 Medical Review By: Luke Maj, MD, MHA
Medical Review By: Luke Maj, MD, MHA
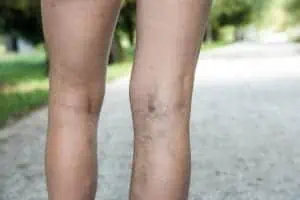
Does diabetes cause varicose veins? If not, is there a connection between varicose veins and diabetes?
It’s true – diabetes can affect the whole body. High blood sugar that builds up in the blood can damage organs and weaken blood vessels. The lining of the blood vessels can become damaged, and that paves the way for plaque to form. It’s one reason people with diabetes are prone to peripheral artery disease, which can cause leg pain when you walk.
While diabetes doesn’t cause varicose veins, being overweight increases the risk for both conditions. And diabetes could indirectly make varicose veins more likely.
Some people with diabetes develop chronic venous insufficiency (CVI), which increases the risk for varicose veins. In CVI, the tiny one-way valves in the leg veins don’t work properly, which means blood traveling back to the heart from the legs can succumb to gravity and pool in the veins. This can weaken and stretch the veins and cause leg pain, cramps and swelling.
Being overweight and having high blood pressure or poor circulation, as many people with diabetes do, seem to make CVI more likely.
Are varicose veins a sign of diabetes?
Varicose veins are not a sign of diabetes. The same holds true with spider veins, which are also caused by weak valves. Varicose veins and spider veins are complex conditions with many contributing factors, including age, genetics and hormonal changes. Women develop them more often than men.
Still, if you notice varicose veins forming, it’s a good time for a checkup. Since varicose veins can be brought on by CVI, which is linked to diabetes, your doctor may want to check your blood sugar levels.
Treating varicose veins
It’s important to see a vein specialist about your varicose veins, which can worsen if left untreated and cause increasing pain. Blood clots are another possible complication. In addition, leg sores called venous ulcers can form near the veins. In people with diabetes, nerve damage and poor circulation can make it harder for these ulcers to heal and more likely for them to become infected.
Both varicose veins and spider veins are treatable. Treatment options include foam sclerotherapy, which involves injecting an irritant into the vein to destroy it.
Preventing varicose veins
Many of the best practices for managing diabetes can also help keep leg veins healthy and keep blood flowing back to the heart.
- Don’t smoke. Smoking damages the lining of blood vessels. One study found that people who smoke a pack or more of cigarettes a day are nearly 2.5 times more likely than nonsmokers to develop CVI.
- Eat a balanced diet. Include plenty of fruits and vegetables in your diet, which promote good circulation and help protect the veins.
- Watch your weight. Losing weight if you need to can improve symptoms of varicose veins, not to mention reduce the risk of developing diabetes. If you have diabetes, losing weight can improve your blood sugar levels.
- Get moving. Standing or sitting in one place for too long can contribute to varicose veins. Experts suggest moving around at least every half hour or so. Regular exercise promotes healthy circulation.
- Drink plenty of water. Staying well hydrated helps keep your blood flowing better. Keep in mind that unquenchable thirst is a possible sign of poorly controlled diabetes.
- Take your medicine. Taking your diabetes medication as directed helps protect your veins from the damage high blood sugar can cause. If you happen to take the widely prescribed diabetes drug metformin, you may get a bonus: One study found that people who took metformin for type 2 diabetes reduced their risk for varicose veins by 44 percent.
Early detection and early treatment of CVI or vein disease is best practice for improved circulatory health and preventing future complications especially in diabetics.
Article Written By: Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.





