrace practices that relieve stress, whether it’s regular exercise or relaxation techniques such as yoga, meditation, or deep breathing, all of which can lower cortisol levels.
Follow an acne diet plan
There is no acne diet per se. But research suggests there are some foods that cause acne, or at least foods that make breakouts more likely in certain people. And they are some of the same foods we tend to “stress eat.”
“When people are stressed, they tend to eat more processed and sugary foods, which can increase inflammation and oil production,” said Dr. Minni. Studies suggest that swapping high-glycemic foods (think white bread, white rice, cookies and soda) for low-glycemic ones (think fruits, vegetables, beans and whole-cut oats) can make acne less severe.
Pre-plan for an important event
Finally, if you have an important event coming up and you’re determined to avoid stress-related acne flares, talk to your dermatologist.
“Certain treatments can be used temporarily to head off stress acne that doesn’t require any downtime, such as anti-inflammatory medications, gentle facials, and light therapy,” said Dr. Minni.
“For an event such as a wedding or the prom, where your appearance is particularly important, your dermatologist may recommend something stronger, such as low-dose steroids, to help you look your best.”
Contact Our Acne Dermatologists at Water's Edge Dermatology
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Medical Review By: Dr. John Minni
5 Myths About Skin Aging and Wrinkles
Medical review by Camila Yepes, PA-C
No one wants to look older than they are. But with so many myths about wrinkles, it can be hard to know what’s true or how to keep your skin looking as smooth and youthful as possible.
Camila Yepes, PA-C, a board-certified physician assistant at Water’s Edge Dermatology, debunks some of the most common misconceptions about wrinkle prevention and treatment and explains what it really takes to keep fine lines and creases at bay.
Myth 1: How much you wrinkle depends mainly on your genes
Fact: Your genes play a role in how your skin ages, but how quickly you develop wrinkles depends mostly on sun exposure.
“You may have good genes, but if you’re not protecting your skin from ultraviolet rays, that’s going to cancel out any genetic advantage you may have,” Yepes said.
Consider what causes wrinkles. They happen because the fat in deep layers of the skin shrinks with age, and because the skin naturally thins and becomes less elastic. Spending too much time in the sun makes things worse by speeding the breakdown of collagen and elastin, proteins that make skin look plump and firm.
Getting too much sun exposure isn’t the only lifestyle factor that encourages wrinkles. Smoking and over-consuming alcohol do, too, Yepes noted.
So even if your parents look great for their age, don’t assume the same will be true for you. To prevent wrinkles, use a broad-spectrum sunscreen with SPF 30 or higher every day, skip the cigarettes and vape pens and curb any excessive drinking.
RELATED: How to Prevent Wrinkles While You Still Can
Myth 2: Botox is always the best treatment for wrinkles
Fact: There are two main types of wrinkles, and Botox is effective against only one of them.
“Botox is a good treatment for dynamic wrinkles, such as crow’s feet and forehead lines, which are caused by muscle contractions that happen with repetitive facial movements,” said Yepes. Botox injections work by temporarily paralyzing the muscles so they can’t contract.
But Botox won’t do anything for the other type of wrinkles, called static wrinkles. These develop due to the loss of elasticity and fat in the skin. Examples of static wrinkles include neck wrinkles, wrinkles under the eyes and marionette lines, which start at the corners of the mouth and extend to the chin.
If you’re bothered by static wrinkles, ask your dermatologist about wrinkle treatments that help minimize them, including retinol cream and dermal fillers such as Juvéderm and Restylane.
Myth 3: Facial exercises are good for preventing wrinkles
Fact: Repetitive movements lead to dynamic wrinkles, so facial exercises and “facial yoga” aren’t going to take years off your face.
“Performing these movements could actually make dynamic wrinkles worse because you’re forcing your facial muscles to contract,” Yepes said.
Whole-body physical exercise, on the other hand, can benefit the skin.
“People who exercise regularly usually look younger than those who don’t,” Yepes noted. Chalk up the benefits in part to better blood flow, which means that more oxygen and nutrients reach the skin and cellular waste and toxins are whisked away faster.
Myth 4: People with oily skin wrinkle less
Fact: People often associate dry skin with wrinkles, but generally speaking, oily skin is just as prone to developing these hallmarks of aging.
“Dry skin sometimes looks older because lack of moisture can make wrinkles and sagging look more prominent, but oil production has nothing to do with how quickly the skin ages,” Yepes said.
One caveat: There’s some evidence that people with oily skin do tend to have shallower forehead wrinkles, thanks to a greater density of sebaceous (sebum-producing) glands in the forehead, which is associated with thicker skin.
If dry skin is making you look older, you may need to use a more effective moisturizer. “Look for one with hyaluronic acid, which is particularly effective at maintaining moisture,” Yepes suggested.
Myth 5: Collagen supplements can reduce wrinkles
Fact: Collagen loss plays a major role in skin aging. But if collagen supplements work for treating wrinkles or sagging skin, there’s no good evidence to prove it.
“Good nutrition is important for the overall health of your skin, but taking extra collagen can’t firm sagging skin,” Yepes said.
Some studies have shown slight improvements in skin appearance with collagen supplementation, but these studies were small and sponsored by the product manufacturers. In reality, it’s not clear whether collagen supplements even enter the bloodstream. Acids in the stomach may break them down before they get there.
“If you want to build collagen, it’s better to use topical products that have been demonstrated to do so, such as retinol cream and vitamin C serum,” Yepes advised.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
Teen Acne Isn’t Just a Cosmetic Problem
Medical review by John Minni, DO
If you’ve ever had acne, you know how frustrating it can be. But for some people, it’s more than frustrating.
“Many people think that acne is just a cosmetic issue, but the condition can lead to depression and anxiety, and teenagers are particularly vulnerable,” said John Minni, DO, a board-certified dermatologist at Water’s Edge Dermatology.
“They’re at a stage when they’re trying to fit in and establish their identity, so it’s disheartening for them to be constantly reminded of their acne, whether they’re looking in the mirror or other people point it out.”
Scientists have long suspected that acne and depression were linked, as well as acne and anxiety. In 2020, a review of 42 studies published in the Journal of the American Academy of Dermatology confirmed these associations. The authors advised dermatologists to pursue aggressive treatment in patients with acne and to consider screening them for mental health issues or referring them to a mental health professional.
Teen acne has wide-ranging effects
Coping with acne, regardless of its severity, can affect nearly every aspect of a teen’s life, Dr. Minni said.
“Acne can contribute to low self-esteem and a poor self-image and make teenagers a target for bullies,” he explained. “As a result, they may try to make themselves invisible.” They may avoid speaking up in class, trying out for sports, joining clubs and hanging out with friends, or making new ones.
Acne can make grooming difficult for teenage boys who are starting to shave and may struggle to avoid nicking blemishes. Body acne may limit clothing choices. Teens ready to date may worry that no one will find them attractive.
Even though many teens get acne, it can create a feeling of loneliness.
“Teenagers are bombarded with images and videos of people with perfect skin, especially on social media sites such as Instagram, that can make them feel like they’re the only person who struggles with acne,” Dr. Minni said. They may not realize that in many cases the photos have been retouched or the person is wearing heavy makeup.
Who’s at risk for acne-related depression and anxiety?
Not every teenager with acne will develop emotional health problems. And not all cases of depression and anxiety in teens are related to acne.
“Acne can be a big instigator of depression and anxiety, but these illnesses are multi-faceted,” Dr. Minni says. “Battling acne may simply be the tipping point for teenagers who are already vulnerable to depression and anxiety due to genetics and environmental factors such as lack of social support.”
Gender may also play a role. Studies have shown that teen girls suffer more emotional distress due to acne than boys. However, the gap appears to be narrowing, according to Dr. Minni.
“The pressure on teen boys to meet certain standards of attractiveness has increased significantly over the years,” he said. “But the good news is that boys are now more likely to see a dermatologist for their acne. It used to be that ‘tough guys’ didn’t do that.”
Acne treatment for teens is critical
Treating acne early on can help reduce the risk of harmful psychological effects. If a teenager has already started showing signs of depression and anxiety related to acne, prompt treatment can help ease or resolve their symptoms, Dr. Minni noted.
“Early intervention is also important because fewer blemishes mean there are fewer opportunities to develop acne scars,” he added. “These scars may be permanent and can cause a lot of distress for years to come.”
Acne does sometimes respond well to over-the-counter cleansers and treatments, but many teens will need to see a dermatologist get results. If OTC products don’t lead to significant improvement after three months of regular use, that’s a sign to see a dermatologist.
“Parents and teens should know that dermatologists have more options for treating acne than ever before that are simple, safe, and affordable,” Dr. Minni said. “Teenagers can get extraordinary results from acne treatment, and that can help restore their confidence.”
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org and many other outlets.
When to Worry About a Spider Bite
Medical Review By: Thomas Pham, MD
Spider bites are more common than you might think. Garden spiders that get trapped in clothing or under hair may bite two or three times before you flick them off or crush them by scratching. Dermatologists sometimes call these bites “breakfast, lunch, and dinner.”
Fortunately, when it comes to spider bites, the ick factor is almost always worse than the bite. While nearly all spiders produce venom, it’s rarely strong enough to harm humans. Plus, most spiders’ fangs are too short to penetrate human skin.
Bites that produce mild pain or itching can usually be treated with over-the-counter hydrocortisone cream or ointment, cold compresses, and an oral antihistamine if needed to help with itching or swelling.
If you’re unlucky, however, you might encounter one of the two types of spiders in the United States that can seriously harm humans: the black widow and the brown recluse. While they’re not aggressive, they do bite in some circumstances, and there’s a chance you may need emergency treatment if you are bitten.
If possible, take a photo of the spider to help your doctor diagnose the bite and choose a course of treatment.
Black widow spiders
What they look like
Black widows have an almost spherical abdomen and are about half an inch long.
Southern black widow spiders are black with a red hourglass pattern on the underside of the body (females) or red and white markings on the sides of the body (males). In Northern black widows, the hourglass pattern is broken, and there may be a row of red spots on the back and diagonal whitish markings on the side (females). Male Northern black widows usually have faint red and white spots on the underside of the body.
What to know
Black widows can be found anywhere in the United States but are more common in the South and West.
While male black widow spiders don’t bite humans, females can and will attack to defend themselves if you disturb them, especially if they’re in their web protecting their eggs.
You’re most likely to run into a black widow’s web in dark and undisturbed areas, such as woodpiles, eaves, fences, and water meter boxes. When indoors, black widows usually build their webs in cluttered areas, such as a garage or basement.
Spider Bite Symptoms and Treatment
Black widow bites cause a sharp, pinprick-like pain. In many cases, reactions are relatively mild and limited to redness and swelling of the bite area. (You may also notice two tiny red spots that are actually tiny fang marks.) These symptoms appear 15 to 60 minutes after you’re bitten and can be treated at home with cold compresses, over-the-counter pain relievers, elevation (if the bite is on your arm or leg), antibiotic cream, or lotion.
Some people develop a severe reaction and experience signs and symptoms such as stiff and painful muscles, fever, chills, nausea, vomiting, difficulty breathing, weakness, tremors, headache, and belly or back pain. These may develop in as little as 15 minutes after the bite or several hours later. If you have a severe reaction, go to the emergency department or call 911.
Fatalities are rare. Elderly people and small children are more likely to have a severe, possibly life-threatening reaction.
Treatments for severe black widow bites include prescription pain relievers, muscle relaxants, and antivenom.
Brown recluse
What they look like
Brown recluse spiders are tan to dark brown with long legs. They often have a darker brown violin shaped-marking just behind their head.

What to know
Brown recluse spiders are typically found in Midwestern and Southern states. They truly are reclusive and would much rather avoid you than attack you. When they do bite, it’s usually because they were trapped against your skin and tried to defend themselves. This may happen if a brown recluse makes its way into your bedsheets, clothes, or shoes.
Brown recluses like to live under rocks, woodpiles, and debris. They’re also well adapted to living indoors, where they prefer dark areas such as basements, attics, closets, and cabinets.
Bite symptoms and treatment
If you’re bitten by a brown recluse, you may not notice right away because the bite is often painless or only mildly painful. In fact, you may never know you’ve been bitten. If symptoms do occur, they typically start three to eight hours after the bite and include redness, tenderness, and a sore at the site of the bite. Other possible symptoms include fever, chills, vomiting, muscle aches, and itching.
Severe symptoms such as extreme pain or trouble breathing require immediate medical attention. Bites in small children, elderly people, and those in poor health also require immediate medical attention.
Brown recluse bites usually heal within three weeks. However, in about 10% of cases, a bite can cause tissue death in the affected area. A skin ulcer or blister with a blue, purple or black center develops and may become infected.
Treatments for severe brown recluse bites include antibiotics, antihistamines, and steroids. Some victims need surgery to remove the damaged tissue around the wound.
At-home treatments for mild bites are the same as those for mild black widow bites.
Hobo and yellow sac spiders: Cause for concern?
These two types of spiders have a nasty reputation. It was once thought that their bites, like that of a brown recluse, could lead to tissue death. But researchers now say there’s no evidence to support that idea. While hobos and yellow sacs do bite occasionally, you’re unlikely to experience symptoms beyond minor pain, swelling, and redness.
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org, and many other outlets.
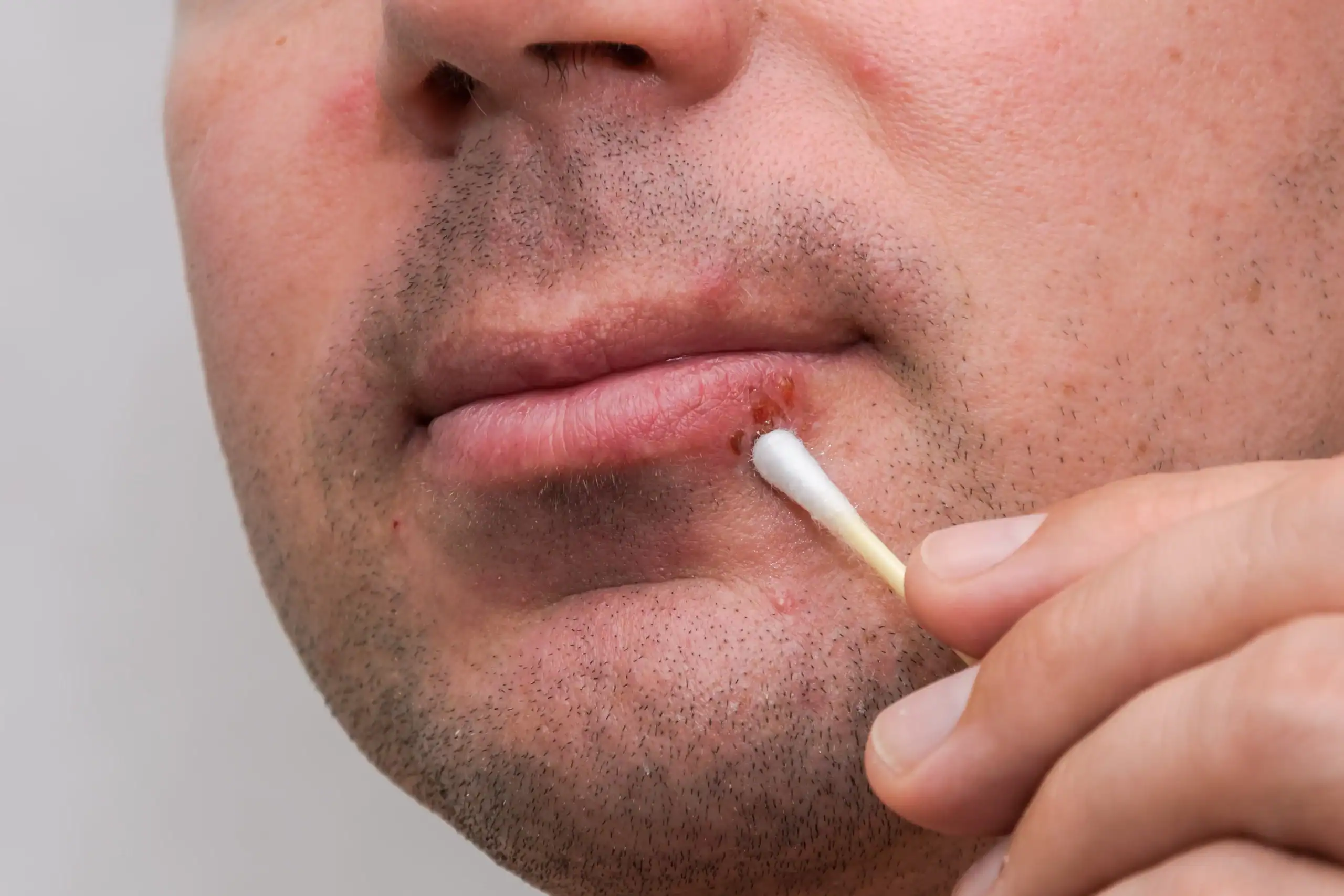
Are Cold Sores Contagious? Here’s What to Know
Medical Review By: Camila Yepes, PA-C
Cold sores, aka fever blisters, are caused by the herpes simplex virus (HSV) — not by colds or fevers. But like colds, they are very contagious. You can spread HSV at any point from the first warning tingle up until the cold sore scab has completely disappeared. It’s even theoretically possible to spread the virus when you don’t have a cold sore.
Read on to learn more about cold sores and how to stop the spread.
What causes cold sores?
Oral herpes infections are spread from person to person, usually through direct contact — for example, through kissing or oral sex. They can also be spread by sharing personal items such as drinking glasses or lip balm.
Of course, you can develop a cold sore without coming into contact with someone who has one. That’s because most adults have already been infected with HSV, typically during childhood, and the virus remains in the body, hiding in nerve cells, for life.
Certain triggers can “wake up” the virus, resulting in a cold sore. These include sun exposure, cold wind, cracked lips, hormonal changes during menstruation or pregnancy, emotional stress, surgery, and anything that taxes your immune system, such as the common cold or another illness.
Cold sore stages
Stage 1: You’ll feel tingling, itching, or burning somewhere around your mouth or at the base of your nose. You’re already contagious at this stage (called the prodome stage). This is the time to apply an over-the-counter product such as Abreva or take an oral antiviral medication such as valacyclovir if your doctor has prescribed one. Valacyclovir is highly effective at shortening outbreaks when taken within the first 24 hours of symptoms.
Stage 2: After a day or two of tingling, blisters filled with clear liquid develop and the skin under and around them reddens. Cold sores spread easily at this stage. Do not break the blisters.
Stage 3: A few days later, usually on day four, the blisters break on their own, creating an open sore. This stage, which doctors call the ulcer or weeping stage, is when a cold sore is the most contagious.
Stage 4: The sore starts to dry out and scab over. It may crack or bleed. The sore is still contagious.
Stage 5: The sore begins to scab over. When the scab falls off, the area may look pink or red for a few days. The sore is no longer contagious once the skin heals.
Stopping the spread
Cold sores can spread through saliva and through skin-to-skin contact. To avoid infecting other people, follow these tips during every stage of a cold sore.
Avoid touching the area. If you must scratch when it itches, wash your hands thoroughly afterward. Apply any topical treatments with a cotton swab, not your finger. Don’t pick at the scab (this will only prolong the healing process).
Don’t share any personal items. This includes food, drinks, eating utensils, straws, toothbrushes, razors, lip balm, petroleum jelly and any cold sore cream or ointment you use.
Don’t kiss anyone or nuzzle your baby. Kissing your baby while you have a cold sore is dangerous because the virus is far more severe in infants, who don’t have a fully developed immune system. You should also avoid close contact with anyone who has a weakened immune system, and anyone who has eczema. People with eczema are at risk of a potentially serious skin infection called eczema herpeticum.
Refrain from oral sex. Genital herpes is typically caused by a different strain of HSV (HSV-2), but it is possible for your partner to develop “oral herpes” (HSV-1) on their genitals from exposure to a cold sore on your mouth.
The best way to avoid spreading cold sores is to avoid getting them in the first place. While you have limited control over some common triggers, you can lower your risk of outbreaks caused by sun exposure by wearing lip balm with an SPF of at least 30.
If you get cold sores several times a year, ask your Water's Edge dermatologist about a prescription for an antiviral medicine to take at the first sign of an outbreak. People who get cold sores many times a year may be prescribed a low-dose antiviral medication to take daily in order to help prevent outbreaks. Taking supplements of the amino acid lysine coupled with avoiding foods high in the amino acid arginine (notably, nuts and seeds) may help, too.
Get Cold Sore Treatment, Contact Our Dermatologists Today!
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention magazine, jnj.com, BCRF.org and many other outlets.
Medical Review By: Camila Yepes, PA-C