Genital warts, also known as venereal warts or condylomata acuminata, are caused by the human papilloma virus (HPV). More than 100 types of HPV are known to exist.
- Low-risk types (HPV 1, 2, and 3) cause warts on the hands, feet, and other parts of the body.
- Types 6 and 11 can cause warts on the genitals or anus (genital warts).
- Other types (HPV 16 and 18) can cause cancer of the cervix, external genitalia, anus, head and neck, tongue and tonsils. The HPV types that cause genital warts only rarely cause cancer.
Genital warts are a type of sexually transmitted disease and all partners should be checked thoroughly. They can also be seen in infants who have been delivered vaginally to mothers with HPV in their genital tracts; therefore, alternate methods of delivery should be considered.
Only a small percentage of people infected with HPV will develop genital warts. Many people are carriers of HPV who may never develop warts, but may still be able to pass HPV to their sexual partners.
The incubation period from contracting HPV until the development of warts may be several months, although some people may not develop warts for years after contact with HPV. People who have lower immunity due to cancer, AIDS, organ transplantation, immune suppressive medications, or certain other medications are more susceptible.
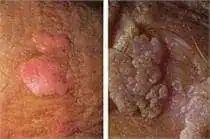
What Do Genital Warts Look Like?
Genital warts may be rough or smooth-surfaced, and are typically flesh-colored, but some may be darker. They can be large or small, and can be found as a single growth or in groups. They can appear on the external genital skin, inside the vagina, or the anus.
Genital warts can itch or bleed and interfere with bowel movements, urination, and sexual intimacy. They are also unsightly and difficult to keep clean.
Genital Warts Treatment
Most genital warts are diagnosed during an examination by a dermatologist. The growth may be surgically removed and sent to the laboratory for microscopic evaluation to confirm the diagnosis.
Treatment depends on the number of warts, their specific location, and other factors. Recurrences are always possible. Your Water’s Edge Dermatology practitioner can use both surgical and nonsurgical (chemical) treatments. Surgery includes:
- Simple excision
- Removal with an electric needle
- Cryosurgery (freezing with liquid nitrogen)
- Laser
These methods may require local anesthesia, and time is required for healing. Nonsurgical methods include chemicals that destroy the warts. These methods require multiple office visits at two- to three-week intervals and include:
- Acid applications (bichloroacetic acid or trichloroacetic acid), which produce irritation
- Interferon injections (an antiviral drug), which often produce fever, chills, and headaches
Prescription medicines that may be used at home include:
- Podofilox gel or solution, which stops the growth of the wart cells
- Imiquimod cream, which helps the body to produce proteins that act against HPV and boost the local immune system. It is associated with the lowest recurrence rate after complete clearance.
Both methods may cause mild irritation.
Removing warts reduces the risk of passing the virus to partners. After successful HPV wart treatment, a person is probably less contagious, yet there is no guarantee that all HPV is gone since the virus may be deep in the layers of the skin.
Genital Warts Prevention
Knowing one’s sexual partner and other forms of safe sex help reduce transmission, but only abstinence is 100% effective. Transmission can be reduced by the proper use of condoms if the appropriate conditions are met, and by the successful treatment of warts. Neither method, however, can prevent transmission in every case, especially for warts found in an area that the condom does not cover.
There is only one vaccine that helps protect against certain diseases (like genital warts) and HPV-related cancers caused by the nine types of HPV (Types 6, 11, 16, 18, 31, 33, 45, 52 and 58). This vaccine is GARDASIL 9. Like many vaccines, GARDASIL 9 works to help prevent disease when given before there is any contact with the virus. The Centers for Disease Control and Prevention (CDC) recommends HPV vaccination for children at age 11 or 12, but it may be given as early as 9 years of age.
