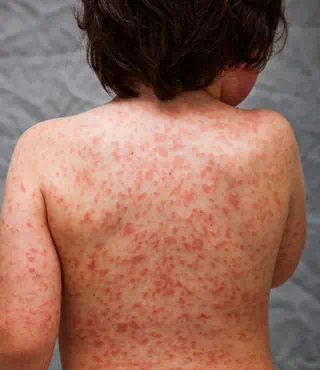
Photo credit: Kawasaki Disease Foundation
Children have largely been spared during the coronavirus pandemic — the virus has mostly struck adults. But recently, alarming images of kids in hospital beds, their skin splashed with red blotches, have peppered the nightly news. The rashes stem from a rare inflammatory disease called pediatric multi-system inflammatory syndrome (PMIS), also known as multisystem inflammatory syndrome in children (MIS-C), possibly brought on by COVID-19. The rashes are similar to those seen in Kawasaki disease, another rare illness that occurs in children.
Ted Schiff, MD, founder and chief medical officer of Water’s Edge Dermatology, weighed in on what parents need to know.
What is PMIS?
PMIS is an inflammatory condition similar to Kawasaki disease. The causes of Kawasaki disease are unknown, but it may in some cases be triggered by an infection, such as a viral infection. “We believe it occurs due to an overreaction by the immune system,” said Dr. Schiff.
That overreaction leads to excessive inflammation throughout the body, including in small blood vessels. “When these blood vessels are compromised by inflammation, they become ‘leaky,’” said Dr. Schiff. As blood seeps through a vessel wall, it causes a reddish rash. Left untreated, Kawasaki disease can lead to serious heart problems.
RELATED: Skin Rashes and Purple Spots: Symptoms of the Coronavirus?
PMIS involves many of the same symptoms, but there are important differences. “Kawasaki disease is usually mild to moderate in severity. People generally don’t die of it,” said Dr. Schiff. “By contrast, PMIS seems like a much more serious disease at this point.”
While Kawasaki’s typically strikes kids younger than 5, children who develop PMIS tend to be older; some are teenagers. Patients may exhibit signs similar to those seen in toxic shock syndrome, including dangerously low blood pressure and damage to the heart and kidneys.
What is the prognosis for PMIS?
PMIS is rare, and though several children have recently died from it, most children who develop it recover with proper treatment. Doctors have found that many respond well to a Kawasaki disease treatment called intravenous immunoglobulin, which calms an overactive immune system. Aspirin and steroids appear to improve symptoms, too.
Knowing how to spot the rash can help ensure that a child with PMIS gets the urgent care needed.
What are the signs and symptoms of PMIS?
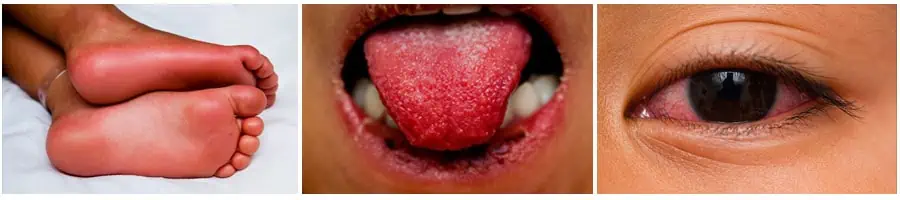
Signs and symptoms of PMIS can develop very quickly. The rash can appear anywhere, including the face, but it most often appears on the trunk, arms and legs. It usually spreads across a wide patch of skin and may be flat and have a mottled appearance or take the form of small red bumps. The rash may be accompanied by persistent fever, cracked lips, a “strawberry” tongue (red, swollen and bumpy), red eyes and swollen hands and feet.
Children with PMIS may also experience fatigue and gastrointestinal problems, such as stomach pain, vomiting and diarrhea. Fewer than half of PMIS patients have respiratory symptoms, such as shortness of breath, which are a hallmark of COVID-19 in adults. For some reason, noted Dr. Schiff, there have been very few if any reports of PMIS in Asia.
“COVID-19 is a mysterious disease, but we’re learning more about it every day,” he said.
Experts believe PMIS can occur weeks after a COVID-19 infection, which may go unnoticed.
If your child develops a rash that is accompanied by other PMIS symptoms, such as a fever or abdominal pain, contact a pediatrician or dermatologist right away. If the symptoms seem severe, seek medical help immediately.
To schedule an appointment with a Water’s Edge Dermatology provider, call (877) 544-3880 or book online. TeleDerm virtual visits are also available. Book a virtual online appointment here.
Article Written By: Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.
Medical Review By: Ted Schiff, MD





