PRP for Hair Loss: Does It Work?
Medical Review By: Emmanuel Loucas, MD
If you’re losing your hair, you may think your choices are Rogaine, a hair transplant or lifelong embarrassment. But there’s another option, called platelet-rich plasma (PRP) therapy, which can help trigger new hair growth. PRP therapy has been used since the 1970s to help athletes heal from injuries, but health practitioners have discovered it can also treat a variety of other issues, including hair loss.
“PRP therapy isn’t a magic cure for hair loss, but it can be very effective in certain people, particularly when it’s used with other treatments such as Rogaine and Propecia,” said Emmanuel Loucas, MD, a board-certified dermatologist at Water’s Edge Dermatology who specializes in PRP therapy.
What is PRP therapy?
PRP therapy is a series of injections of platelet-rich plasma taken from your own blood. (Platelets are cell fragments that are essential to blood clotting. Plasma is a yellowish liquid that makes up about half of a person’s blood volume.) Platelet-rich plasma contains proteins called growth factors that stimulate the growth of tissue. It’s believed that these growth factors, when injected in the scalp, are what trigger new hair growth.
“Your hair follicles don’t die when you lose hair, so the goal of most available hair loss treatments is to reactivate them,” Dr. Loucas said. “PRP therapy is another method of ‘waking up’ the hair follicles so they’ll function properly again.”
What the treatment entails
When you arrive at your appointment, the doctor will draw about 1 to 2 ounces of blood by placing a needle in your arm. The needle contains a small amount of an anticoagulant to prevent clotting. It can cause a brief stinging sensation, Dr. Loucas said.
Next, the doctor will place your blood in a centrifuge to separate out the plasma. The plasma is then injected in multiple locations on your scalp. Patients usually need 40 to 50 injections per session.
“I know that sounds painful and a little scary, but your doctor will numb the area first with a topical anesthetic or nerve blocker so the injections don’t hurt,” Dr. Loucas explained.
The whole process takes about an hour or two. Recovery is quick. Your scalp may be a little red following treatment, but any redness fades in a few hours. You may also experience some swelling of the scalp for a couple of days.
How many treatments are needed?
A full course of PRP treatment for hair loss involves three sessions spaced eight weeks apart. You should notice new hair growth in four to six weeks following treatment. The effects of PRP are not permanent. You’ll need to get maintenance treatments every six to 12 months to continue seeing results.
The best candidates for PRP therapy
PRP therapy can treat androgenic alopecia, the most common type of hair loss, also known as male-pattern and female-pattern baldness. However, it’s more likely to be effective if you start treatment in the early stages of hair loss, Dr. Loucas said. “You can’t show up with a huge bald spot and expect great results.”
It can also be effective in people with alopecia areata, an autoimmune disorder that causes hair to fall out in clumps, leaving round bald spots.
PRP therapy is less likely to work if your hair loss is due to a condition that causes scarring of the scalp, such as lupus. Once scarring has occurred, hair follicles typically can’t be reactivated.
You may get better results by combining PRP therapy with other hair loss treatments, though some people see good results with PRP therapy alone.
PRP therapy may not be recommended if you have an inflammatory skin condition such as psoriasis or a weakened or suppressed immune system.
Possible risks and side effects
Because it uses your own plasma, PRP is generally safe and well-tolerated, Dr. Loucas said. It’s possible to develop an infection, but your doctor will take measures to prevent this, such as cleaning the scalp with alcohol. Other risks include injury to the blood vessels or nerves, calcification at the injection site and development of scar tissue.
To reduce the risk of side effects, it’s important to choose a provider who has taken a training course in PRP therapy and has been performing it for at least a couple of years.
“Technique and training really matter here,” Dr. Loucas said. “Plus, an experienced provider can more accurately determine if you’re a good candidate for PRP therapy, so there’s a greater chance that you’ll get the results you’re seeking.”
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. She has written for Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many other outlets.
6 Home Remedies for Dry Skin on Feet
Why does it seem like no matter how much moisturizer you slather on your feet, they still look and feel as if you’ve been living in a desert? The skin on the feet has fewer oil glands to keep them hydrated, so it’s no wonder that trying to keep them soft and smooth can be rough going. That goes double if you suffer from hard, dry, cracked heels.
Dry, cold weather, standing for long periods, walking a lot, wearing shoes that are too tight and using harsh soaps can contribute to dry, cracked feet and heels. But so can skin conditions such as athlete’s foot, eczema and psoriasis. Diabetes can also cause changes in the feet that lead to dry, cracked foot skin.
For many people, the following six home remedies can help turn the skin on the feet from rough, dry and uncomfortable to smooth, hydrated and soft.
1. A Pumice Stone or Foot Scrub
Exfoliation gets rid of dry, dead skin, revealing the softer, smoother skin underneath. You can exfoliate using a pumice stone or an over-the-counter foot scrub, preferably after a shower, bath or foot soak in warm water (add a little Epsom salt for good measure), when the skin is soft. If you use a pumice stone, don’t be overly aggressive. Apply a moisturizing cream when you’re done.
Do not exfoliate your feet if you have sores or open wounds.
2. A Foot File or Rasp
A foot file is a tool with a handle and an abrasive metal surface that mechanically exfoliates the skin. Some foot files look like cheese graters. These may be too rough on the feet and in most cases should only be used on calloused heels, if at all.
Like pumice stones, foot files are best used after a bath, shower, or foot soak, when the skin has been softened. An electronic foot file with a head that spins is another option, especially for removing hard, dead skin from the heels. These are typically used on your feet when they are dry, but some waterproof models can be used in the shower.
3. Foot Cream or Heel Balm
For seriously dry feet, skip the lotion. Lotions contain a lot of water and aren’t as moisturizing as creams and ointments. Consider buying a cream or balm designed specifically for feet or heels. These are typically thicker and may contain softening and exfoliating ingredients such as alpha hydroxy acid, salicylic acid, hyaluronic acid, lactic acid or urea. Regular use helps prevent cracked heels.
At night, apply a heavy moisturizing cream, a foot cream or a thin layer of petroleum jelly to your feet and wear cotton socks to lock in the moisture and keep your sheets clean.
4. Moisturizing Gel Socks or Heel Socks
Available online, moisturizing foot socks or heel socks, also called heel sleeves, can give you the effects of moisturizer-plus-cotton-socks without the mess. They’re designed with a hydrating gel lining. Wear them for a few hours a day or while you sleep.
5. Foot Peel Masks
Foot peel masks are the latest internet sensation. These bootie-shaped sheet masks are worn for an hour, then discarded. In a week or more, dead skin will begin peeling off in large patches, revealing baby-soft skin beneath.
6. Liquid Bandage
If you have deep cracks in your heels, consider applying a liquid bandage, which is not a bandage at all, but a spray. These products form a seal over cracks, making walking less painful and closing the entryway for dirt and bacteria.
If these home treatments for dry, cracked skin on your feet aren’t working, see a Water's Edge dermatologist or podiatrist. The provider can examine your feet, determine whether any health conditions may be playing a role and develop an effective treatment plan.
ADVISORY: If you have diabetes, avoid home remedies until speaking with your doctor about the dry skin on your feet. If you suspect you may have athlete’s foot, see a dermatologist or your primary care physician. In addition to dryness on the bottoms or sides of your feet and cracking of the skin, symptoms of athlete’s foot include itching, burning, stinging, and flaking between the toes.
Article Written By: Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation, and many more.
How to Get Rid of Chapped Lips
If you ski or spend time in the snow or the sun, you’ve probably experienced chapped lips, which doctors refer to as cheilitis. They can be as uncomfortable as they are unsightly. In the case of severely chapped lips, cracks and sores may develop, and the lips may even bleed.
In most cases, a few simple changes to your daily habits and lip care routine will treat the chapping and give you back the soft, smooth, healthy lips nature intended.
Chapped lips causes
Lips are especially vulnerable to dryness and inflammation because they lack oil glands. The following factors can push the dryness over the edge and lead to chapping.
- Wind and cold weather. Frigid temperatures, low humidity and wind, especially when combined, can deplete moisture from the lips, leaving them flaky, scaly or swollen.
- Sun exposure. Lips are especially sensitive to ultraviolet (UV) rays because the layer of skin that covers them is thin and contains little melanin, the pigment that helps protect skin from the sun. Years of sun damage can cause a precancerous condition called actinic cheilitis, which may look like extremely chapped lips. In addition to dryness and cracking, signs include swelling and redness or white patches, usually on the lower lip. Over time the patches may become scaly and rough. In some cases, the border separating the lower lip from the skin below it becomes less distinct.
- Licking your lips. It’s tempting to do this when your lips feel parched, but it’s counterproductive. While a coating of saliva on dry lips may bring temporary relief, the saliva evaporates quickly, taking moisture with it and leaving lips drier than before.
- Certain medications and supplements. Chapped lips are a common side effect of topical retinoids such as Retina-A, vitamin A supplements and lithium, a medication used to treat bipolar disorder. Chemotherapy also can cause lips to become dry and chapped.
- Dehydration and diet. Chapped lips could be a sign of dehydration, or a diet that’s lacking critical nutrients, including B vitamins, zinc and iron.
- Excess saliva. If saliva collects in the corners of the mouth due to factors such as wearing braces or poorly fitting dentures or having a misaligned bite, the saliva can irritate the skin. What’s more, yeast and bacteria can flourish, causing reddish, inflamed, possibly crusty patches on the skin at the corners of the lips. This painful condition is called angular cheilitis. A deficiency of iron or vitamin B2 (riboflavin) is another possible culprit. Licking the lips makes the condition worse.
- The wrong balm or lipstick. Some products irritate the lips, making chapped lips more likely. The American Academy of Dermatology (AAD) advises steering clear of products that contain camphor, eucalyptus, fragrance, flavoring (such as citrus, mint or cinnamon), lanolin, menthol, octinoxate or oxybenzone, phenol (or phenyl), propyl gallate or salicylic acid.
Chapped lips remedies
For most people, using a good lip balm or ointment is the fastest route to healing chapped lips. Choose one labeled “fragrance free” and “hypoallergenic.” Look for at least one of these ingredients recommend by the AAD:
- Castor seed oil
- Ceramides
- Dimethicone
- Hemp seed oil
- Mineral oil
- Petrolatum
- Shea butter
- White petroleum jelly
For extremely chapped lips, the AAD recommends using an ointment that contains white petroleum jelly. Ointments are more effective at sealing in moisture than waxes or oils. Don’t use any lip balm that makes your lips tingle, sting or burn. If you find that your lip product dries out your lips, choose a different product.
When you’re outdoors, no matter the season, use a lip balm with SPF 30 or above that contains titanium oxide or zinc oxide, and reapply it every couple of hours. In the winter, cover your mouth with a scarf, ski mask or face gator to protect your face and lips from the elements.
Indoors, running a humidifier can help keep your lips hydrated. Run it in the room where you spend the most time.
Drink plenty of water throughout the day to keep your lips, and the rest of your body, hydrated. Avoid licking, biting or picking at your lips.
If these steps don’t resolve the problem, see a skincare provider. All cases of actinic cheilitis should be treated by a dermatologist to reduce the risk that the patches will become cancerous. People with angular cheilitis may also need a doctor’s care.
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.
Skin Signs of Heart Disease
Medical review by John Minni, DO
Your eyes may be the window to your soul, but your skin can reveal what’s in your heart — or at least offer clues that something in your cardiovascular system might be amiss. Who would have thought that in some cases, for instance, a skin rash can suggest a risk of heart disease? Or that certain conditions that slow down blood circulation can change the skin’s appearance?
Read on to discover some of the hidden connections between the skin and the heart.
Psoriasis
What’s the link between psoriasis and heart disease? People with this skin condition appear to have an increased risk of heart attack and stroke.
"It’s a hot topic in dermatology,” said Dr. John Minni, DO, a board-certified dermatologist and psoriasis expert at Water’s Edge Dermatology.
Psoriasis involves chronic inflammation, which causes the skin to develop scales that often hurt and itch. (It also causes changes to the fingernails and toenails.) That same inflammation wreaks havoc throughout the body, including the arteries that feed the brain and heart, damaging them in ways that make clots more likely to form.
There’s still a lot to learn about the link between psoriasis and cardiovascular disease. For example, is the risk for a heart attack even higher if you also have psoriatic arthritis, which is common in people with psoriasis? “We think so, but we’re not sure yet,” said Dr. Minni.
Can controlling your psoriasis lower your odds of developing heart disease or having a stroke? That’s a promising area of research — and potentially another good reason for you to take a biologic or another medication that has anti-inflammatory effects if your doctor has prescribed one. “It’s going to help with your overall health, not just make a rash go away,” said Dr. Minni.
Lower-leg skin and vein changes
Are your lower legs and ankles swollen? Has the skin there developed a leathery look? Does it flake or itch? These could be signs of chronic venous insufficiency (CVI), which occurs when malfunctioning veins can’t push blood back to the heart efficiently, causing it to pool in the lower limbs. Another possible sign of CVI include varicose veins. In severe cases, you can develop sores that won’t heal.
A temporary first treatment for CVI is to wear compression garments. Minimally invasive procedures offer a permanent treatment by closing off damaged veins and rerouting blood flow.
Cold feet and shiny, hairless legs
If you have peripheral artery disease (PAD), which occurs when narrowed arteries reduce blood flow to the limbs, your legs and feet may feel cold. Your legs might also lose hair, appear shiny and turn pale when elevated. Your toes might turn blueish-purple.
Medication can improve blood flow and help prevent PAD from worsening, though sometimes bypass surgery is necessary to reroute blood flow around a clogged artery. In other cases, a doctor can unclog a blocked leg artery with a less invasive procedure called angioplasty.
Pale, thickened nails
If your fingernails and toenails turn pale and thicken, it could be a sign of PAD, though pale nails can also be a sign of other medical conditions.
Reddish or brownish streaks in nails
These streaks are splinter hemorrhages, which can look like tiny shreds of wood under the nail. Rarely, splinter hemorrhages can be caused by a heart valve infection, a condition called vasculitis that involves blood vessel inflammation, or tiny clots in the capillaries under the nails. It’s much more likely, however, that you simply whacked or stubbed your nail.
Orange-yellow bumps
People who have very high levels of cholesterol or blood fats called triglycerides may develop eruptive xanthomatosis, a rash that can cover a large swath of skin. The waxy, pea-sized bumps can show up anywhere on your body but often appear on the legs, arms, shoulders and backside. In some cases, Dr. Minni notes, eruptive xanthomatosis occurs in people with an inherited condition that causes extremely high cholesterol.
The bumps may go away on their own after a few weeks, but a cardiologist will likely prescribe treatment to bring your cholesterol and triglycerides under control.
Written by Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.
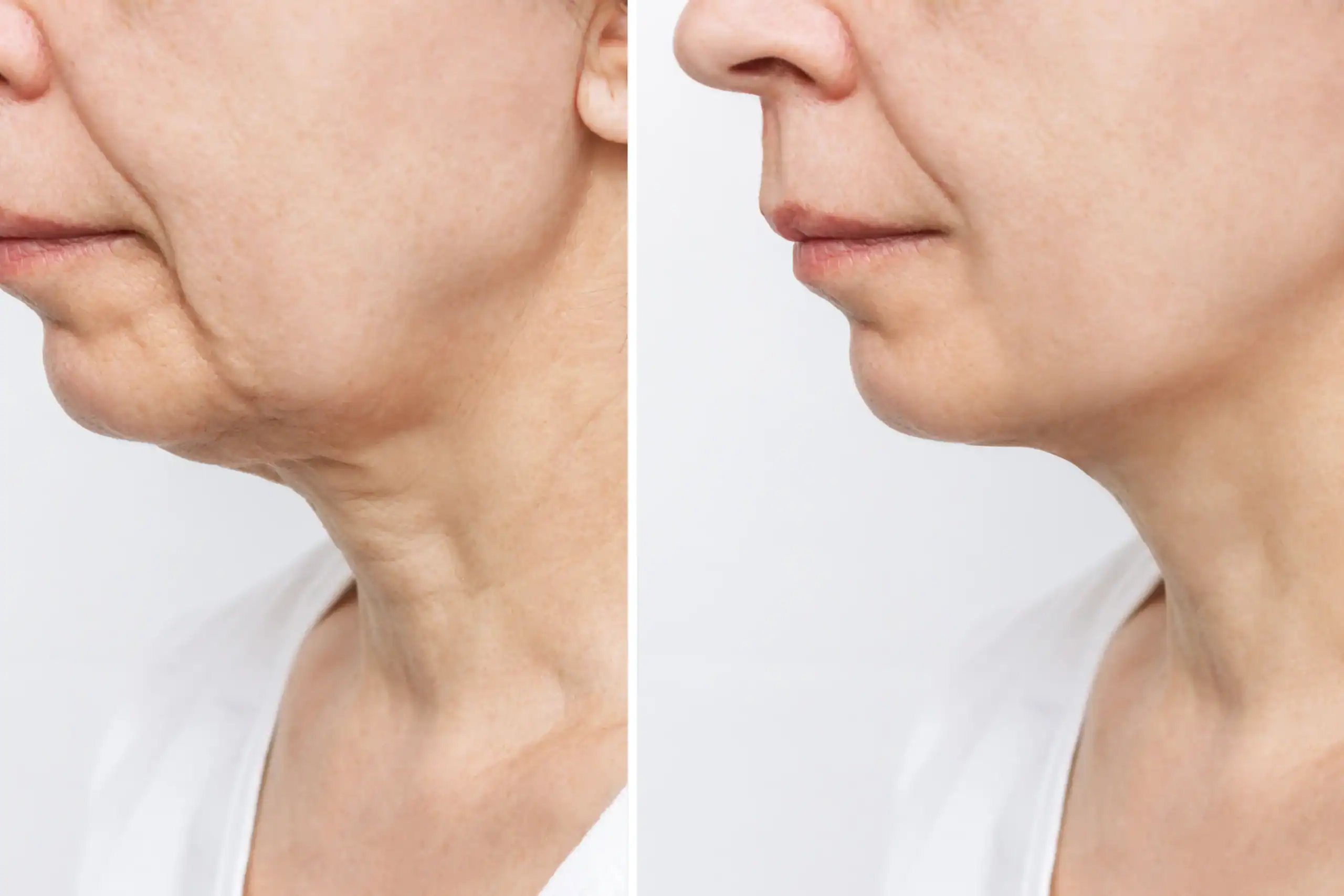
What Is a Mini Neck Lift?
Medical Review By: Juan Giachino, Jr., MD
Getting older? One of the first signs of aging is the dreaded "turkey neck." It’s no coincidence that author Nora Ephron titled her book about aging "I Feel Bad About My Neck."
This area is delicate because neck skin is especially thin. It can start to sag, wrinkle or look crepey as the skin loses collagen and elasticity, the neck muscles weaken and gravity starts to win out.
The best way to get rid of turkey neck is to remove excess skin through a neck lift or mini neck lift, which reduces sagging and wrinkles.
A mini neck lift is a minimally invasive surgical procedure that removes excess skin in the jowl area and under the chin to create a more contoured, youthful-looking jawline and neck. The procedure is less extensive than a traditional neck lift, with smaller incisions, fewer risks, and a shorter recovery period.
“Essentially, the difference between a mini neck lift and a full is how much dissection you do, and with the mini, you’re not dissecting as much,” said Dr. Juan Giachino Jr., MD, a board-certified plastic surgeon specializing in cosmetic and reconstructive plastic surgery at Water’s Edge Dermatology.
He notes that surgeons may define a “mini” procedure differently, so it’s important for patients to discuss their goals during the initial consultation. Many surgeons make incisions only around the ear during a mini neck lift; others may also make incisions under the chin and tighten two strips of neck muscle, called the platysma muscle, to reduce the look of verticals bands caused by muscle looseness.
Who is an ideal candidate for a mini neck lift?
A mini neck lift is an effective option for younger people whose skin is still moderately elastic and who have only a small amount of hanging skin and sagging.
“A great candidate is someone in their 40s or 50s who’s just starting to get some early jowling, or recurrent jowling if they’ve had a neck or face lift before, and a little laxity in the front of the neck,” said Dr. Giachino, Jr. Someone with a heavier, sagging neck should opt for a full neck lift.
Patients who smoke must stop for at least three weeks prior to the procedure, since nicotine impedes wound healing.
What happens during a mini neck lift?
A mini neck lift is performed under local anesthesia, with or without sedation depending on the surgeon and the needs of the patient. The procedure typically takes about an hour.
The surgeon begins by injecting a local anesthetic around the ears and hairline to numb the areas. Small incisions are made at both earlobe curves and behind the ears, extending up to the hairline. Next, excess skin is removed, and the skin is sewn back together with stitches. Some surgeons will also tighten the platysma muscle.
Mini neck lift recovery
After the procedure, the patient’s neck and head is wrapped for approximately one day. The patient can shower within 48 hours. Pain is typically managed with Tylenol, although some surgeons may prescribe a pain medication for the first 24 hours. Some swelling and bruising should be expected.
“The nice part about a mini neck lift is that it’s less invasive for faster healing and recovery,” says Dr. Giachino, Jr.. “A full neck lift requires more downtime to recover and extended delays in resuming fitness activities.”
What results can I expect?
A slimmer, more defined jawline and a smoother, crepe-free neck are visible immediately. The neck’s appearance continues to improve over the next two days as swelling subsides.
Dr. Giachino, Jr. estimates that the average mini neck lift lasts up to five years, especially if you use sunscreen and avoid dramatic weight fluctuations.
“Most of the time, after five years the patient comes back in for another mini neck lift,” he noted. “You can do this procedure multiple times as the skin stretches out, and the second and third time around is always easier than the first because the dissection has already been done, so there’s a lot less swelling and bruising.”
Although a mini neck lift lasts only half as long as a traditional neck lift, it also costs half as much.
How can I make my mini neck lift last longer?
To prolong or enhance the results, Dr. Giachino, Jr. recommends an active skin care regimen. Start with small additions, such as a prescription Retin-A product to increase collagen production if your dermatologist recommends it. Chemical peels can reduce the appearance of fine lines, which a mini neck lift cannot. Laser treatments can reduce wrinkles and also tighten the skin when it begins to sag again.
Article Written By: Kaitlin Clark, a beauty writer specializing in skin and plastic surgery content. Clark contributes regularly to a variety of major outlets including Allure, InStyle, RealSelf, Vox Media and Refinery 29, covering everything from new FDA guidelines to trending aesthetic procedures.
What Causes Dry Skin?
Many people experience dry skin, known to doctors as xerosis cutis, at some point in their lives. Dry skin occurs when the skin loses too much water or oil, making the skin flake and feel tight. It may also itch or crack. But what are the root causes of dry skin?
The list is long. It could be that the soap you use is too harsh, the baths or showers you take are too hot or the air you’re living in is too dry. Or it could be something else entirely.
If you’ve been struggling with dry skin and can’t figure out why, consider these potential triggers.
Environmental Causes
The world around you can conspire to rob your skin of water and oil.
- The weather. Many people are plagued by dry skin in the winter due to colder temperatures and lower humidity. Dry skin can be a year-round problem for those who live in a cold climate or a hot, low-humidity climate.
- Indoor heating. In winter you spend more time indoors, where you’re exposed to dry, heated air. Heating indoor air — whether via central heating, a fireplace, a wood-burning stove or space heater — lowers the humidity and saps moisture from your skin.
- Sun exposure. Heat from the sun also leaves skin parched. If you’ve accumulated a lot of sun damage, your skin may look dry and rough all the time.
Lifestyle Causes
Some of your daily habits could be contributing to dry skin.
Frequent bathing. Long and/or hot showers and baths break down the skin’s lipid barrier, which seals in moisture.
Harsh soaps and detergents. Deodorant and antibacterial soaps rob the skin of natural oils. Even a caustic laundry detergent can trigger dry, itchy skin.
Harsh facial skincare products. If you’re using certain acne products or a high-concentration retinol product, for example, you may see dry, flaky skin on your face.
Smoking. Smoking accelerates the aging process in several ways and can lead to dry, coarse skin.
Frequent hand washing. People who must wash their hands frequently, such as healthcare professionals and cooks, are vulnerable to dry skin. Constantly wetting and drying your hands can break down the skin barrier. And when any water that remains on the skin evaporates, it reduces oil in the skin. This is also why handwashing is a common hand eczema trigger.
Exercising outdoors. If you do most of your workouts outdoors, your dryness may be due to exposure to the sun and wind, which causes moisture to evaporate from your skin.
Swimming in pools. Swimming in any pool can dry out the skin. A heavily chlorinated pool can dry it out even more thanks to the chemicals in the water.
RELATED: How to Heal Dry, Cracked Hands
Genetics and Aging
People who have fair, brown or black skin are more likely to develop dry skin than those who have a medium complexion, such as those with a Mediterranean background. Genetics may also dictate how well your skin barrier functions.
As you age your skin produces less sebum, the oily substance that protects the skin and keeps it moisturized. For women, the most dramatic drop in sebum production occurs in their 40s and continues to decline from there. Loss of sebum production happens later in life for men.
Medical Causes
Certain medications. Dry skin is a side effect of several types of drugs, including certain drugs used to treat high blood pressure, high cholesterol, allergies, and acne.
Vitamin and mineral deficiencies. Being low on zinc, vitamin A, vitamin D, niacin or iron can make your skin dry. People who are malnourished in general, including those with anorexia, are susceptible to dry, yellowish skin.
Certain skin conditions. Dryness often goes hand-in-hand with eczema, seborrheic dermatitis, psoriasis and fungal infections such as athlete’s foot.
Diabetes. Dry, scaly skin is common in people with diabetes. In fact, skin changes are sometimes the first sign a person has the disease. When blood sugar levels are high, the body pulls fluid from cells in order to make enough urine to excrete the sugar from the body. As a result, the skin becomes dry. Other causes of parched skin include in people with diabetes include fungal infections and nerve damage, which can interfere with the production of skin-softening perspiration.
Hypothyroidism. An underactive thyroid can cause dry skin. The thyroid hormones regulate many bodily functions, including the turnover of dead skin cells. When thyroid hormone levels are low, it takes far longer for dead skin cells to be shed and replaced by new ones, so skin looks dry and flaky.
Kidney disease. People in the later stages of kidney disease develop extremely dry, often itchy skin that feels rough and cracks easily. The cause is chronic dehydration and, in the end-stage of the condition, shrinking sweat and sebaceous glands.
HIV. Because people with HIV have a weakened immune system, they’re more likely to develop certain skin conditions that cause dryness, including seborrheic dermatitis and fungal infections.
For most people, using the right moisturizer, switching from soap to a gentler cleanser in the shower, choosing a hydrating facial cleanser, and shortening showers and baths goes a long way toward helping the skin retain the moisture it needs. A humidifier can help solve the problem of dry indoor air.
But if your dry skin continues, or you’re not sure what’s causing it, your dermatologist can take a medical history, perform a skin evaluation and devise a treatment plan for you.
Article Written By: Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.
Face Fillers and the COVID Vaccine: Know the Facts
Medical Review By: Ted Schiff, MD
If you’ve had face fillers (also known as cosmetic fillers or dermal fillers) such as Juvedérm or Restylane, you may be wondering if it’s safe to get the vaccine for COVID-19. According to news reports, a few people experienced swelling at the site of their filler injections after getting vaccinated.
The short answer: Yes, it is safe. Here’s what we know right now.
Filler swelling as a side effect
Three participants in the clinical trial for Moderna’s COVID-19 vaccine experienced swelling at the filler injection site. One of the patients had the filler injected two weeks before getting vaccinated, while another received filler injections six months prior. A third person, who had gotten more than one lip filler injection in the past, experienced swelling in the lips two days after getting the vaccine. That person had previously experienced a similar reaction to the flu vaccine.
Is it just the Moderna vaccine?
So far there have been no public reports of similar reactions to the other COVID vaccine currently being administered in the United States, made by Pfizer. But since vaccines ramp up the body’s efforts to fight foreign invaders, any vaccine could theoretically trigger a reaction to a foreign substance in the body, such as a dermal filler.
“Most dermatologists have seen similar immune reactions to other vaccines in the past, like the flu shot and the shingles vaccine,” said Ted Schiff, MD, Water’s Edge Dermatology founder and chief medical officer. “It’s likely a sign that the vaccine is doing what it’s supposed to do — heighten the body’s immune response.”
How big is the risk?
There’s no reason for serious concern. The possibility of filler swelling shouldn’t deter you from protecting yourself and those you love by getting vaccinated for COVID-19 as soon as you can. First, this reaction occurred in only a small handful of patients — three out of more than 30,000 participants in the Moderna trial, or less than .01%. Second, all the reactions were mild, temporary, and easily treated with antihistamines or steroids. None required the use of an EpiPen or hospitalization.
“We want to reassure our patients that it is safe to get the COVID-19 vaccine,” said Dr. Schiff. “Reactions like this are typically both rare and minor.”
Dr. Schiff noted that the risk of contracting COVID-19 is far more serious than the risk of temporary, treatable inflammation.
“Water’s Edge Dermatology will continue to monitor the situation with both available vaccines, as well as with any future COVID-19 vaccines that are rolled out in the U.S.,” he added.
If you’ve had a reaction to a previous vaccine at the site of filler injections, tell the doctor or other medical provider when you are preparing to be vaccinated. If you have any questions or concerns about fillers or implants you’ve received, don’t hesitate to contact your Water’s Edge provider.
Article Written By: Gina Shaw, an award-winning writer based in New Jersey who has covered health and medicine topics for more than 20 years.
Beard Care 101: Tips for a Healthy Beard
You’ve grown a beard, or you’re growing one. Now what? To keep your beard soft and the skin underneath it healthy and itch free, you’ll want to make sure you have the proper skin and hair care routine.
Here’s what you need to know about how to care for a beard and the beard care products that can help moisture the skin under your beard, prevent ingrown beard hair, stave off beard dandruff and more.
How often should you wash your beard?
To rid your beard of grime and bacteria, you need to wash it. Ideally, you’re already washing your beard twice a day because you’re washing your face twice a day, once in the morning and once at night.
Some men skip washing their face in the morning because they think their face doesn’t get dirty overnight. Surprisingly, it does. Pillowcases trap dust and collect oils, sweat and bacteria while you sleep, so a morning wash is a must. You should also wash your face after any activity that makes you sweat.
For extra cleansing, you might want to shampoo your beard once or twice a week, particularly if you live in a humid area (like Florida), sweat excessively or have oily skin. The shampoo you use on your hair may be too harsh for the more delicate skin on your face, so consider using a beard shampoo.
How to care for the skin under your beard
The trick to avoiding dryness, itching and flaking skin under your beard is simple: Skip the bar soap — especially deodorant soap — and buy a facial cleaner. Choose the right facial cleanser for your skin type.
- Normal skin: Any gentle, non-comedogenic (not pore clogging) facial cleanser will do. A good choice is wederm Exfoliating Gentle Cleanser.
- Dry skin: Look for a creamy, hydrating cleanser that is non-comedogenic and fragrance free. Helpful ingredients include hyaluronic acid, ceramides, squalene and glycerin. Try ZO Skin Health Hydrating Cleanser.
- Oily/acne-prone skin: A non-comedogenic gel cleanser that contains salicylic acid or glycolic acid is an ideal choice for keeping pores clear. Consider wederm Exfoliating Gentle Cleanser. The option containing 2% salicylic acid and 5% glycolic acid is better for oily skin.
- Sensitive skin: Choose a non-comedogenic, creamy cleanser labeled soap free and fragrance free. For best results, gently apply the cleanser to your face and beard using circular motions and rinse thoroughly with warm water. To avoid frizz, pat your beard dry with a towel instead rubbing it.
If you’re still in the stubble phase, apply a moisturizer after you cleanse, while your face is still damp. Do this even if your skin is oily or acne-prone. The aloe-based wederm Ultra Lite Facial Moisturizer is a great choice. Another good choice is a light, gel-based moisturizer. Neither will appear greasy or cause acne.
Help for ingrown beard hair
If you’re prone to ingrown beard hairs, use a gentle exfoliating scrub a few times a week, particularly when you’re in the process of growing your beard. This helps loosen the ingrown hairs trapped under your skin and prevent new ones from forming.
Choosing the best beard care products
Once your beard has grown in, use a beard conditioning product to moisturize the skin under your beard and soften the beard itself. (People with sensitive skin may want to stick with a moisturizer.) These products hydrate both the beard hair and the skin underneath. As with facial cleansers, choosing the right beard conditioning product depends on your skin type.
- Beard oil is ideal for people with normal or dry skin, and also for those with long beards. A little oil goes a long way, so apply it a drop or two at a time to avoid a greasy look.
- Beard balm is thicker than oil (it resembles pomade), so it’s good for dry skin types. Because it also provides hold, it can help shape longer beards and tame fly-away strands.
- Beard conditioners are a better bet for oily and acne-prone skin because they’re lighter and less greasy than oils and balms. You can choose a leave-in conditioner (apply to your beard when it’s damp from cleansing) or a rinse-off conditioner you use in the shower.
More tips for a healthy beard
For a clean, good-looking beard that doesn’t irritate the skin under it, remember to:
Trim your beard regularly. Even if you prefer a long beard, you’ll want to trim it on occasion to get rid of spilt ends and achieve a cleaner look.
Prep your skin before your trim. Apply a shaving cream, gel or oil to prevent skin irritation. It’s best to use an electric razor, though people with long beards may prefer to use scissors.
Keep your grooming instruments clean. Bacteria and oil can collect on razors, scissors, combs and brushes and be transferred back to your face. Wipe, soak, disinfect and dry as necessary.
Avoid touching your face or stroking your beard. You’ll spread the germs and oils on your hands to your face and beard.
Written by Jessica Brown, a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.
How to Identify Scabies (With Pictures)
Medical review by Ted Schiff, MD
If your skin has red bumps that are mighty itchy, the cause could be a mite. Here’s what to know about the contagious infestation known as scabies and how to recognize it so you or your child can get treated before the itching becomes unbearable.
What is scabies?
Scabies is a skin condition caused by an infestation of microscopic eight-legged mites called Scarcoptes scabiei. The mites cause extreme itching and a rash. Symptoms develop after pregnant female mites burrow into the skin and lay eggs. When the eggs hatch, the young mites return to the surface of the skin via the burrows created by the females. Without treatment, the cycle repeats itself as the young mites mate and tunnel under the skin to lay their eggs.
What does scabies look like?
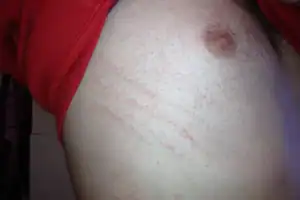
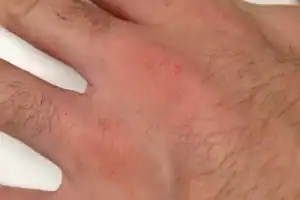
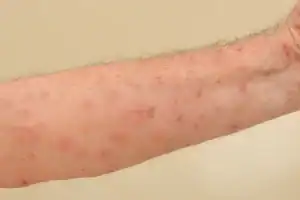
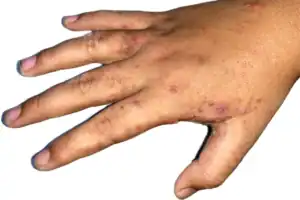
The scabies rash takes the form of small, red bumps that may look like pimples, bug bites, hives or knots under the skin. You might be able to see the burrow tracks created by the mites, which appear as raised lines of tiny blisters or bumps. Some people develop scaly patches that resemble eczema.
Because the rash is so itchy, sores may result from constant scratching and can become infected. Itching is worse at night and can interfere with sleep.
A less common and more severe type of scabies called crusted or Norwegian scabies happens when an exceptionally large number of mites invades the skin. There may be hundreds or thousands of mites compared with only 10 or 20 in typical scabies. People with crusted scabies develop thick crusts of skin that contain mites and eggs. They may or may not experience itching and a rash.
Once someone has been exposed to scabies, symptoms develop four to eight weeks later. (In someone who’s had scabies before, symptoms may develop in just a few days.) It’s possible to spread scabies to others during the pre-symptomatic stage as well as the symptomatic stage.
Adults who contract scabies tend to develop the rash in certain areas of the body, which include:
- Armpits
- Between the fingers
- Inner elbows
- Sides of the wrists
- Waist
- Around a nipple
- Knees
- Buttocks
- Male genitals
- Soles of the feet
- Areas covered by jewelry like bracelets, watches and rings
Infants and very young children are more likely to get scabies on the:
- Head
- Face
- Neck
- Palms
- Soles of the feet
How do you get scabies?
Scabies is transmitted by prolonged skin-to-skin contact with someone who has it. A quick hug or handshake is unlikely to spread scabies; you’re more likely to get it from a member of your household or through sexual activity. You can also contract scabies by touching personal items that someone with scabies has used, such as towels, furniture, bedding and clothing, though this mode of transmission is less common. You cannot get scabies from an animal that has mites.
Who gets scabies?
Scabies has nothing to do with poor personal hygiene or dirty surroundings. In truth, anyone can get it. People who are more vulnerable to contracting scabies include:
- Children
- Mothers of young children
- Sexually active young adults
- People who live in group settings, such as nursing homes, assisted living facilities and extended care facilities
- Elderly people
- People with a weakened immune system
- People who have received an organ transplant
Crusted (Norwegian) scabies primarily affects elderly people and those with a weakened immune system, disability or neurological condition. It’s more contagious than typical scabies because it spreads via person-to-person contact and also through the shedding of the skin crusts. When crusts fall off, the mites inside can survive for up to a week, which gives them time to find another host.
Scabies treatment
If you suspect you might have scabies, see a dermatologist promptly. He or she will check for signs of mites and may take a skin scraping from the area and look for mites and their eggs under a microscope.
Scabies is treated with prescription medications called scabicides, which kill the mites. Permethrin 5% is the most commonly prescribed scabicide. While these medications kill mites quickly, the itching may last for several weeks. Skin usually heals within four weeks.
Treating crusted scabies is more challenging, and treatment may last for several weeks or longer if necessary. People with crusted scabies may be prescribed both a scabicide and another mite killer called benzyl benzoate, along with a keratolytic cream, which helps reduce crusting of the skin and allows for better absorption of permethrin or benzyl benzoate.
Some scabies patients may be prescribed additional medications such as an antibiotic (if an infection is present) and medications to help control itching, such as a steroid cream and antihistamine.
Because scabies is highly contagious, your dermatologist may recommend that members of your household and your sexual partner(s) be treated for scabies as well. You’ll also need to do a thorough cleaning of your home, including vacuuming floors, rugs and all upholstered furniture. (Discard the vacuum bag afterward.) Items such as towels, sheets, blankets and clothing should be washed in hot water and dried on high heat or dry-cleaned. Another option is to seal the items in a plastic bag for at least 72 hours, since mites that aren’t in skin crusts die within a few days without a host.
The good news is there’s no need to use insecticides or fumigants to get rid of mites — in fact, the Centers for Disease Control and Prevention doesn’t recommend them — so you don’t have to expose your family to these chemicals or endure their odor to make your home safe again. And, since the scabies mite can’t survive on animals, there’s no need to treat your pet.
Written by Jessica Brown is a health and science writer/editor based in Brooklyn, New York. Her work has appeared in Prevention, Johnson & Johnson, the Breast Cancer Research Foundation and many more.
*Wikimedia Commons photo licenses:
Man's chest with scabies: Fhgd, CC BY-SA 3.0 via Wikimedia Commons
Hand scabies: Fhgd, CC BY-SA 3.0 via Wikimedia Commons
8 Common Skin Conditions in Elderly Adults
Medical review by Ted Schiff, MD
Like every part of the body, the skin changes with age. The teen years bring dreaded pimples. Middle age brings telltale wrinkles. In elderly adults, skin conditions may become more numerous — and more noticeable — as the skin continues to thin and lose fat, elasticity, and moisture.
Skin cell turnover decreases dramatically, which slows wound healing. Aging weakens the immune system, so skin infections are more common. Age spots may take up more acreage. Large, dark bruises may spring up out of nowhere.
Some skin problems, like dark bruises, are alarming but are mostly harmless. Others require medical attention. Here are eight skin conditions in elderly adults and what older adults, loved ones and caregivers should know.
1. Easy bruising
Why do old people bruise easily? Aging skin is thinner, and there’s less fat to act as cushioning. Also, blood vessels are more fragile and easily broken. Bruises happen when blood leaks out of blood vessels, so more broken vessels means more bruising. Older people who take blood thinners or even over-the-counter painkillers such as aspirin or ibuprofen may bruise more easily.
A minor bump or scrape can result in a surprising amount of bruising and make concerned loved ones wonder what’s happening. The bruises are usually harmless. But anyone who often develops large bruises with no logical explanation should see a doctor to rule out an underlying health problem.
If a loved one or caregiver has any reason to suspect abuse as the cause of bruising, they should investigate. Most accidental bruises occur on the extremities, according to the National Institute of Justice, whereas bruises in abused elders are more likely to occur on the head, neck or torso, and they tend to be large.
Take action
To treat bruises:
- Apply a cold compress for up to 20 minutes a time.
- Apply Dermaka cream, a bruise treatment made with plant extracts and vitamins, according to the package directions.
- If a leg or foot is bruised, keep it elevated when resting.
2. Dryness and itching
Dry skin in elderly adults is very common; in fact, more than half of older adults have it. A loss of sweat and oil glands is one reason. Not drinking enough liquids may be another. In addition, certain chronic health conditions, such as diabetes and kidney disease, can cause dryness and itching, as can some of the medications used to treat them.
Skin may become cracked and painful. Scratching can cause skin irritation and open the way for infection-causing germs to enter.
Take action
If you have dry, itchy skin:
- Take shorter, cooler baths or showers and use a moisturizing soap (skip the deodorant soap)
- Use a moisturizing ointment or cream daily. (Avoid lotions, which contain more water.) CeraVe, Cetaphil and Vanicream all make gentle, effective moisturizers.
- Drink more water.
- Run a humidifier if the air is dry.
- If the itching doesn’t subside, tell your doctor. It could be a sign of liver, kidney or thyroid disease.
3. Age spots

Take action
- Wear sunscreen with at least 30 SPF to help prevent more age spots from developing.
- See a dermatologist to make sure the spots are in fact age spots and not something else, especially if they change in appearance.
- If your age spots bother you, a skin care provider can treat them.
4. Skin tags
Skin tags are soft, spongy, often flesh-colored growths of tissue that typically appear on eyelids, neck, thighs and skin folds such as the armpits, groin and under the breasts. They may hang from the skin on small stalks. Skin tags are more common in women, people who are overweight, older adults and people with diabetes. They can become irritated if clothing rubs them or jewelry snags them.
Take action
- Skin tags are harmless, but if you want one removed, see a dermatologist. A dermatologist will remove it for you.
- Don’t try to remove a skin tag yourself. It’s a bad idea for several reasons.
5. Skin cancer
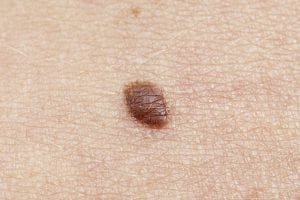
Take action
- Perform a skin check once a month to look for new growths and changes in existing moles. Evaluate moles using the ABCDE test. Make an appointment with your dermatology provider if you see something suspicious.
- Have a skin cancer screening based on the schedule your dermatologist recommends, but at least once a year.
6. Shingles
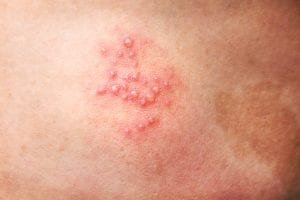
Shingles starts with burning, itching, tingling or extreme sensitivity in one area of the skin. A painful rash then develops, often along with a fever or headache. The rash eventually blisters. Skin infections and long-term nerve pain are possible complications.
Take action
- See a doctor as soon as symptoms appear. Early treatment with an oral antiviral medication may reduce the duration and severity of an outbreak.
- Take an over-the-counter pain medication for pain and use cool compresses, calamine lotion and lukewarm baths with colloidal oatmeal (oats ground into a fine powder) for itching.
- To prevent shingles, get both doses of the Shingrix vaccine.
7. Bed sores
Bedridden or wheelchair-bound older adults are susceptible to open wounds called bed sores or pressure ulcers. These develop in areas subject to pressure when you sit or lie down, such as the tailbone, shoulder blades, backs of the knees and heels. People with diabetes, poor circulation or poor nutrition face a higher risk of bed sores.
Prevention is critical. Bed sores can be very difficult to treat once they develop, and they may become infected.
Take action
- In bed, reposition every two hours. In a wheelchair, change position every 15 minutes.
- Keep skin clean and dry.
- Watch for redness and warmth in one area of the skin; it’s an early warning sign. If you’re a caregiver, call the doctor if you notice this or see a sore, scrape or blister. A wound care nurse may be needed to coordinate care.
- Consider a gel or foam mattress topper or a mattress with alternating air pressure, which can help prevent pressure sores.
8. Skin tears
The fragile skin of elderly adults tears more easily, especially in people who take oral or topical corticosteroids, which can weaken the skin. The skin might tear when you bump into something, or when a caregiver removes wound tape or dressing.
Take action
- Use moisturizer and drink plenty of water to keep skin hydrated, which can help prevent tears.
- Wear long pants and a long-sleeved shirt or arm sleeves to protect the skin.
- If a small tear occurs, wash the wound with gentle soap and water. Put the skin flap back in place if there is one, then cover the wound with gauze.
- See a doctor for more serious tears or if you notice signs of infection, such as redness, swelling, fever, worsening pain or a bad odor.
Written by Jennifer L. Cook, an award-winning editor and writer whose work has appeared in Good Housekeeping, Prevention, Consumer Reports on Health, and Woman’s Day and on Investopedia.com and Bottomlineinc.com.