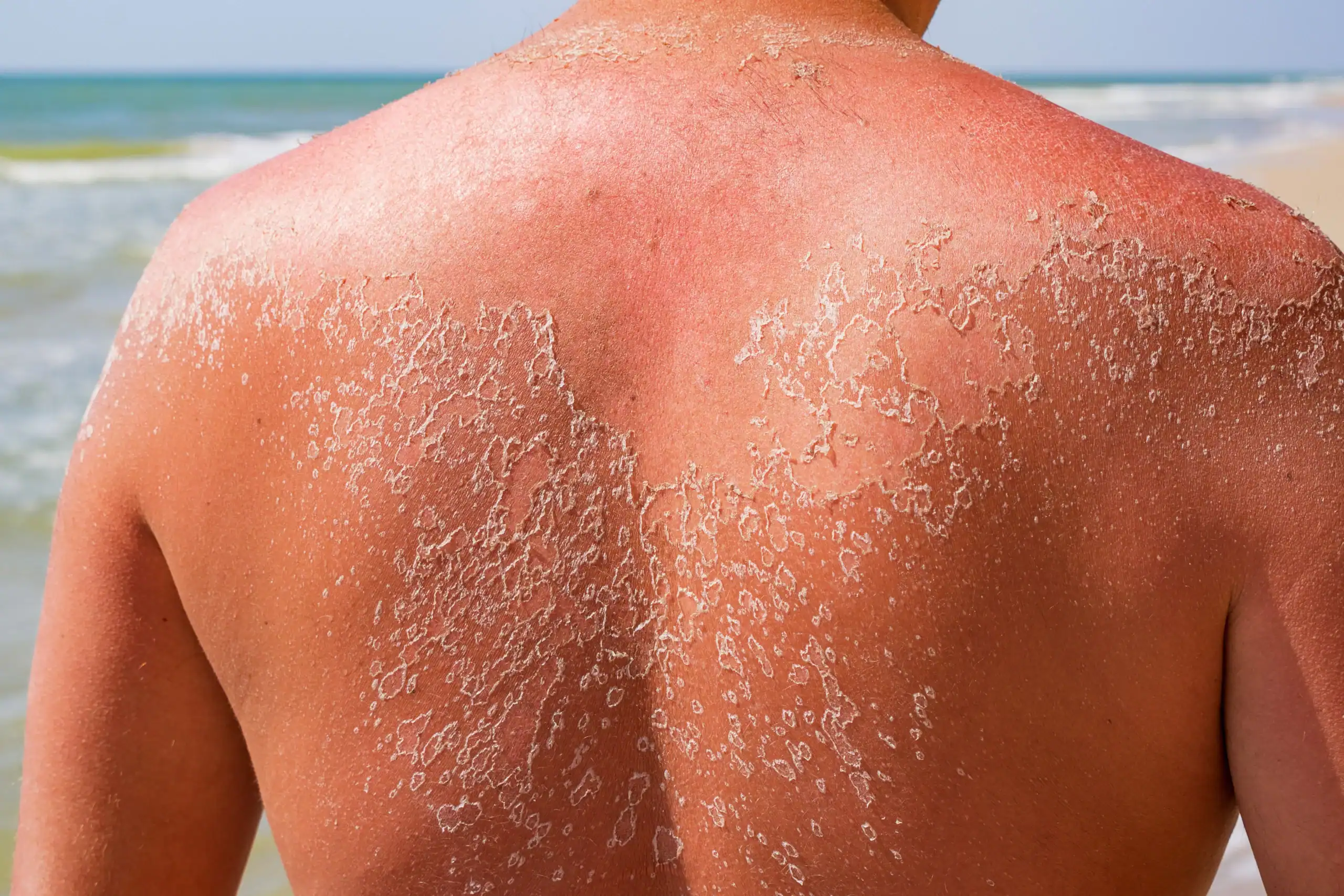
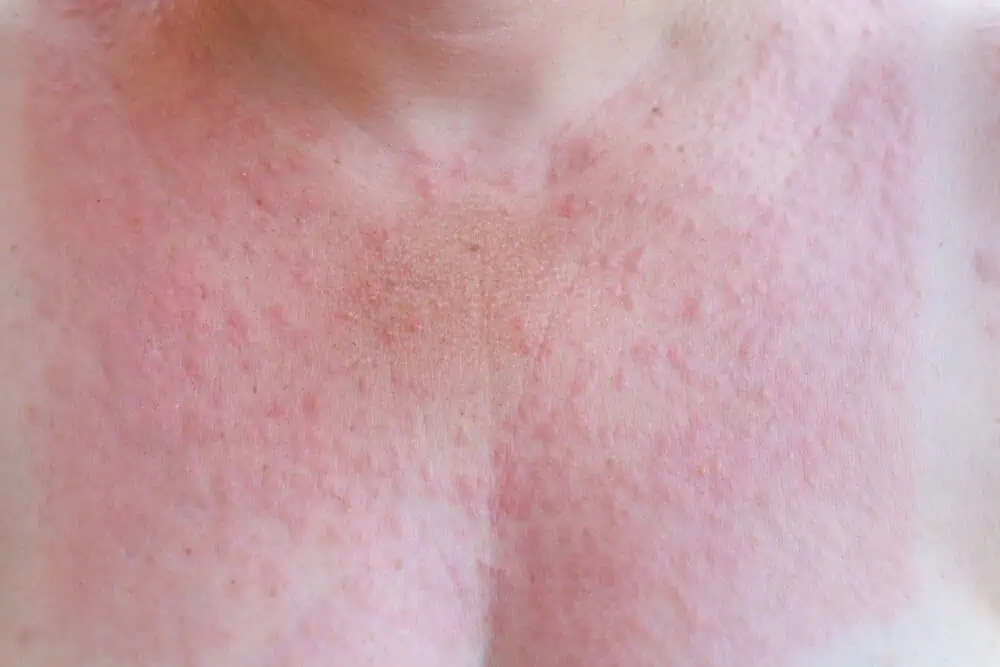
Sunscreen
Sunscreen and other sun safety measures help prevent skin damage and wrinkles, and reduce the risk of developing skin cancer. Newer broad-spectrum sunscreens contain products to block both UVA and UVB rays. To be effective, sunscreen should be reapplied at least every two hours. The American Academy of Dermatology (AAD) recommends seeking shade when possible. Avoid sunbathing, and always wear a wide-brimmed hat, sunglasses and protective clothing.
A typical white T-shirt has an SPF of 3. Colorless dyes that increase the SPF of fabrics to an SPF of 30 are available as laundry products. If you must be in the sun, use a broad-spectrum sunscreen with an SPF of at least 30, even on cloudy days. Even when you are wearing sunscreen, be aware that some ultraviolet light may still get through, so do not prolong your sun exposure.
Sunscreen FAQs
Sunscreens work by absorbing, reflecting or scattering the sun’s rays on the skin. They are available in many forms, including ointments, creams, gels, lotions, sprays and sticks. All are labeled with SPF numbers. The higher the SPF, the greater the protection from sunburn caused mostly by UVB rays; however, this does not increase the length of time for sun exposure.
Broad-spectrum sunscreens protect against both UVA and UVB rays. They do a better job of protecting skin from other effects of the sun, including photodamage, photodermatitis and rashes from sun exposure.
Sunscreens that block UVB rays are composed of some or all of the following chemicals: padimate O, homosalate, octyl methoxycinnamate, benzophenone, octyl salicylate, phenylbenzimidazole sulfonic acid and octocrylene.
Broad-spectrum sunscreens add oxybenzone or avobenzone (Parsol 1789) to block UVA rays. Mexoryl is a chemical that blocks UVA; its broad-spectrum characteristics allow sunscreens to be made with very high SPF factors. Physical sunscreens/blocks or chemical-free sunscreens contain titanium dioxide and/or zinc oxide, which reflect UVA and UVB and are especially useful for people allergic to chemical sunscreens.
Sunscreen should be applied 30 minutes before exposure to the sun. Even water-resistant sunscreens should be reapplied often, about every two hours or after swimming, drying off or sweating.
Sunscreen should be applied generously and evenly so as not to miss any areas of exposed skin. It should be kept out of the eyes, and UV light-blocking sunglasses should be worn. Read our sunscreen facts file for more helpful information.
Self-tanning lotions and sprays are a safe alternative to tanning. They contain dihydroxyacetone, which interacts with proteins in the skin to produce an orange/tan color that does not wash off. However, the color of self-tanners only has an SPF of 4. This is not enough protection from the sun; therefore, sunscreen with an SPF of at least 15 must be used and reapplied every two hours.
Tips for Sun Protection
Sun exposure is the most preventable risk factor for all skin cancers, including melanoma. You can have fun in the sun and limit your risk of developing skin cancer.1,2
Stay safe in the sun with these basic tips, and see our sun safety page for more.
- Generously apply a water-resistant sunscreen with an SPF of at least 30 that provides broad-spectrum protection from both ultraviolet A (UVA) and ultraviolet B (UVB) rays to all exposed skin. Reapply approximately every two hours, even on cloudy days, and after swimming or sweating. Look for the AAD SEAL OF RECOGNITION™ on products that meet these criteria.
- Wear protective clothing, such as a long-sleeved shirt, pants, a wide-brimmed hat and sunglasses.
- Seek shade when appropriate. Remember, the sun’s rays are strongest between 10am and 4pm. If your shadow is shorter than you are, seek shade.
- Protect children from sun exposure by playing in the shade, using protective clothing and applying sunscreen.
- Use extra caution near water, snow and sand because they reflect the damaging rays of the sun, which can increase your chance of sunburn.
- Get vitamin D safely through a healthy diet that may include vitamin supplements, not the sun.
Your sun protection plan isn’t complete without a dermatology team. Find the Water’s Edge location nearest you and call today.
[1] American Cancer Society. 2016 Cancer Facts and Figures.
[2] Robinson, JK. Sun Exposure, Sun Protection and Vitamin D. JAMA 2005; 294:1541-1543.
Squamous Cell Carcinoma (SCC) Skin Cancer Treatment in Florida
Squamous cell carcinoma (SCC) is a common form of skin cancer that develops from abnormal squamous cells in the outer layers of the skin. SCC often arises from long‑term sun exposure and may develop from actinic keratosis, a precancerous skin condition.
At Water’s Edge Dermatology, our specialists provide comprehensive squamous cell carcinoma treatment in Florida, offering both surgical and non‑surgical options based on the size, location, and aggressiveness of the tumor.
If left untreated, squamous cell carcinoma can grow deeper into the skin and surrounding tissues and, in some cases, may spread to lymph nodes or other areas of the body. Early diagnosis and treatment significantly improve outcomes.
Squamous Cell Carcinoma FAQs
SCC usually looks like a red, crusted, or scaly patch on the skin, a non-healing ulcer, or a firm red nodule. SCC generally appears on sun-exposed areas such as the head, neck, ears, trunk, and arms, but it also can develop on other areas of the body.
With early detection and proper treatment, SCC is curable. Allowed to progress, SCC can invade and destroy much of the tissue surrounding the cancerous tumor, which can be disfiguring.
Some SCCs, such as those that develop on a lip or an ear, can be particularly aggressive. Left untreated, aggressive SCCs have a greater risk for metastasis (spreading) to the lymph nodes and other internal organs. This makes early diagnosis and treatment of SCC essential.
A Water’s Edge Dermatology practitioner should examine any lesion that looks like a red, crusted or scaly patch, or a non-healing sore.
Avoiding unprotected exposure to the sun’s UV rays is the best form of skin cancer prevention at any age, even if you’ve had an SCC removed. Here’s how you can stay safe in the sun:
- Generously apply a broad-spectrum, water-resistant sunscreen with an SPF of 30 or more to all exposed skin. Broad spectrum provides protection from both ultraviolet A (UVA) and ultraviolet B (UVB) rays. Reapply approximately about every two hours, even on cloudy days, and after swimming or sweating.
- Wear protective clothing, such as a long-sleeved shirt, pants, a wide-brimmed hat, and sunglasses, where possible.
- Seek shade when appropriate, remembering that the sun’s rays are strongest between 10 a.m. and 4 p.m. If your shadow is shorter than you are, seek shade.
- Protect children from sun exposure by playing in the shade, using protective clothing, and applying sunscreen.
- Use extra caution near water, snow, and sand because they reflect the damaging rays of the sun, which can increase your chance of sunburn.
- Get vitamin D safely through a healthy diet that may include vitamin supplements. Don’t seek the sun.
- Avoid tanning beds. Ultraviolet light from the sun and tanning beds can cause skin cancer and wrinkling. If you want to look like you’ve been in the sun, consider using a sunless self-tanning product, but continue to use sunscreen with it.
- Check your skin regularly. If you notice anything changing, growing, or bleeding on your skin, see a Water’s Edge Dermatology practitioner. Skin cancer is very treatable when caught early.
Diagnosis and Treatment of Squamous Cell Carcinoma
Before SCC can be treated, the diagnosis must be confirmed with a biopsy. This simple procedure can be performed in the office and involves removing a small amount of tissue so that it can be examined under a microscope.
Most patients with localized SCC (cancer that is confined to the tumor and that has not spread) have an excellent prognosis. Cure rates range from 85-95% or greater.
If the diagnosis is SCC, a variety of surgical and nonsurgical skin cancer treatment options are available. Your Water’s Edge Dermatology practitioner will choose an appropriate treatment after considering the location of the tumor, size, microscopic characteristics, health of the patient, and other factors.
Treatment for squamous cell carcinoma depends on the location, size, depth, and microscopic features of the tumor, as well as the patient’s overall health. Water’s Edge Dermatology offers a range of skin cancer treatment options, including both surgical and non‑surgical therapies, to ensure appropriate and effective care.
Most treatment options are relatively minor, office-based procedures that require only local anesthesia.
These include:
- Simple surgical excision. Removes the cancer and some of the surrounding healthy tissue. The removed specimen is examined under a microscope to determine if all of the skin cancer has been removed.
- Mohs Micrographic Surgery. Performed by a specially trained dermatologic surgeon, Mohs surgery allows the surgeon to spare as much normal skin as possible while simultaneously removing the cancer.
- Cryosurgery. Removes the tumor by freezing it with liquid nitrogen.
- Electron Beam Therapy is a specialized non‑surgical radiation therapy used to treat select squamous cell carcinomas. EBT delivers targeted radiation to destroy cancer cells while minimizing damage to surrounding healthy tissue.It is often recommended for SCCs located on cosmetically sensitive or high‑risk areas such as the face, ears, lips, nose, or eyelids, or when surgery may not be the best option.Learn more about Electron Beam Therapy for Skin Cancer
- Topical therapy. Medications such as imiquimod and 5-fluorouracil can be applied at home to treat the cancer.
Water’s Edge Dermatology treats squamous cell carcinoma at multiple locations throughout Florida, providing patients access to advanced skin cancer care close to home.
FOR ALL PATIENTS undergoing cryosurgery, biopsy or curettage and electrodessication:: Read this PDF for wound care instructions for cryosurgery (liquid nitrogen), biopsy, curettage and electrodessication (C&D) | (PDF is also available in Spanish.)
Follow-Up Care
Follow-up appointments with a Water’s Edge Dermatology practitioner are essential. SCC can recur, and studies show that individuals who develop SCC have an increased risk of developing future skin cancers, including melanoma.
The recommended follow-up may include a full-body skin examination at least once a year to check for abnormal moles or lesions. Patients also should perform regular skin self-examinations and should be alert to any non-healing sores and other changes that develop on the skin. If any of these are spotted, schedule an appointment to see a Water’s Edge Dermatology practitioner.
Who May Benefit From Non‑Surgical Squamous Cell Carcinoma Treatment?
Non‑surgical treatments, including electron beam therapy, may be appropriate for patients who:
- Have SCCs in areas where surgery may affect appearance or function
- Have recurrent or high‑risk lesions
- Are not ideal surgical candidates
- Prefer a non‑surgical treatment approach when clinically appropriate
A dermatology consultation is required to determine the safest and most effective treatment plan.
If you’ve been diagnosed with squamous cell carcinoma or have a suspicious skin lesion, schedule an evaluation with a Water’s Edge Dermatology specialist to discuss your treatment options.
Learn More About Skin Cancer
Moles
Moles, also known as nevi, may be pigmented or skin-colored. They arise in the pigment-producing cells of the skin (melanocytes). While moles may be congenital (present at birth), they more commonly develop throughout childhood. Moles may be flat or elevated, and grow to about the size of a pencil eraser. They can develop anywhere on the body and may disappear with time.
Moles are typically brown or black, but may range in color from pink to tan or skin-toned. Most adults have between 10 and 40 moles. A changing or irregular mole should be looked at by a Water’s Edge dermatologist right away, as it may indicate cancer. All moles should be examined by a dermatologist annually, and suspicious lesions should be biopsied. Moles also may be removed if they become irritated or for cosmetic reasons. Any mole that grows, changes in shape or color, or bleeds should be evaluated by a Water’s Edge Dermatology practitioner.
Types of Moles
Your Water’s Edge dermatologist can tell you if your skin moles are benign or could be cancerous. The following types of moles often require treatment:
Atypical Nevus or Mole (Dysplastic Nevus)
Atypical nevi are often large with an irregular shape and uneven coloring. More than four atypical moles suggests a higher chance of developing melanoma, a serious form of skin cancer.
Congential Mole
Congenital moles are present at birth and can range in size from small to giant (larger than 20 centimeters). Approximately 1% of the population is born with congenital moles. Having large or giant congenital moles increases the risk of developing melanoma.
Spitz Nevus
Spitz nevus so closely resemble melanoma that dermatologists often cannot tell the difference by looking at them, so they are generally biopsied. These moles are usually pink, raised and dome-shaped, and they may bleed or ooze.
Acquired Mole
Acquired moles appear after birth and are common, but people with numerous acquired moles have a higher risk for developing melanoma.
Prevention Tips for Moles
Moles cannot be prevented, but you should examine your skin regularly to look for any new moles or changes in existing moles. Use the ABCDEs of Melanoma Detection to help you recognize moles needing further examination by your Water’s Edge dermatologist:
A — Asymmetry; one half is unlike the other
B — Border is irregular, scalloped, or poorly defined
C — Color is varied from one area to another
D — Diameter; melanomas are usually greater than 6 mm
E — Evolving; a mole or skin lesion that looks different or has changed
Steps to reduce development of melanoma in moles:
- Wear a broad-spectrum sunscreen with an SPF of 30 and reapply every two hours.
- Wear protective clothing, sunglasses, and a wide-brimmed hat.
- Stay in the shade when the sun’s rays are strongest, between 10 a.m. and 4:30 p.m.
- Avoid tanning beds; they have been proven to cause skin cancer, including melanoma.
- Give yourself a regular skin examination and have suspicious moles examined by your Water’s Edge dermatologist.
Treatment for Moles
Moles are common, but if you have more than 50 moles or you find a mole displaying any of the ABCDEs of Melanoma Detection, which are detailed below, visit your Water’s Edge dermatologist. You may need mole treatment to determine whether your mole is cancerous. Your particular mole treatment will depend on factors such as the size of your mole and its location. If your mole looks suspicious, your Water’s Edge dermatologist may have it biopsied to confirm whether cancer is present. If the mole is cancerous, further treatment is necessary. Seek mole treatment if:
- Your mole causes discomfort
- Your mole bleeds or is irritated
- You find the mole unattractive
- Your mole changes shape or size
- Your mole has an irregular shape
- You suspect skin cancer
Water’s Edge Dermatology offers two mole treatment options: surgical excision and surgical saving. Surgical excision involves surgically removing the entire mole from the skin and then closing the wound with stitches. With surgical shaving, the mole is saved off the skin with a surgical blade. Your Water’s Edge dermatologist will determine the right mole treatment for you.
FOR ALL PATIENTS undergoing cryosurgery, biopsy or curettage and electrodessication:: Read this PDF for wound care instructions for cryosurgery (liquid nitrogen), biopsy, curettage and electrodessication (C&D) | (PDF is also available in Spanish.)
Learn More About Skin Cancer
Merkel Cell Carcinoma
What Is Merkel Cell Carcinoma?
Merkel cell carcinoma (MCC) is a rare and aggressive type of skin cancer. It occurs when Merkel cells, which are found in the epidermis (the top layer of skin), grow out of control. The cancer can spread rapidly to the surrounding tissues, nearby lymph nodes and distant parts of the body.
Merkel Cell Carcinoma FAQs
MCC typically appears as a single, firm bump that is shiny and usually painless. It may be skin-colored, red, blueish-red or purple. It might bleed if it’s been scraped or nicked.
These tumors can develop anywhere on the body, but they most often appear on areas exposed to sunlight, such as the face, neck and arms. They tend to enlarge quickly over weeks and months.
MCC does not appear to run in families. Certain risk factors are thought to increase the likelihood of developing it, including:
- Being over the age of 50, Caucasian and male
- Having a history of heavy sunlight exposure or tanning bed use
- Having had photodynamic therapy for a condition such as psoriasis or vitiligo
- Having a history of other types of cancer
- Having a weakened immune system, either from a condition such as HIV or from taking medication that suppress the immune system
The cause of MCC is not known. In about 8 out of 10 cases, a very common virus that lives on the skin, called Merkel cell polyomavirus, is present. Experts aren’t sure how or whether it contributes to the development of MCC.
You can reduce your risk of MCC and other skin cancers by following these tips:
- Limit sun exposure. This is particularly important when sunlight is strongest, usually between 10 a.m. and 4 p.m.
- Wear sunscreen every day. Choose a broad-spectrum, water-resistant sunscreen with SPF 30 or higher and apply it generously at least every two hours.
- Cover up outdoors. Wear sunglasses, a wide-brimmed hat, long pants and a lightweight long-sleeved top if possible.
- Avoid artificial sunlight. Tanning beds and lamps are just as harmful to your skin as the sun.
- Perform skin checks. Report any bump, freckle or mole that changes in size, color or shape to your doctor ASAP.
- Schedule skin cancer screenings, especially if you’ve had any type of skin cancer in the past.
Every case of cancer is different. Survival rates for MCC depend in part on where it started, how it responds to treatment and whether it has spread to nearby areas, to distant body parts or not at all. The cancer can be fatal, but more than 75% of people whose MCC has not spread are alive five years after diagnosis.
New treatments are being tested in clinical trials.
Merkel Cell Carcinoma Treatment
The tumor is usually removed via surgery. However, because MCC has a high risk of recurring, most patients will receive additional treatment to prevent it from returning.
During surgery, the doctor will excise (cut out) the tumor and remove some healthy surrounding tissue as well. He or she may opt to do this using a procedure called Mohs surgery, in which a single layer of tissue is removed at a time. The tissue is analyzed to determine whether it’s cancerous, and if it is, the doctor repeats this process until no cancer cells are detected.
Prior to surgery, the doctor will likely perform a sentinel node biopsy to determine whether the cancer has reached nearby lymph nodes. If it has, the surgeon may remove the lymph nodes during surgery.
Radiation therapy may be given after surgery to kill any cancer cells that may remain. It is also sometimes used to treat affected lymph nodes.
If the patient isn’t healthy enough for surgery or if the tumor’s location makes it difficult or impossible to fully remove, radiation therapy may be used instead.
If MCC has spread to other parts of the body, radiation therapy may be advised, sometimes along with other treatments, to shrink the tumors or slow their growth and/or to reduce symptoms. Another option is immunotherapy, which involves giving medications intravenously (by IV) to help the body’s immune system recognize and destroy the cancer cells.
Chemotherapy is typically used only in people who haven’t responded to other treatments or are in the later stages of the disease. That’s because MCC often becomes resistant to chemotherapy drugs.
FOR ALL PATIENTS undergoing cryosurgery, biopsy or curettage and electrodessication:: Read this PDF for wound care instructions for cryosurgery (liquid nitrogen), biopsy, curettage and electrodessication (C&D) | (PDF is also available in Spanish.)
Learn More About Skin Cancer
Skin Cancer Patient Education
Skin cancer is the most common type of cancer people develop. According to the Skin Cancer Foundation, there are more new cases of skin cancer in the U.S. each year than the combined incidence of breast, prostate, lung and colon cancer. Approximately one in five Americans will develop skin cancer in the course of a lifetime, and skin cancer is increasing in all races.
While basal cell carcinoma (BCC) is the most common form of skin cancer, melanoma is the most deadly, accounting for more than 10,000 deaths per year in the U.S. alone. Actinic keratosis is the most common pre-cancer.
Skin Cancer FAQs
Sun exposure is the most preventable risk factor for all skin cancers, including melanoma. You can have fun in the sun and decrease your risk of skin cancer. Here’s how to stay safe in the sun:
- Generously apply a broad-spectrum, water-resistant sunscreen with an SPF of 30 or more to all exposed skin. Broad spectrum provides protection from both ultraviolet A (UVA) and ultraviolet B (UVB) rays. Reapply approximately every two hours, even on cloudy days, and after swimming or sweating.
- Wear protective clothing, such as a long-sleeved shirt, pants, a wide-brimmed hat, and sunglasses, where possible.
- Seek shade when appropriate, remembering that the sun’s rays are strongest between 10 am and 4 pm. If your shadow is shorter than you are, seek shade.
- Protect children from sun exposure by playing in the shade, wearing protective clothing, and applying sunscreen.
- Use extra caution near water, snow, and sand because they reflect the damaging rays of the sun, which can increase your chance of sunburn.
- Get vitamin D safely through a healthy diet that may include vitamin supplements. Don’t seek the sun.
- Avoid tanning beds. Ultraviolet light from the sun and tanning beds can cause skin cancer and wrinkling. If you want to look like you’ve been in the sun, consider using a sunless self-tanning product, but continue to use sunscreen with it.
- Check your birthday suit on your birthday.
Skin cancer is treatable when caught early. You should have your skin examined by a qualified dermatologist once a year to help watch for any changes in your skin or signs of early-stage skin cancer. Additionally, you should also perform regular skin exams on your own.
If you notice any spots on your skin changing, growing or bleeding, you should immediately call your Water’s Edge dermatologist for an appointment. Your provider will examine your area(s) of concern, make a diagnosis and recommend treatment options when appropriate.
Don’t wait! Have your skin screened today by one of our highly skilled skin care experts. Call to schedule an appointment or schedule one online.
People of all colors and races get skin cancer. Those with light skin who sunburn easily have a higher risk. Risk factors include:
- Sunburns
- Family history of skin cancer
- Exposure to X-rays
- Weakened immune system
- Scarring caused by a disease or burn
- Exposure to cancer-causing compounds such as arsenic
- Using indoor tanning devices such as tanning beds and sunlamps also increases the risk of developing skin cancer.
There are different types of skin cancer, and each tends to look a bit different.
Actinic keratosis
These dry, scaly patches or spots are considered the earliest stage in the development of skin cancer. In rare cases, an actinic keratosis (AK) can progress to a type of skin cancer called squamous cell carcinoma (SCC).
People who get AKs usually have fair skin. Most people see their first AKs after 40 years of age because AKs tend to develop after years of sun exposure. But even teens can have AKs when they live in sunny areas or use indoor tanning.
AKs form on skin that gets lots of sun exposure, such as the head, neck, hands, and forearms. Because AKs increase the risk of getting SCC, AKs are usually treated. Proper use of sunscreens can help prevent AKs.
Basal Cell Carcinoma
This is the most common type of skin cancer. It frequently looks like a flesh-colored, pearl-like bump. It also can appear as a pinkish patch of skin. Like AKs, basal cell carcinoma (BCC) develops on skin that gets frequent sun exposure, such as the head, neck, and arms. Many BCCs also form on the trunk and lower limbs.
BCC frequently develops in people who have fair skin, but it can occur in people with dark skin. BCC usually does not grow quickly and it rarely spreads to other parts of the body, but it should be treated promptly. This cancer can invade the surrounding tissue and grow into the nerves and bones, causing damage and disfigurement.
Squamous Cell Carcinoma
Squamous cell carcinoma (SCC) is the second most common type of skin cancer. This skin cancer often looks like a firm bump, scaly patch, or an ulcer that heals and then re-opens. It is usually reddish in color.
SCC tends to form on skin that gets frequent sun exposure, such as the rim of the ear, face, neck, arms, and trunk. People who have light skin are most likely to develop SCC, but it can also develop in dark-skinned people, especially those who have scarring.
Because SCC can grow deep, it can cause damage and disfigurement. Early treatment can prevent this and stop SCC from spreading to other areas of the body.
Merkel Cell Carcinoma
Merkel cell carcinoma (MCC) is a rare and aggressive type of skin cancer that’s potentially even more dangerous than melanoma.
It typically appears as a single firm bump that may be skin-colored, red, blueish-red or purple. It can develop anywhere on the body, but it most often appears on areas exposed to sunlight, such as the face, neck and arms. The cancer can spread quickly to other parts of the body.
MCC can affect anyone, but it is most common in Caucasian males over the age of 50. Because it spreads quickly, it’s important to catch it early, when it’s easier to treat.
Melanoma
This skin cancer frequently develops in a mole or appears suddenly as a new dark spot on the skin. Either way, melanoma can be deadly. Every year, more than 76,000 Americans develop melanoma and over 10,000 (nearly one person per hour) die from melanoma, making it the deadliest form of skin cancer.
Are there warning signs for melanoma?
A change is often the first sign of melanoma; therefore, it is important to know where moles appear and what they look like. When detected and properly treated before it spreads, melanoma has a high cure rate.
The ABCDE warning signs of melanoma can help people detect change. Changes that can indicate melanoma are pain, itching, or bleeding in a mole or new spot on the skin.
Atypical Fibroxanthoma
Atypical fibroxanthoma is a rare skin cancer that often appears on the head, ears or neck in the form of a red or pink bump. The lesions are typically small (1 to 2 centimeters in diameter) but often develop quickly. They usually aren’t itchy or painful. They can be crusty, scaly or broken open in the middle, and they may bleed.
Atypical fibroxanthoma is most often caused by cumulative sun exposure and typically appears in older adults with fair skin. It doesn’t normally spread to other parts of the body.
Kaposi Sarcoma
Kaposi sarcoma (KS) is a rare type of cancer that develops in cells that line blood vessels and lymphatic vessels. Kaposi sarcoma lesions usually appear on the skin and mucous membranes (such as inside the mouth or throat), but they can also develop in the lymph nodes, lungs and digestive tract. They can be flat patches, raised patches or bumps and may be red, purple or brown. They commonly appear on the face, legs and feet.
The lesions are usually painless, but lesions on the legs or in the groin area may cause painful swelling of the legs and feet.
With early detection and proper treatment, the cure rate for BCC and SCC is about 95 percent. When melanoma is detected before it spreads, it also has a high cure rate. Regular skin exams help people find skin cancers early.
One type of skin exam is the skin self-exam. During a self-exam, people examine their own skin for signs of change. If a growth, mole, sore, or skin discoloration appears suddenly, or begins to change, see a Water’s Edge Dermatology practitioner.
People who have spent time in the sun, have a family history of skin cancer (especially melanoma), have many moles or atypical moles, or have other risk factors for skin cancer should see a dermatologist for regular skin exams. Some people should have this exam once a year. Others need more frequent exams. A Water’s Edge Dermatology practitioner will recommend the frequency that is best for each patient.
If the dermatologist sees a potential skin cancer during the skin exam, he or she will remove the growth (or part of it) so it can be examined under a microscope. This is called a biopsy. A Water’s Edge dermatologist can safely and quickly perform this procedure during an office visit.
If the biopsy report confirms that the suspicious growth is skin cancer, more treatment may be needed. When caught early and when the entire growth is removed, sometimes further treatment is not needed.
If further treatment is needed, the dermatologist will choose from an array of medical and surgical treatments for skin cancer. Treatment varies with the type of skin cancer, the size and location of the skin cancer, and the needs of the patient.
Several risk factors increase a person’s likelihood of getting skin cancer. One risk factor is sun exposure. It is important to protect the skin with sunscreen and clothing, and never sunburn.
Another risk factor is light skin. However, people with skin of color get melanoma as well. In skin of color, melanoma usually appears on the palms of the hands, soles of the feet, under the nails, in the mouth, or on the genitals.
A few risk factors significantly increase a person’s risk of getting melanoma.
- If one or more first-degree relatives (parent, sibling, or child) has had melanoma, the risk significantly increases.
- Having many moles (50-100 or more) or several atypical moles also increases the risk. An atypical nevus or mole is not cancerous, but because of its different appearance, these moles need to be closely monitored for any changes.
- Having had melanoma also increases your chances of having additional melanomas.
Most skin cancer can be found early.
Your Water’s Edge dermatologist will diagnose skin cancer with a biopsy taken in the office. He or she will remove a small amount of tissue so that it can be examined under a microscope.
If skin cancer is diagnosed, there are a variety of surgical and nonsurgical treatment options available. Treatment depends on the location, size, and microscopic characteristics of the skin cancer, as well as the health of the patient and other factors.
Skin Cancer Treatment Options
- Simple surgical excision. The dermatologist cuts out the cancer and some of the surrounding healthy tissue. The removed specimen is examined under a microscope to determine if all of the skin cancer has been removed.
- Mohs Micrographic Surgery. Mohs surgery is performed by a specially trained dermatologic surgeon who removes the visible portion of the skin cancer, along with a layer of the surrounding skin. The removed tissue is then examined under a microscope to determine of it’s necessary to remove any more skin.
- Electron Beam Therapy. Electron Beam Therapy (EBT)damages or kills the cancerous cells with high-energy X-rays, which also help to prevent continued growth.
- Topical therapy. Medications such as imiquimod and 5-fluorouracil can be applied at home to treat the cancer.
Melanoma
What Is Melanoma?
Melanoma, also called malignant melanoma, is one of the deadliest forms of skin cancer. It begins in cells called melanocytes, which are located in the upper layer of skin and produce the pigment that gives skin, hair and eyes their color.
Melanoma occurs when melanocytes are damaged and start to grow uncontrollably. If not detected early, the cancer can grow deep within the skin and reach the blood and lymphatic vessels. Once there, it can spread (metastasize) throughout the body. Melanoma that has spread to other tissues is called metastatic melanoma.
Melanoma is more dangerous than most other forms of skin cancer, such as basal cell carcinoma and squamous cell carcinoma, but when it’s detected and treated early, it has a high cure rate.
Melanoma FAQs
It’s not clear how all melanomas develop, but exposure to ultraviolet (UV) radiation plays a role, particularly in fair-skinned people. A history of sunburns, especially blistering sunburns as a child or teenager, increases the risk, as does the use of tanning beds.
Not all melanomas are caused by UV radiation exposure alone. While most melanomas develop on areas of sun-exposed skin, such as the head and legs, some occur in areas that sunlight never reaches.
Melanoma typically begins on the surface of the skin. This type of melanoma is called cutaneous melanoma. Other, rare types include:
Mucosal melanoma:Develops in mucus membranes that line the body, such as the mouth (oral melanoma), throat, genitals (vaginal melanoma and vulvar melanoma), gastrointestinal tract and anus (anal melanoma).
Ocular melanoma (eye melanoma): Develops in the eye.
Subungual melanoma (nail melanoma): Develops under and around the fingernails and toenails
More than 1 million people are living with melanoma. The lifetime risk of the disease is highest in Caucasians (about 2.6%). The lifetime risk is lower among Black people (0.1%) and Hispanic people (0.6%).
Five to 10% of melanoma patients have a family history of the disease. People with at least one relative who had melanoma have a 2.2-fold risk of developing it.
Melanoma can be cured, especially when it’s caught and treated at an early stage. The five-year relative survival rate for patients with stage 0 melanoma is 97%. It drops to 10% in people with stage 4 (IV) melanoma.
Melanoma patients have a lifelong risk of developing new melanomas, especially if the melanoma was thick or had spread to nearby lymph nodes before treatment. Follow-up appointments with your dermatologist are essential.
Melanoma usually isn’t painful; only 3.7% of melanoma patients report pain according to one study. Squamous cell cancers and basal cell cancers are more likely than melanoma to hurt.
Melanoma can itch, but typically it doesn’t. Only 15% of melanoma patients report itching.
Some metastatic melanomas metastasize very quickly, while others take more than five years to spread. A notable exception is nodular melanoma, the second most common type of cutaneous (skin) melanoma, which can spread to vital organs within months of detection. The main sign of nodular melanoma is a firm bump or node that rises above the surface of the skin.
Melanoma risk factors include:
- Fair skin that tans poorly or burns easily
- Red or blond hair
- Blue or green eyes
- Having many moles or 10 or more atypical moles
- A history of sunburns or indoor tanning
- Blood relatives (parents, children, siblings, cousins, aunts, uncles) who have had melanoma
- Immune system weakness due to disease, organ transplant or medication
- A history of melanoma or other skin cancer
- Being age 50 or older
Dermatologists strongly encourage everyone, especially people who have one or more of these risk factors, to perform regular skin self-examinations. Self-exams can help people recognize any skin changes that could be cancerous.
An atypical nevus or mole, also called a dysplastic nevus, is a mole that looks different from other moles but is benign (not cancerous). Atypical moles may have some of the same ABCDE traits of melanoma. For instance, they may be larger than other moles or different in color. People with 10 or more atypical moles have 12 times the risk of melanoma according to the Skin Cancer Foundation.
Melanoma can develop in any mole, including an atypical mole. If your Water’s Edge dermatologist suspects that an atypical mole has become cancerous, he or she may perform a biopsy.
Signs of Melanoma
What does melanoma look like? That’s hard to answer because it can vary greatly in appearance. The ABCDE rules describe how melanoma often looks in the early stages. Melanomas tend to have one or more ABCDE traits, and some have several.
- A stands for ASYMMETRY. One half of the mole or spot doesn’t match the other half.
- B stands for BORDER. The mole or spot has an irregular, scalloped or poorly defined border.
- C stands for COLOR. The mole or spot is uneven in color and includes shades of tan, brown and black. There may be areas of white, red, pink, gray or blue.
- D stands for DIAMETER. Melanomas are usually larger than 6 millimeters (the size of a pencil eraser) when diagnosed, but they can be smaller.
- E stands for EVOLVING. The mole has changed in size, shape or color or a new lesion has developed.
When performing a skin self-exam, it’s helpful to keep in mind that normal moles are generally uniform in color, round to oval in shape and have a well-defined border. A skin care practitioner should examine all new growths and any mole that has one or more ABCDE traits.
Melanoma develops in an existing mole in just 20% to 30% of cases. When it does, the first sign is usually a change in the shape, color, size or texture of the mole. Other changes that could indicate melanoma include a mole that becomes painful or begins to bleed or itch.
In 70% to 80% of cases, melanoma arises as a new lesion. It most commonly appears on the head, neck or back (in men) and the back, arms or lower legs (in women), though it can appear anywhere.
When melanoma develops in people with dark skin, it often occurs in areas that get less sun, including the lower leg and the bottom of the foot or the palms (acral lentiginous melanoma).
Signs of subungual melanoma (nail melanoma) include dark brown or black vertical lines beneath the nail or a darker band of skin around the nail. The affected nail may start to separate from the nail bed or split down the middle.
Melanoma Treatment
Treatment typically begins with surgical removal of the melanoma and some normal-looking skin around the cancer (a safety margin). With early detection, surgical removal may be the only treatment required. When melanoma is limited to the epidermis (top layer of skin), the cure rate with surgical removal is close to 100%.
If testing indicates that the melanoma has metastasized to the lymph nodes or other areas of the body, treatment may include additional surgery to remove the cancer, immunotherapy, radiation therapy, chemotherapy or clinical trials. If the melanoma is advanced, the patient often receives a combination of treatments.
FOR ALL PATIENTS undergoing cryosurgery, biopsy or curettage and electrodessication:: Read this PDF for wound care instructions for cryosurgery (liquid nitrogen), biopsy, curettage and electrodessication (C&D) | (PDF is also available in Spanish.)
Understanding the Stages of Melanoma
Determining how far the cancer has spread is called staging. The melanoma stages are:
- Stage 0 melanoma (melanoma in situ): The melanoma is confined to the epidermis (top layer of skin).
- Stage 1 melanoma (stage I melanoma): The melanoma is confined to the skin and is no more than 2 millimeters thick; the skin may be intact or ulcerated, meaning the top layer of skin is absent.
- Stage 2 melanoma (stage II melanoma): The melanoma is confined to the skin and is more than 1 millimeter thick and may be thicker than 4 millimeters; the skin may be intact or ulcerated.
- Stage 3 melanoma (stage III melanoma): The melanoma has spread to one or more nearby lymph nodes or small areas of nearby skin.
- Stage 4 melanoma (stage IV melanoma): The melanoma has spread to internal organs, beyond the closest lymph nodes to other lymph nodes, or areas of skin far from the original tumor.
One way the melanoma stage is determined is by analyzing a tissue sample under a microscope. Sometimes a sentinel lymph node biopsy (SLNB) is performed. When melanoma spreads, it frequently travels to the closest lymph node, known as the sentinel node, first. Removing and analyzing that node helps doctors determine whether the cancer has spread.
One or more imaging techniques may also be used to determine if melanoma has spread beyond the original site. These include X-ray, ultrasound, computed tomography (CT), magnetic resonance imaging (MRI), positron emission tomography (PET) and radio-isotopic scans of the bones or organs.
Melanoma Prevention
Protecting your skin from UV radiation can reduce the risk of melanoma.
- Before going outside, generously apply a broad-spectrum, water-resistant sunscreen with a sun protection factor (SPF) of 30 or more to all exposed skin. Reapply approximately every two hours, even on cloudy days, and after swimming or sweating.
- Wear protective clothing, such as a long-sleeved shirt, pants, a wide-brimmed hat and sunglasses.
- Seek shade when possible.
- Protect children from UV exposure by dressing them in protective clothing, applying sunscreen and encouraging them to play in the shade.
- Use extra caution near water, snow and sand. These surfaces reflect the sun and increase the chance of sunburn.
- Get vitamin D through a healthy diet that may include vitamin supplements. Don’t try to get vitamin D from the sun.
- Avoid tanning beds. If you want to look like you’ve been in the sun, consider using a sunless self-tanning product, but continue to use sunscreen.
Learn More About Skin Cancer
Basal Cell Carcinoma (BCC) Skin Cancer Treatment in Florida
Basal cell carcinoma (BCC) is the most common form of skin cancer and is highly treatable when diagnosed early. At Water’s Edge Dermatology, our specialists provide comprehensive basal cell carcinoma treatment in Florida, offering both surgical and non‑surgical options based on the size, location, and behavior of the cancer.
What Is Basal Cell Carcinoma?
Basal cells line the deepest layer of the epidermis, which is the outermost layer of our skin. New skin cells are produced from basal cells. These new cells push older cells toward the skin’s surface, causing the old cells to die and slough off.
A mutation in the DNA of a basal cell causes it to multiply rapidly and continue growing when it would normally die. The accumulating abnormal cells may eventually form a cancerous tumor.
Basal cell carcinoma typically develops on sun‑exposed areas such as the face, scalp, ears, neck, and arms. While BCC rarely spreads to other parts of the body, it can grow deeper into surrounding tissue if left untreated, leading to functional or cosmetic damage.
Basal Cell Carcinoma FAQs
There are five warning signs that may signal the presence of BCC:
- An open sore that bleeds, oozes, or crusts and remains open for a few weeks, only to heal up and then bleed again. A persistent, non-healing sore is a common sign of an early BCC.
- A reddish patch or irritated area, frequently occurring on the face, chest, shoulders, arms, or legs. Sometimes the patch crusts and it may also itch. At other times, it persists with no noticeable discomfort.
- A shiny bump or nodule that is pearly or translucent and is often pink, red, or white. The bump can also be tan, black, or brown, especially in dark-haired people, and can be confused with a mole.
- A pink growth with a slightly elevated rolled border and a crusted indentation in the center. As the growth slowly enlarges, tiny blood vessels may develop on the surface.
- A scar-like area that is white, yellow, or waxy and often has poorly defined borders; the skin itself appears shiny and taut. This warning sign may indicate the presence of an invasive BCC that is larger than it appears to be on the surface.
A Water’s Edge Dermatology practitioner should examine all new growths and changes to your skin.
The most common cause of skin cancer of any kind is exposure to the sun or using commercial tanning beds. People who live in sunny or high-altitude climates are exposed to more UV radiation. Other risk factors include:
- Fair skin
- Blond or red hair
- Blue or green eyes
- Family history of skin cancer
- Weakened immune system
- Received radiation therapy
- Exposure to coal tar, pitch, creosote, or arsenic
- Age
Basal cell carcinoma usually develops over many years, although dermatologists are seeing more people in their 20s and 30s with it.
Only in exceedingly rare cases can BCC spread to other parts of the body and become life threatening, but it can invade and destroy surrounding tissue, causing permanent disfigurement.
When a BCC tumor develops near an organ such as an eye, ear, or nose, or grows near a nerve, this can be especially concerning. If the cancer invades, you could lose an eye. Early diagnosis and proper treatment can prevent this.
Diagnosis and Treatment of Basal Cell Carcinoma
A biopsy is required to diagnose skin cancer. A dermatologist in our office can perform this simple procedure by numbing the area and then removing the suspicious lesion (or a portion of it). The removed tissue is examined under a microscope to see if cancer is present. In some cases, the dermatologist might perform the biopsy and provide treatment during the same office visit.
When the diagnosis is BCC, Water’s Edge gives our patients a number of surgical and nonsurgical options. The appropriate treatment depends on the size, location, and characteristics of the tumor, as well as the overall health and needs of the patient.
Most BCCs are treated with one of the following:
Simple Surgical Excision
The Water’s Edge Dermatology provider cuts out the tumor and some of the surrounding healthy tissue. The removed tissue is examined under a microscope to see if all of the skin cancer has been removed.
Mohs Micrographic Surgery
Performed by a specially trained dermatologic surgeon, Mohs micrographic surgery involves removing the visible tumor and then successive layers of skin one at a time until cancer cells are no longer found.
Electrodesiccation and Curettage
Your Water’s Edge Dermatology provider removes the tumor by scraping or “curetting” it, and then burning the base with an electric needle (electrodessication).
Cryosurgery
Your Water’s Edge Dermatology provider destroys the tumor by freezing it with liquid nitrogen.
Electron Beam Therapy (EBT)
Electron Beam Therapy (EBT) is a specialized non‑surgical radiation therapy used to treat select basal cell carcinomas, particularly when surgery may be challenging or cosmetically concerning.
EBT uses a targeted electron beam to destroy cancer cells while minimizing exposure to surrounding healthy tissue. It is often recommended for BCCs located on the face, nose, ears, eyelids, or lips, or for patients who prefer a non‑surgical treatment option.
Learn more about Electron Beam Therapy for Skin Cancer.
Laser Surgery
High-intensity focused light waves are used to destroy the cancerous tissue.
Topical Therapy
Your Water’s Edge Dermatology practitioner prescribes a cancer-fighting medication, such as imiquimod or 5-fluorouracil, which you can apply to the skin cancer at home.
Photodynamic Therapy
A medication is applied to the skin and light is used to activate the medication. Learn more about photodynamic therapy (PDF) and what to expect.
Erivedge
Erivedge™ is a new treatment that is used in extraordinarily rare cases of metastatic BCC or locally advanced BCC that is life-threatening. Erivedge or vismodegib, is an oral drug that was approved by the FDA in early 2012 for advanced BCC. It’s only used for very limited circumstances where the nature of the cancer precludes other treatment options (such as surgery or radiation). Due to a risk of birth defects, Erivedge should not be used by women who are pregnant or attempting to conceive.
FOR ALL PATIENTS undergoing cryosurgery, biopsy or curettage and electrodessication:: Read this PDF for wound care instructions for cryosurgery (liquid nitrogen), biopsy, curettage and electrodessication (C&D) | (PDF is also available in Spanish.)
Who May Benefit From Non‑Surgical Basal Cell Carcinoma Treatment?
Non‑surgical treatments such as electron beam therapy, topical therapy, or photodynamic therapy may be considered for patients who:
- Have BCCs in cosmetically sensitive areas
- Are not ideal surgical candidates
- Have recurrent basal cell carcinoma
- Prefer to avoid surgery when appropriate
A dermatology evaluation is required to determine the safest and most effective treatment option.
Post-Treatment: What To Expect
After receiving treatment for BCC, the patient will schedule follow-up appointments. These appointments are essential because studies show that a person who develops BCC has an increased risk of developing another BCC or other form of skin cancer, including melanoma. Follow-up visits are also important because BCC can return after treatment. Cure rates and survival rates are highest with early detection and treatment.
Performing regular self-examinations of your skin can help detect skin cancer in its earliest stage. Be alert to non-healing sores and other changes to your skin.
Preventing Basal Cell Carcinoma
The most important thing you can do to reduce your risk of developing skin cancer of any sort is to avoid direct sunlight and tanning beds. When you do go out in the sun, wear protective clothing, hats, sunglasses, and sunscreen with an SPF of 30 or higher. Make sure to choose a broad-spectrum sunscreen and reapply every two hours or after swimming or sweating.
Here are a few other important reminders:
- Seek shade when appropriate – the sun’s rays are strongest between 10 am and 4 pm. If your shadow is shorter than you are, seek shade.
- Protect children from sun exposure by playing in the shade, using protective clothing, and applying sunscreen.
- Use extra caution near water, snow, and sand because they reflect the damaging rays of the sun, which can increase your chance of sunburn.
- Get vitamin D safely through a healthy diet. Don’t seek the sun.
- Avoid tanning beds. If you want to look like you’ve been in the sun, consider using a sunless self-tanning product, but continue to use sunscreen.
- Check your birthday suit on your birthday. Tell your Water’s Edge dermatologist if you see any new, unusual, or changing moles or growths on your skin.
- Regular, thorough skin examinations are also important, especially if you have a large number of moles or other risk factors. While this will not prevent skin cancer from developing, it may help to catch it early, when it can be treated more easily.
Learn More About Skin Cancer
Atypical Nevus
What Is an Atypical Nevus?
An atypical nevus, also called dysplastic nevus or atypical mole, is a benign mole that looks different. The word atypical means “not like the rest.”
Atypical moles are benign, but some people who have these moles have a higher risk of getting melanoma. The risk of getting melanoma increases significantly when a person with atypical moles has:
- Many atypical moles
- Had melanoma in the past
- A first-degree blood relative (parent, sibling, or child) who had melanoma
If a person has a few (one to four) atypical moles and none of the above risk factors, the increased risk of getting melanoma is small.
Atypical Mole FAQs
Atypical moles tend to vary in appearance. An atypical mole can be larger than other moles. Some are more than one color. Others have a jagged border. These traits also are warning signs of melanoma.
Your Water’s Edge Dermatology practitioner should examine all moles that show any of the following ABCDEs of melanoma:
- A stands for ASYMMETRY: One half is unlike the other half
- B stands for BORDER: Irregular, scalloped, or poorly defined border
- C stands for COLOR: The mole is varied from one area to another, with shades of tan, brown, and black; may also be white, red, or blue
- D stands for DIAMETER: While melanomas are usually greater than 6mm (the size of a pencil eraser) when diagnosed, they can be smaller
- E stands for EVOLVING: A mole or skin lesion that looks different from the rest or is changing in size, shape, or color
If a mole has any of these traits, it is important to see a Water’s Edge dermatologist. Other changes also should be reported, such as a mole that begins to burn or itch. The number of newly diagnosed melanomas continues to rise. With early detection and treatment, melanoma has a high cure rate.
Atypical moles usually begin to appear at or around puberty. These moles can appear in adults as well. While they can occur anywhere on the body, they most commonly develop on the trunk. Atypical moles rarely appear on the face but may develop on the scalp, head, and neck.
An atypical mole is not the same thing as a melanoma, so an atypical mole does not always need to be treated. If a dermatologist suspects that an atypical mole may be a melanoma, the dermatologist will remove the mole (or part of it) so that the mole can be examined under a microscope. This is known as a biopsy.
Because melanoma can develop within an atypical mole, anyone who has atypical moles should watch these (and all) moles for change. A mole can change in size, color, or shape. It can start to itch or burn. If a mole changes in any way, a Water’s Edge Dermatology practitioner should examine the mole.
xxx
xxxx.
Some people who have many atypical moles have Familial Atypical Multiple Mole Melanoma (FAMMM) syndrome. People with FAMMM syndrome have:
- A first-degree relative (parent, sibling, or child) or second-degree relative (grandparent, grandchild, aunt, or uncle) who has had melanoma
- A large number of moles, often more than 50, with some moles being atypical moles and the moles often varying in size
- Moles that show certain features when viewed with a microscope
- A person who has FAMMM syndrome should have a full-body screening from a Water’s Edge Dermatology practitioner every three to six months, beginning at puberty. Screenings may be less frequent once the moles appear stable.
Your Water’s Edge dermatologist also may recommend regular examinations from an ophthalmologist (eye doctor), skin photography, or regular screenings for relatives. All of these approaches help with early detection and treatment of melanoma. When detected and properly treated in the early stages, melanoma has a high cure rate.
People with FAMMM syndrome also should examine their own skin at least every three months and possibly more frequently. The purpose of this examination is to find the earliest changes to a mole.
What You Can Do: Prevention Tips
Sun exposure is the most preventable risk factor for all skin cancers, including melanoma. As unprotected sun exposure is thought to increase the number of moles, reducing sun exposure is an easy way to reduce your risk for skin cancer. Here’s how to protect adults and children from sun exposure by playing in the shade, wearing protective clothing, and applying sunscreen.
- Use extra caution near water, snow, and sand because they reflect the damaging rays of the sun, which can increase your chance of sunburn.
- Get vitamin D safely through a healthy diet that may include vitamin supplements. Don’t seek the sun.
- Avoid tanning beds. Ultraviolet light from the sun and tanning beds can cause skin cancer and wrinkling. If you want to look like you’ve been in the sun, consider using a sunless self-tanning product, but continue to use sunscreen with it.
- Check your birthday suit on your birthday. If you notice anything changing, growing, or bleeding on your skin, see a dermatologist. Skin cancer is very treatable when caught early.
Learn More About Skin Cancer
Atypical Fibroxanthoma
What Is Atypical Fibroxanthoma?
Atypical fibroxanthoma (AFX) is an uncommon skin cancer that most often appears on the head, ears or neck in the form of a red or pink bump. The lesions are typically small (1 to 2 centimeters in diameter) but often develop quickly. They usually aren’t itchy or painful. They can be crusty, scaly or broken open in the middle, and they may bleed.
AFX is thought to be caused by cumulative sun exposure and tanning bed use. It can also occur in people who have received radiation treatment.
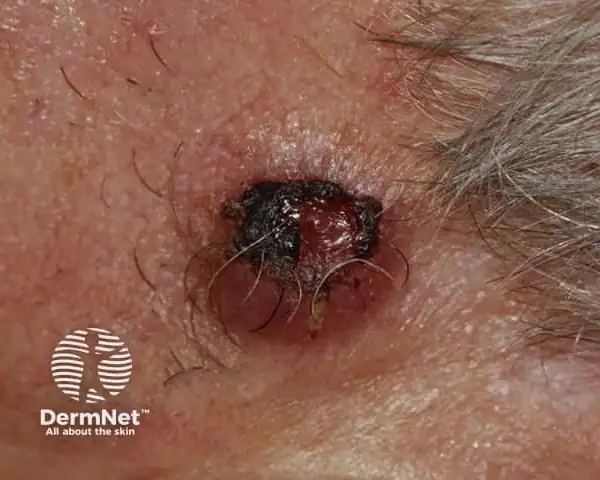
A crusted atypical fibroxanthoma (Credit: DermNet)
FAQs About Atypical Fibroxanthoma
AFX usually affects people with fair skin. It develops more frequently in people in their 70s and 80s and is more common in men than women. AFX is not hereditary.
People with AFX usually have an excellent outcome after treatment, though lesions re-grow in the same area in up to 10% of cases. It’s rare for AFX to spread to other parts of the body.
The best way to protect yourself from AFX is to practice sun safety.
- Use a broad-spectrum, water-resistant sunscreen with an SPF of 30 or higher every day. When outdoors, reapply sunscreen every two hours and after swimming or sweating.
- Avoid spending time in the sun between 10 a.m. and 2 p.m., when the sun’s rays are usually strongest.
- Wear sunglasses with UV protection, a wide-brimmed hat and sun-protective clothing, such as a long-sleeved shirt and pants.
- Do not use tanning beds.
- Schedule skin cancer screenings, especially if you’ve had any type of skin cancer in the past.
Atypical Fibroxanthoma Treatment
An AFX lesion is typically removed via surgery. The doctor may remove it surgically along with a small amount of surrounding tissue or remove it in stages using a technique called Mohs surgery. During a Mohs procedure, the doctor removes a small amount of tissue and examines it under a microscope to check for cancerous cells. That process is repeated until there are no cancerous cells present in the tissue removed. This procedure allows more healthy tissue to be spared, and scarring to be kept to a minimum. Depending on the amount of skin removed, a small skin graft may be necessary.