Medical Review By: Luke Maj, MD, MHA
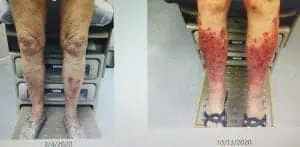
Red/brown patches or visible veins on your legs? It’s tempting to dismiss them as age-related cosmetic concerns, no worse than a few wrinkles on your face or a bald spot on your head. But they may be symptoms of vein disease in the legs — specifically, symptoms of chronic venous insufficiency — and ignoring them now could land you in hot water later on.
Unfortunately, some people with early signs of chronic venous insufficiency (CVI) put off treating it, said interventional radiologist Luke Maj, MD, director of The Vein Center at Water’s Edge Dermatology.
“We explain to the patient that this is a medical issue,” said Dr. Maj. “But some patients don’t believe us. They say, ‘It’s probably nothing.’” Invariably, the next time Dr. Maj sees one of those patients, their condition has worsened.
What is chronic venous insufficiency?
In CVI, the valves in the leg veins that keep blood moving back to the heart don’t work properly. As a result, instead of flowing up to the heart, the blood flows back down the legs and pools in the veins. Some people inherit faulty veins, but CVI can also develop as a result of deep vein thrombosis (DVT) – in layman’s terms, a blood clot in the leg. If you are obese, sedentary, over the age of 50 or female, your risk of CVI is increased.
Over time, pooled blood in the legs can lead to a host of problems in the lower legs, including:
- Aching
- Swelling
- Itching or numbness
- Painful cramps
- A heavy sensation
- Varicose veins and spider veins
- Reddish patches or reddish skin that may become brownish as the condition worsens
- Leg wounds, also known as venous ulcers
Benefits of early treatment
Treating CVI early on can help you feel significantly better and also prevent leg ulcers. These open sores can be extremely painful and difficult to treat. Once treated, they take months to heal.
Treatments for CVI improve the skin’s appearance (though in some cases, skin discoloration is permanent) while relieving aches and other symptoms. It may take several weeks or months to see the full benefits, but you’ll likely notice a difference much sooner.
“I feel better already,” one patient told Dr. Maj the day after having one of her legs treated. “I have more spring in my step!”
CVI treatments
To diagnose CVI, doctors use ultrasound imaging to look for faulty valves and blood flowing the wrong way. If you have CVI or suspected CVI, the doctor will likely prescribe compression socks or stockings while you decide on a treatment plan. For some patients, compression wear alone may be enough to manage symptoms, though these garments can be a tough sell in warm climates, noted Dr. Maj.
Minimally invasive surgery can close a bad vein permanently and get you back on your feet quickly. Doctors often zap the vein shut using heat in the form of radio waves (radiofrequency ablation, or RFA) or light (endovenous laser treatment, or EVLT). Dr. Maj uses both approaches but says RFA tends to cause less post-procedure pain and bruising.
Another option is sealing the vein with a glue-like adhesive called VenaSeal. According to Dr. Maj, VenaSeal is considered an implant as it remains in the patient’s body, but treatment works as well as RFA and EVLT. In rare cases, patients have a bad reaction to the adhesive, which then has to be surgically removed.
In sclerotherapy, the doctor injects a chemical into the vein that damages the lining, causing the vein to collapse. Dr. Maj uses sclerotherapy mainly to treat varicose veins and spider veins.
No matter what course of treatment you and your doctor choose, the key is to listen to your doctor’s recommendation and take action when advised. Like wrinkles on your face, symptoms of vein disease in the legs won’t go away on their own. Unlike wrinkles, they can affect not just your looks but your quality of life.
Article Written By: Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.





