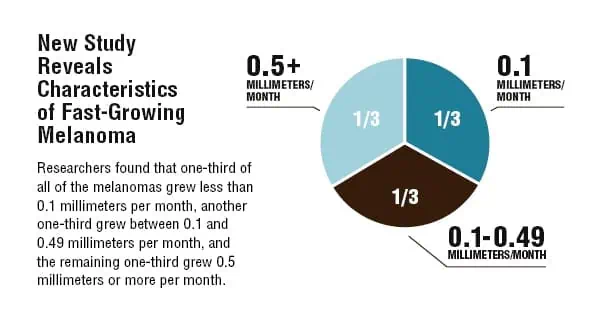
New Study Reveals Characteristics of Fast-Growing Melanoma
No matter what your past experience with skin problems may be, noticing a new growth on your skin is always a cause for concern, particularly if it is a fast-growing skin growth. Whether it looks more like a lesion or a rash, this change in your skin should be examined by the best rated dermatologist in your area immediately. However, this is especially true if the growth resembles an atypical nevus, one of the moles that can signal skin cancer. An Australian study recently revealed that certain characteristics may be a sign that melanoma will develop faster and may become fatal.
Melanoma is the most serious form of skin cancer, marked by the uncontrolled growth of pigment-producing cells. While an estimated one in every five Americans will develop skin cancer at some point in their life, people are more likely to develop melanoma if they have more than 50 moles, or if those moles are large or unusual. However, in an article published in the December edition of the Archives of Dermatology, researchers reported that these risk factors might not accurately determine who will develop fast-developing melanoma. Instead, their study showed that this potentially fatal situation could occur in anyone.
In the study, a team of dermatologists from Melbourne asked 404 patients with invasive melanoma and their families to recall when they first noticed a spot on their skin that eventually became melanoma, and when they saw that the mole had changed. The patients' skin was also examined, and the researchers collected additional data on demographics, skin cancer risk factors, tumor characteristics, and who had first detected the cancer. According to their research, the team determined that fast-growing melanoma is more likely to occur in those without large numbers of moles and freckles, especially the elderly. The moles that develop are more likely to be red than brown and black, symmetrical, elevated and symptomatic. Using their data to determine growth rates, the researchers also found that one-third of all of the melanomas grew less than 0.1 millimeters per month, another one-third grew between 0.1 and 0.49 millimeters per month, and the remaining one-third grew 0.5 millimeters or more per month.
The Australian report draws attention to an important fact about skin cancer and melanoma: anyone can develop these serious conditions, regardless of age, noticeable risk factors and other problems. For this reason, if you notice a fast-growing change in your skin, seek out the best rated dermatologist in your area for a diagnosis. Even if the problem is not melanoma, your health could still be at risk. By making an appointment at the best rated dermatologist clinic near you immediately, you can be sure that you will get the treatment and care you need before serious consequences take effect.
Three Ways Dermatology Might Change in the Future
Currently, millions of people around the world turn to dermatologist clinics to treat a variety of medical conditions and cosmetic concerns affecting their skin. Many of these patients may be seeking treatment for acne, an extremely common skin problem that can affect everyone from teenagers to the middle-aged and can typically be treated with a variety of acne treatment products and procedures.
Others, meanwhile, will seek care for conditions like skin cancer and psoriasis, which affect more than 9.5 million people in the United States. More people still will be interested in cosmetic procedures, such as hair loss treatments, a popular option for the more than 50% of men who will experience male pattern baldness by their 50th birthday. With the wide number of people who visit local dermatologists, it isn't surprising that the industry is constantly improving and expanding, offering more opportunities to patients and doctors alike.
However, this raises questions about what shape dermatology will take in the future. Will we all work with online dermatologists and give ourselves at-home laser acne treatments? Or will the traditional structure continue?
The American Academy of Dermatology (AAD) has some ideas. According to their magazine, Dermatology World, a number of changes are currently brewing in the industry that could mean serious changes for the future. Read on to learn how your trip to the dermatologist might differ in years to come.
Payment
While dermatology currently isn't covered under reforms like the Affordable Care Act, the skin care epidemic and other factors have made dermatology a target for changes in the way we pay for healthcare. While practices presently use a "fee for service" model, the AAD reports that a number of insurance companies and clinics have started considering value-based payment models, accountable care, and more. While it's impossible to guess which direction the industry will move in, a change in how you pay for your skin care is highly likely.
Online Services
At least one app already offers online dermatologists for conditions like acne, but most of the industry is more likely to begin offering online scheduling tools, improved communication methods, and an increased focus on telemedicine, which offers new opportunities for payment, prescriptions and more. In a few years, a patient who might be experiencing an allergic reaction to their medication might be able to video-chat with their doctor, be prescribed a different medication, and schedule a follow-up appointment in person in a matter of minutes, simply by using their smartphone or computer.
Treatments
One of the most exciting changes the dermatology industry is likely to see is the arrival of new tools, procedures, and treatment products. For example, photo recognition software might be used to better track patient progress and identify solutions to their skin problems. Additionally, research into the human genome and various skin conditions has the potential to create more targeted medications and better treatment regimens.
While it is impossible to predict the exact ways dermatology will change in coming years, there is no doubt that the industry will evolve and thrive to better meet the needs of patients. Whether that means switching to online dermatologists or simply improving payment methods, the potential benefits and opportunities are limitless. Are you ready for the skin care of the future?
Three Tips to Help Find the Best Dermatologist for You
If you are prone to acne outbreaks that can be difficult to treat and do not respond to acne treatment products, you are not alone: more than 85% of people will develop acne at some point in their lives, with more than 40 million Americans affected today. While acne and acne scarring are most common during adolescence, adults in their 20s, 30s, 40s and even 50s can develop the skin condition as well. If you have this common skin problem, you likely have heard that scientific research has lead to many new acne therapies and dermatologist acne treatments that may be able to help you. But how do you find the best rated dermatologist in your area, a skin specialist who will work with you to unveil beautiful, healthy skin? Read these tips to find out!
Know the Type of Dermatologist That Is Right for You
There are generally two types of skin specialists: general dermatologists and cosmetic dermatologists. Some practices will act as a combination of the two types, but the rest can often be easily classified by the services they offer. General dermatologists, for example, offer treatment for acne, rashes, hair loss and common skin problems, as well as skin maps to check for skin cancer. Cosmetic dermatologists, however, offer more advanced treatments for everything from deep-set wrinkles to severe acne, and typically use peels, injections and lasers to yield more dramatic results. Search for a dermatologist who offers the services you need.
Check Out Their Background
The best rated dermatologists often have a background that matches their skill level, so look at a dermatologist clinic's website to see how the specialist was trained and licensed. Keep an eye out for board certifications from the American Association of Dermatology (AAD), as well as a formal education in dermatology. Surprisingly, a high number of dermatologists originally studied other medical fields and only opened dermatology clinics to earn a profit, making them an inadvisable choice to help treat your skin.
Go In for a Consultation
Make an appointment to discuss your skin with a dermatologist at the practice. While it may be inconvenient, take it as a good sign if you have to wait a few weeks to see someone: this means that the services are trusted and therefore in high demand. At your appointment, ask lots of questions and listen carefully to how the dermatologist responds. What treatment do they recommend? Would they be conducting the procedure themselves, or merely supervising? While this consultation usually isn't free, it is extremely useful and the fee is typically put toward the cost of a procedure.
Whether you have acne, psoriasis, or another skin condition, finding the right dermatologist can have a significant effect on your self esteem, comfort and daily life. With the right treatment, you can reveal the beautiful, healthy skin you have always wanted. And by following the tips above, you can find a specialist who is not only the best rated dermatologist in your area, but also the best for you and your unique case.
Four Important Questions to Ask Before Choosing a Dermatologist
Skin conditions are an unfortunately common problem in the United States. Research shows that around 50 million Americans suffer from acne, 7.5 million Americans have psoriasis, and as many as one in five people will develop skin cancer over the course of their lifetime. To treat these conditions, many people will visit a dermatologist clinic for treatment over the course of their lives. But how do you find the best dermatologist for you? By asking these four questions, you can typically determine if a dermatologist has the expertise that you can trust, or if you would be better off choosing another doctor.
- Is there a doctor on site? The amount of time a doctor spends on site is regulated at the state level and differs accordingly. However, some dermatologists leave much of the day-to-day work to technicians. And while the technicians may be very qualified, the absence of a doctor leads to logical questions about the quality of the clinic's service, the treatment you will receive, and the trust you can place in the establishment.
- Is the doctor board-certified in dermatology? Shockingly, there is no law requiring that a doctor be certified or trained in dermatological medicine. And due to the high profits associated with cosmetic dermatology, some physicians set up dermatologist clinics without actual experience or knowledge of skin disorders. Whether you're interested in acne treatment products or treating skin cancer, these uncertified clinics do not deserve your trust or your business.
- How long have they been in business? While it may not be fair to assume that a new business might not have the expertise to properly treat skin disorders, research shows that many new dermatologist clinics and skin care centers fail after only a few years. The best dermatologists will have demonstrated excellent customer service and a proven ability to treat skin conditions, and will therefore have avoided this fate. Look for a clinic that has been in business for five or more years.
- Who will be performing the procedure? It is reasonable for experienced technicians to perform a number of fairly non-invasive treatments, such as laser acne treatment and laser varicose vein treatments. However, these technicians should be certified, trained and be able to prove their ability to successfully perform the procedure. And if the procedure is surgical in nature, it should be performed by a doctor.
Top 5 Tips for Fighting Toenail Fungus
Getting rid of a toenail fungal infection can be tough and it can take up to a year to achieve completely clear nails. A toenail fungus infection usually begins with swollen skin or pain around your nail, and you may notice dents, ridges or lines in your nails.
Your medical dermatologist will examine your nails and determine a treatment plan to help clear your toenail fungus. Here are five tips you can use to make your treatment plan even more effective:
- Keep your nails trimmed and filed to make sure you remove any fungus build up on your toenails. This helps keep the fungus from spreading.
- Follow your treatment plan. Missing oral treatments or skipping topical treatments prevent your treatment from working as well as it could.
- Ask your dermatologist if a nail lacquer, such as Penlac®, can help keep your toenail fungus infection from spreading. These nail lacquer treatments alone do not always clear infections, but they can aid your treatment plan.
- Keep your feet clean and dry to ensure the condition of your feet does not encourage fungal growth.
- Take steps to prevent future toenail fungus infections. In cases when patients do not continue to take steps for prevention, the nail fungus can return, according to the National Institute of Health.
If you are concerned you may have a toenail fungus infection, make an appointment with your Water’s Edge medical dermatologist today. He or she will take a culture of your nail and determine the best course of treatment for you. At Water’s Edge Dermatology, we have serious medicine for your skin.
Adult Dermatology: Changes in Aging Skin
We won’t stay young forever, but that doesn’t mean our skin can’t continue to look its best. Adult skin changes as it ages, and some of these changes are more obvious than others. The trick to keeping your skin looking healthy and young for longer is prevention. Your Water’s Edge adult dermatologist can help you stall some of the side effects of age. Here are the five most common effects of aging skin:
- Skin gets drier. Your skin produces fewer moisturizing oils as you age, so it’s important to protect your skin from losing moisture to wind, hot baths or the sun.
- Your skin begins to thin. Adult skin thins as you lose some of the fatty layer below your skin. Your skin cells regenerate more slowly and your collagen and elastin levels decrease as you age.
- Skin begins to sag. As your skin thins and you experience lymphatic drainage, gravity begins to pull on your skin. The decreasing levels of collagen and estrogen mean there is less structure for your skin as well.
- Age spots develop on exposed skin. Age spots are areas approximately the size of freckles. They are caused by melanin overproduction due to sun exposure.
- Wrinkles form and deepen. The most common causes of wrinkles are sun exposure, muscle and skin movement from facial expressions, slower skin cell regeneration and less collagen production. These are made more prominent by sagging skin.
Your skin is an indicator of your health, so keep it looking as good as you feel. Your adult dermatologist can treat dry and sagging skin, wrinkles and age spots. Make your appointment with a Water’s Edge dermatologist today and get serious medicine for your skin.
Treating Adult Acne
Acne is frequently considered a skin disorder of adolescents and teens. Unfortunately, acne can affect adults in their 20s, 30s and beyond. Many factors can contribute to the appearance of acne, including hormones, disorders of the hair follicles and infections. While there is no cure for acne, there are many effective ways to control and treat adult acne.
Adult acne can be divided in two groups of patients. The common acne in children can also occur in an adult, which is known as acne vulgaris. Another form of adult acne is known as acne rosacea. Acne rosacea is commonly recognized by the inflammation and redness of the face, but most often lacks the appearance of blackheads or open comedones.
Acne can be controlled with over-the-counter products as well as prescription medications. Establishing a skin care regimen with a dermatology provider can be very helpful in treating acne. Many treatments are available, including cleansers, topical treatment, oral antibiotic therapy, oral isotretinoin courses and even blue light therapy.
Starting with a mild antibacterial cleanser or benzoyl peroxide wash twice daily keeps the face and body clean and keeps oil to a minimum. Do not scrub the face and body clean as friction can increase the acne lesions.
Prescription treatments available for acne can be topical creams, gels or solutions. The topical medications can include one or more medications. Topical medications should be used consistently and as prescribed by your provider for best results. Topical treatments can be drying, so it is important to speak with your provider about adding a moisturizer or decreasing the frequency of use if this occurs.
Oral antibiotics can be used to treat acne and acne rosacea in adult patients. Oral antibiotic therapy can be given for short-term or long-term treatments, depending on the response to treatment and the medication prescribed by your provider. Low dose, long-term antibiotic therapy is available and effective for many patients.
Oral isotretinoin is an option for severe acne. It was previously marketed under the name Accutane but is available now in generic forms. This particular medication is available if other oral medications have failed. Isotretinoin is closely monitored by a program called iPledge. Blood work is monitored each month by your provider. Two forms of birth control must be in place for female patients as this medication can cause birth defects if pregnancy occurs during the time period the medication is being administered. This medication is generally given for a course of four to six months.
The most important key to the management of acne is to be consistent with your use of medication. Consistency is important.
Finally, even acne prone skin needs sunscreen each day. Finding a sunscreen that is oil-free and non-comedogenic is important. Please visit a Water’s Edge office for EltaMD Shield, which is a zinc sunscreen that is lightweight, absorbs completely and is great for oily skin types.
References: Acne (n.d.) American Osteopathic College of Dermatology. Retrieved from aocd.org.
How Dermatologists Help Treat the Symptoms of Serious Disease
If you have problem skin, it's likely that you have considered making an appointment with a skin dermatologist to discuss your treatment options. Currently, there are an estimated 7,575 dermatologist clinics in the United States, comprising an industry that has generated an estimated $11 billion in revenue. The dermatologists that work in these clinics are well-versed in providing care for a wide variety of aesthetic and medical skin conditions, from laser varicose vein treatments to different forms of treatment for melanoma skin cancer, and have the knowledge and experience to devise a plan for relieving your individual case or symptoms.
One of the most common skin conditions skin dermatologists treat is acne, which nearly 85% of people will experience at some point in their lifetime. Of this number, and estimated 40 to 50 million Americans are believed to suffer from this problem. Many people experience acne during their teenage years, with more than 40% of adolescents reporting acne or acne scarring by their mid-teens. However, people of all ages can be affected by this condition. Skin dermatologists can treat acne with a number of different methods; often, they will prescribe acne treatment products, procedures such as laser acne treatment, or even a combination of several of these options. Their diagnosis and prescription will depend on the severity of the acne, the afflicted areas of the skin, and the patient's overall health, as well as several other factors. For this reason, dermatologist acne treatments are often far more effective than common home treatments and drug store products.
Dermatologists also treat a number of more serious skin conditions, including skin cancer, which affects an estimated one in every five Americans at some point during their lifetime. There are several different treatments for skin cancer, with the most common being surgery and radiotherapy, though the procedure used will depend on the severity of the cancer and the patient. Skin dermatologists also often treat conditions that develop as a result of serious illness. Candida infections, for example, which can affect the patient's lungs and liver in addition to the skin, commonly develop in people with cancer, HIV, and other conditions that weaken the immune system. Likewise, Kaposi's sarcoma, dark or purplish lesions that form on the skin, form as part of the weakened immune caused by contracting the AIDS virus and can spread to the organs. Dermatologists are able to help treat these conditions when they manifest on the skin, reducing the patient's experience of the full extent of their sickness.
Skin dermatologists treat a wide variety of aesthetic and medical skin complaints every day, from performing laser hair removal to diagnosing a possible case of skin cancer and prescribing treatment if necessary. For this reason, if you have a problem with your skin, whether it is a case of acne or a Candida infection, a dermatologist may be able to help you. Contact a dermatology specialist in your area today to schedule an appointment.
Treatment Options for Eczema
If you or someone you know has eczema, you know it can be itchy, irritating and hard to manage. It often can feel like no matter what you do to get rid of it, the rash stays or keeps coming back.
Eczema often starts at a young age, with 10-20 percent of children diagnosed with the condition. While it can be lifelong, eczema tends to become less severe with age.
Unfortunately, there are not effective, easy, over-the-counter treatments for eczema. There are, however, tools dermatologists can use to appropriately diagnose and treat eczema.
Medical research continues to show that the most effective treatment plan involves treating the skin and making lifestyle changes.
Eczema Treatment Options
Your Water’s Edge Dermatology practitioner may recommend any number of combinations of the following options to manage your eczema:
- Corticosteroid or an immune-modifying medication, which can help reduce the inflammation and itch
- An antihistamine can improve eczema that’s triggered by allergies
- Antibiotics if there’s an infection, which is common
- Ultraviolet (UV) light therapy
Lifestyle Changes for Eczema
Talk to your Water’s Edge Dermatology practitioner before you implement any of these lifestyle changes:
- Frequently applying an appropriate moisturizer
- Avoiding certain clothing
- Using eczema-friendly bathing techniques
If you think you or a loved one has eczema, schedule an appointment to have your condition properly diagnosed and to begin the path toward relief.
When it Comes to Staph Infections, Prevention is the Key
Different varieties of Staphylococcus aureus bacteria, commonly called "staph," exist. “Staph infections” are common and a term I remember hearing since I was a child, so this is not something new. Staph bacteria are normally found on the skin and in the nose of about one-third of the population. The bacteria are generally harmless unless they enter the body through a cut or other wound, and even then they usually cause only minor skin problems in healthy people. However, Methicillin-Resistant Staphylococcus Aureus (MRSA) is different. MRSA infections are caused by a strain of staph bacteria that's become resistant to the antibiotics commonly used to treat ordinary staph infections.
Most MRSA infections occur in people with questionable immune function who have been in hospitals or other healthcare settings, such as nursing homes and dialysis centers. When it occurs in these settings, it's known as healthcare-associated MRSA (HA-MRSA). HA-MRSA infections typically are associated with invasive procedures or devices, such as surgeries, intravenous tubing or artificial joints.
Another type of MRSA infection occurs in the wider community — among healthy people. This form, community-associated MRSA (CA-MRSA), often begins as a painful skin boil. It's spread by skin-to-skin contact. At-risk populations include groups such as high school wrestlers, child care workers and people who live in crowded conditions.
Staph skin infections, including MRSA, generally start as small red bumps that resemble pimples or boils. It is not uncommon for the patient to suspect a spider bite. These can quickly turn into deep, painful abscesses that require surgical draining. In most situations, the bacteria remain confined to the skin. But in the case of the HA-MRSA, they can also burrow deep into the body, causing potentially life-threatening infections in bones, joints, surgical wounds, the bloodstream, heart valves and lungs.
Antibiotic Resistance
MRSA is the result of decades of unnecessary antibiotic use. For years, antibiotics have been prescribed for colds, flu and other viral infections that don't respond to these drugs. Even when antibiotics are used appropriately, they contribute to the rise of drug-resistant bacteria in part because they don't destroy every germ they target. In addition, patients who do not take their entire course of antibiotics also play a role in the emergence of these resistant strains. Bacteria live on an evolutionary fast track, so germs that survive treatment with one antibiotic soon learn to resist others.
Because hospital and community strains of MRSA generally occur in different settings, the risk factors for the two strains differ.
Risk Factors for HA-MRSA
- Being hospitalized. MRSA remains a concern in hospitals, where it can attack those most vulnerable — older adults and people with weakened immune systems.
- Having an invasive medical device. Medical tubing — such as intravenous lines or urinary catheters — can provide a pathway for MRSA to travel into your body.
- Residing in a long-term care facility. MRSA is prevalent in nursing homes. Carriers of MRSA have the ability to spread it, even if they're not sick themselves.
Risk Factors for CA-MRSA
- Participating in contact sports. MRSA can spread easily through cuts and abrasions and skin-to-skin contact.
- Living in crowded or unsanitary conditions. Outbreaks of MRSA have occurred in military training camps, child care centers and jails.
- Men having sex with men have a higher risk of developing MRSA infections.
When to See a Healthcare Professional
Keep an eye on minor skin problems — pimples, insect bites, cuts and scrapes — especially in children. If wounds become infected, seek medical care. Do not attempt to treat an MRSA infection yourself. You could worsen it or spread it to others.
What You Can Do
Create a list that includes:
- Detailed descriptions of your symptoms
- Information about medical problems you've had
- Information about the medical problems of your parents or siblings
- All the medications and dietary supplements you take
- Questions you want to ask the doctor
What to Expect During Your Visit
During your physical exam, your doctor will closely examine any skin lesions you may have. He or she might take a sample of tissue or liquid from the lesions for testing.
Both healthcare-associated and community-associated strains of MRSA still respond to certain antibiotics. In some cases, antibiotics may not be necessary. For example, your doctor, NP or PA may choose to drain a superficial abscess caused by MRSA rather than treat the infection with drugs.
Preventing HA-MRSA
In the hospital, people who are infected or colonized with MRSA often are placed in isolation as a precaution to prevent the spread of MRSA. Visitors and healthcare workers caring for people in isolation may be required to wear protective garments and must follow strict hand hygiene procedures. Contaminated surfaces and laundry items should be properly disinfected.
Preventing CA-MRSA
Wash your hands. Careful hand-washing remains your best defense against germs. Scrub hands briskly for at least 15 seconds, then dry them with a disposable towel and use another towel to turn off the faucet. Carry a small bottle of hand sanitizer for times when you don't have access to soap and water.
Keep wounds covered. Keep cuts and abrasions clean and covered with sterile, dry bandages until they heal. The pus from infected sores may contain MRSA, and keeping wounds covered will help keep the bacteria from spreading.
Keep personal items personal. Avoid sharing personal items such as towels, sheets, razors, clothing and athletic equipment. MRSA spreads on contaminated objects as well as through direct contact.
Shower after athletic games or practices. Shower immediately after each game or practice. Use soap and water. Don't share towels.
Sanitize linens. If you have a cut or sore, wash towels and bed linens in a washing machine set to the hottest water setting (with added bleach, if possible) and dry them in a hot dryer. Wash gym and athletic clothes after each wearing.
Most patients have come to know and often fear the term MRSA. However, when these infections are encountered the general community, in patients who are otherwise healthy, there is little to fear. Your healthcare provider will know exactly how to manage your condition and you are sure to recover without complication. Even so, it is still good behavior to practice the sound preventive measures we discussed above.