Medical review by Ted Schiff, MD
Sunburns are a summer bummer, but they’re hardly the only annoying skin problem that can crop up after fun in the sun. Spending more time outdoors, decked in shorts or a swimsuit, increases your odds of developing a variety of summer skin rashes, from heat rash to folliculitis to swimmer’s itch.
Here are 10 skin rashes to watch for.
1. Heat rash, aka prickly heat
Perspiring helps cool down your body when the mercury hits “sweltering,” but heavy-duty sweating can cause prickly heat, which doctors call heat rash. It occurs when sweat glands get clogged. The result is reddened skin and, in most cases, itchy, blister-like bumps. The rash may sting or tingle. Chilling out in a cool room and keeping your skin dry can help relieve heat rash.
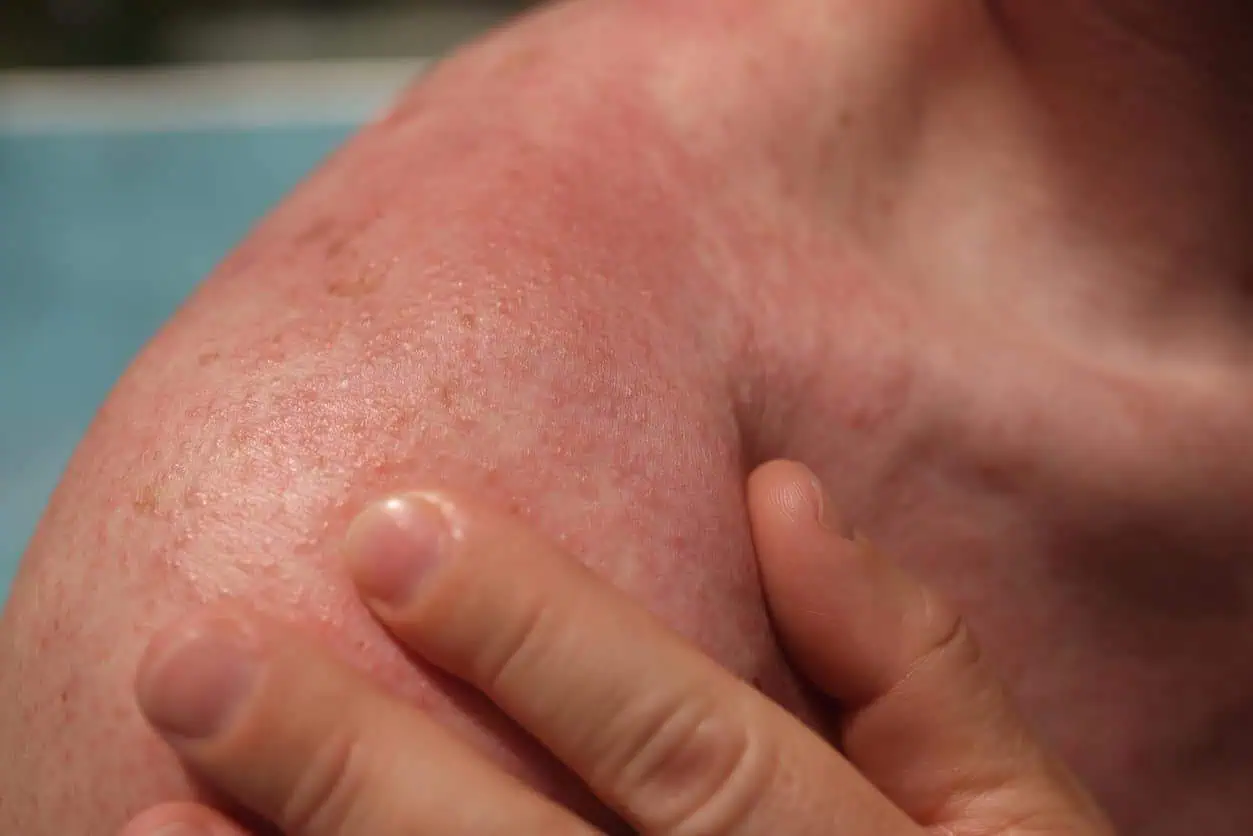
2. Photosensitivity
Certain drugs, health conditions and skin care products can make the skin more sensitive to UV rays. In people with photosensitivity, spending time in the sun may trigger a reaction that looks (and feels) like a bad sunburn or a rash.
Lupus is one condition that can trigger photosensitivity. Retinols, benzoyl peroxide and vitamin C are some of the skin care ingredients that can do the same. Among the oral medications that can lead photosensitivity are hydroxychloroquine and certain:
- Antibiotics, such as doxycycline and tetracycline
- Nonsteroidal anti-inflammatory drugs, such as ibuprofen and naproxen
- Anti-arrythmia drugs
- Antifungals
- Retinoids
- Diuretics
- Statins
- Antihistamines
If your skin blisters or you develop a fever or other flu-like symptoms, see your doctor.
The best way to avoid a bad reaction to the sun is to stay out of it or cover up. If you do expose your skin to the sun, be sure to wear a broad-spectrum sunscreen with an SPF of at least 30.
3. Folliculitis
Every hair on your body sprouts from a tiny structure called a follicle. Wearing tight clothes on a hot day or sitting in a hot tub can damage thefollicles, making it easier forbacteria or fungi to enter and cause an acne-like rash that may itch or hurt. You can get folliculitis any time of year, but your skin is particularly vulnerable when it’s hot and damp. Choose loose-fitting clothes to reduce your risk.
4. Athlete’s foot
There’s nothing like hanging around a pool on a hot summer day, but beware that a microscopic fungus that causes athlete’s foot can lurk on surfaces around the water, as well as the floors of changing rooms and showers. Athlete’s foot causes a red, itchy, scaly skin rash on the feet, often between the toes, and can spread to other body parts. A related problem, jock itch, is more common in warm weather, too.
Wear flip-flops to avoid athlete’s foot, which responds well to anti-fungal treatments. To help prevent jock itch, shower after working out or sweating, wear boxers instead of briefs, change your underwear during the day if you sweat a lot, avoid staying in a wet bathing suit and dry your groin before drying your feet so the towel doesn’t spread foot fungus to your privates.
5. Melasma
Melasma isn’t really a rash, but it’s a skin condition that can worsen from spending too much time in the sun. It occurs when the cells that give skin its color, called melanocytes, make too much pigment. The result is dark patches, usually on the face. Melasma mostly affects women.
If you have melasma, stay in the shade as much as possible, and wear sunscreen (SPF 30 or higher) and a wide-brimmed hat when you go in the sun.
6. Poison ivy rash
Within a few hours or days of a too-close encounter with poison ivy — or one of its evil cousins, poison oak and poison sumac — you can develop a red rash that is unbearably itchy and may blister. Cold compresses, hydrocortisone cream, calamine lotion and oral antihistamines can help with the itching. If you have a severe case of poison ivy rash, your dermatologist might prescribe a stronger corticosteroid cream.
See a doctor if you develop a fever or you can’t sleep because of the discomfort, or if the rash doesn’t fade after seven to 10 days or begins oozing pus.
Learning to recognize these poisonous plants can spare you a lot of misery.
7. Polymorphic light eruption
Polymorphic light eruption (PLME), also called polymorphous light eruption, can cause a variety of skin symptoms, including reddening, tiny bumps, eczema-like dry patches, blisters, and welts similar to hives. No one knows what causes it, but symptoms are triggered by sun exposure, so protect your skin when you’re outdoors. The skin usually clears up on its own over time, but topical or oral corticosteroids prescribed by your dermatologist can help.
8. Sea bather’s eruption
Plunging into the ocean or the local swimming hole is a great way to cool off on sweltering days, but tiny critters in the water can leave you with an itchy rash after your dip. Sea bather’s eruption, aka sea lice, is caused not by sea lice (despite its nickname) but by the larvae of thimble jellyfish or a certain type of sea anemone. These larvae get trapped under your bathing suit. Once there, they release toxins that cause a tingly, itchy rash. The rash gets worse when you take a shower or rub your skin with a towel.
Some doctors recommend applying diluted vinegar or rubbing alcohol for relief. Cool compresses and over-the-counter hydrocortisone cream can also help.
RELATED: 6 Common Water Rashes and How to Treat Them
9. Swimmer’s itch
A swim in the lake is a summer highlight for kids, and plenty of adults, too, but if the water is contaminated with microscopic parasites released by infected aquatic snails, you could break out all over in small, reddish pimples within a day. The pimples may turn into small blisters. Your skin might tingle, burn or itch. The same parasites can contaminate salt water, too. Shallow water near the shoreline is more likely to contain them than deeper water.
Cool compresses, hydrocortisone cream, colloidal oatmeal baths and oral antihistamines are among the remedies that can help relieve swimmer’s itch.
10. Solar urticaria
Just a short spell under the sun can cause people with this rare condition, a form of sun allergy, to develop hot, itchy skin and welts that resemble hives. (“Urticaria” means hives.)
Solar urticaria is more likely to flare up in the summer, when you start wearing shorts, tank tops and bathing suits. That’s because it tends to affect skin that’s normally covered, though even covered skin may react. In some cases, solar urticaria can cause other symptoms, such as light-headedness and vomiting. The good news: Symptoms begin to fade when you take cover. Stay out of the sun until they clear.
If you think you may have solar urticaria, talk to your dermatologist about treatments that can help manage it.
Written by Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.