Microneedling + Dermaplaning: Learn Why, When & Where
You may have heard the buzz about microneedling and dermaplaning. These are two terrific beauty treatments we perform with great regularity and success at all our Water’s Edge Dermatology locations that offer aesthetic treatments. The most common questions about these amazing aesthetic services are Why? and When?
Why choose microneedling and dermaplaning, as opposed to other aesthetic services? Why choose one vs. the other? And when is the right time to choose them?
To answer these and other questions, let’s take a closer look at both microneedling and dermaplaning. There are some very good reasons why they’re trending so heavily days, and not only with women.
Addressing an 'Age-Old' Problem with Microneedling & Dermaplaning Treatments
Do you feel a twinge of envy when you see someone with flawless, baby-smooth skin? Do you sigh when you look in the mirror? Fine lines, wrinkles, blemishes, scars, spots – almost everyone has them. With age, uneven texture and signs of sun damage are common. The skin loses collagen and elastin proteins, giving it the characteristic aged appearance. But smoother skin doesn’t have to remain a dream. Here are two minimally invasive procedures that can give you smoother, brighter, more youthful skin.
Microneedling To Turn Back Time
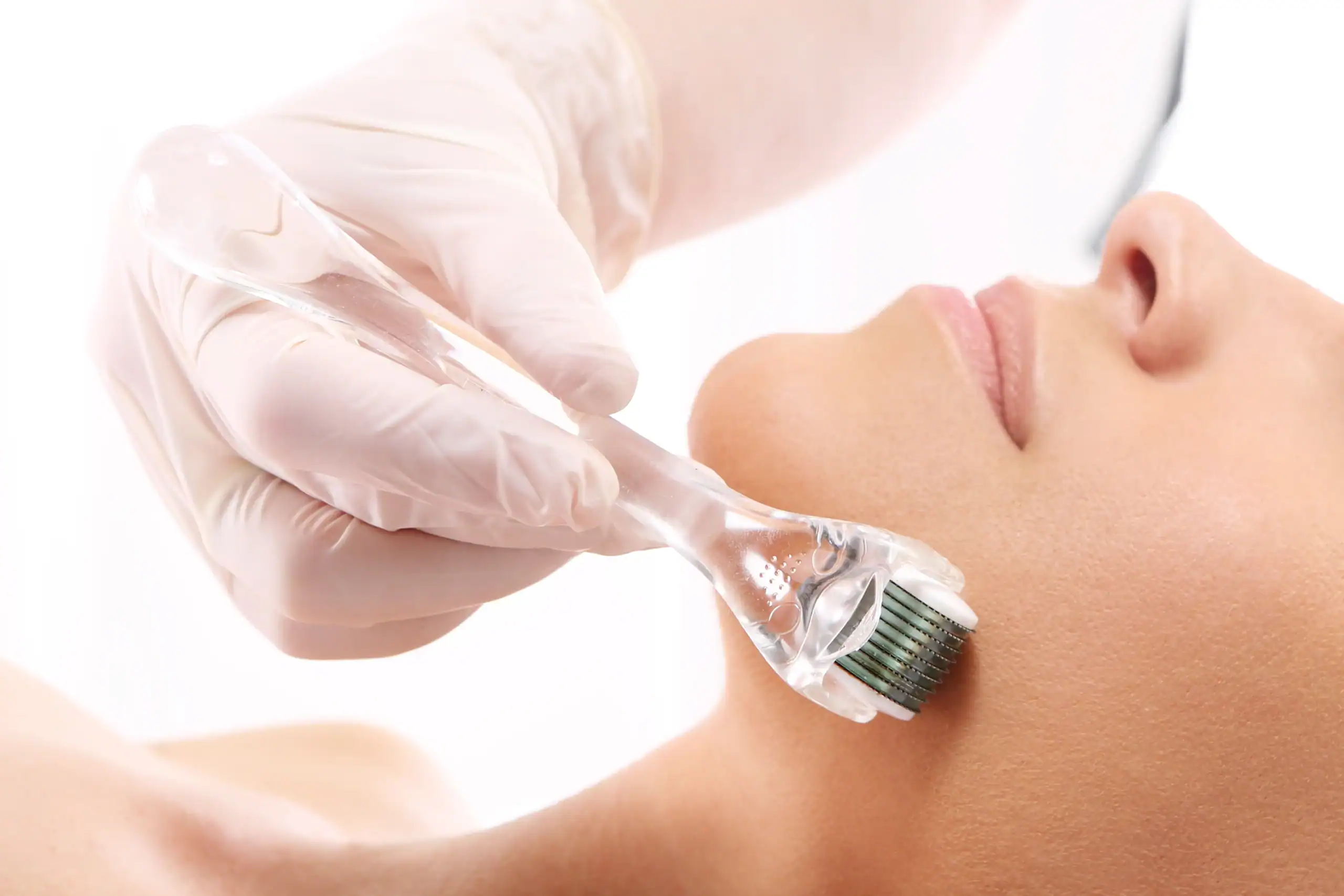
Microneedling involves piercing the top layer of your skin with a dermaroller. This small hand-held instrument is like a paint roller coated with tiny needles. It creates hundreds of little invisible punctures that jump-start the skin’s natural healing mechanisms.
That may sound a bit scary, but this in-office, minimally invasive procedure is virtually painless. Afterwards, you may have some mild swelling and slight bruising. If so, that all resolves within 2-3 days…revealing the beautiful new you underneath.
You’re probably wondering how puncturing the skin can be a good thing. Well you see, we know for sure that aging skin lacks collagen. And the microneedling punctures stimulate collagen production. That’s why it’s also called “collagen induction therapy”. An added benefit is that your skincare products penetrate and are absorbed better, after a microneedling session.
At a microneedling treatment session or two, you’ll notice a reduction in fine lines, deep wrinkles, and crow’s feet. Studies show that nearly 100% of people report excellent results on the anti-aging front.
And, microneedling treatments are also showing outstanding results in reducing the severity of acne scars following treatment. So whether it’s turning back the clock, helping clear old acne scars (or maybe both) … microneedling may be right for you.
Dermaplaning for Healthy, Radiant Skin
Have you ever wondered why your favorite exfoliating cleanser makes your skin look smoother? It’s because it scrapes off that lurking outer layer of dull, dead cells on the skin surface. Dermaplaning is essentially the same thing – exfoliation – but it’s extra-effective because it’s performed by a licensed, trained skincare professional using a sterile surgical-grade scalpel (if that sounds scary, think of it as a fancy razor!).
Dead skin cells and fine hairs need to go, because they make your complexion dull and flaky. They clog pores and predispose your skin to breakouts. Removing dead skin with dermaplaning can benefit all skin types (except people with active inflammatory acne), and restore that youthful glow you long for.
This is a noninvasive in-office procedure that gently shaves the skin surface. You’ll notice improved tone and texture – how does silky smooth skin sound? There’ll be a reduction in acne scars and hyperpigmentation. You’ll have less peach fuzz and your makeup will go on super smooth. Your skincare products will penetrate and work better. Periodic follow-up sessions will keep you glowing.
A dermaplaning treatment at one of our Water’s Edge Dermatology offices is painless and there’s virtually no downtime, other than some slight redness. So, you could get a treatment during your lunch break and head straight back to the office.
When it comes to beauty treatments such as dermaplaning and microneedling, remember that these are precision procedures. You don’t simply want to find "the best deal" and take your chances. You want to find the best facility.
Dermaplaning and microneedling treatments are best done by highly trained, experienced, licensed and insured aestheticians or dermatologists trained in cosmetic dermatology. That's how we do it at Water’s Edge Dermatology. For proper peace of mind, cosmetic procedures are best performed in the safety of a medical office setting.
New Aging Hands Treatment at Water’s Edge Dermatology
Ever meet someone with enough "youthful glow", to be shocked when you see they have very visibly aging hands? Fact is, when you see noticeably aging hands on a middle-aged or younger person… it raises questions.
The cause could be genetic inheritance, too much sun exposure, dry skin, other skin problems, or a combination of all.
The key question is:
What's the most effective new treatment for aging hands?
Let’s face it. You can turn back the clock and get your youthful glow on with a variety of FDA-approved dermal fillers and injectable treatments. From Juvaderm and Scupltra, to Radiesse and Botox, you can shave years off the age showing in your face.
But then you reach out to shake someone’s hand, or give a wave. And your aging hands just do not match the face. In fact, they look almost as sunken, wrinkly and veiny as Grandma’s… ouch.
That’s why our Director of Cosmetic Services Kimberly Van Keuren (R in photo) and Aesthetic Medicine specialist Dr. Bebe Pajo (center-photo) are so excited. They're excited for Water’s Edge Dermatology patients. Kimberly explains, “This new treatment for aging hands, Restylane Lyft, is a dream come true for many of our longtime cosmetic dermatology and aesthetic patients. It's just the kind of help with their aging hands that they’ve been longing and waiting for.”
That wait ends now, with Water's Edge Dermatology (WEderm), among the first dermatology practices nationwide chosen to perform Lyft treatments for aging hands. This new FDA-approved hyaluronic acid (HA) dermal filler has been carefully tested and approved for the correction of volume loss in aging hands.
Giving those aging hands an anti-aging LYFT
Restylane Lyft is the first and only hyaluronic acid dermal filler to receive FDA approval for treating an area other than the face. Dr. Pajo, WEderm’s nationally renowned “Top 20 Sculptra Injector”, elaborates:
“As we age, our hands begin to lose volume, resulting in the appearance of wrinkles, bones, bulging veins and visible tendons. Many of my patients ask what they can do about their aging hands, and I am pleased that we can now offer them an injectable hyaluronic acid treatment that works wonders. Now, their hands can complement rather than clash with the youthful beauty of their face.”
The best thing about getting Restylane Lyft treatments for your aging hands at one of our many Water’s Edge Dermatology offices across South and Central Florida? As with all our cosmetic procedures and aesthetic treatments, your Lyft treatment for aging hands will be performed in a safe, comfortable medical setting.
If you’re ready to book an appointment, great! And if you have questions, please don’t hesitate to contact Cosmetic Director Kimberly for more information, at kvankeuren@wederm.com.
New Skin Cancer Research & Treatment: Mid-2018 Update
For millions of Americans living with basal and squamous cell carcinoma, or melanoma, each new breakthrough in skin cancer research & treatment matters deeply.
For some, it can mean the difference between life and death.
Thankfully, there’s a wealth of productive skin cancer research & treatment activity occurring worldwide in 2018. There’s also more effort than ever to educate the public about prevention. More than ever, people understand that un/under-protected sun (or tanning bed) exposure damages the skin, and causes skin cancer.
But while more people are taking preventive measures, skin cancer rates keep rising. And to nobody’s great surprise, Florida leads the nation in annual diagnosed skin cancer cases.
Given these troubling truths, here’s to raising hopes as well. Let’s take a look at some of 2018’s brighter prospects in skin cancer research & treatment.
Breakthrough in Basal Cell Carcinoma Drug Resistance
With about 2 million new cases yearly, basal cell carcinoma is the most common skin cancer in America – and the most common cancer, period. If caught early enough, it can be treated successfully with surgical removal or targeted radiation treatment. If not, it can spread throughout the body. And, it can become notoriously drug-resistant.
That’s why the early-year announcement from Stanford University researchers was so potentially important. They’ve identified the protein behind the drug resistance and have had initial success blocking it. This has “significantly slowed the growth of drug-resistant basal cell carcinoma in mice”. More research and ultimately clinical trials on humans will be needed, but for now, hopeful news.
New Treatment for Advanced Squamous Cell Carcinoma
Cutaneous squamous cell carcinoma is the second most common skin cancer with a million or so new cases a year. As with basal cell carcinoma, most cases can be treated successfully with surgery and/or radiation. But what if the disease progresses, what then?
For these advanced cases, there’s cause for new hope. The University of Texas MD Anderson Cancer Center announced the breakthrough in early June. A relatively new “immunotherapy” (more on that in a moment) drug called cemiplimab successfully shrank the tumors of almost half the patients in the study, by at least 30 percent.
Those are impressive numbers in the world of skin cancer research & treatment. Impressive enough for the FDA to grant “breakthrough therapy” status to the proposed new treatment, fast-tracking approval – and raising the hopes of many.
Focus of Melanoma & Skin Cancer Research & Treatment Shifting to Immunotherapy
The deadliest form of skin cancer, melanoma, kills another American every hour. More than 175,000 new cases will be diagnosed in 2018… and about ten thousand people will lose their lives.
If caught early and surgically removed, treatment is overwhelmingly successful. At more advanced stages, chemotherapy can be used, while newer targeted therapy and also combination therapy drug treatments are showing increasing success.
In recent years though, much of the focus in skin cancer research and treatment of malignant melanoma has shifted to immunotherapy. These are drug therapies intended to stimulate the patient’s own immune system to detect and kill cancer cells.
Immunotherapy can be systemic, traveling the bloodstream through the entire body. Or it can be local, targeted to particular areas of the body, to specific tumors and lesions.
New targeted and combination treatments using different immunotherapy drugs have gained approval in recent years. Still other new drug therapies are in development. Results are promising.
For individuals and their families coping with advanced stage skin cancer, this can be life-changing or life-saving news. It’s especially worth noting that immunotherapy and other clinical trial opportunities are abundant, and available.
Good Bacteria May Help Treat Skin Cancer
You may have heard increasing evidence in recent years, that “good” bacteria (think probiotics) are critical to our intestinal and overall health. In February, new research from the University of California San Diego School of Medicine showed that the same principle may also apply to skin cancer research and treatment.
Initial tests on mice were intended to show whether common, usually harmless Staph bacteria from our skin could kill dangerous group A strep bacteria (strep throat, etc.). What they report finding instead, is big news:
"This unique strain of skin bacteria produces a chemical that kills several types of cancer cells but does not appear to be toxic to normal cell. We showed activity against melanoma, squamous cell carcinoma and ultraviolet-induced precancerous lesions."
Needless to say, there’s much more research and testing to come. But for now, another exciting 2018 development in skin cancer research.
Significant Weight Loss = Significant Skin Cancer Risk Reduction?
Maybe it’s not so surprising, given the role obesity plays in other diseases and cancers. But the world of skin cancer research and treatment was caught a bit off guard recently when Swedish researchers released their report.
The large-scale study examined 2,000+ patients who’d had bariatric surgery for obesity, studying their overall health outcomes for nearly 20 years following the surgery. The results unexpectedly uncovered a skin cancer risk reduction of more than 40 percent. The risk of developing melanoma? Reduced by more than 60 percent.
Much more study is needed to assess all other factors and cement the seemingly causal link. But for now, more reason for optimism.
In general, 2018 is shaping up as a dynamic year for promising and successful new developments in skin cancer research and treatment. We can only hope for the same, and then some, for 2019 and beyond.
Finding the Right Partner in Skin Cancer Prevention, Detection & Treatment
All the best research in the world can't help people who remain beyond the healing reach of professional dermatological education, detection and treatment. Developing an ongoing partnership with a great dermatologist in Arcadia, Jensen Beach, Lighthouse Point, West Palm Beach or any other Florida locality, really is vitally important.
Having an already-established relationship with a top skin care team specializing in skin cancer can be a huge advantage. There’s simply no better way to understand, prevent, detect, and if necessary, treat skin cancer at the very earliest possible stage – when success rates are extremely high.
From comprehensive annual skin cancer screenings and preventive education to raise skin cancer awareness, to state-of-the-art diagnosis and treatment, to the latest word on the newest skin cancer research and treatment therapies… we’re here, all across the Sunshine State, to unite and work with all Floridians in the fight against skin cancer.
Notes from a Veteran Dermatology Nurse: Getting Started & Sticking With It
A special guest post, written by veteran dermatology nurse Lisa Cheek.
Last week’s observance of National Nurses Week got me thinking and reminiscing. As a veteran dermatology nurse (16 years!), I’ve got plenty of stories, and memories. Some of them good, some of them bad, some happy, some sad.
You may wonder how a young woman gets into dermatology nursing in the first place – and how and why she sticks with it. Allow me to share my story.
I was living in a small Indiana town called Kokomo, going to school for graphic design. A friend working in a dermatologist’s office tells me one day just how busy the office is, that they need help. She asks if I’m interested.
I needed a job and thought to myself, “How hard can it be to treat acne?!” Little did I know how little I really knew about skin, skincare, and dermatology. It didn’t take long after plunging in for me to realize; I had no idea what I was getting myself into.
The jargon and terminology, the difficult diagnoses, the multitude of symptoms, treatments, fluids, smells and more… were just the beginning.
On my very first day, I experienced the smell of cauterization (burning skin) while observing a procedure. Wasn’t sure I was going to make it through the day and remember it like it was yesterday. Could hardly eat my lunch I was so haunted by the smell. But kept telling myself we were helping people… and managed to get past it and move forward.
Onto my next early hurdle. Cysts. If you haven’t seen and smelled what’s sometimes inside one of these, you don’t know what you’re missing – and you don’t want to. Didn't help that the nurse practitioner working with me seemed to express deliver cyst cases my way. Sometimes they ruptured while I was simply numbing the surrounding skin. It seemed like cyst goo followed me around the office.
Then there’s the unique language of dermatology. It was daunting and difficult to get accustomed to. And it kept going into far more depth and detail than I ever imagined it could or would.
To be honest… I really did think dermatology would be mostly acne problems. It didn’t take long to see firsthand just how far off base I was. I had no idea dermatology nurses did so much case-by-case documentation either – the lion’s share, and then some.
There were also aspects of dermatology care I wasn’t even aware of when I started. I had no clue that cosmetic treatments and aesthetic medicine were involved!
Back in the day, it felt like the doctor had to chase some patients around just to inject the filler they’d come to be treated with. Because so unlike today’s treatments, injections involved a very large needle, and it could be painful. Frankly, it was sometimes hard to watch. Thank goodness for the genius who decided we should start adding numbing, painkilling lidocaine to the mix!
I had a lot to learn. A lot. Just like any dermatology nurse, even the ones coming out of nursing school with knowledge and skills I didn’t have when I started. But more so. I set about getting up to speed as quickly as I could, with help.
The dermatologist I was working with would quiz me about each patient’s diagnosis, sometimes right there in the exam room with the patient! It made me nervous and uncomfortable in the beginning. I thought he was just being a pain and trying to make me look dumb.
In fact, he was helping me learn, and grow. It worked. I was like a sponge. I couldn’t get enough of it. I would take notes every day, then go home to study and research dermatology conditions and cases even further.
My compassion and caring for patients and their problems combined with my curiosity and thirst for knowledge. Together, they fueled my professional growth. Developing those habits early on helped make me a better-and-better nurse. They still do. Even 16 years later, I’m still learning about new diagnoses and treatments, still seeing cases I’ve never seen before.
And I am proud of the nurse I have become.
There’s nothing to compare with the gratitude of someone whose suffering has been eased, much less entirely eliminated. To play some small part in that is a great reward.
At the end of the day, that’s what keeps me and most dermatology nurses going, seeing how much we can help people in great distress. That, and for me, the pleasure of sharing my experiences and knowledge with others. Which I look forward to doing more of with all of you, from time to time.
Shingles, Seniors & Medicare Coverage
Chances are, most young people have little idea of what Shingles is, much less how doctors treat it, or Medicare covers it. But the skin disease that’s scourge to so many millions of seniors has its roots in childhood. Chickenpox, in fact.
Back in the day as they say, there wasn’t a vaccine preventing most kids from contracting the varicella-zoster virus that causes chickenpox. On the other hand, children traditionally experience a significantly milder version of the virus than adults do. In fact, many parents have breathed a sigh of relief when their little ones presented with the telltale red, itchy spots; relieved to get it over and done with.
Well, there’s over and done with. And then there’s the difficult reality that if you did have chickenpox as a child, your body still hosts the varicella-zoster virus. It hides out in your nerve tissue near the spinal cord, waiting for years. Then, when the immune system of some unsuspecting senior dips low enough, it can reactivate as shingles.
So, What’s Shingles & What Do You Do About It?
While chickenpox is generally not feared, shingles is another story. While not a life-threatening condition, it remains a skin disease dreaded by at-risk seniors. Dreaded, because as anyone who’s suffered through it can tell you, shingles can be extremely painful. Think itchy red rash, fluid-filled blisters, numbness and/or burning in the skin.
The good news is, shingles is preventable for more than 9 out of 10 people, with a new, more effective-than-ever shingles vaccine. And if you do contract shingles, more good news is that it usually goes away on its own after 2-3 weeks.
Getting to your dermatologist’s office in the first 2-3 days of a shingles outbreak can be a huge help. This allows common treatments such as oral antiviral medication, pain relievers and possibly corticosteroids to provide real relief before things get out of hand.
If you’re over 50, certainly if you’re over 60, the shingles vaccine is highly recommended. Good alternative to all the medical care and treatment you’ll need if you do get it. Which raises a question important to so many senior healthcare patients/consumers:
What Will Medicare Cover When It Comes To Shingles?
Medicare Part A covers hospital benefits and Part B covers outpatient benefits. If you develop shingles, your visits to the dermatologist for diagnosis and treatments are covered by Medicare Part B.
After you meet your annual Medicare Part B deductible ($183 in 2018), Medicare pays 80% of the cost of your doctor visits and related lab tests. You’re responsible for the other 20%, unless you purchase “Medigap” coverage to help limit out-of-pocket costs for such deductibles and copayments.
While Part B covers your doctor’s visits related to shingles, the medications for treating and/or preventing shingles are generally going to fall under Medicare Part D coverage.
How can Medicare Part D Drug Coverage help with Shingles?
Beneficiaries purchase Part D policies from private insurance companies. Some Part D companies include the varicella-zoster vaccine in their drug formularies. When considering aPart D policy, you’ll want to check on that. While this vaccine might cost $200 or more without coverage, beneficiaries with Part D often pay around half that amount when they use their coverage.
For individuals with an active case of shingles, Part D plans should cover a number of medications which help control the infection. Having Part D coverage means you’ll only be responsible for your plan’s required copayment for any of these covered medications instead of full cost.
The most common and least expensive medication is Acyclovir. This medication has been around since the 1980’s and is a generic form of the brand-name antiviral medication called Zovirax.
Your doctor may also prescribe valacyclovir or famciclovir, which are two newer forms of antivirals that may treat shingles more rapidly than acyclovir. That means it’s worth checking for Part D coverage of these drugs too.
Do take note though; many seniors with Medicare Part D Drug coverage still have to confront the infamous Medicare Part D “Donut Hole” (till 2020). This is an actual reduction in coverage that kicks in for seniors whose drug costs exceed a prescribed monthly and/or annual limit.
For the time being, seniors and their loved ones need to take this and all the other above information into consideration when evaluating the costs and coverages for prevention or treatment of shingles.
Latest Eczema Treatments Offer Hope for a Cure
Anyone searching for effective eczema treatments and dreaming of a cure knows, it can be an emotional roller coaster ride. When scientists identify a previously unknown outbreak trigger for what textbooks call atopic dermatitis, hopes rise. But it's hard to stay positive when the next painfully itchy flare-up strikes.
Although there are a number of eczema treatments already available and giving relief to many people, too many people still suffer. So researchers and scientists keep searching for new treatments, and better understanding of this common but still incurable skin disease.
The good news is that recent research does offer eczema sufferers hope for a future with itch-free, unbroken, healthy skin. In fact more than 40 studies are currently underway to find a cure. In the meantime, a couple of promising new eczema treatments are finally available.
Crisaborole: New Ointment for Eczema
Crisaborole (brand name Eucrisa) is a topical (locally applied), non-steroidal ointment. It’s meant to control the symptoms (itching, redness, inflammation, skin cracking/bleeding) of mild-to-moderate eczema, allowing skin to heal.
Being non-steroidal is a big plus for this promising new eczema treatment. While topical corticosteroid ointments can offer symptomatic relief, they can also have potentially dangerous side effects for some people after 3+ months of use.
After being proven safe and effective with less side effects in clinical trials, Crisaborole received FDA approval. This eczema treatment is intended for mild to moderate cases of the skin disorder, for patients aged 2 and older. It’s the first new topical eczema treatment that has been approved in more than a decade. Hopes are high that it will ease the suffering of millions worldwide.
Dupilumab: New Eczema Injection
Dupilumab (brand name Dupixent) is another promising new eczema treatment. It’s given by weekly or biweekly injection to individuals with uncontrolled, moderate-to-severe atopic dermatitis. This is a treatment only for adults, not for pediatric cases.
The hope is that people who have had no luck with topical treatments may now be able to benefit from these injections. And clinical trial results were promising. A large majority of trial participants saw a 50 percent or greater reduction in the severity of their eczema. Even more encouraging is that a healthy number of them are now enjoying almost completely clear skin.
Time will tell, but just the availability of an alternative to topical creams and ointments is a major step forward in eczema treatment.
New Understanding, New Hope for a Cure
Efforts to finally find a cure for atopic dermatitis have been in progress all over the world for years. Still no cure. But a big breakthrough last year can only help the cause moving forward.
Researchers at Newcastle University in England appear to have found a causative factor to explain why people get eczema in the first place. It seems to come down to a deficiency in levels of the human protein called fillagrin.
According to a Newcastle team spokesman, "We have shown for the first time that loss of the filaggrin protein alone is sufficient to alter key proteins and pathways involved in triggering eczema. This research reinforces the importance of filaggrin deficiency leading to problems with the barrier function in the skin and predisposing someone to eczema."
Needless to say, that discovery is lighting a fire under researchers around the globe. Much of their work can now thankfully focus on addressing the root cause of the disease, and finding a cure. Experts agree that as a result, prospects for a cure have never been better.
The maddening question that nobody can answer is of course...When?
Until we have an answer, know that the new (and some of the older) eczema treatments can still provide great symptomatic relief for many people. It’s just a question of partnering with a great dermatologist near you, and finding out what will work best for your particular skin, and your specific case of atopic dermatitis.
Is Blue Light from Screens Bad for Your Skin?
Updated June 3, 2020
Medical review by Ted Schiff, M.D.
Americans are inseparable from their screens, and it’s not just teens staying up late into the night on YouTube and Snapchat. A Nielsen survey found that adults over age 65 spend nearly 10 hours a day watching TV and using computers, smartphones and tablets. The blue light those screens emit can rob us of sleep if we don’t power down a few hours before bed. (Blue light suppresses the release of melatonin, which induces sleep.) But lately, some people have been wondering: Is blue light bad for your skin?
Researchers have begun to investigate whether too much screen time might accelerate skin aging and even cause dark patches to form.
As you read this article in the glow of a digital device, you’ll discover what scientists know and don’t know, and what you can do to protect your skin if you’re concerned about blue light damage.
What is blue light?
Visible light from the sun is made up of rays from all the colors in the rainbow — red, orange, yellow, green, blue, indigo and violet. Light in the blue/violet range, also called high energy visible (HEV) light, has a short wavelength and more energy than other colors. It’s the scattering of these rays that makes the sky look blue in the daytime.
Your home is probably awash in artificial sources of blue light, including screens and also LED lights, compact fluorescent light bulbs (the coil-shaped variety) and any fluorescent lights you may have.
What are the concerns about blue light and skin damage?
A small amount of research suggests that exposure to blue light from digital devices could potentially damage the skin, causing premature aging and hyperpigmentation, or dark patches. (There’s no evidence that blue light causes cancer.)
In one experiment, scientists exposed skin cells that make collagen (the main building block of skin) to light from two models of iPhones and an iPad. After just one hour, the cells experienced oxidative stress, which is thought to contribute to skin aging and wrinkles. However, the screens were positioned just one centimeter from the skin cells — a whole lot closer than you hold your smartphone or tablet to your body.
Other research suggests that too much exposure to blue light may cause hyperpigmentation in certain people. In one study, exposing skin to blue-violet light caused dark patches to form in those with a medium or dark skin tone (not fair-skinned people), and the patches lasted for three months. Red light had no such effect. In a later study, skin cells that produce melanin, the dark pigment responsible for skin tanning, seemed to respond to blue light by making more pigment. Dark skin is rich in melanin.
What we don’t know
These studies raise interesting questions, but much more research is needed to know what harm to the skin, if any, artificial blue light causes.
Some studies have found no evidence that exposure to blue light from devices causes skin problems. A report published in the Journal of the American Academy of Dermatology in 202o found that exposure to light filtered to contain the same color as device by screens for eight hours on five consecutive days didn’t worsen melasma, a condition that causes dark patches on the skin. Blue light from the sun does cause melasma to flare up.
“We don’t need to be overly worried about this at this point,” said Dr. Ted Schiff, founder and chief medical officer at Water’s Edge Dermatology. “All of the research that has been done in the past 50 years has been about ultraviolet light, first UVB and now UVA. It’s only recently that people have considered visible light on the skin. That’s all being researched now. The main focus of skin protection is always going to be ultraviolet rays — they are much more powerful and damaging than any visible wavelengths.”
What can you do if you’re worried?
If you’re concerned about blue light from screens, some fairly simple steps can lower your exposure. In most cases, you can reduce the amount of blue light your computer, tablet or smartphone emits by switching the display settings to “dark mode.” (You can find instructions online.) You can also purchase clear screen coverings designed to filter blue light or download apps that do so.
Some skin care products are said to block blue light (regular sunscreen doesn’t). But be prepared to pay a high price for questionable benefits. Only sunscreens that contain the minerals titanium dioxide, zinc oxide or iron oxide block blue light. In the first two cases, only products that look white on your skin do the job.
“Very little research has been done on these products,” said Dr. Schiff. “Current sunscreens have been tested only for UV, but not any other wavelengths.”
You can also find skin care products containing antioxidants such as vitamin C and vitamin E, which in theory help prevent or repair damage from oxidative stress. In addition, some “sun supplements” claim to protect you from free radicals and UV rays from inside the body. But eating colorful foods and using sunscreen are likely the best bets.
“A healthy diet and lifestyle and use of sunscreens have proven to be effective, compared with supplements that have not been rigorously studied or approved by the FDA,” said Dr. Schiff. “The best way to avoid free radical damage is by wearing sunscreen.”
Finally, to cut down on blue light exposure from screens, consider a digital diet — maybe take a walk after dinner instead of binge-watching Netflix. Unlike the effects of screens on skin, the (positive) effects of walking are well known.
Written by Timothy Gower, an award-winning journalist who writes about medicine and health. His work has appeared in more than two dozen national magazines.
Ten Tips for Super Spring Skincare Routine
Spring is a time for reawakening, rebirth and renewal – including for your skincare routine! If you’re wondering what updates to make, and which cosmetic treatments can work a little extra magic in combination with a spring-freshened skincare routine, read on.
Winter to Spring Skincare Transition
The winter months are dehydrating for your skin. It’s not uncommon for your outermost layer of skin (epidermis, and you knew that, right?!) to appear dull, rough, even raw. Think of what happens when you dry out a plump and juicy plum. Yup… prunes.
In similar fashion, when stripped of moisture your skin tends to shrink and wrinkle. That’s fine for a plum, not so hot for your face. Staying well-hydrated inside and out is an important baseline for spring skincare.
Take heed of some of the following tips too, and you'll have your gorgeous, youthful glow back in no time.
Ten Tips That Can Help
-
- Spring cleaning of your skincare supplies: Throw out old makeup and other skin products and refresh your bathroom shelf.
- Reboot your cleansers: Use moisturizing cleansers to hydrate winter-dried skin. Products with vitamins A, E, C work best when used with warm and not hot water.
- Lighten up: Revise that winter skincare routine for spring by using fewer products overall. Swap heavy creams for lightweight moisturizers with an SPF 30 or more.
- Exfoliate: Once a week, remove dead skin cells to help get all your glow back where it belongs. This also helps your moisturizers penetrate and benefit your skin.
- Wear sunscreen daily without fail: With longer days and stronger sunshine, you have to be more careful than ever to use daily SPF 30+ moisturizer. Using lightweight moisturizer with the sunscreen already included is a good option.
- Eat your way to restored elasticity: Promote collagen formation with foods rich in Vitamin C. Oranges and other citrus, broccoli, kiwis and peppers, all great choices. Foods with the bioflavonoid anthocyanins, such as cherries, and most berries, also help promote collagen levels and elasticity.
- Account for allergies: Facial fallout from seasonal allergies can wreak havoc with even the most seasonally fine-tuned skincare routines. Talk to your favorite dermatologist about impact and treatment for springtime allergies, which cause redness, inflammation, under-eye bags.
- Soothe and comfort your skin: Soak in a warm bath with Epsom salts and/or soothing natural botanical ingredients. Maybe a massage with using therapeutic body oils to slough off dead skin and flush out toxins? You get the idea!
- Consider a cosmetic peel or other rejuvenation treatment: Spring is a great time to get a seasonal-specific chemical peel or other aesthetic treatment. Best to do that with a licensed aesthetician in a dermatologist’s office. These treatments can be game-changers, sloughing off dead skin, brightening the fresh new layer, and reducing age/brown spots.
- Find & wear the right hats: Can't hurt to make a little shopping part of your new spring skincare routine. Look for wide-brimmed, fashionably fun hats that will protect as much of your head and neck as possible.
In addition to the tips above, consultation with an aesthetic medicine specialist will give you great options for treatments best-suited to your individual skin type this spring. There’s an exciting new range of aesthetic treatments available to help you put your best face forward, right through Labor Day and beyond.
Working in partnership with your dermatologist and/or aesthetic medicine specialist, here’s to hoping your skincare routine gets the “Spring Awakening” it needs and deserves this year!
How to Deal With Period-Related Skin Problems
When we talk about menstrual skin, we’re talking about a whole range of skin problems women can encounter during their menstrual cycle each month.
Between the ages of 10-15, most girls begin to menstruate, i.e., they start getting their monthly period. This shedding of tissues and blood from the uterine lining occurs every month for the next 40-something years in most women.
Powerful hormones such as estrogen and progesterone, which help regulate your skin’s ongoing elasticity, circulation and appearance, also control menstruation. That means your period and your skin condition are intimately related, for decades.
The hormonal changes associated even with normal menstruation alone can wreak havoc on a woman’s skin. Added to that, some women also struggle with hormonal imbalances and menstrual cycle irregularities – adding to skin problems such as acne, dryness and flakiness, excessive facial and body hair.
So, what menstrual skin changes occur during your period? Are there special skin care tips for healthy, glowing skin at every stage of your monthly cycle? Here’s the lowdown on menstrual skin, and how to cope with it.
The Menstrual Cycle & Skin Changes
With the start of each monthly period and menstrual cycle, estrogen levels fall and tend to give your skin a dull, washed-out appearance. Then as if that’s not challenge enough, while you’re on your period, your skin is drier and more sensitive than usual.
But have the smartphone and selfie-stick ready for the days immediately after menstruation; because that’s when your skin is at its healthiest.
Then towards the end of the menstrual cycle, just before your next cycle and period begin, progesterone, testosterone and cortisol levels all go up, helping lead to excessive oil production and sending many women with acne-prone skin into an outbreak.
Menstrual Skin Care: What to do when?
For dull, flaky skin at the start of your period:
- Moisturize with gentle skin care products that help retain moisture.
- Hydrate from the inside out by drinking plenty of water.
- Eat healthy fats, such as avocado, nuts, and fish.
For dry, sensitive skin during your period:
- Calm and soothe with gentle products containing Aloe Vera and chamomile.
- Use only a lightweight moisturizer, since the roller-coaster that is your menstrual cycle will have you overproducing oil within a couple of weeks.
- Improve circulation and nourish your skin with regular exercise.
- Eat vitamin-rich foods, such as broccoli, almonds, and fruit.
To maximize skin benefits immediately after your period:
- Go easy on make-up and let your skin breathe.
- Consider a HydraFacial to extract pore-clogging, acne-causing debris from your skin.
- Eat and drink foods rich in anti-oxidants, such as green tea.
For oily, acne-prone skin in the premenstrual period:
- Cleanse with gentle products containing salicylic acid.
- Exfoliate and moisturize with an oil-free moisturizer.
- Eat acne-fighting foods and avoid greasy foods.
All-in-all, it can be daunting, trying to maintain healthy, glowing skin at each stage of your menstrual cycle. But it is entirely possible, and worth the effort. Plenty of sleep, a healthy diet, regular exercise and some basic skin care; these are the first steps. They should lay a solid foundation for maintaining healthy, attractive skin throughout your menstrual cycle.
And if you run into a menstrual skin problem persistently pestering you that you just cannot seem to solve, it’s time to consult with your professional partner in skincare – hopefully one of our outstanding ed providers located across South-Central Florida.
Three Major Misconceptions & Myths About Professional Acne Treatment
We’ve heard more than our share of acne treatment myths in recent years; from how people get acne, to how they can get rid of it, and just about everything in between. Let’s look at three of the more common misconceptions about professional acne treatment.
Myth 1: Dermatologists are basically professional strength pimple-poppers
This is probably the biggest myth about what dermatologists bring to the table when treating acne here in 2018. If psychiatrists are sometimes referred to as “shrinks”, and chiropractors as “bone crackers”, maybe it's understandable that dermatologists are labeled by some (we forgive you!) as glorified “pimple poppers”. But, it's also inaccurate.
Popping pimples is what plenty of people choose to do for themselves already. Plenty more watch graphic videos of the process on YouTube. But our Water’s Edge Dermatology acne experts and others will tell you, pimple-popping is perhaps the worst thing you can do to cystic acne.
This inflammatory act may satisfy an emotional need in the heat of an impulsive moment. But it traumatizes the pimple – both the clogged pore and the skin surrounding it. Your fingers may also be introducing bacteria to your skin and bloodstream that can actually worsen an acne outbreak.
Perhaps the worst part about giving in to frustration and impulsively popping a pimple (or carefully plotting the dark deed for days, either way!) is that it greatly increases your risk of developing an acne scar — either a permanent depression or bump.
So, no; professional acne treatment by a credentialed, qualified dermatology provider has nothing to do with pimple popping. The provider actually uses a very thin, sterilized needle to inject the pimple with medicine, usually an anti-inflammatory. Within minutes to hours, the pimple shrinks from the inside, which smooths the skin. No blood, pus, popping or scarring involved.
Myth 2: I had isotretinoin treatment, so I can’t have a facial
People with severe acne sometimes need a powerful oral medication called isotretinoin. Doctors used to caution patients to wait up to a year after stopping isotretinoin treatment before having cosmetic procedures and/or aesthetic treatments. Imagine just how frustrating that would be. You’re finally getting control of your acne with the right medication – but then hear you have to wait a year to have treatments that could rid you of acne scars and blemishes!
Thankfully, a panel of experts has concluded that there isn’t sufficient evidence to support such cautionary recommendations or restrictions any longer. While patients who have taken oral isotretinoin should still avoid mechanical dermabrasion and laser ablation procedures for 6-12 months, that’s all they need to avoid. There is no good reason to avoid manual dermabrasion, superficial chemical peels, laser hair removal, fractional laser procedures, or even some forms of facial surgery. If you have taken isotretinoin and want a cosmetic treatment or aesthetic procedure, discuss what for you with your cosmetic dermatology provider.
Myth 3: Stronger (more highly concentrated) treatments are always better
While a “stronger” dose makes sense for many medications (e.g. extra strength pain relievers, maximum strength cold relief, etc.), a higher concentration on the label doesn’t necessarily mean an acne treatment is any better for treating acne, or better for you.
When you apply something to your skin for acne, there’s a delicate balance between effectiveness and irritation. Products like benzoyl peroxide do tend to work a little better at higher concentrations. But the maximum concentration isn’t the best for everyone. In fact, many skin products such as benzoyl peroxide can be highly irritating to the skin at higher concentrations.
The bottom line on “stronger” formulas is to proceed with caution, always doing spot tests of any topical ointment being introduced to your skin for the first time. The most foolproof way to be sure you’re getting the best possible treatment for your particular skin and acne, at the right concentration and strength, is to find a Water’s Edge Dermatology office near you and receive professional acne treatment and guidance from a licensed, credentialed and experienced dermatology provider.