Athletes
Foot
Call (877) 900-3223
Athlete’s Foot: Causes and Symptoms
Overview
What is Athlete’s Foot?
Symptoms of Athlete’s Foot
Causes of Athlete’s Foot
Treating Athlete’s Foot
Preventing Athlete’s Foot
Overview
Athlete’s foot, also called tinea pedis, is the most common type of fungal infection. It can affect any boy, girl, man, woman, athlete, or couch potato. It’s contagious, too, which means that being aware of how it spreads could reduce your chances of getting it. The medical dermatologists at Water’s Edge Dermatology can help diagnose and treat athlete’s foot.
What is Athlete’s Foot?
Athlete’s foot is an infection caused by a group of mold-like fungi called dermatophytes. These tiny organisms are everyday residents in our skin, but their growth is kept in check when the skin is clean and dry. It’s when the skin stays moist for too long in tight spaces (like shoes) that those dermatophytes wake up with expansion on their mind. If your socks and shoes remain damp for too long, it can create a favorable atmosphere for the growth of fungi.
Another type of fungal infection could mimic athlete’s foot, so if you have thick, crumbling nails that separate from the nail bed, schedule an appointment with your Water’s Edge Dermatology practitioner to diagnose the problem. He or she will also check for eczema or psoriasis, as those can look a lot like athlete’s foot.
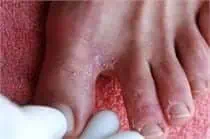
Symptoms of Athlete’s Foot
The symptoms of athlete’s foot include itching, burning, stinging, and flaking between your toes. Another common signal is a red rash. You could also have itchy blisters or excessive dryness on the bottoms or sides of your feet, including cracking of the skin. Toenails that are thick, crumbly, ragged, discolored, or pulling away from the nail bed are another indication that you may have athlete’s foot.
You probably won’t have all of the symptoms, which most commonly occur between the toes. Onychomycosis, a fungal infection of the nail, may develop with or without other signs and symptoms of athlete’s foot.
Causes of Athlete’s Foot
Athlete’s foot is closely related to other fungal infections, including ringworm and jock itch. A group of mold-like fungi called dermatophytes causes these infections. These microscopic organisms are normal inhabitants of your skin, and their growth stays in check as long as your skin is clean and dry. However, dematophytes thrive in damp, close environments.
Athlete’s foot thrives in thick, tight shoes that squeeze the toes together and create warm, moist areas between them. Damp socks and shoes and warm, humid conditions also favor the organisms’ growth. Plastic shoes, in particular, provide a welcoming environment for fungal growth and infection.
Athlete’s foot is contagious and can be spread by contact with an infected person or with contact with contaminated surfaces, such as towels, floors, and shoes.
Risk factors
You are at higher risk of athlete’s foot if you:
- Are a man
- Frequently wear damp socks or tight fitting shoes
- Share mats, rugs, bed linens, clothes or shoes with someone who has a fungal infection
- Walk barefoot in public areas where the infection can spread, such as locker rooms, saunas, swimming pools, communal baths and showers
- Have a weakened immune system
Treating Athlete’s Foot
While most cases of athlete’s foot can be controlled with over-the-counter remedies, usually in the form of sprays, creams, or powders, severe cases should be treated by a Water’s Edge Dermatology practitioner. He or she can prescribe a prescription-strength topical or oral medication.
If your athlete’s foot recurs frequently, your dermatologist may recommend that you stay on medication for a long period of time. Let them know about all the medications you’re taking because of potential interaction complications.
Complications
If athlete’s foot goes untreated, a secondary infection can occur where bacteria cause tissue breakdown. If this happens, the skin between your toes erodes, which can be very painful. An allergic response that causes blistering on your hands, fingers, and toes could also occur. Doing something about athlete’s foot before it gets to the toenails is crucial because once it’s there, it’s difficult to eliminate.
Preventing Athlete’s Foot
Preventing athlete’s foot starts in your own environment. If you exercise in sneakers, chances are your socks get moist. Remove them as soon as you can and wash and dry your feet. Drying out your feet is the best thing you can do to prevent athlete’s foot.
If you wear the same pair of shoes every day, you’re at greater risk because your shoes don’t have the chance to get totally dry, so you’re slipping your feet into an environment well suited for fungi. If you have a great pair of shoes that actually breathe, then this isn’t a problem.
Here are a few more tips:
- Choose natural materials. Wear socks made with natural material, like cotton, or a synthetic fiber designed to draw moisture away from your feet.
- Change socks and stockings regularly. If your feet sweat a lot, change your socks twice a day.
- Wear light, well-ventilated shoes. Avoid shoes made of synthetic material, such as vinyl, plastic, or rubber.
- Protect your feet in public places. Wear waterproof sandals or shower shoes in communal showers, pools, fitness centers, and other public areas.
- Treat your feet. Use powder, preferably antifungal, on your feet daily.
- Don’t share shoes. Sharing risks spreading a fungal infection.
- Don’t share towels. If you wipe with an infected towel, the fungus could spread to you.