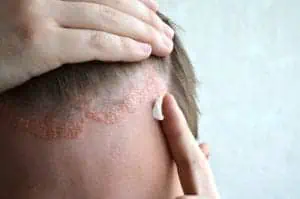
Itchy, flaky scalp? It could be dandruff — or scalp psoriasis, a form of plaque psoriasis, caused by an overactive immune system that makes skin cells grow too quickly.
Much like plaque psoriasis elsewhere on the body, psoriasis on the scalp typically appears in the form of reddened plaques covered with silvery scales, though the scales are often thickened and even itchier.
“Scalp psoriasis is usually very scaly, and there can be caking of the hair and even some hair loss,” said Dr. John Minni, a board-certified dermatologist at Water’s Edge Dermatology who is also board certified in family practice.
About half of people with psoriasis will have psoriasis on their scalp at some point. Still, because scalp psoriasis can look like other scalp conditions — and sometimes exist at the same time — it can be hard to diagnose.
Is it psoriasis or seborrheic dermatitis?
Psoriasis on the scalp can look and feel a lot like seborrheic dermatitis, which causes dandruff. Seborrheic dermatitis inflames skin on the scalp and can cause redness, itching, scales and flakes. But there are some differences that can help you and your dermatologist tell them apart.
The location
The first difference is where on the scalp the problem occurs. “Seborrheic dermatitis is often scattered throughout the whole scalp,” said Dr. Minni. “It fades in and out of the skin across the whole scalp.” Scalp psoriasis, by contrast, tends to have a clear beginning and end.
Scalp psoriasis is also more likely to appear beyond the hairline — on the neck or forehead or behind (or even in) the ears.
The scales
Psoriasis patches are often drier than the greasy scales common with seborrheic dermatitis. They may also be more tender and itch more. If you scratch or pick at psoriasis scales, you may experience bleeding.
“Seborrheic dermatitis is generally a lot less inflamed and is often less scaly,” Dr. Minni said. “You’re more likely to have a dusting of flakes rather than the large flakes that can happen with psoriasis.”
Your skin elsewhere
It’s rare for people to have psoriasis only on their scalp. If you don’t have psoriasis somewhere else on your body, your scalp issues are most likely to be seborrheic dermatitis.
People can also have sebopsoriasis, a mix of both conditions. Sometimes dermatologists can’t tell where one condition ends and the other begins, even when they test a sample of skin.
Scalp psoriasis treatment
Whether you have pure scalp psoriasis or a mix of conditions, treatment often involves a combination of therapies. Dr. Minni usually begins with a potent foam or liquid corticosteroid. These steroids can quickly reduce scalp inflammation as well as redness, itching and scaling.
Along with topical steroids, Dr. Minni may recommend a medicated shampoo that contains coal tar or salicylic acid. Coal tar can reduce itching, while salicylic acid softens and helps lift away thick scales so it’s easier for steroids to reach the scalp. He uses a similar combination of treatments for sebopsoriasis.
These treatments don’t always work well enough to control symptoms, which can have a huge effect on a person’s quality of life. When topical treatments aren’t sufficient or scalp psoriasis is severe, Dr. Minni often turns to oral medicines, such as methotrexate, that tamp down immune system activity. For other patients, biologics are the answer. These are more powerful, highly targeted and given by injection or infusion.
Dr. Minni advises his patients not to scratch or pick at their scalp psoriasis. “Every time you scratch scalp psoriasis, you can actually make more psoriasis through a process called the Koebner response,” he explained.
If your scalp is itchy and scaly, getting an accurate diagnosis from a dermatologist is the first step to finding relief.
“Scalp psoriasis can be very frustrating for patients, but we can usually bring it under good control with the right therapies,” said Dr. Minni.
Article WrittenBy: Emily Delzell, a freelance health and medical journalist based in Birmingham, Alabama.
Medical Review By: John Minni, DO