Actinic Cheilitis
Actinic cheilitis is a precancerous lesion on the lip caused by chronic exposure to ultraviolet (UV) rays. It’s common in people who spend a great deal of time outdoors. For that reason, it’s sometimes called sailor’s lip or farmer’s lip.
You might mistake the symptoms, which include rough or swollen lips with whitish patches, for garden-variety chapped lips. But actinic cheilitis can progress to squamous cell carcinoma if left untreated. Squamous cell carcinoma can spread to the mouth and other parts of the body.
FAQs about Actinic Cheilitis
- They get more sun exposure because they protrude from the face. The lower lip typically protrudes further than the upper lip, so most actinic keratosis lesions form there.
- The skin of the lips is thinner than that of other parts of the body. It also has fewer sebaceous (oil) glands and less melanin, the pigment produced by skin to protect it from UV rays.
- Are over the age of 60
- Are male
- Have fair skin that burns or freckles easily
- Have worked outdoors for more than 25 years
- Have a history of nonmelanoma skin cancer
- Have a weakened immune system
- Scaly whitish patches on the lip
- Dryness or peeling that won’t heal
- A rough, sandpapery texture
- Blurring of the border between the lip and the adjacent skin
- Loss of color in the skin of the lip
- Swelling or redness of the lip
The most effective way to protect your lips from precancerous or cancerous lesions is to shield them from the sun whenever you’re outside, even on cloudy days and in the winter. Use a lip balm with SPF 30 or higher and apply it frequently. Wear a wide-brimmed hat that shades the front of your face, including your lips.
If you notice any changes to your lips that don’t resolve on their own, see a dermatologist promptly.
Actinic Cheilitis Treatment
Actinic cheilitis is treated with either an in-office surgery or topical medicine. The best treatment depends on the severity of the condition, how much area of the lip is involved and the location.
Surgical options include:
- Cryotherapy (freezing the lesion to remove it)
- Electrocautery (using an electric current to burn off the lesion), sometimes coupled with curettage to scrape it off
- CO2, pulsed dye or erbium laser treatment
- Vermilionectomy (surgery to cut out the lesion)
Topical treatments are typically used when the affected area is large. They include:
- Fluorouracil cream, also known as 5FU
- Imiquimod cream
- Ingenol mebutate gel
- Trichloroacetic acid, a type of chemical peel
- Diclofenac gel, a topical nonsteroidal anti-inflammatory drug
Learn More About Skin Cancer
Nothing found.
Actinic Keratosis
What Is Actinic Keratosis?
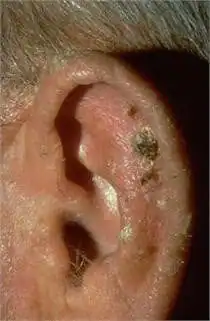
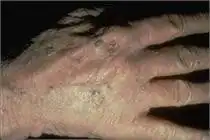
Actinic keratosis is the most common precancer, affecting more than 58 million Americans. Actinic keratosis (AKs) are dry, scaly, rough-textured patches or lesions that form on areas of the body that have received long-term exposure to sunlight, such as the face, ears, lip, scalp, neck, forearms and back of the hands. Some AKs will progress to squamous cell carcinoma.
While AKs share common characteristics, not all AKs look alike. Some are skin-colored and may be easier to feel than see. These lesions often feel much like sandpaper. Others can appear as red bumps; scattered, thick, red scaly patches or lesions; or crusted lesions varying in color from red to brown to yellowish black. The size of an AK ranges from a pinhead to larger than a quarter.
When an AK undergoes rapid upward growth, it becomes a “cutaneous horn,” so named because it resembles the horn of an animal. The size of a cutaneous horn may range from that of a pinhead to a pencil eraser, and the shape may be straight or curved. Sometimes skin cancer hides below a cutaneous horn.
If an AK forms on the lip, it is called actinic cheilitis (key-LITE-iss) and appears as a diffuse, scaling lesion on the lower lip that dries and cracks.
Be sure to see a Water’s Edge Dermatology practitioner if you notice a lesion that looks like any of the above or a lesion that begins to thicken, bleed, itch, or grow. AKs are considered the earliest stage in the development of skin cancer and have the potential to progress to melanoma. Melanoma is considered the most lethal form of skin cancer because it can rapidly spread to the lymph system and internal organs.
(Photos: National Library of Dermatologic Teaching Slides)
What Actinic Keratosis Are Not
While the terminology that dermatologists use can seem confusing, the precise terms allow dermatologists to clearly differentiate skin conditions and prescribe appropriate treatment. Described below are some skin conditions that patients may confuse with AKs. The following conditions are not AKs:
Actinic Porokeratosis
Similar in appearance to AKs, this is an uncommon, usually inherited, skin condition characterized by sun sensitivity that causes reddish brown scaly spots to develop, primarily on the arms and legs.
The lesions appear after years of sun damage to the skin, so they are typically seen in middle-aged and older individuals. The lesions tend to grow or itch after sun exposure and are fairly resistant to treatment.
Seborrheic Dermatitis
Seborrheic dermatitis is a red, scaly rash that itches. Seborrhea is excessive oiliness of the skin, especially on the scalp and face, without redness or scaling. If seborrhea progresses to seborrheic dermatitis, redness and scaling appear.
Seborrheic Keratosis
Also called benign keratoses, these non-cancerous growths have a waxy, pasted-on look and develop on the outer layer of skin. Lesions range in size from a fraction of an inch in diameter to larger than a half dollar. AKs are flatter, redder, and rougher to the touch than seborrheic keratosis.
Actinic Keratosis FAQs
Years of sun exposure cause AKs to develop. All AKs, including actinic cheilitis, develop in skin cells called the keratinocytes, which are the tough-walled cells that make up 90% of the epidermis, the outermost layer of skin, and give the skin its texture.
Years of sun exposure cause these cells to change in size, shape, and the way they are organized. Cellular damage can even extend to the dermis, the layer of skin beneath the epidermis.
Other risk factors include:
- Fair skin
- Blond or red hair
- Blue or green eyes
- Weak immune system
- Age
AKs usually appear after age 40 because they take years to develop. However, those who live in areas that receive high-intensity sunlight year round, such as Florida and Southern California, or those who use tanning beds may develop AKs earlier.
AKs have unique physical characteristics that allow a dermatologist to visually identify these lesions. However, if an AK is especially large or thick, the lesion may be surgically removed for microscopic examination (biopsy) to determine if squamous cell carcinoma is present.
If you find a suspicious skin lesion, be sure to see a Water’s Edge Dermatology practitioner for diagnosis, even if the lesion seems to appear and then disappear for weeks or months and reappear. Our dermatologists receive extensive medical training in skin conditions and have the experience necessary to diagnose various skin lesions. An accurate diagnosis is the first step to successful treatment.
When an AK is diagnosed, your Water’s Edge dermatologist considers a number of factors before choosing the most appropriate treatment method. Factors include:
- Size, number, location, and stage of the lesions
- Age, health, and medical history
- Occupation
- Cosmetic expectations and treatment preferences
- Patient compliance (i.e., willingness to self-treat as needed for several weeks)
- History of previous treatment
Actinic keratosis develops in skin that has been exposed to the ultraviolet (UV) light of the sun for years. Therefore, the best defense against AKs is to practice skin self-examinations and being screened by a dermatologist as needed can help detect AKs and skin cancer in the earliest and most treatable stages.
Actinic Keratosis Treatment Options
Actinic keratosis (AKs) are so common today that treatment for these lesions ranks as one of the most frequent reasons people consult a dermatologist. Treatment options include:
- Cryosurgery (freezing the lesion off)
- Surgical excision
- Curettage (scraping the lesion off) with or without electrosurgery (heat generated by an electric current)
- Topical (applied to the skin) medications. (See PDF instructions for overall AK treatment, Zyclara and Carac.)
- Laser resurfacing
- Medical-grade chemical peels
- Photodynamic therapy: Read our Photodynamic Care Instructions (PDF) to learn more.
Patients who have multiple AKs may not have all lesions treated at the same time, and in some cases, the dermatologist or dermatologic surgeon will use more than one treatment option.
Self-treating by picking off the lesions is not effective because the lesions will grow back. Since AKs have the potential to progress to squamous cell carcinoma, a form of skin cancer that can be life-threatening, AKs should be treated.
Follow your Water’s Edge provider’s advice on how to manage a wound caused by treatment.
What to Expect After Treatment
After being treated for AK, your Water’s Edge Dermatology practitioner will follow up with you for routine re-examinations. It is extremely important to keep these re-examination appointments because when enough sun damage occurs to cause AKs, the possibility of developing more AKs or even skin cancer greatly increases.
Frequency depends on the extent of the AKs, sun-damaged skin, and the treatment method. Your dermatologist may want to re-examine you as frequently as every 8 to 12 weeks or only once or twice per year.
Retreatment is sometimes necessary, as new AKs can develop and occasionally recur. In some cases, your Water’s Edge dermatologist may prescribe topical (applied to the skin) retinoids (vitamin A derivatives) to help prevent new AKs from developing.
Learn More About Skin Cancer
Nothing found.
Sun Safety
Awareness Is the First Step of Sun Safety
The sun is good for many things. It makes flowers grow, warms the earth and provides light. The sun also can harm your skin because it emits ultraviolet radiation. The sun’s ultraviolet A (UVA) rays are called the “aging” rays. UVA can cause wrinkles and age spots. Ultraviolet B (UVB) rays are known as the “burning” rays because UVB rays cause sunburn. Both types of UV rays reach the earth every day. Even on a cloudy day, UV rays can damage your skin. There is no safe UV light, and there is no such thing as a “safe” tan.
In the past, sun exposure was thought to be a healthy benefit of outdoor activity. Modern scientific information, however, has shown many unhealthy effects of sun exposure, such as skin cancer, for adults and children.
Sun Safety FAQs
Part of the sun’s energy that reaches earth is composed of rays of invisible ultraviolet (UV) light. When UV light rays (UVA and UVB) enter the skin, they damage the skin cells, causing visible and invisible injuries. Without protection, the following can occur:
Heightened Risk of Skin Cancer
Most skin cancers develop on areas of the skin that get years of sun exposure, like the face, neck, ears, forearms, hands and trunk. Basal cell carcinomas and squamous cell carcinomas are the most common, but melanomas are the deadliest.
- Squamous cell carcinoma (SCC) can look like a red scaly patch, raised, firm bump or a sore that heals and re-opens. People who have light skin are most likely to develop SCC, but it can develop in dark-skinned people, especially those who have scarring. With early detection and proper treatment, SCC has a high cure rate. Left untreated, SCC can be disfiguring. In rare cases, untreated SCC can spread to other areas of the body and can be fatal.
- Melanoma may develop in a mole or it can appear on the skin as a new, dark spot. Sometimes melanoma contains shades of red, blue or white. When found early, melanoma often can be cured. Left untreated, melanoma can spread to other areas of the body and can be fatal. One person dies of melanoma every hour.
- Actinic Keratosis (AKs) are dry, scaly, rough-textured patches or lesions that form on areas of the body that have received long-term exposure to sunlight, such as the face, ears, lip, scalp, neck, forearms and back of the hands.
Sunburn
Sunburn is the most visible type of damage, which appears just a few hours after sun exposure. In many people, this type of damage also causes tanning of the skin. Freckles, which occur in people with fair skin, are usually due to sun exposure. Freckles are nearly always a sign that sun damage has occurred.
Too many sunburns and sunburns that blister increase your risk of developing skin cancer. Avoiding sunburn is important. If you do get sunburned, find relief from cool, wet compresses, cool baths and soothing lotions. When a fever, chills, upset stomach or confusion develops, you may need to seek immediate medical attention.
Tanning
Tanning is often mistaken as a sign of good health. What a tan actually means is the skin has been injured and scarred. A tan develops when the skin tries to protect itself from harmful UV rays. Indoor tanning is not a safe alternative to sun exposure. Indoor tanning equipment, including tanning beds and sun lamps, emit harmful UV radiation. This radiation can be stronger than that given off by the sun. Whether radiation comes from indoor tanning or the sun, it increases a person’s risk of developing skin cancer, including melanoma. There is no such thing as a “safe” tan.
Aging
Constant exposure to UV rays makes skin age more quickly than normal, and can cause it to become tough and leathery. Skin exposed to the sun can also develop large freckles, age spots, wrinkles and scaly growths or AKs, which are considered an early stage in the development of skin cancer.
Allergic Reactions and Other Conditions
For some people, sun exposure causes an allergic reaction. Common signs of a sun allergy are bumps, hives, blisters and red blotches on the skin. People taking certain medications can develop a rash after being in the sun. Medications that interact with UV light and can cause this reaction include birth control pills, antibiotics and medications for treating blood pressure, arthritis and depression.
Sun exposure can also worsen some diseases. People who have lupus erythematosus or cold sores should protect their skin from the sun. If a flare-up occurs, be sure to consult a dermatologist.
Teach your children to follow the ABCs for fun in the sun.
A = AWAY. Stay away from the sun in the middle of the day. (10 a.m.-4 p.m.)
B = BLOCK. Always use a sunscreen with SPF 30 or higher.
C = COVER UP. Cover as much skin as possible when in the sun. Wear a T-shirt and a hat.
S = SPEAK OUT. Talk with family and friends about sun protection.
Sun protection should begin at infancy and continue throughout life. It is estimated that we get about 80% of our total lifetime sun exposure in the first 18 years of life. Therefore, sun prevention in childhood is very important to prevent skin cancer later in life.
Stay away from the midday sun and its intense rays. Schedule play times and outdoor activities before 10 a.m. and after 4 p.m. (Daylight Savings Time: 9 a.m. to 3 p.m.). The sun’s energy is greatest when it travels through less atmosphere at midday. Sun exposure is more intense closer to the equator, in the mountains and in the summer. The sun’s damaging effects are increased by reflection from water, white sand and snow, so use extra caution in these scenarios.
Avoid long periods of direct sun exposure. Sit or play in the shade, especially when your shadow is shorter than you are tall. Avoid sunburn. Be aware of the length of time you are in the sun. It may take only 15 minutes of midday summer sun to burn a fair-skinned person.
If you take care to be sun smart, you can safely work and play outdoors without increasing skin cancer risk or aging prematurely. It’s never too late to start protecting your skin. Here’s how to stay safe in the sun:
- Generously apply a broad-spectrum, water-resistant sunscreen with a sun protection factor (SPF) of 30 or more to all exposed skin. Broad-spectrum provides protection from both ultraviolet A (UVA) and ultraviolet B (UVB) rays. Reapply approximately every two hours, even on cloudy days, and after swimming or sweating.
- Wear protective clothing, such as a long-sleeved shirt, pants, a wide-brimmed hat and sunglasses.
- Seek shade when appropriate. Remember, the sun’s rays are the strongest between 10am and 4pm. TIP: If your shadow is shorter than you are, seek shade.
- Protect children from sun exposure by playing in the shade, wearing protective clothing and applying sunscreen.
- Use extra caution near water, snow and sand because they reflect and intensify the damaging rays of the sun, which can increase your chance of sunburn.
- Get vitamin D safely through a healthy diet that may include vitamin supplements, not the sun.
Yes! Block sun damage by applying a broad-spectrum UVA and UVB sunscreen lotion, gel or sunstick with an SPF of 30 or higher and reapply approximately every two hours, even on cloudy days. If swimming or participating in intense physical activity, sunscreen may need to be applied more often.
Choose a sunscreen with an SPF 30 or higher. The protective ability of sunscreen is rated by sun protection factor (SPF); the higher the SPF, the stronger the protection. SPF numbers indicate the length of time one can spend in the sun without risk of burning.
When using an SPF 30 sunscreen, a fair-skinned person who normally sunburns in 20 minutes of midday sun exposure may tolerate 15 x 20 minutes (300 minutes) without burning. Apply as much sunscreen as you would a lotion for dry skin. Spread it evenly over all exposed skin, including ears and lips, but avoid the eyelids. Apply sunscreen 30 minutes before sun exposure. Reapply after swimming or excessive sweating.
Invisible sunscreens work by trapping the ultraviolet energy and preventing that energy from damaging the skin. Visible, opaque white or colored sunblock creams prevent all light from entering the skin. They often contain zinc oxide or titanium dioxide (chemical-free sunscreens). They are useful for high-risk areas such as the nose, lips and shoulders.
Infants under 6 months old should be kept out of direct sun and covered by protective clothing. Apply sunscreen beginning at six months. Children under 6 months old should not have prolonged sun exposure, but if this cannot be prevented, sunscreen should be used.
Cover your skin with a hat and light-colored clothing when outdoors. Don’t play or work outside without a shirt. Wear a T-shirt while swimming and a hat after swimming. In addition to filtering the sun’s damaging rays, tightly woven clothing reflects heat and helps keep you cool. Sunglasses that block ultraviolet rays protect the eyes and eyelids.
Get vitamin D safely through a healthy diet that may include vitamin supplements.
Speak out about sun protection now. Do your part to protect others from sun damage. Show your family how to apply a sunscreen by spreading it evenly over your skin. Remember to keep babies out of the sun and use an umbrella over the stroller.
Talk to your child’s coach, camp counselor, scout leader, gym teacher and others about the ABCs for fun in the sun. Ask them to help you with the simple changes that can prevent sun damage. Start preventing sun damage now.
If you notice a mole differs from another or a spot on your skin changes, itches or bleeds (even if it is small), you should immediately contact your Water’s Edge Dermatology provider. These changes can be signs of skin cancer. With early detection and treatment, skin cancer has a high cure rate.
Years of sun exposure also accelerate the signs of aging, such as freckles, sun spots and wrinkles. If you dislike signs of aging that appear on your skin, you also may want to see a Water’s Edge dermatologist to learn about options to treat or help reduce the signs of aging skin.
Learn More About Skin Cancer
Nothing found.
Electron Beam Therapy (EBT) for Skin Cancer in Florida
EBT: Basal Cell and Squamous Cell Skin Cancer Treatment
Electron beam therapy (EBT) is a highly targeted, non‑surgical radiation therapy used to treat select skin cancers, including basal cell carcinoma (BCC) and squamous cell carcinoma (SCC).
At Water’s Edge Dermatology, we are one of the few dermatology practices in Florida offering electron beam therapy as an alternative to surgery for patients who may not be ideal candidates for Mohs surgery or who prefer a non‑surgical treatment option. EBT is especially effective for skin cancers located on delicate or cosmetically sensitive areas such as the nose, ears, eyelids, lips, and face.
Dr. David Herold, a board-certified radiation oncologist at Water’s Edge Dermatology, recommends electron beam therapy in circumstances where Mohs surgery can prove challenging and for patients who desire or prefer a non-surgical treatment option.
Skin Cancers Treated with Electron Beam Therapy
Electron beam therapy may be recommended for certain non‑melanoma skin cancers, including:
- Basal cell carcinoma (BCC) – including superficial and nodular BCCs
- Squamous cell carcinoma (SCC) – including invasive squamous cell carcinoma in select cases
- Skin cancers arising from actinic keratosis that have progressed or are at high risk
Treatment recommendations are based on the size, depth, location, and pathology of the cancer, as well as the patient’s overall health and treatment goals.
Benefits of Electron Beam Therapy for Skin Cancer
Compared to traditional surgery, electron beam therapy offers an effective, non‑invasive approach for appropriately selected skin cancers, particularly when cosmetic outcome and tissue preservation are priorities.
- 90% to 98% cure rate, depending on location
- Little or no discomfort during treatment
- Each treatment lasts less than five minutes
- Side effects are limited to the treatment site, usually involving gradual development of skin irritation, redness or “sunburn” that gradually dissipates after completing treatment
- Cosmetically satisfying results, with minimal or no scarring
Learn more about how EBT works in another video of Dr. Herold.
Who Is a Good Candidate for Electron Beam Therapy?
Electron beam therapy may be recommended for patients who:
- Have basal cell or squamous cell skin cancer in areas where surgery may be difficult
- Have tumors on the face, nose, ears, eyelids, or lips
- Are not ideal candidates for surgery due to medical conditions
- Prefer a non‑surgical skin cancer treatment
- Have recurrent skin cancer after previous treatment
A consultation and evaluation by our dermatology and radiation oncology specialists is required to determine whether EBT is the most appropriate treatment option.
Our Electron Beam Therapy Locations in Florida
Water’s Edge Dermatology offers electron beam therapy at select Florida locations. Patients searching for electron beam therapy near me can receive care at the following offices:
Meet our Electron Beam Therapy Specialists
Electron Beam Therapy FAQs
Cancer cells, unlike normal healthy cells, have a reduced ability to repair damage from electron beam treatment. The electron beam is created by a computer-controlled medical linear accelerator that produces a pure therapy beam that is customized to the cancer site.
Unlike older technologies that use penetrating X-rays or strong, high-dose radioactive sources, the electron beam system used at Water’s Edge Dermatology protects healthy tissues. It works by delivering a series of small electron beam treatments to the cancer site that destroy cancer cells but allow healthy cells to heal.
Superficial electron beam treatment is very effective at destroying both basal cell and squamous cell carcinomas. Most of the published studies report cure rates ranging from 90% to 98%. However, many factors can affect the likelihood of cure, including the cancer size and location, the subtype of histology, if the cancer was treated previously, etc.
Water’s Edge Dermatology offers electron beam therapy (EBT) at the following locations in Florida:
The total length of treatment time depends on several factors, including the size and location of the cancer and the overall desired cosmetic outcome. Most patients complete treatment in 10 to 30 sessions, each lasting less than five minutes. The longer treatment courses tend to deliver better cosmetic results. Throughout the course of treatment, normal everyday activities can be continued, including work and sports. There are no restrictions or limitations.
Side effects are limited to the treatment site. The type of side effects experienced depends on the size and location of the cancer and the length of treatment. In general, most patients gradually develop skin irritation or a sunburn-like redness in the treatment area. Prescription creams or lotions are available to help the healing process. Side effects do not usually begin until the second or third week of treatment and peak a few days after treatment is completed. Then, over the course of two to four weeks, the side effects gradually dissipate. You may lose hair at the treatment site, which might not grow back. There may be subtle lightening of the skin in the treatment area or the development of small spider veins years later. However, most patients are very pleased with their treatment results.
Electron beam therapy is a medically accepted form of treatment for skin cancer. It is covered by Medicare and most major insurance carriers. Our billing specialists can confirm your insurance benefits to determine any out-of-pocket expenses you may incur with this treatment.
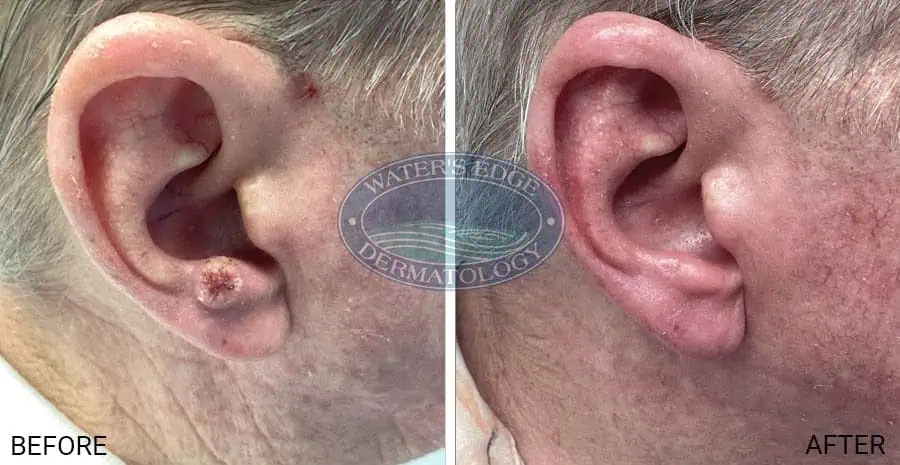
EBT Before + After Photos
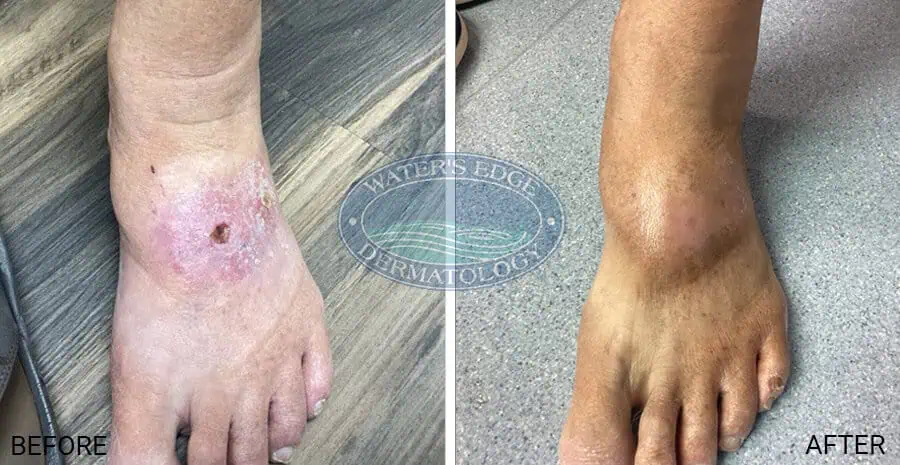
Mohs Surgery
Water’s Edge Dermatology specializes in Mohs micrographic surgery, a highly effective technique for removing skin cancer. The procedure was developed in the 1930s by Dr. Frederic Mohs at the University of Wisconsin and is now practiced throughout the world.
Mohs surgery differs from other skin cancer treatments in that it permits the immediate and complete microscopic examination of the removed cancerous tissue, so that all “roots” and extensions of the cancer can be eliminated. Due to the methodical manner in which tissue is removed and examined, Mohs surgery has been recognized as the skin cancer treatment with the highest reported cure rate.
Typically, Mohs surgery is performed as an single visit and procedure in your Water’s Edge Dermatology office. The patient is awake during the procedure and will experience minimal discomfort.
The Mohs procedure at our Florida offices involves removing the visible portion of the skin cancer, along with a layer of the surrounding skin. The removed tissue is then divided into sections, color-coded and processed to create microscope slides. These slides are immediately examined by one of our expert Water’s Edge Mohs surgeon, who reviews the undersides and edges of each section microscopically for evidence of remaining cancer cells.
If cancer is present in the tissue on the slides, another layer of tissue is removed. It is important to note that any additional tissue removed is only removed from the area(s) where cancer cells are still evident upon microscopic examination. This process is repeated until no further evidence of cancer remains.
Mohs Surgeons: Training and Experience
Residency training in dermatology provides the skill set from which the Mohs micrographic technique is derived: skin cancer pathology, cutaneous histopathology, dermatologic surgery and the repair of complex surgical defects. These skills are further enhanced during residency and, once in practice, through repeated observation and performance of the Mohs technique.
Formal Mohs fellowships are available post-residency and include challenging medical education courses with an emphasis on Mohs surgery and observing other highly experienced Mohs surgeons. Further advancement and refinement of surgical skills allows a Mohs surgeon to treat more complex Mohs cases.
Special Qualifications of Mohs Surgeons
The Mohs surgeons at Water’s Edge Dermatology have specialized skills in dermatology, dermatologic surgery, dermatopathology and Mohs surgery. Basic and advanced training in Mohs surgery is available through selected residency programs, specialized fellowships, observational preceptorships and intensive training courses.
In addition, your Water’s Edge Dermatology Mohs surgeon has the required surgical and laboratory facilities needed to perform the procedure, and is supported by a well-trained Mohs nurse and histotechnological team.
Your Water’s Edge Dermatology Mohs surgeon can provide you with detailed information regarding his or her training in the above disciplines, as well as all applicable professional affiliations.
We Take a Team Approach to Skin Cancer Treatment
In an effort to provide the best possible medical care at Water’s Edge Dermatology, Mohs surgeons sometimes treat patients in partnership with other specialists such as oculoplastic surgeons, ENT (ear, nose and throat) specialists, oral surgeons, plastic surgeons and radiation oncologists.
Mohs Surgery FAQs
Mohs surgery is the preferred treatment for skin cancer found in the eyelid, nose, ear, finger, toe and genitalia, where preserving the maximum amount of surrounding healthy tissue is critical for functional and/or cosmetic purposes. Mohs surgery is also used to remove previously treated skin cancer that has recurred, skin cancer containing scar tissue, large areas of skin cancer, skin cancer with undefined borders and skin cancer that demonstrates unusual growth patterns.
Skin cancer with aggressive subtypes, such as sclerosing or infiltrating basal cell carcinomas, may also require Mohs surgery. A highly skilled dermatologist considers a number of factors in determining whether Mohs surgery is the best treatment option for each case of skin cancer.
If you have any type of suspicious skin lesion, you should seek evaluation by a qualified dermatologist. If skin cancer is suspected, he or she may recommend and perform a biopsy. Mohs surgery may be recommended based on the type and location of the skin cancer, as well as other factors. If your dermatologist does not perform this technique, he or she will be able to refer you to a Mohs surgeon in your area.
Mohs surgery is typically slightly more expensive than other skin cancer treatments because it involves a special multistep process. It is important to consider the effectiveness (five-year cure rates, approaching 99% for new cancers and 95% for recurrent cancers) and advantages of the Mohs technique (healthy tissue sparing capabilities, lower recurrence rate, etc.) in examining the total cost. Our billing specialists can provide you with estimated insurance reimbursement rates and/or possible payment plan information.
Most insurance policies, including Medicare, cover Mohs surgery and any reconstruction needed at the site of the surgery (if necessary). Please enlist the aid of your employee benefits administrator and/or our billing specialists to determine the out-of-pocket expenses you may incur from Mohs surgery.
All surgical procedures have the potential for some degree of visible scarring. The appearance of a post-Mohs surgical scar depends on several factors, including size and location of the skin cancer, individual skin characteristics and the reconstruction options available. You should keep in mind, however, that the tissue-sparing technique of the Mohs procedure may result in a smaller, less noticeable scar than other skin cancer removal methods. The Mohs surgeon also may be able to incorporate suture lines into natural skin lines and folds. Most scars improve in appearance naturally over time, and future scar revision techniques may be employed if necessary.
If you choose to have Mohs surgery to remove the skin cancer on your face, Water’s Edge Dermatology recommends that the surgery be performed by a dermatologist with specialized training in Mohs surgery. Not only are Mohs surgeons skilled at this particular procedure, but they are also trained in the histopathology component of the procedure (examining the tissue samples for evidence of cancer throughout the procedure). At Water’s Edge Dermatology, our Mohs surgeons are highly skilled at Mohs surgery and using techniques to minimize scarring, such as incorporating suture lines into your natural skin lines and folds. For the most complex cases, we also have plastic surgeons on staff to assist.
Another option you have at Water’s Edge is Electron Beam Therapy (Radiation), which is a non-surgical method of treating skin cancers. Water’s Edge Dermatology is one of the only dermatology practices in Florida who offers this alternative surgery option to its patients. With a high success rate and excellent cosmetic results, electron beam therapy might be a good option for you. Read more about it here.
There is no formal board certification process specific to Mohs surgery, as the procedure represents a technique utilized by dermatologists to treat skin cancer. American Society for Mohs Surgery (ASMS) Fellow and Affiliate members must be board-certified in dermatology by the American Board of Dermatology or the American Osteopathic Board of Dermatology. The surgical, histopathologic interpretation and reconstruction components of Mohs surgery are learned by dermatologists during their residency training. In addition, dermatologists are examined in these areas by their respective boards.
Some skin cancers can be deceptive in size – meaning, they appear small on the surface of the skin, but are far more extensive under the skin. These cancers may also have “roots” in the skin or along blood vessels, nerves or cartilage. Additionally, skin cancers that have recurred following previous treatment may send out extensions, or roots, deep under the scar tissue that has formed at the site. Mohs surgery is specifically designed to remove these cancers by tracking and removing these cancerous roots.
For this reason, it is impossible to predict how much skin will have to be removed during Mohs surgery prior to the procedure. The surgeon may only have to remove a little more skin than what is initially seen on the surface but occasionally, more skin needs to be removed due to the presence of deep roots of a skin cancer. It is important to remember that Mohs surgery removes only the cancerous tissue – the healthy, normal tissue is left untouched. Removing the roots of the skin cancer also greatly reduces the likelihood of recurrence.
Clinical studies have shown that Mohs surgery provides five-year cure rates, approaching 99% for new cancers and 95% for recurrent cancers.
What To Expect: Mohs Micrographic Surgery
1. Preparing for Mohs Surgery
If you are taking prescription medications, continue to take these unless otherwise directed by a physician. However, you should inform your Water’s Edge Mohs surgeon if you are taking blood-thinning medications such as Coumadin, Plavix, aspirin, aspirin substitutes (such as Advil, Motrin, Naprosyn, etc.), vitamin E, gingko, garlic, ginseng, ginger, ephedra or other nutritional supplements. These medications and supplements can sometimes cause an increased chance of bleeding after surgery. Prescription blood thinning medication should never be discontinued without approval of the prescribing physician.
2. After Surgery
Most patients do not complain of significant pain. If there is some discomfort, normally Tylenol (acetaminophen) provides adequate relief. However, stronger pain medications are available and will be prescribed when needed. You may experience some bruising and swelling around the wound, especially if surgery is performed near the eye area.
3. Wound Healing, Scarring and Scar Revision
As with all forms of surgery, a scar will remain after the skin cancer is removed and the surgical area has completely healed. Mohs micrographic surgery, however, will leave one of the smallest possible surgical defects and resultant scars. Often, wounds allowed to heal on their own result in scars that are barely noticeable. Even following extensive surgery, results are frequently quite acceptable.
In addition, scars do have the ability, through the body’s own natural healing properties, to remodel and improve in appearance for a six- to 12-month period. There are also many other techniques available to the patient for enhancement of the surgical area following skin cancer surgery.
Depressed or indented scars may be elevated using a facial filler such as Radiesse or Sculptra. Likewise, a raised or roughened scar may be smoothed using laser resurfacing or chemical peeling techniques. Skin flaps and grafts also may require a subsequent touch-up procedure to further improve their appearance. Talk to your surgeon or other members of your Water’s Edge Dermatology team to understand what options are a good fit for your situation.


















